Micahs Mystery A Case of Seizures in a




























- Slides: 36

Micah’s Mystery: A Case of Seizures in a Golden Retriever Ashley D. Justice

Meet Micah • 11 year old intact male Golden Retriever • Agility Champion • Presented to Auburn’s neurology service on 8/18/09 due to recent onset of seizure activity.

History • No previous history of seizures • No other medical conditions other than hypothyroidism. • First seizure activity on 6/13/09 • Transported to emergency clinic • Micah was placed on phenobarbital (63. 8 mg tablet BID)

History cont. • Micah was weaned off of the medication, then suffered another seizure a week later (8/9/09). • Controlled with rectal diazepam • Micah was placed back on the phenobarb • r. DVM tested for E. canis, Lyme disease, RMSF

Physical Examination • Bright, Alert, Responsive • Temperature, pulse, and respirations were all within normal limits. • No significant abnormalities found

Neurologic Examination • Mental status: normal • Gait and Posture: normal with the exception of a slightly abnormal rear limb gait • Slight, intermittent right head tilt was present, otherwise, all cranial nerves WNL • Spinal reflexes: WNL • Postural reactions: WNL

Seizures • Definition: the clinical manifestation of an excessive discharge of hyperexcitable cerebrocortical neurons. • Generalized, simple partial, or complex partial • Brief/isolated vs. Cluster • Micah: generalized

Pathophysiology • Imbalance between normal excitability and inhibitory mechanisms due to an intra or extra cranial disease process.

Seizure Classification • Primary epileptic seizures – 44%- no identifiable cause of seizure activity – Large breed dogs – 1 -5 yrs. (most initial episodes are from 6 mo. -3 yrs) – Longer inter-ictal period (>4 wks) – Generalized motor seizures – Considered familial or inherited

Seizure Classification • Secondary epileptic seizures – 46% - animal has an identifiable intracranial abnormality – Bimodal onset- <1 yr. or >7 yr. – Partial seizures included – First seizure is usually between midnight and 8 am. – Many etiologies

Seizure Classification • Reactive epileptic seizures – 10% – Metabolic, toxic, or other noxious insult capable of inducing seizures. – Most likely when inter-ictal period is <4 wks. – Most involve organ or endocrine disease. – All ages – Many etiologies

Initial Treatment • When to treat – >1 seizure in a 24 hour period – >1 seizure every 6 weeks – History of status or clusters – Judgement call • Goal: to reduce the seizure frequency to less than one single seizure every 6 -8 weeks ASAP. • Potassium Bromide and Phenobarbital are the most common treatment options.

KBr vs. Phenobarb • KBr - • Dosage: 40 -50 mg/kg q 24 (lower dose when used as an adjunct) • Contraindication: renal insufficiency • Ensure stable dietary chloride intake • Side effects: ataxia, lethargy, PU/PD • Phenobarb - • Dosage: 2. 5 -4 mg/kg q 12 – If seizures are occurring at intervals of less than 7 days, initiate PB therapy with an IV loading dose of 15 -25 mg/kg. – Measure levels in 2 wks. (target level is 20 -45 mcg/ml) • Contraindication: liver disease

Other considerations • Only if no seizures have occurred in 6 -12 months, consider slowly weaning over a period of a few months. • Do not administer drugs that interfere with the metabolism of PB: – Chloramphenicol, cimetidine, ranitidine, and tetracyclines. • Do not administer drugs which may lower the seizure threshold: – Ace, xylazine, ketamine, estrogens, tricyclic antidepressants, bronchodilators.

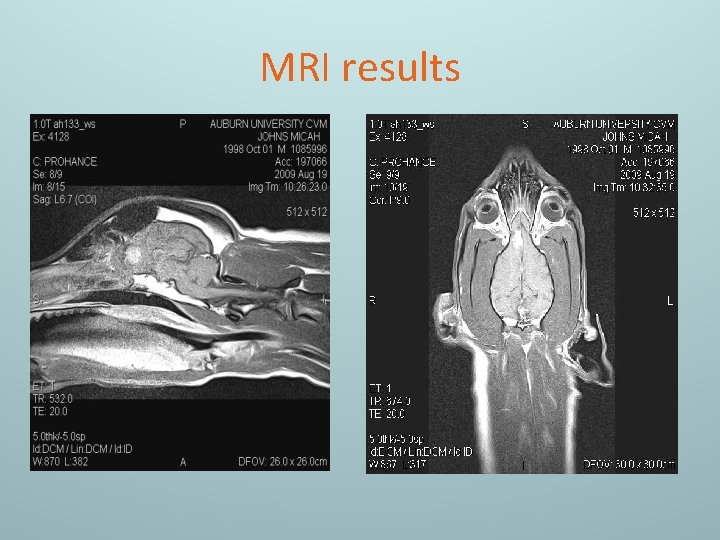
Initial Diagnostics • CBC, Serum chemistries, Urinalysis- no significant abnormalities. • 3 view thoracic radiographs- WNL • Titers for RMSF, E. canis, Neospora, Distemper, Toxoplasma- RMSF again mildly elevated, but likely represents previous exposure or exposure to a non-pathogenic strain. Distemper borderline increased, but probably not clinically significant. • Brain MRI

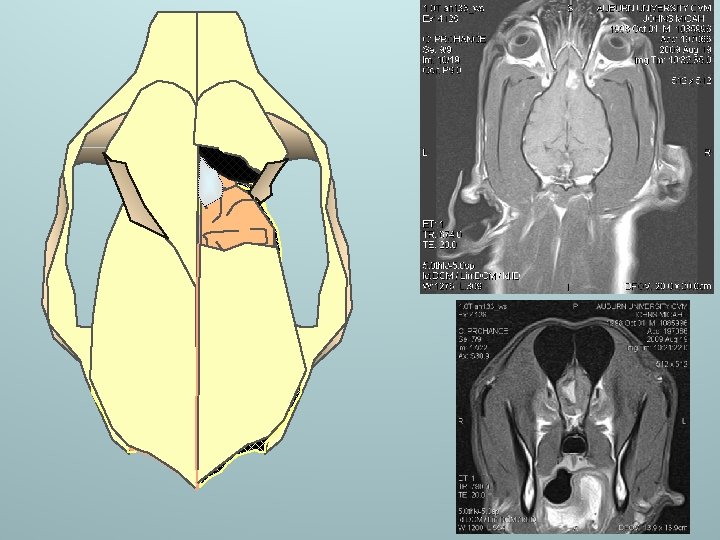
MRI results

2 7/14 4 12

Intracranial Tumors • Seizures could be the result of expansile growth or peri-tumoral effects (edema, compromised blood flow) • Rarely disseminate throughout the CNS by hematogenous or CSF routes. • Incidence: 14. 5 in 100, 000

Types of Intracranial Tumors • • • Astrocytic tumors Oligodendroglial tumors Ependymal cell tumors Mixed gliomas Tumors of the Meninges

Treatment Plan • Continue with the current drug regimen (phenobarb, saloxine) • Discharge (8/19/09) to return on 8/25/09 for brain surgery.

8/25/09 • Micah returns to Auburn for brain surgery • Bright, alert, and responsive with no seizure activity noted by owner.

Surgical Considerations • Intracranial pressure dynamics is the most important consideration for the patient prior to performing a craniotomy. • Monroe-Kellie Doctrine: the contents of the cranial vault are blood, CSF, and parenchymaan increase in any of these 3 results in a net decrease in the other 2 components.

Surgical Considerations (cont. ) • Pre-operative steroid administration – Dexamethasone: to reduce edema and CSF production – Sodium prednisolone succinate or methyl prednisolone succinate- antiinflammatory and tissue protective as oxygen free radical scavengers and stabilizers of the lysosomal membranes. – Micah: solu-delta cortef • Prophylactic antibiotic usage – To decrease CNS bacterial contamination – Micah: cefazolin

Craniectomy • Sternal recumbency • Transfrontal approach






Post-operative • Critical care • Monitoring: – – Check heart rate, respirations, and blood pressure every two hours. Flip sides every four hours, as well as ice pack incision every 4 hours. NPO LRS- 70 ml/hr • Medications: – – – – Cefazolin Lasix Buprenorphine Phenobarb Levothyroxine Midazolam Domitor Famotidine

Post-operative • Walked outside with assistance day 1 • NPO • Began offering food on day 2 and switched to oral antibiotic and pain control • Spiked a fever on day 3 but was controlled easily, received surgical histopathology results • Gradually increased food intake and walking distance

Meningioma • Most frequent CNS tumor seen in vet med • MST – Surgical excision followed by radiation therapy- 16 mo. – Surgical excision alone- 11 mo. – No treatment- variable – could be weeks to months. • • Breed predilection: dolicocephalic Age predilection: mature adults Behavior- generally benign Location: usually solitary – Cerebrum> cerebellum> spinal cord>ventricles

August 30, 2009 - Micah goes home!

Recheck-9/14/09 • BAR, incision healing nicely • Neurologic examination- inconsistent right eye menace response and droopy right eyelid • Owner reported Micah to be weak in his rear limbs • Pretreatment CT for radiation therapy

10/2/09 • Micah is receiving his 13 th of 16 fractions of radiation today. • He is doing great with no abnormalities thus far!

Thank You…. . • God • Family • Micah • Dr. Ortinau and Dr. Shores • Class of 2010 • Gran 1932 -2009 Phil. 4: 13 - “I can do all things through Christ who gives me strength. ”