Acute Compartment Syndrome Marc Hirner Demographics n Incidence


















- Slides: 24

Acute Compartment Syndrome Marc Hirner

Demographics n Incidence: Men n Women n n 7. 3/100, 000 0. 7/100, 000 69% due to trauma 36% fx tibia n 9. 8% distal radius n 23% soft tissue injury without fx n n 10% on anticoagulants


Case 1 n Patient with ? Trivial knee injury Seen in ED and admitted Registrar to ward , pulseless limb Was in fact a knee dislocation that reduced spontaneously End result popliteal artery repair , fasciotomy , ligament reconstruction and eventual BKA

Case 2 n Simple fibula fracture Referred to White Cross several days after injury with tight swollen calf Diagnosed acute compartment syndrome 5 days late Fasciotomy of no use as muscles necrotic

Case 3 n Child required IV access so the tibia was used for rapid infusion Fluid into the calf Acute compartment syndrome Orthopaedics notified late Fasciotomy no use as muscles necrotic

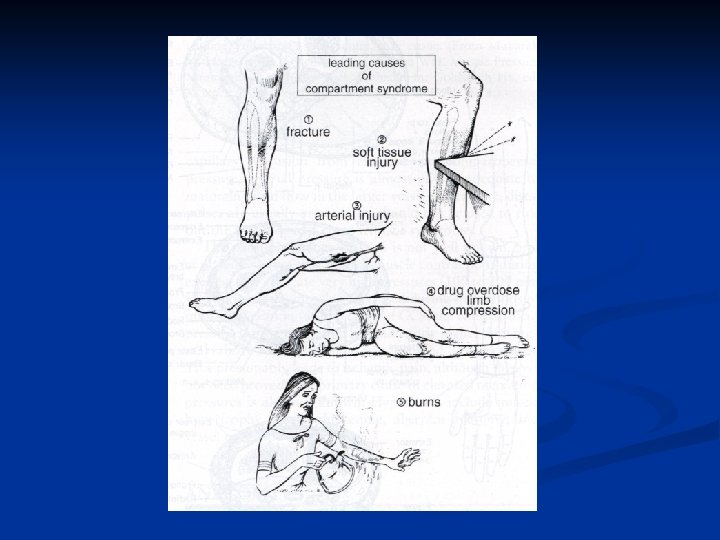
Etiology

Pathophysiology Increased compartment pressure Increased venous pressure Decrease A-V gradient resulting in muscle and nerve ischemia.

Diagnosis History n Clinical exam: the Ps n Compartment pressures n Laboratory tests n CPK n Urine myoglobin n

Clinical Diagnosis n The six ‘Ps’: Pressure n Pain n Paresthesia n Paralysis n Pallor n Pulselessness n

Pressure n Early finding n Only objective finding n Refers to palpation of compartment and its tension or firmness

Pain n Out of portion to injury n Exaggerated with passive stretch n Earliest symptom but inconsistent n Not available in obtunded patient

Paresthesia n Early sign Peripheral nerve tissue is more sensitive than muscle to ischemia n Permanent damage may occur in 75 minutes n n Difficult to interpret n Will progress to anesthesia if pressure not relieved

Paralysis n Very late finding n n Irreversible nerve and muscle damage present Paresis may be present early n Difficult to evaluate because of pain

Pallor & Pulselessness n Rarely present n Indicates direct damage to vessels rather than compartment syndrome n Vascular injury more of contributing factor to syndrome rather than result

Compartment Pressure n When n n Confirm clinical exam Obtunded patient with tight compartments Regional anesthetic Vascular injury Technique n n Whiteside infusion Stic technique: side port needle Wick catheter Slit catheter

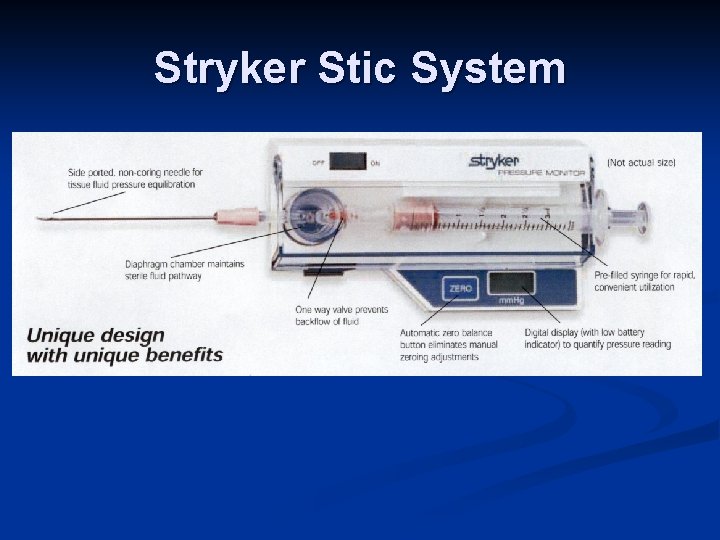
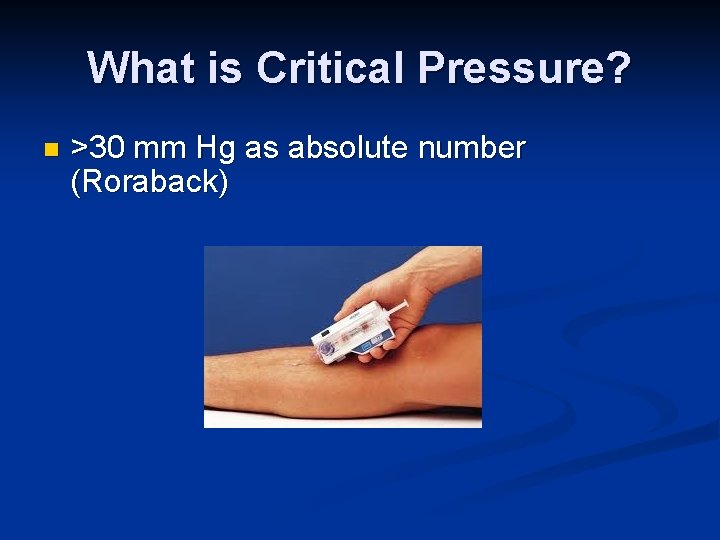
Stryker Stic System Easy to use n Can check multiple compartments n Different areas in one compartment n

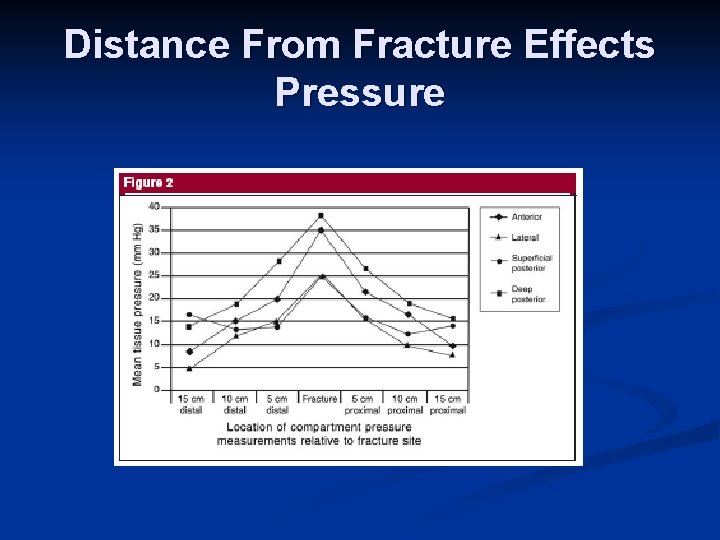
Distance From Fracture Effects Pressure

What is Critical Pressure? n >30 mm Hg as absolute number (Roraback)

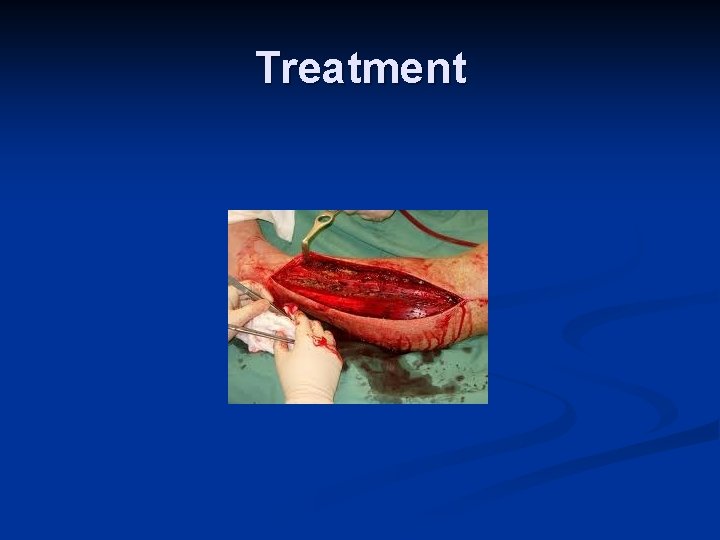
Treatment n Lower leg to level of the heart n Remove cast n Split all dressings down to skin

Treatment If concerned refer these patients early n Fasciotomy if continued clinical findings and/or elevated compartment pressure

Treatment

Wound Care n Soft tissue coverage by 5 -7 days n Delayed closure n Vascular loop ‘lace technique’ n Split thickness skin graft n Flaps or free tissue transfer

NO ONE EVER BLAMES US FOR DOING A FASCIOTOMY BUT MISSING COMPARTMENT SYDROME IS A DISASTER