Caesarean Section Max Brinsmead MB BS Ph D

Caesarean Section Max Brinsmead MB BS Ph. D February 2020

Advances in Caesarean section: n n n n n Blood transfusion Spinal anaesthesia* Joel Cohen-type incision* Cord traction for the placenta* Peritoneum not sutured* Suture fat if >2 cm but do not drain* Prophylactic antibiotics* (before skin incision and not co-amoxiclav) Early oral fluids and ambulation Rectal NSAID for analgesia More Caesareans n n Quicker operations Sooner rather than later *Confirmed by RCT

Yet to be tested. . . n n n n n Role of the assistant Fetal pillow (2 nd stage cephalic) Exteriorising the uterus (more pain) Single or dual layer closure uterus Mucosa-excluding suture When to drain (routinely not recommended) PPH prophylaxis (5 IU Syntocinon by slow IV) Thromboprophylaxis When CS is better than vaginal delivery n n n Breech Previous Caesarean section Twins Midcavity arrest Symphysiotomy or CS All patients!!

So who needs a Caesarean section? n n n I really don’t know But many of my obstetric colleagues seem to know So 50 – 70% of Caesareans are now elective procedures And we should be aiming for 100% elective CS Because non elective CS is the worst of the 3 options

Absolute indications for Caesarean: n n n Two or more previous CS Transverse lie Repeat APH unless placenta previa can be absolutely excluded Known contracted pelvis Complex twin presentations e. g. breech and transverse (Source: Lawson, Harrison & Bergstrom)

Risks of Caesarean Delivery n Difficult to quantify because: Most studies do not distinguish between elective and emergency operations n The reason for the CS needs to be considered n Some events are rare n n The question will only be resolved by: n. A randomised trial n With long term follow up

More likely with Caesarean birth: Hospital stay 2 -fold Intensive care 9 -fold Maternal death 2 -10 fold Bladder or ureter damage 30 -fold Hysterectomy 40 -fold Thromboembolism 4 – 16 fold Stillbirth in next pregnancy 2 -fold Rate of preterm in subsequent pregnancies Placenta previa in next pregnancy 2 -fold Placenta accreta in future pregnancies For the Neonate: Respiratory distress esp. after elective CS <39 w Asthma, atopy and obesity ? due to altered microbiome

Same rate for vaginal and CS Birth: Postpartum haemorrhage Endometritis Genital tract injury Faecal incontinence Postnatal depression Back pain Dyspareunia

More Likely with Vaginal Birth: Perineal pain 2. 5 -fold Urinary incontinence 1. 6 -fold Uterovaginal prolapse 2 -fold
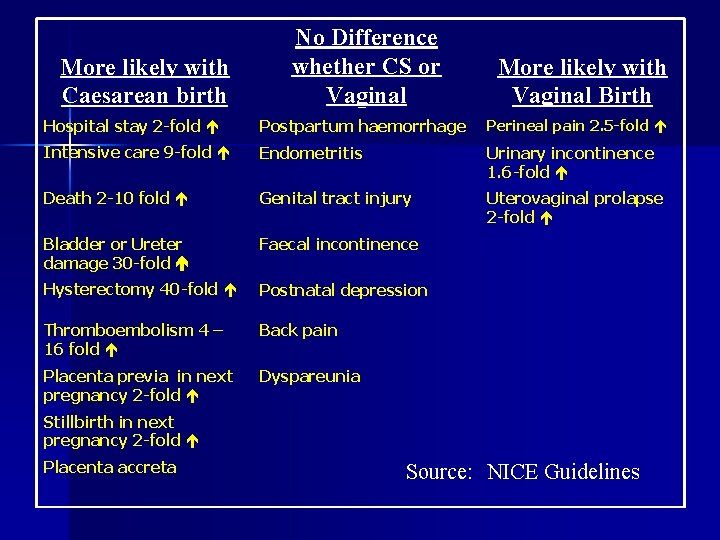

More likely with Caesarean birth No Difference whether CS or Vaginal More likely with Vaginal Birth Hospital stay 2 -fold Postpartum haemorrhage Perineal pain 2. 5 -fold Intensive care 9 -fold Endometritis Urinary incontinence 1. 6 -fold Death 2 -10 fold Genital tract injury Uterovaginal prolapse 2 -fold Bladder or Ureter damage 30 -fold Faecal incontinence Hysterectomy 40 -fold Postnatal depression Thromboembolism 4 – 16 fold Back pain Placenta previa in next pregnancy 2 -fold Dyspareunia Stillbirth in next pregnancy 2 -fold Placenta accreta Source: NICE Guidelines

VBAC – The Controversy n “Once a Caesarean always a Caesarean” – Edwin Cragin – 1916 – In an era of classical CS – Designed to prevent unnecessary primary CS For 60 years “Trial of (lower segment) scar” was standard British practice n But repeat CS more common in the US n Controversy broke out again in 2000 n And it was all about fetal risks n

VBAC – The Controversy Smith et al from Cambridge UK in JAMA 2002 Reviewed 313, 238 singleton births, 37 - 43 w, cephalic presentation in the Scottish Morbidity Register 1992 -1997 excluding congenital malformations and found… 1. Rate of perinatal death 11 times higher for VBAC compared to elective CS 2. This is 2 times higher than for multiparas having a vaginal birth

VBAC – The Controversy Guise et al from Portland Oregan in BMJ July 2004 Reviewed 568 publications on VBAC vs elective CS but found only 71 had useful data Concluded that the additional risk of perinatal death from attempted VBAC was 1. 4 per 10, 000 (95 percent confidence limits 0 - 9. 8) In only 5% of uterine ruptures did the baby die This means that one has to perform 7142 elective CS to prevent one baby death

Advantages of VBAC n Greater maternal satisfaction – But it’s not all about “me” n Quicker recovery – But not always n Cheaper – But not much cheaper than elective CS and can be much more costly n Less RDS for babies – But greater risk of death & disability n Less maternal morbidity and mortality – But these are rare with elective CS

Advantages of VBAC - 2 n More vaginal births in the future – But what’s the point if there’s only to be two kids! n Less maternal depression – But there is no evidence that this is so n Breast feeding more likely to succeed – Occurs in the delivery room – Easier for mothers without wound pain n Avoids risks unique to CS – But these are rare

Advantages of Elective CS n Certainty of timing – That’s the modern way! n Certainty of outcome – If I have a 30 – 50% chance of CS just do one! – Emergency CS more dangerous n It’s Pain-free – More or less guaranteed! n Often preferred by fathers & obstetricians – That’s a male thing

Advantages of Elective CS n Protects the pelvic floor – Controversial because – Some risk arises from the pregnancy itself – And CS may not be protective n Safer for babies – But the absolute risk of VBAC is small n Avoids the risk of scar rupture – But there is much uncertainty about the frequency of this – and the maternal and fetal risks

VBAC Risk to the Fetus n n n The rate of perinatal death is 11 x higher than for elective CS BUT… This risk is equivalent to that of being a fetus to a Primigravida The absolute risk is only 4. 5 per 10, 000 births Confidence limits are wide In the 2002 UK publication all emergency CS were classified as attempted VBAC

Maternal Risk from VBAC n Meta analysis of risk of death – 2. 8 per 10, 000 with trial of scar – 2. 4 per 10, 000 for elective CS – No maternal death ever attributed to scar rupture n Scar rupture – Much confusion in the literature over the definition – Rate of asymptomatic scar rupture the same whether VBAC or elect CS – Overall rate approx. 0. 5% or 1: 200 – Was 0. 35% in the largest combined contemporary study n Hysterectomy – Additional risk from trial of scar is 3. 4 per 10, 000 – Requires 2941 elective CS to prevent one hysterectomy

Patient selection for VBAC n Type of previous CS – 10% risk of rupture from classical and T incisions – Myomectomy and Hysterotomy n Indication for Previous CS – But 50 -75% of patients can VBAC after previous CS for CPD! n Previous obstetric history – VBAC success >90% if there has been prior vaginal birth – Dilatation at the time of previous CS – Gestation at previous CS – was there a lower segment? n Number of previous CS – Increasing risk with increasing number

Patient selection for VBAC -2 n Time since previous CS – Risk of scar rupture is 2 – 3 x greater if <12 m n Maternal weight – Miserable rates of VBAC for women >135 Kg n Lower uterine segment thickness – No uterine ruptures if >4. 5 mm n Maternal Age – Clear evidence for declining uterine performance with age at first labour n Family history of labour performance – A field ripe for study

Patient selection for VBAC - 3 n Size of the mother and baby – But we are very bad at estimating this n Other pregnancy problems – Should be assessed according to obstetric principles n Engagement and cervical ripening – Best assessed at the onset of labour n Labour performance – That’s why it’s called trial of scar – Dilatation and descent – Progress rather than arbitrary time limits n Psychological Factors – The patient’s willingness and drive – The support provided

More than one previous CS? Tahseen & Griffith BJOG Jan 2010 in a systematic analysis of available data and meta analysis concluded: 1. 2. 3. 4. Overall success 71. 1% Risk of scar rupture 1. 36% (this is 3 x greater than for one CS) Perinatal risk is 0. 09% (this is 3 x greater than for one CS) The overall maternal morbidity was the same as that for elective CS Hysterectomy, transfusion, febrile morbidity etc

More than two previous CS? Cahill et al BJOG 2010 in a retrospective cohort study 89 women with >2 previous CS concluded: 1. 2. 3. Overall success 79. 8% No cases of uterine rupture The overall maternal morbidity was the same as that for elective CS Hysterectomy, transfusion, febrile morbidity etc

Lower segment thickness and risk of scar rupture Rozenberg et al Lancet 1996 studied 642 women with ultrasound , measured the thinnest point of the lower segment against a filled bladder, then attempted VBAC: >4. 5 mm - no ruptures or dehiscence 3. 6 - 4. 5 mm 2% rate of scar rupture 2. 6 - 3. 5 mm 10% rate of scar rupture <2. 6 mm 16% rate of scar rupture (278) (177) (136) (51) Can be technically difficult particularly in obese woman Vaginal and 3 -dimensional measures promising

VBAC for the Obese? Carrel et al (Am J OG in 2003) studied 70 women >200 lb, 70 who were 200 -300 lb and 69 >300 lb 81. 8% success for those <200 lb 57. 1% success for those 200 -300 lb 13. 3% success for those >300 lb Infection rate was: 5. 7% group 1 11. 4% group 2 39% group 3 (Very similar results published in 2001)
VBAC for Older Women? Byfield et al Am J OG in 2004 studied 659 women <30 years age, 721 who were 30 -35 years age and 370 >35 years age 72% success for those <30 71% success for those 30 -35 65% success for those >35 Scar rupture rate was: 2. 0% group 1 1. 1% group 2 1. 4% group 3

Pregnancy Interval and Risk of Scar Rupture Byfield et al Am J OG in 2002 studied 1527 women who attempted VBAC at <12 to >36 months after previous CS: 4. 8% ruptured for those <12 m 2. 7% ruptured for those 13 -24 m 0. 9% ruptured for those 25 -36 m 0. 9% ruptured for those >36 m Also found 4 -fold increased rate of rupture when the previous CS was a single layer closure (Similar finding published in 2000)

Induction of Labour for VBAC? Ravasia et al Am JOG 2000 studied 2119 women attempting VBAC between 1992 and 1998 of whom 27% had an induction of labour Spontaneous labour rupture rate Induced labour Cx ripening c PGs Cx ripening c Foley IOL not using PGs 0. 45% scar 1. 4% 2. 9% 0. 7%

Induction of Labour for VBAC -2? Lyndan-Rochelle et al NEJM 2001 studied all women attempting VBAC between 1987 and 1996 in Washington state Rate of Scar Rupture No labour 1. 6 per 1000 Spontaneous labour 5. 2 " " Induced labour (not PGs) 7. 7 " " Induced with PGs 24. 5 " " However this study used ICD 9 codes for identifying scar rupture and these are only 40% accurate

Induction of Labour for VBAC -3? Lin & Rayner Am JOG 2004 studied 3533 women attempting VBAC after one or more CS, 2523 in spontaneous labour, 438 by elective CS, 430 induced with oxytocin and 142 induced with Misoprostol Rate of scar rupture was significantly higher when labour was induced. No significant difference between oxytocin (0. 8%) and Misoprostol (1. 1%)

Canadian College Surgeons & Physicians Guidelines 1993 - 1 Trial of labour should be recommended to all women who have had only one previous CS. Except for: Previous classical, T or unknown uterine incision Previous hysterotomy or full thickness myomectomy Previous uterine rupture Any contraindication to labour in this pregnancy eg placenta previa, transverse lie etc. The wish of the patient is paramount (and the partner should ideally also be involved)

Canadian College Surgeons & Physicians Guidelines 1993 - 2 The patient should be made aware of the hospital’s resources and any limitations The previous obstetric record should be consulted Consultation with a specialist obstetrician is not mandatory Induction of labour with oxytocin or Foley catheter is acceptable Augmentation with oxytocin is acceptable but caution required if arrest has occurred in the active phase of labour

Canadian College Surgeons & Physicians Guidelines 1993 - 3 Continuous EFM required only when induction or augmentation of labour is used The problem of false positives No evidence that it is a specific indicator of scar rupture Epidural anaesthesia not contraindicated Twins not contraindicated Suspected fetal macrosomia & diabetes not contraindicated

Caesarean Sections are Popular because: n Caesarean Section is Convenient n Caesarean Section is Simple n Caesarean Section is Safe n Caesarean Section is better for babies n When you have done a Caesarean you have done everything possible – the medicolegal imperative

Caesarean Sections are Popular because: n n n Vaginal Birth is Painful Vaginal Birth is Unpredictable - If there is a 1: 3 or even a 1: 5 chance of requiring a CS why not just do one? “Vaginal Birth Ruins your Sex Life” n n n There is no evidence for this And the contrary may be true “Vaginal Birth Destroys the Pelvic Floor” n n n Risk of urinary incontinence rises 1. 6 –fold But only exclusive CS will prevent that and. . . 40% of parous women will have incontinence in later life regardless of mode of delivery

Caesarean Sections are Popular because: n “Once a Caesarean always a Caesarean” n The Term Breech Trial n Loss of Obstetric Skills n Pressures on Medical Resources

More Caesarean Sections occur when: n n n Fetal distress is diagnosed by CTG There is concern about transmission of an infection e. g. Herpes, Hep C, HIV There are medical problems and non obstetricians are involved e. g. diabetes, back pain, epilepsy Patients are privately insured GPs and midwives compete with specialists

Caesarean Sections are Popular because: n The Power of Choice n Fathers have influence n It is Fashionable n Reduced Family Size

Caesarean Sections are increasing because: n There is an obesity epidemic n Maternal age is increasing n Epidurals sometimes fail n Induction of labour sometimes fails n An epidemic of sexual abuse?

Caesarean Sections are increasing because: n “My mother and my sisters all had Caesareans” n “This is an IVF baby” n Evolution of the species?

Questions or Comments Please leave a Note on the Welcome Page to this website
- Slides: 42