Neonatal Necrotizing Enterocolitis NEC Nelson Textbook of Pediatrics

Neonatal Necrotizing Enterocolitis (NEC) Nelson Textbook of Pediatrics, 18 th editon By: S. M. A Shahkarami, MD Resident of Pediatrics Isfahan University of Medical Sciences

GENERAL CONSIDERATIONS 10/6/2020 By: S. M. A Shahkarami, MD 2

l NEC is the most common life-threatening emergency of the gastrointestinal tract in the newborn period. l Mucosal or transmural necrosis of the intestine. l The cause of NEC remains unclear (multifactorial). l The incidence of NEC is 1– 5% of infants in NICU l Both incidence and case fatality rates increase with decreasing birthweight and gestational age. 10/6/2020 By: S. M. A Shahkarami, MD 3

10/6/2020 By: S. M. A Shahkarami, MD 4

PATHOLOGY AND PATHOGENESIS 10/6/2020 By: S. M. A Shahkarami, MD 5

l Development of a necrotic segment of intestine, l Gas accumulation in the submucosa of the bowel wall (pneumatosis intestinalis) l Progression of the necrosis to perforation, peritonitis, sepsis, and death l The distal part of the ileum and the proximal segment of colon are involved most frequently 10/6/2020 By: S. M. A Shahkarami, MD 6

l This triad has classically been linked to NEC: intestinal ischemia (injury), enteral nutrition (metabolic substrate), and pathogenic organisms 10/6/2020 By: S. M. A Shahkarami, MD 7

The greatest risk factor for NEC is prematurity. 10/6/2020 By: S. M. A Shahkarami, MD 8

S. M. A Shahkarami, MD 9

l Coagulation necrosis is the characteristic histologic finding of intestinal specimens. l Various bacterial and viral agents, including Escherichia coli, Klebsiella, Clostridium perfringens, Staphylococcus epidermidis, and rotavirus, have been recovered from cultures. Nonetheless, in most situations, no pathogen is identified 10/6/2020 By: S. M. A Shahkarami, MD 10

l NEC rarely occurs before the initiation of enteral feeding and is much less common in infants fed human milk. Aggressive enteral feeding may predispose to the development of NEC. 10/6/2020 By: S. M. A Shahkarami, MD 11


CLINICAL MANIFESTATIONS 10/6/2020 By: S. M. A Shahkarami, MD 13
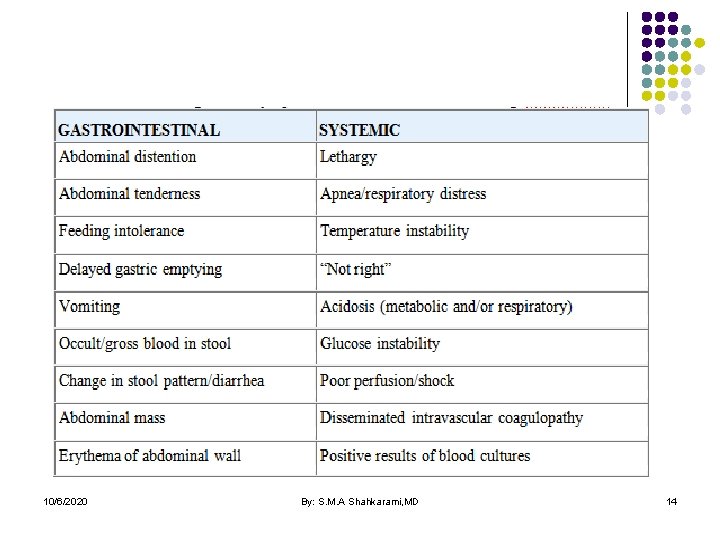
10/6/2020 By: S. M. A Shahkarami, MD 14

l The onset of NEC usually occurs in the 1 st 2 wk of life but can be as late as 3 mo of age in VLBW infants. l Age of onset is inversely related to gestational age. l The 1 st signs of impending disease may be nonspecific including lethargy and temperature instability or related to gastrointestinal pathology such as abdominal distention and gastric retention. l Obvious bloody stools are seen in 25% of patients. l Because of nonspecific signs, sepsis may be suspected before NEC. 10/6/2020 By: S. M. A Shahkarami, MD 15

l The spectrum of illness is broad and ranges from mild disease with only guaiac-positive stools to severe illness with bowel perforation, peritonitis, systemic inflammatory response syndrome, shock, and death. Progression may be rapid but it is unusual for the disease to progress from mild to severe after 72 hr 10/6/2020 By: S. M. A Shahkarami, MD 16

S. M. A Shahkarami, MD 17

DIAGNOSIS 10/6/2020 By: S. M. A Shahkarami, MD 18

Plain abdominal x-rays are essential to make a diagnosis of NEC l l pneumatosis intestinalis (air in the bowel wall) confirms the clinical suspicion of NEC and is diagnostic Portal venous gas is a sign of severe disease, and pneumoperitoneum indicates a perforation. Hepatic ultrasonography may detect portal venous gas despite normal abdominal roentgenograms. 10/6/2020 By: S. M. A Shahkarami, MD 19

Differential Diagnosis l l specific infections (systemic or intestinal) gastrointestinal obstruction Volvulus isolated intestinal perforation Idiopathic focal intestinal perforation can occur spontaneously Or after the early use of postnatal steroids and indomethacin. 10/6/2020 By: S. M. A Shahkarami, MD 20

10/6/2020 By: S. M. A Shahkarami, MD 21

TREATMENT 10/6/2020 By: S. M. A Shahkarami, MD 22

Rapid initiation of therapy is required for suspected as well as proven NEC No definitive treatment , therefore, therapy is directed at supportive care: l cessation of feeding, nasogastric decompression, and administration of intravenous fluids. l Careful attention to respiratory status, l Ventilation should be assisted in the presence of apnea or if abdominal distention is contributing to hypoxia and hypercapnia. l coagulation profile, l acid-base and electrolyte balance l systemic antibiotics (with broad coverage based on the antibiotic sensitivity patterns of the gram-positive, gram-negative, and anaerobic organisms) should be started immediately. l If present, umbilical catheters should be removed 10/6/2020 By: S. M. A Shahkarami, MD 23

Close Monitoring l frequent physical assessments l sequential anteroposterior and cross-table lateral or lateral decubitus abdominal x-rays to detect intestinal perforation l and serial determination of hematologic, electrolyte, and acid-base status l Gown and glove isolation l and grouping infants from other infants to contain an epidemic. 10/6/2020 By: S. M. A Shahkarami, MD 24

S. M. A Shahkarami, MD 25

l A surgeon should be consulted early Indications for surgery: l evidence of perforation on abdominal X-rays: (pneumoperitoneum) l positive abdominal paracentesis (stool or organism on Gram stain from peritoneal fluid). Relative indications for exploratory laparotomy: l a single fixed bowel loop on roentgenograms, abdominal wall erythema, or a palpable mass Ideally, surgery should be performed after intestinal necrosis develops, but before perforation and peritonitis occurs. 10/6/2020 By: S. M. A Shahkarami, MD 26

l The role of peritoneal drainage in lieu of laparotomy in a patient with perforation secondary to NEC remains to be determined l more successful in patients with isolated intestinal perforation l In many patients with isolated intestinal perforation treated by drainage, no further surgical procedure is needed 10/6/2020 By: S. M. A Shahkarami, MD 27

10/6/2020 By: S. M. A Shahkarami, MD 28
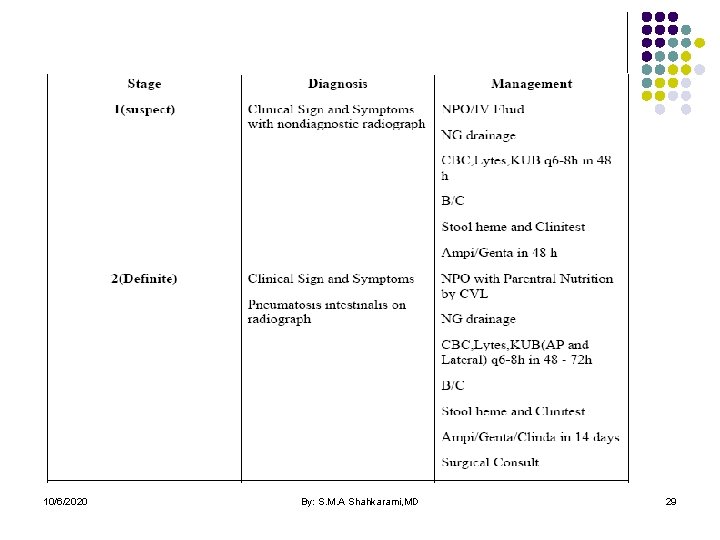
10/6/2020 By: S. M. A Shahkarami, MD 29
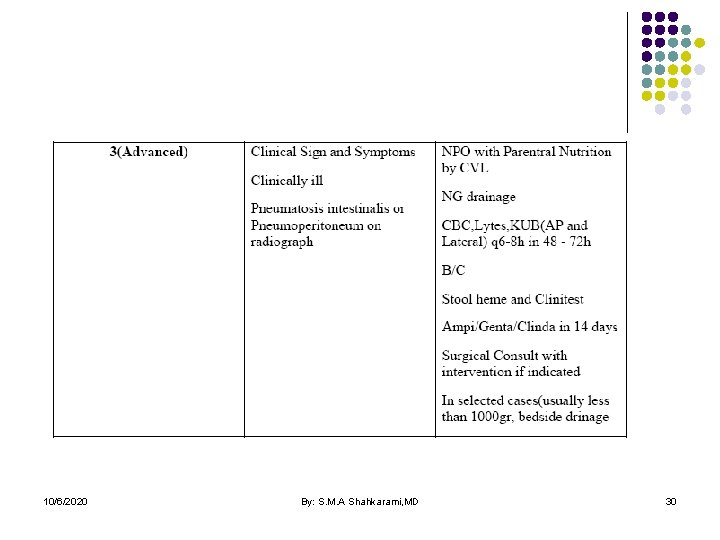
10/6/2020 By: S. M. A Shahkarami, MD 30

PROGNOSIS 10/6/2020 By: S. M. A Shahkarami, MD 31

l Medical management fails in about 20– 40% of patients with pneumatosis intestinalis at diagnosis; of these, 10– 30% die. l Early postoperative complications include wound infection, dehiscence, and stomal problems (prolapse, necrosis). Later complications: l intestinal strictures that develop at the site of the necrotizing lesion in about 10% of surgically or medically managed patients. l After massive intestinal resection, complications from postoperative NEC include short-bowel syndrome (malabsorption, growth failure, malnutrition), l complications related to central venous catheters (sepsis, thrombosis), and cholestatic jaundice. 10/6/2020 By: S. M. A Shahkarami, MD 32

10/6/2020 By: S. M. A Shahkarami, MD 33

PREVENTION 10/6/2020 By: S. M. A Shahkarami, MD 34

l Newborns exclusively breast-fed have a reduced risk of NEC l Whereas early initiation of aggressive feeding protocols may increase the risk of NEC in VLBW infants l gut stimulation protocol of minimal enteral feeds followed by judicious volume advancement may decrease l ↓ the risk Probiotic preparations have also decreased the incidence of NEC. 10/6/2020 By: S. M. A Shahkarami, MD 35

10/6/2020 By: S. M. A Shahkarami, MD 36

HIGHLY TRULY YOURS & WARM REGARDS S. M. A Shahkarami, MD 10/6/2020 By: S. M. A Shahkarami, MD 37
- Slides: 37