National Emergency Laparotomy Audit Improving Patient Care www















- Slides: 39

National Emergency Laparotomy Audit Improving Patient Care www. nela. org. uk info@nela. org. uk

• Summary of year 3 results • Trends in national picture • How NELA might change in next few years

NELA participation so far… Clinician Engagement • Year 1: 21, 000 patients from 191/195 hosps – 65% case ascertainment • Year 2: 23, 000 patients from 186/191 hosps – 70% case ascertainment • Year 3: 25, 000 patients from 187/191 hosps – 80% case ascertainment

Year 3: 25, 000 patients (83%) from 187 hospitals • Personal practice still improving • Organisational change still challenging • Still considerable variation 4

i)Processes

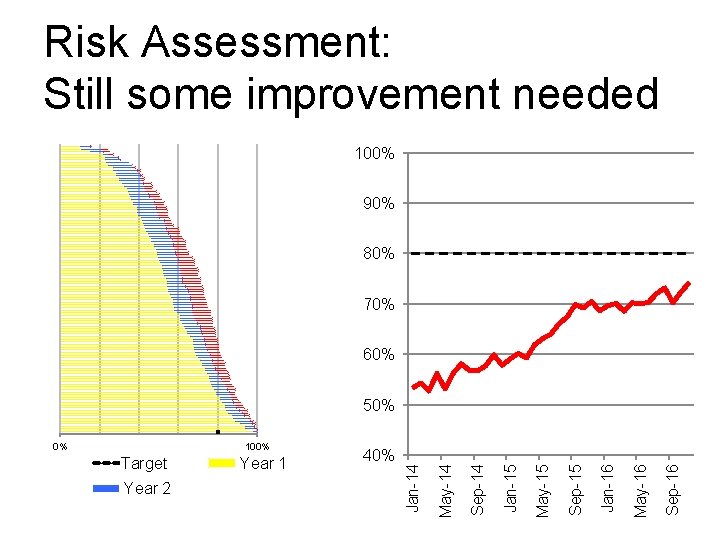
Risk Assessment: Still some improvement needed 100% 90% 80% 70% 60% 50% Sep-16 May-16 Jan-16 Sep-15 May-15 40% Jan-15 Year 2 Year 1 Sep-14 Target May-14 100% Jan-14 0%

Risk Assessment, appreciation and communication of risk leads to better standards of care Key aim to improve care is to improve risk assessment

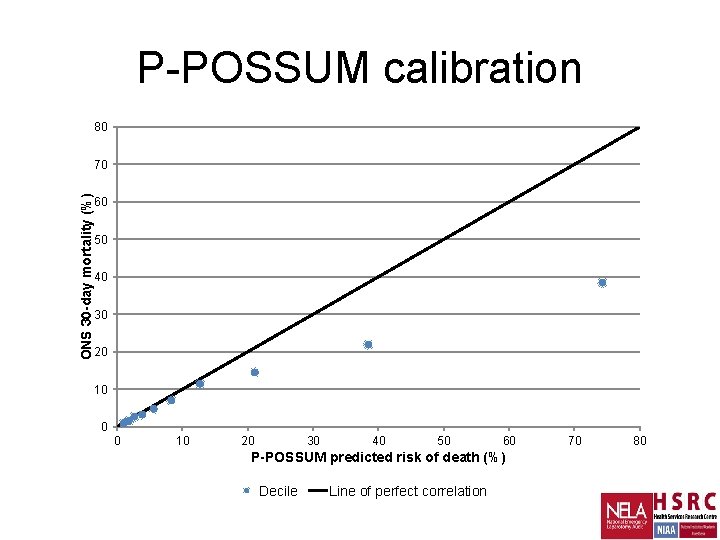
P-POSSUM calibration 80 ONS 30 -day mortality (%) 70 60 50 40 30 20 10 0 0 10 20 30 40 50 60 P-POSSUM predicted risk of death (%) Decile Line of perfect correlation 70 80

POSSUM implications • Useful for allocation of resources if mortality risk <15% • Falsely reassuring for O: E mortality calculations, especially at higher risk • Recalibrated mortality now NELA website and app

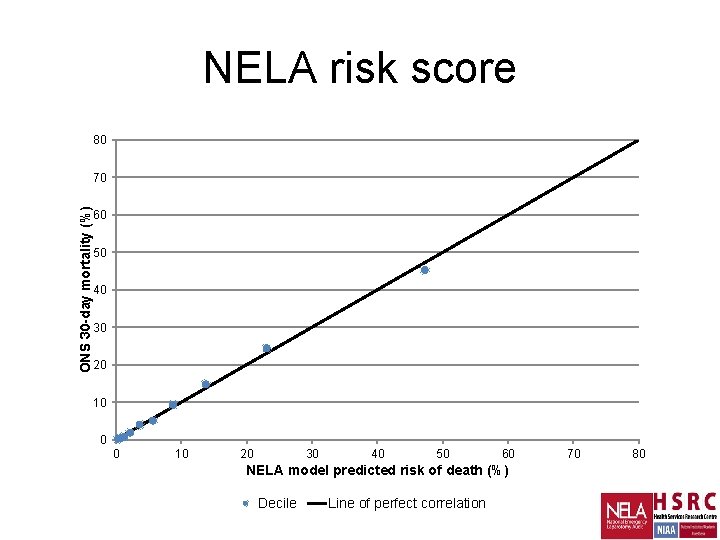
NELA risk score 80 ONS 30 -day mortality (%) 70 60 50 40 30 20 10 0 0 10 20 30 40 50 60 NELA model predicted risk of death (%) Decile Line of perfect correlation 70 80

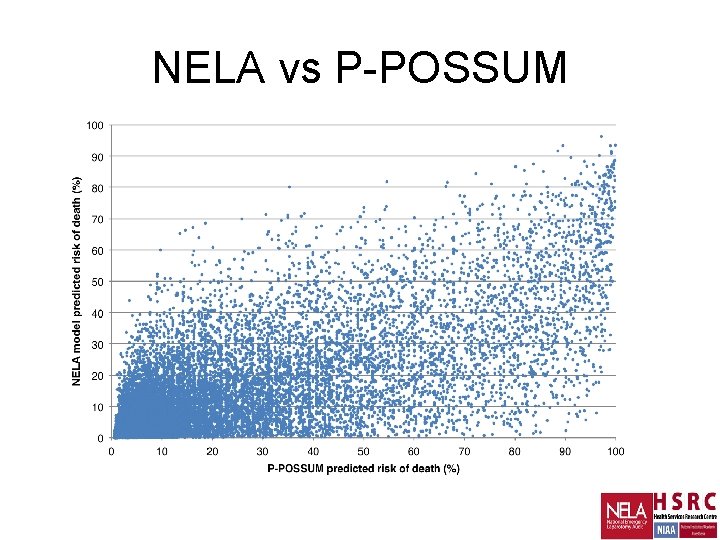
NELA vs P-POSSUM

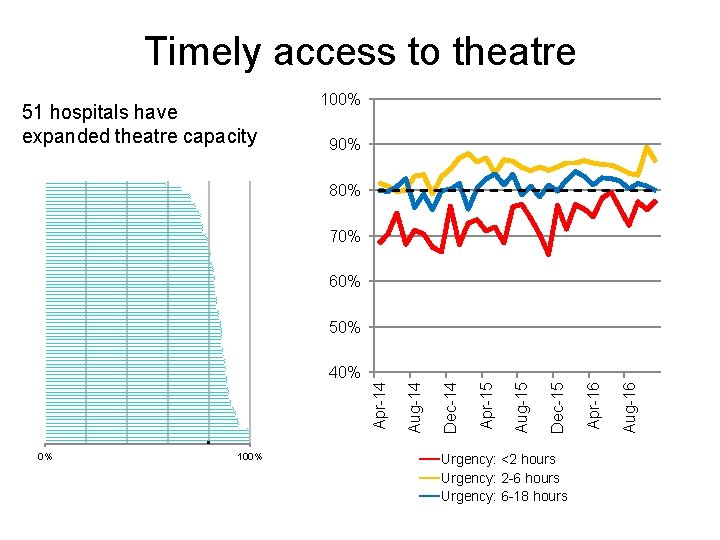
Timely access to theatre 51 hospitals have expanded theatre capacity 100% 90% 80% 70% 60% 50% 0% 100% Urgency: <2 hours Urgency: 2 -6 hours Urgency: 6 -18 hours Aug-16 Apr-16 Dec-15 Aug-15 Apr-15 Dec-14 Aug-14 Apr-14 40%

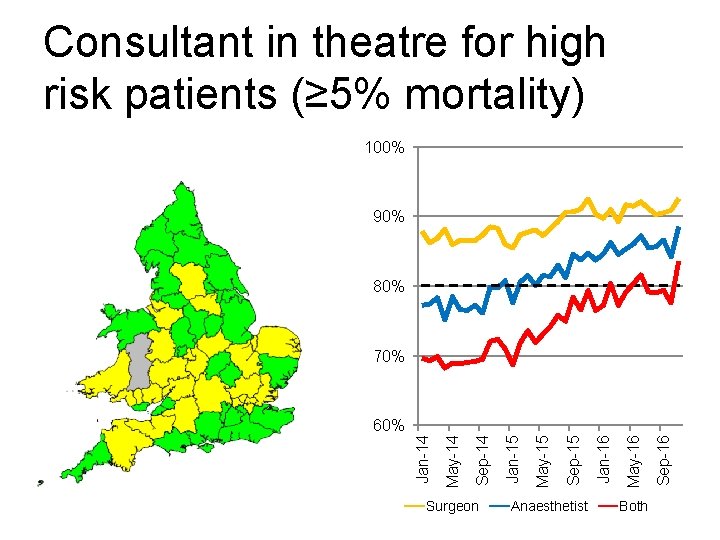
Consultant in theatre for high risk patients (≥ 5% mortality) 100% 90% 80% 70% Surgeon Anaesthetist Both Sep-16 May-16 Jan-16 Sep-15 May-15 Jan-15 Sep-14 May-14 Jan-14 60%

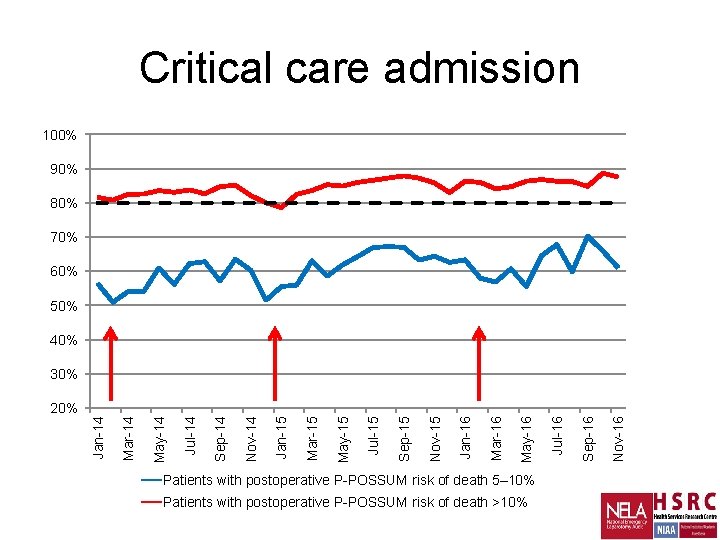
Critical care admission 100% 90% 80% 70% 60% 50% 40% 30% Patients with postoperative P-POSSUM risk of death 5– 10% Patients with postoperative P-POSSUM risk of death >10% Nov-16 Sep-16 Jul-16 May-16 Mar-16 Jan-16 Nov-15 Sep-15 Jul-15 May-15 Mar-15 Jan-15 Nov-14 Sep-14 Jul-14 May-14 Mar-14 Jan-14 20%

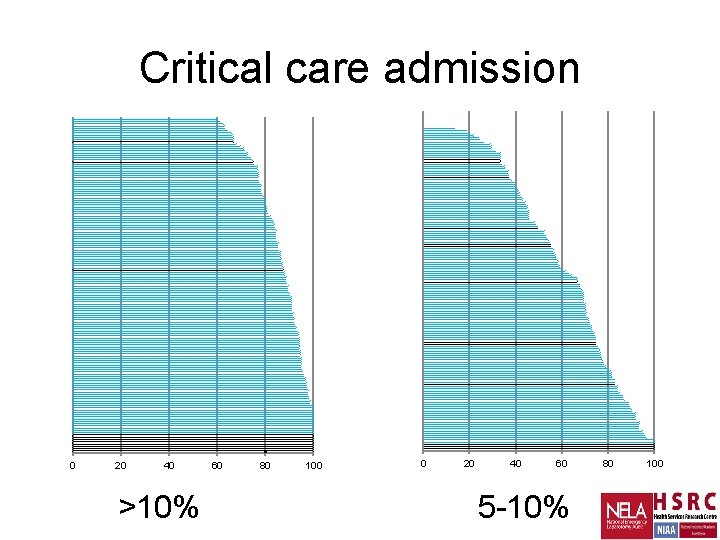
Critical care admission 0 20 40 >10% 60 80 100 0 20 40 60 5 -10% 80 100

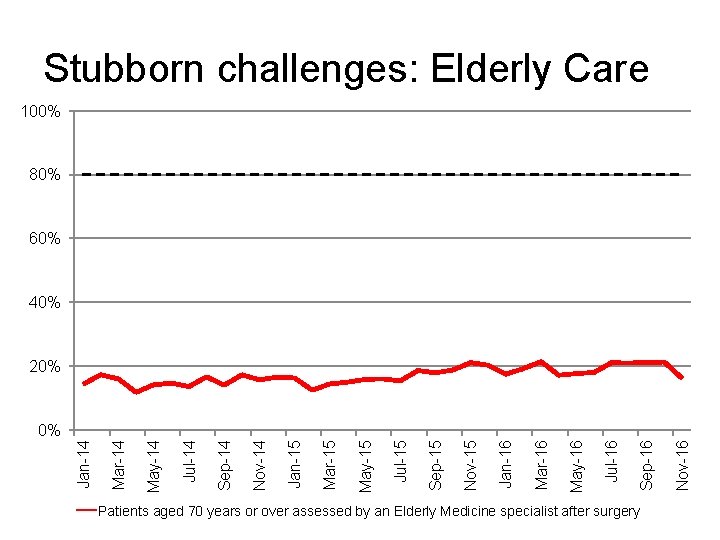
Stubborn challenges: Elderly Care 100% 80% 60% 40% 20% Patients aged 70 years or over assessed by an Elderly Medicine specialist after surgery Nov-16 Sep-16 Jul-16 May-16 Mar-16 Jan-16 Nov-15 Sep-15 Jul-15 May-15 Mar-15 Jan-15 Nov-14 Sep-14 Jul-14 May-14 Mar-14 Jan-14 0%

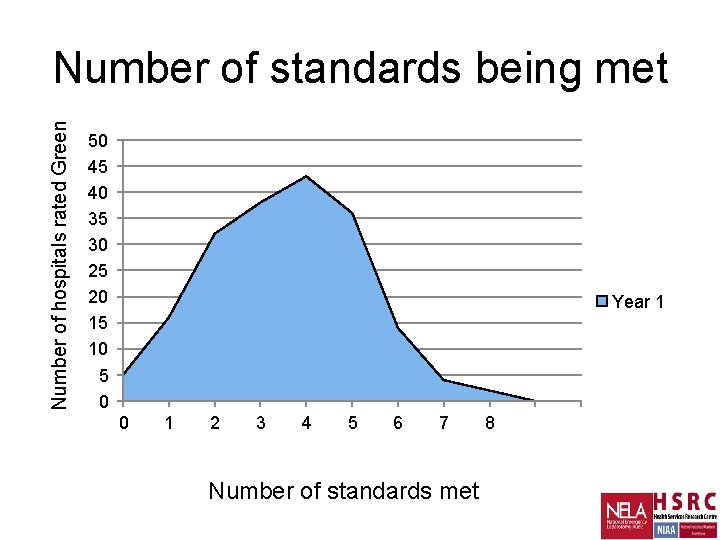
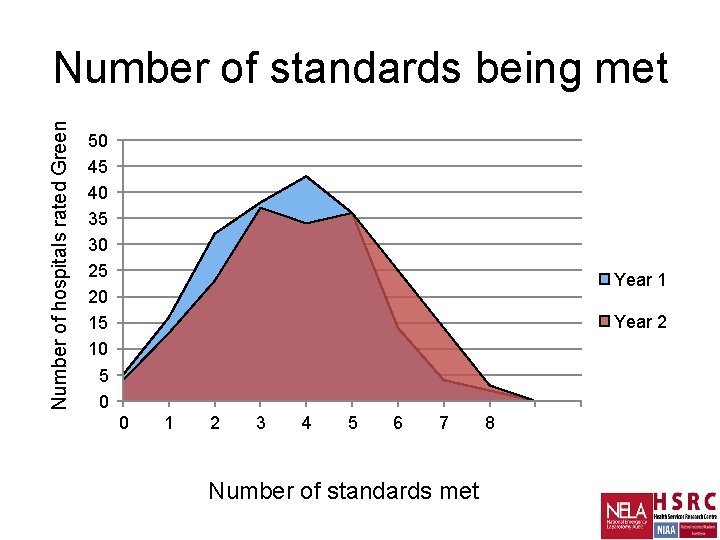
Number of hospitals rated Green Number of standards being met 50 45 40 35 30 25 20 15 10 5 0 Year 1 0 1 2 3 4 5 6 7 Number of standards met 8

Number of hospitals rated Green Number of standards being met 50 45 40 35 30 25 20 15 10 5 0 Year 1 Year 2 0 1 2 3 4 5 6 7 Number of standards met 8

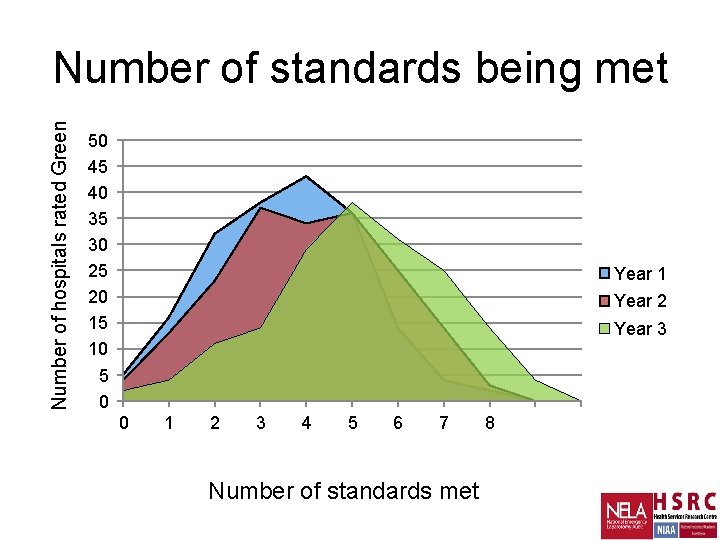
Number of hospitals rated Green Number of standards being met 50 45 40 35 30 25 20 15 10 5 0 Year 1 Year 2 Year 3 0 1 2 3 4 5 6 7 Number of standards met 8

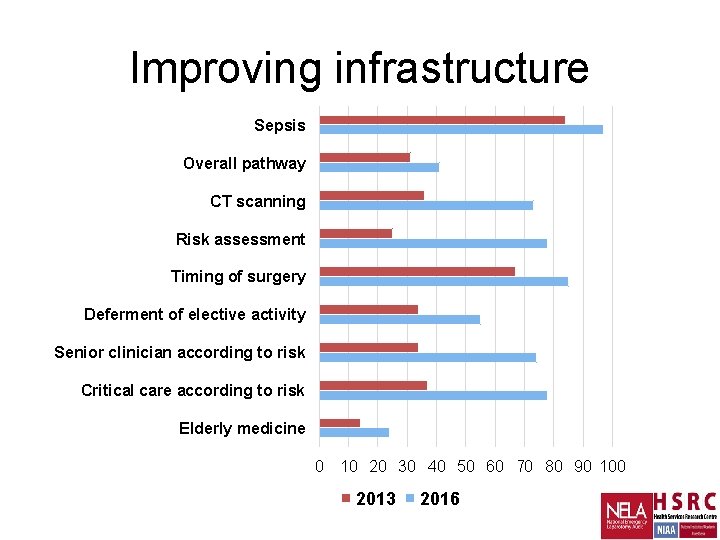
Improving infrastructure Sepsis Overall pathway CT scanning Risk assessment Timing of surgery Deferment of elective activity Senior clinician according to risk Critical care according to risk Elderly medicine 0 10 20 30 40 50 60 70 80 90 100 2013 2016

Outcomes

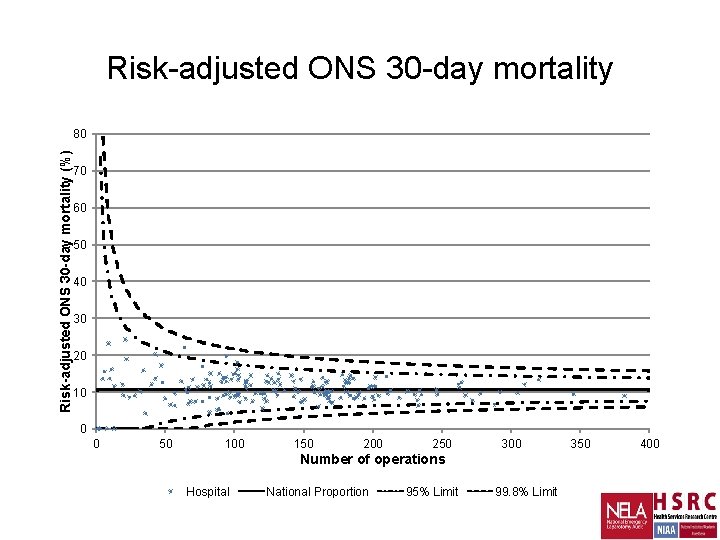
Risk-adjusted ONS 30 -day mortality (%) 80 70 60 50 40 30 20 10 0 0 50 100 150 200 250 300 Number of operations Hospital National Proportion 95% Limit 99. 8% Limit 350 400

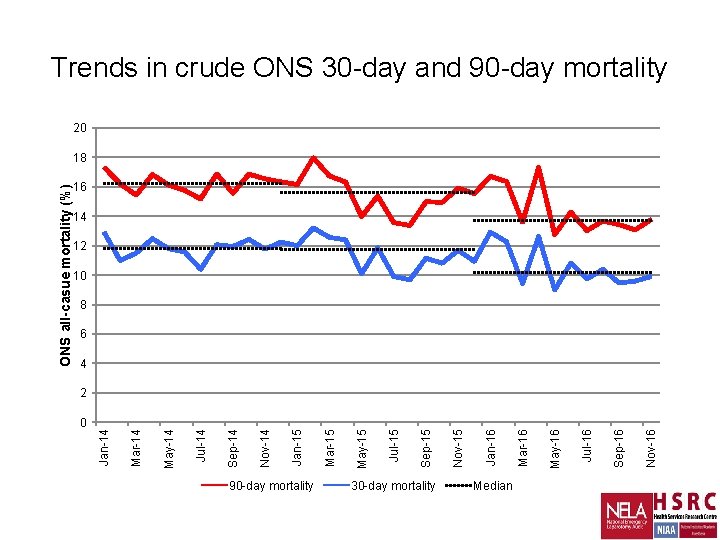
0 90 -day mortality 30 -day mortality Median Nov-16 Sep-16 Jul-16 May-16 Mar-16 Jan-16 Nov-15 Sep-15 Jul-15 May-15 Mar-15 Jan-15 Nov-14 Sep-14 Jul-14 May-14 Mar-14 Jan-14 ONS all-casue mortality (%) Trends in crude ONS 30 -day and 90 -day mortality 20 18 16 14 12 10 8 6 4 2

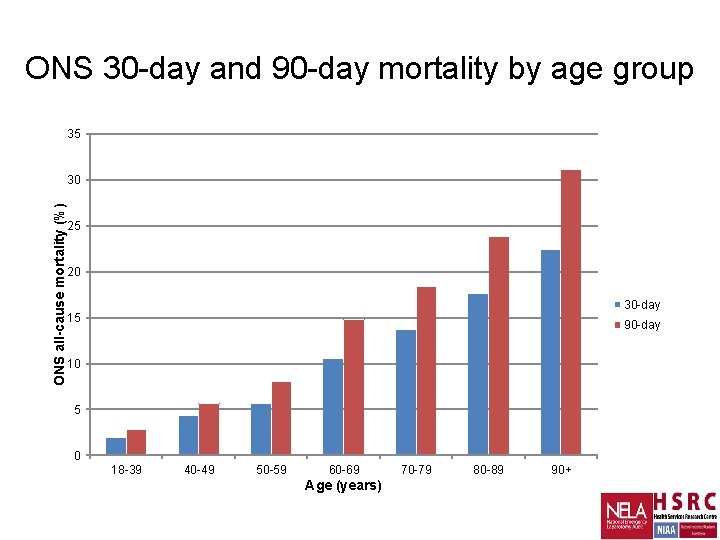
ONS 30 -day and 90 -day mortality by age group 35 ONS all-cause mortality (%) 30 25 20 30 -day 15 90 -day 10 5 0 18 -39 40 -49 50 -59 60 -69 Age (years) 70 -79 80 -89 90+

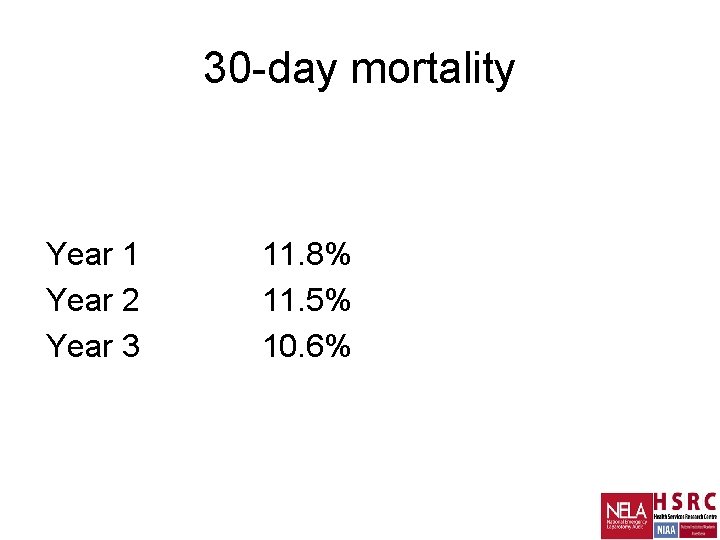
30 -day mortality Year 1 Year 2 Year 3 11. 8% 11. 5% 10. 6%

30 -day mortality Year 1 Year 2 Year 3 11. 8% 11. 5% 10. 6%

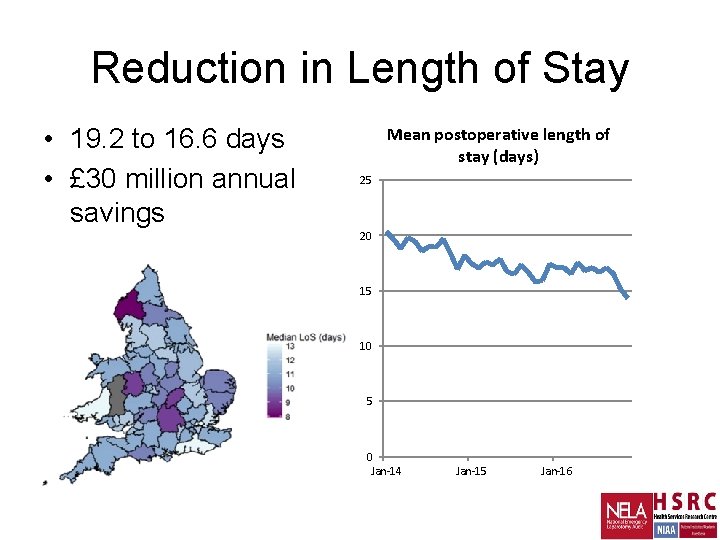
Reduction in Length of Stay • 19. 2 to 16. 6 days • £ 30 million annual savings Mean postoperative length of stay (days) 25 20 15 10 5 0 Jan-14 Jan-15 Jan-16

Going forwards… • Greater emphasis on QI • More frequent public reporting • RAG rating boundaries will increase • Mandatory and discretionary measures • Best Practice Tariff

What next for NELA/NELQIP? • Greater emphasis on QI • Targeted /themed reporting, eg commissioners • Secondary research • Parsimonious risk model

The Problem With Audit Data

The Problem With Audit Data Local QI

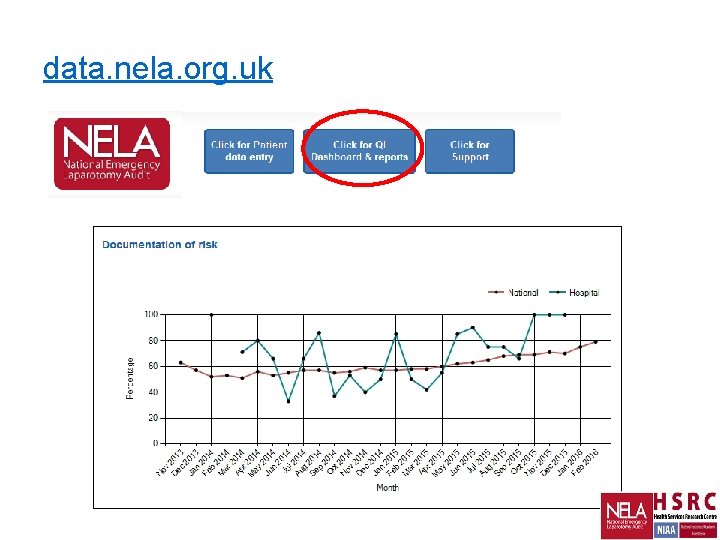
data. nela. org. uk

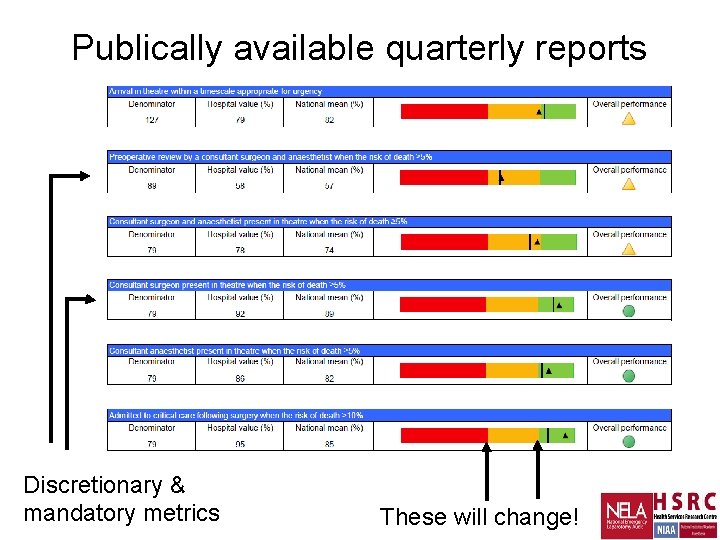
Publically available quarterly reports Discretionary & mandatory metrics These will change!

Best Practice Tariff • • Consultant presence? Theatre on time? Critical care? Elderly care?

Research… www. epochtrial. org www. floela. org

Ongoing projects • NELA Surgical sub-speciality analysis Perforated peptic ulcer (AUGIS) Subtotal colectomy for colitis (ACPGBI) Bowel Obstruction (ASGBI) Hartmann’s (ACPGBI) Bowel Cancer (ACPGBI) • NELA Risk Tool Replace / augment P-POSSUM

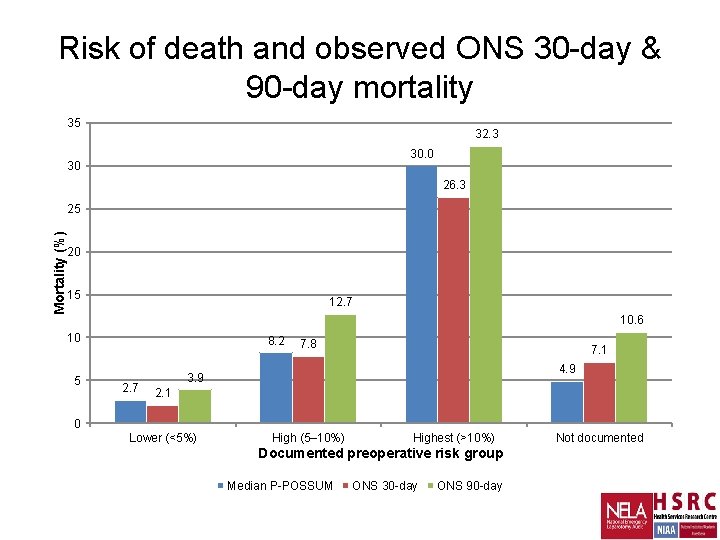
Risk of death and observed ONS 30 -day & 90 -day mortality 35 32. 3 30. 0 30 26. 3 Mortality (%) 25 20 15 12. 7 10. 6 10 5 8. 2 2. 7 7. 8 7. 1 4. 9 3. 9 2. 1 0 Lower (<5%) High (5– 10%) Highest (>10%) Documented preoperative risk group Median P-POSSUM ONS 30 -day ONS 90 -day Not documented

l a e t y l S s s e l e m a h S 38

Summary • Thank you for: 75, 000+ patients Improvement seen at personal level • Risk Assessment drives resources • Need organisational change • Not “National Audit”, but local Quality Improvement