10 SIGNS OF VITALITY Recognizing Earlier Patients AtRisk



































- Slides: 49

10 SIGNS OF VITALITY Recognizing Earlier Patients At-Risk MERCY MEDICAL CENTER REDDING MAY 2016 Frank Sebat, MS, MD FCCP, FCCM Director, KRITIKUS FOUNDATION

CLASSIC VITAL SIGNS 1. Temperature 2. Pulse 3. Color / Blood pressure 4. Respirations 5. Pain – the fifth vital sign (American Pain Society 1995) Florence Nightingale 1820 -1910 2

EXPANDED ASSESSMENT 6. LOC 7. O 2 sat 8. Urine output 9. Capillary refill 10. Temp <36°, ↑ BD or LA, ↓ Scv. O 2 / Sv. O 2 or (often reflect global tissue hypoperfusion) ALL TOGETHER REPRESENT THE 10 SOV

4 STa. RRS : Early Detection of At-Risk Patients 10 SIGNS OF VITALITY TOOL A QUICK and ACCURATE HEAD TO TOE PATIENT Back to last question ASSESSMENT 6/23/14

10 SOV FOR RECOGNIZING AT-RISK PATIENTS 5

DO WE RECOGNIZE CRITICAL ILLNESS EARLY? Research Supports: • Early warning signs - often missed • A, B, C’s of resuscitation are often suboptimal prior to transfer to higher level of care

SCENARIO #1: AN EXAMPLE OF MISSED OPPERTUNITY 32 y. o. female in good health prior • Calls 911 because of lightheadness with Hx of MVR • EMT notes - anxious, cool extremities, poor CAP refill, RR 22, SBP=80 by palpation • EMT notifies ED – patient at-risk by criteria, 1000 cc NS IV – • In ED- pt. sitting up in bed: alert / anxious, SBP 110, RR 22, CAP refill 4 seconds

SCENARIO #1 (cont. ) ED PHYSICIAN, AND INTENSIVIST EXAMINE PATIENT: • RRT alert canceled • Admitted to floor by 1°MD w/dx of mild hypovolemia • At 2 am, code blue • In ED lactic acid = 7 • Platelet count 83, 000 and DIC screen pos EMT ADHERES TO PROTOCOL. . . PHYSICIANS DO NOT

SCENARIO #2: MISSED OPPORTUNITY Michael W. Donnino et al, Emanuel Rivers Henry Ford Hospital, Detroit, MI, Abstract SCCM 2004 In the ED with sepsis, Lactic Acid > 4 and normotensive, your chances of survival are: A. Less if you are hypotensive B. Greater if you are hypotensive B. Patients Normotensive Mortality 70% Control (n=23) Hypotensive Control (n=133) 46. 5%

MISSED OPPORTUNITY Scenario 3 : 10/25 - 26 y. o. female in ED with abd pain. Hx of ↑ TG, ↑ amylase / lipase, RR 24, P 106, BP 136/70, afebrile admitted to floor 10/26 - Hb 13 → 15, RR = 22, ↑ abd pain 11/1, 17: 30 - RR = 42, HR = 122, BP = 118/66 - RRT called, Cap refill is > 3 sec. agitated, use of accessory muscles. Skin cold and clammy - What is the first thing you should do ?

OPPORTUNITY FOR IMPROVEMENT Scenario 3 : • 18 : 45 Pt. coded • 4, 650 min or 3. 2 days - Time RRT was mobilized, minus the time patient at-risk by 10 SOV criteria

RAPID RESPONSE TEAM. . . THE EFFERENT ARM The RRT is the most visible component of a RRS But less important than you might think. The afferent arm is the key to early recognition and Rx. 12

1 3 The Afferent Arm- Most Important YOU ARE The bedside RN using the 10 SOV tool to recognize at-risk patients earlier 6/23/14

INCIDENCE OF UNEXPECTED CARDIAC ARRESTS OF FLOOR PATIENTS and RRTs Pre 10 sov USA: 5. 0 - 0. 25 arrest and 5 -56 RRTs per 1, 000 hospital d/c Kaweah Delta: 4. 29 arrest and 11 RRTs per 1, 000 hospital d/c (2009)

Which Patients Are At-Risk For Failure To Rescue ? 15

Neurological Deterioration PATIENTS AT-RISK FOR ACUTE Respiratory Deterioration DECOMPENSATION Hemodynamic Deterioration ALL LEAD TO SHOCK -100% MORTALITY IF UNCORRECTED

1 7 CHOC OR SHOCK HOW DO WE GET THERE? - IS IT OUR WATERLOU ? From 1560 s Middle French; choc is a violent attack, military term violent encounter of armed forces

SHOCK IS A SYNDROME OF GLOBAL INADEQUATE TISSUE OXEGENATION 1. Altered level of consciousness 2. Tachypnea, RR ≥ 20 3. Sa. O 2 < 90% 4. Cool or mottled extremities, CAP refill >3 sec 5. Hypotension, BP < 90 frequently present, but not always 6. Decreased urine output, 25 cc/hr, 300 cc/12 hr 7. Metabolic acidosis BE < -5 , LA > 2. 0 8. Hypothermia, T < 36 WHICH OF THE THREE 10 SOV ARE MISSING? 18

VITAL ORGAN HYPOPERFUSION / SHOCK LEADS TO DECREASED BLOOD FLOW TO : • Brain • Coronary arteries • Intercostal and diaphragmatic muscles - require 50% cardiac output during sever illness Leads to decreased airway protection, cardiac performance and respiratory muscle function Left Untreated Code Blue

TYPES OF SHOCK • Hypovolemic Shock, hemorrhage • Septic or Distributive Shock • Cardiogenic Shock

TYPES OF SHOCK • Obstructive Shock • Anaphylactic Shock • Hypoxic / Respiratory Shock

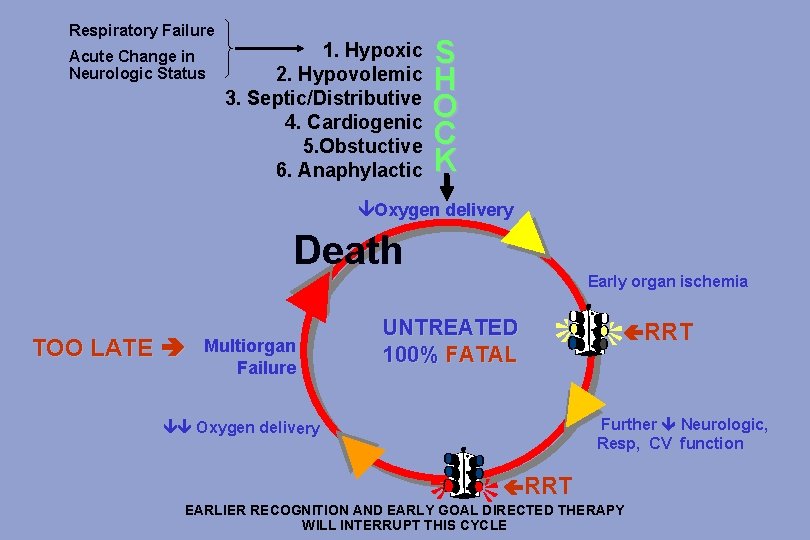
Respiratory Failure Acute Change in Neurologic Status 1. Hypoxic 2. Hypovolemic 3. Septic/Distributive 4. Cardiogenic 5. Obstuctive 6. Anaphylactic S H O C K Shock Cycle Oxygen delivery Death Early organ ischemia TOO LATE Multiorgan Failure UNTREATED 100% FATAL RRT Further Neurologic, Resp, CV function Oxygen delivery RRT EARLIER RECOGNITION AND EARLY GOAL DIRECTED THERAPY © 2011 STa. RRS Education Presentation WILL INTERRUPT THIS CYCLE

10 SOV Early Recognition Assessment & Communication Tool for At-Risk Patients - Shock

10 SOV : AT-RISK TRIGGERS FREQUENTLY SUBTLE • Tachypnea - almost always present, but nonspecific, underappreciated- lower RR trigger ≥ 20 • Hypotension - not always present or detected, double check BP by a second method • Oliguria - takes time to assess- but very important

STa. RRS : AT-RISK TRIGGERS FREQUENTLY SUBTLE • Anxiety or apathy are early signs-needs to be appreciated • CAP refill >3 sec. usually present needs to be measured

C. N. S. MANIFESTATIONS OF AT-RISK PATIENTS Anxiety Apathy Lethargy / Stupor Coma © 2011 STa. RRS Education Presentation 26

TEMPERTURE • TEMP > 38 important but unlikely to lead to sudden decompensation • TEMP < 36 often significant when combined with other 10 SOV o Liver is main organ of thermogenesis at rest o Reflects decreased blood flow to the liver o Generally the kidney will also have reduced blood flow in this setting

RESPIRATORY RATE • Tachypnea - almost always present in at-risk patients • Nonspecific • Underappreciated • Frequently charted without being measured • Lower RR trigger ≥ 20

OXYGEN SATURATION • Sa. O 2 < 90 • Coupled with one of the other 7 key 10 SOV indicates “hypoxic shock” • Hypoxia kills quickly • Hypercapnia kills slowly

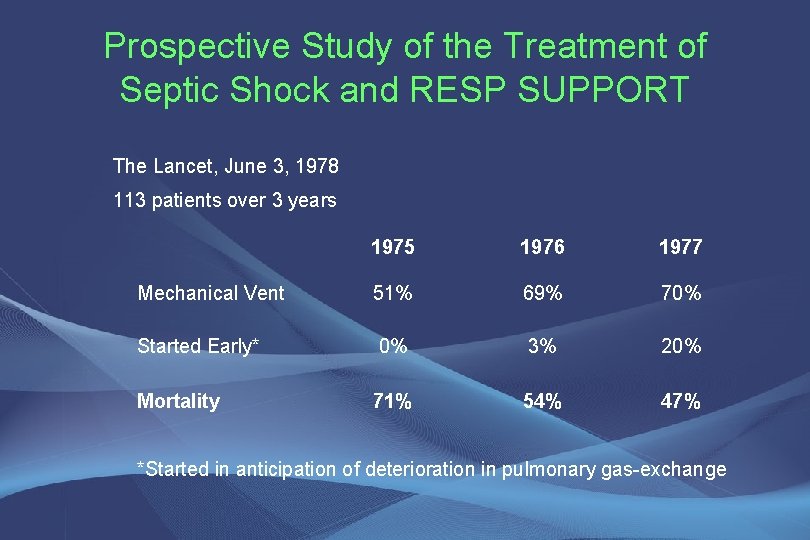
Prospective Study of the Treatment of Septic Shock and RESP SUPPORT The Lancet, June 3, 1978 113 patients over 3 years 1975 1976 1977 Mechanical Vent 51% 69% 70% Started Early* 0% 3% 20% Mortality 71% 54% 47% *Started in anticipation of deterioration in pulmonary gas-exchange

Hypotension • SBP < 90, MAP < 60 • Not always present • Frequently not detected - double check BP by a second method

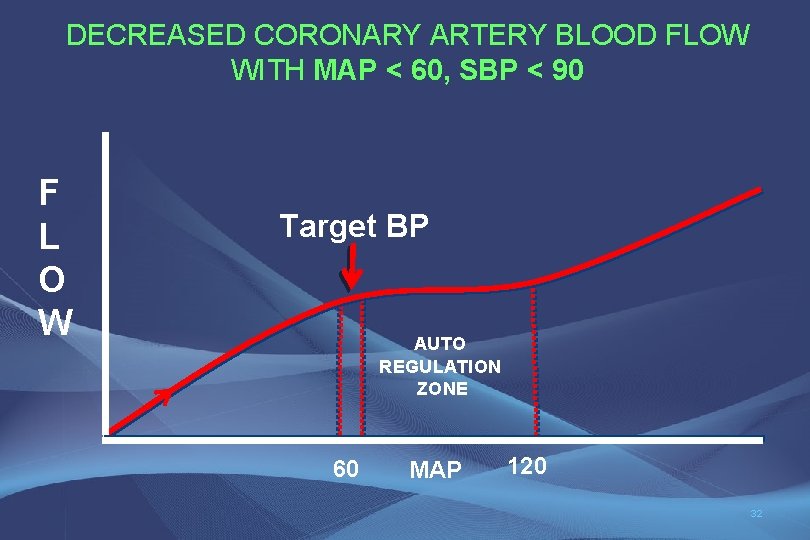
DECREASED CORONARY ARTERY BLOOD FLOW WITH MAP < 60, SBP < 90 F L O W Target BP AUTO REGULATION ZONE 60 MAP 120 32

ALLSHOCK SYNDROMES LEAD TO CARDIOGENIC SHOCK 33

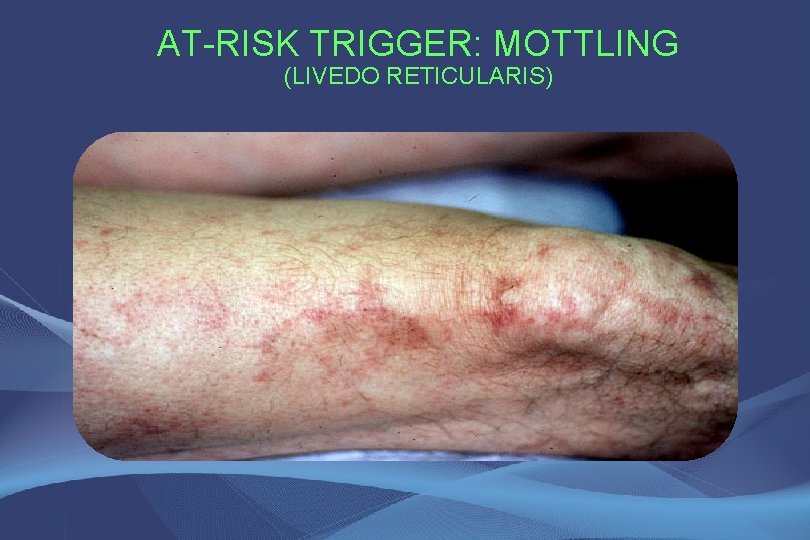
AT-RISK TRIGGER: MOTTLING (LIVEDO RETICULARIS)

CAPILLARY REFILL TIME Critical Care Medicine. 37(3): 934 -938, March 2009 Fifty consecutive adult patients admitted to the intensive care unit When cap refill > 4. 5 sec, 77% vs. 23% progressed to worsening organ function (p < 0. 05) Subjective assessment of peripheral perfusion can identify patients at-risk for more severe organ dysfunction and higher lactate levels

Capillary Refill Test > 3 Seconds 6/23/14 play Mouse over picture and click to 36

ABDOMINAL MANIFESTATIONS OF SHOCK • Oliguria • Ileus and increased liver function tests • Temperature <36°C or 96. 8°F

URINE OUTPUT • Our hour by hour window of abdominal perfusion • < 25 cc/hr or 300 cc/12 h in absence of known ARF reflect decreased kidney perfusion • Can be masked by diuretics

METABOLIC ACIDOSIS • Easy to check, • LA > 2 meg/l abn , > 4 is severe • BD > 5 (BE < -5) abn, check anion gap

The other 3 SOV • Pain, responsible for a 200% increase in resp failure – Brain trumps Pain • Fever, needs evaluation but not general associated with suden decompensation • Heart rate by itself does not reflect end organ hypoperfusion or hypoxia

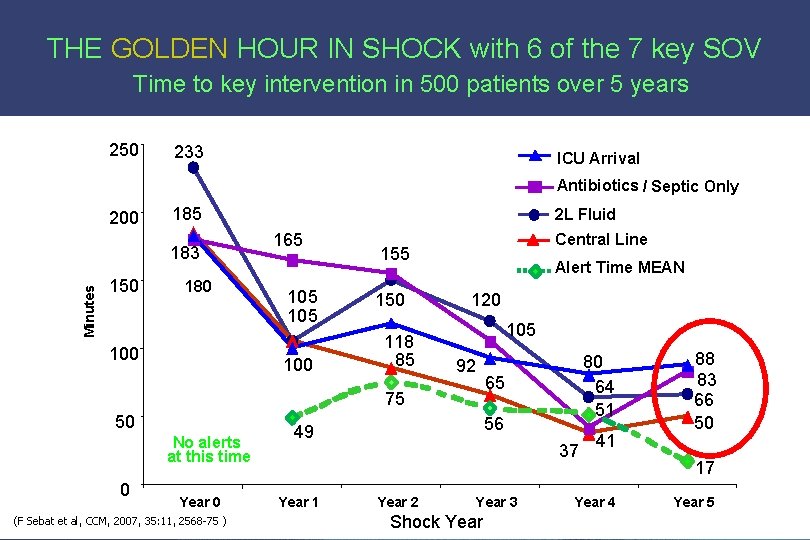
THE GOLDEN HOUR The 1 st hour after the onset of illness, which if recognized and treated results in best outcomes: • Trauma • AMI • Stroke • Shock • Other At-Risk Patients – 10 SOV

THE GOLDEN HOUR IN SHOCK with 6 of the 7 key SOV Time to key intervention in 500 patients over 5 years 250 233 ICU Arrival Antibiotics / Septic Only 200 Minutes 183 150 185 180 100 2 L Fluid 165 105 100 Central Line 155 150 118 85 Alert Time MEAN 120 105 92 75 50 No alerts at this time 0 Year 0 (F Sebat et al, CCM, 2007, 35: 11, 2568 -75 ) 65 56 49 Year 1 80 64 51 37 Year 2 Year 3 Shock Year 41 Year 4 88 83 66 50 17 Year 5

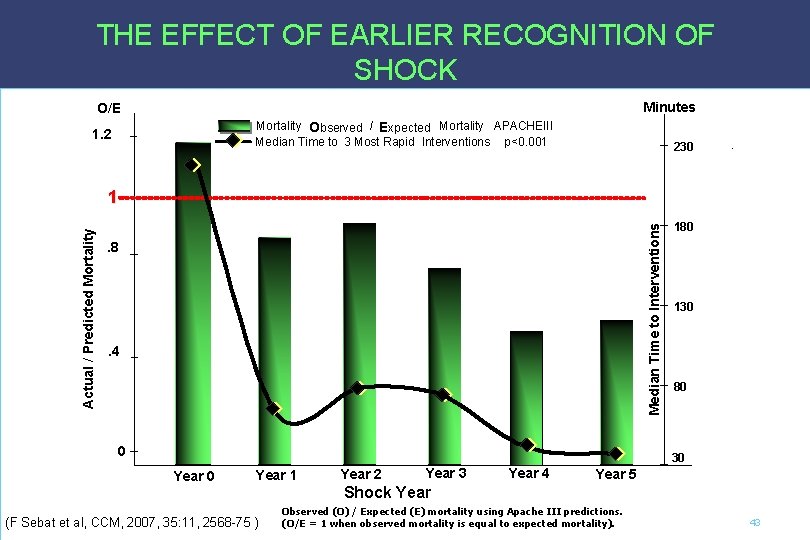
THE EFFECT OF EARLIER RECOGNITION OF SHOCK O/E Mortality Observed / Expected Mortality APACHEIII Median Time to 3 Most Rapid Interventions p<0. 001 1. 2 Minutes 230 . . 8 . 4 0 Year 0 Year 1 (F Sebat et al, CCM, 2007, 35: 11, 2568 -75 ) 130 80 30 Year 2 180 Median Time to Interventions Actual / Predicted Mortality 1 Year 3 Year 4 Year 5 Shock Year Observed (O) / Expected (E) mortality using Apache III predictions. (O/E = 1 when observed mortality is equal to expected mortality). 43

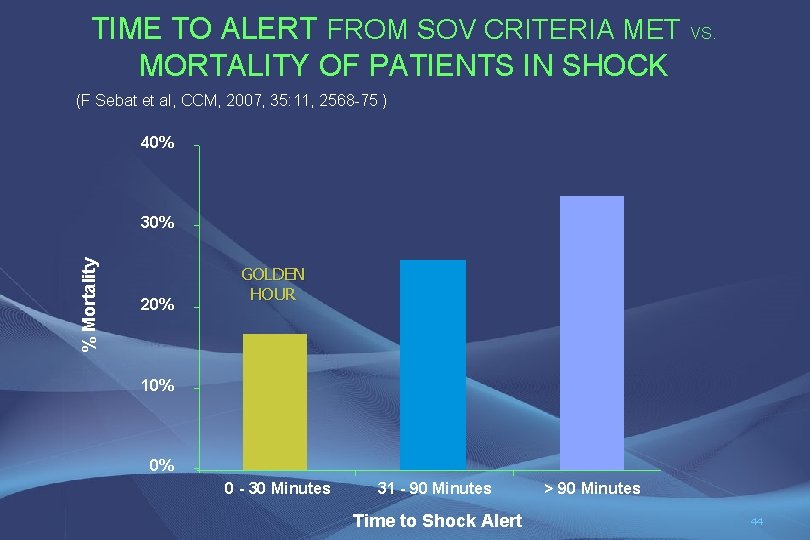
TIME TO ALERT FROM SOV CRITERIA MET VS. MORTALITY OF PATIENTS IN SHOCK (F Sebat et al, CCM, 2007, 35: 11, 2568 -75 ) 40% % Mortality 30% 20% GOLDEN HOUR 10% 0% 0 - 30 Minutes 31 - 90 Minutes Time to Shock Alert > 90 Minutes 44

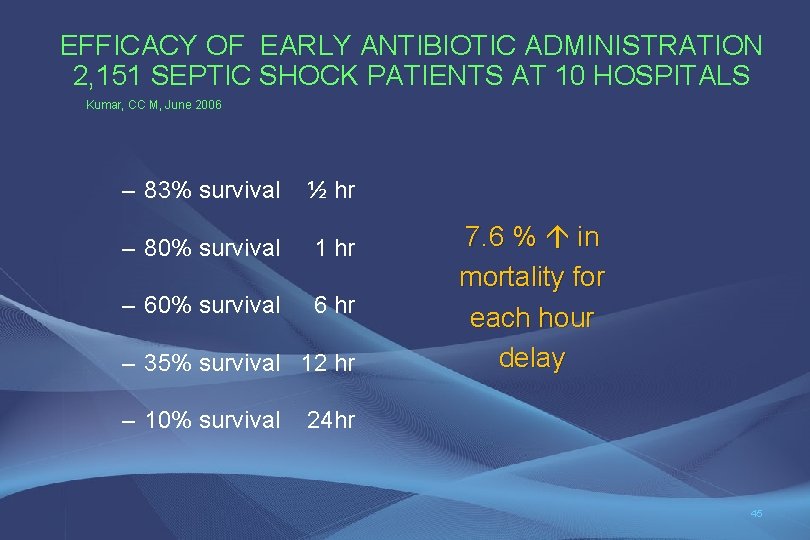
EFFICACY OF EARLY ANTIBIOTIC ADMINISTRATION 2, 151 SEPTIC SHOCK PATIENTS AT 10 HOSPITALS Kumar, CC M, June 2006 – 83% survival ½ hr – 80% survival 1 hr – 60% survival 6 hr – 35% survival 12 hr – 10% survival 7. 6 % in mortality for each hour delay 24 hr 45

STa. RRS ACTIVATION BADGE FOR STAFF FRONT BACK

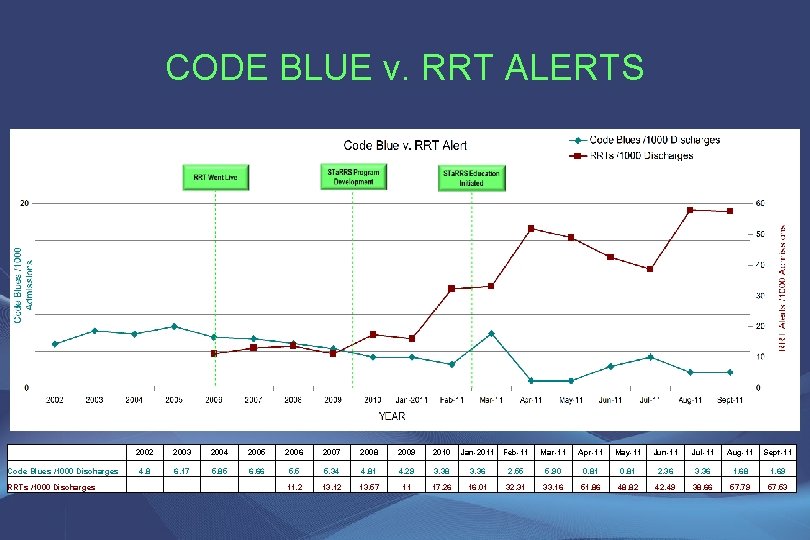
CODE BLUE v. RRT ALERTS Code Blues /1000 Discharges RRTs /1000 Discharges 2002 2003 2004 2005 2006 2007 2008 2009 2010 Jan-2011 Feb-11 Mar-11 Apr-11 May-11 Jun-11 Jul-11 Aug-11 Sept-11 4. 8 6. 17 5. 85 6. 66 5. 5 5. 34 4. 81 4. 29 3. 38 3. 36 2. 55 5. 90 0. 81 2. 36 3. 36 1. 68 1. 69 11. 2 13. 12 13. 57 11 17. 26 16. 01 32. 31 33. 16 51. 86 48. 82 42. 49 38. 66 57. 79 57. 53

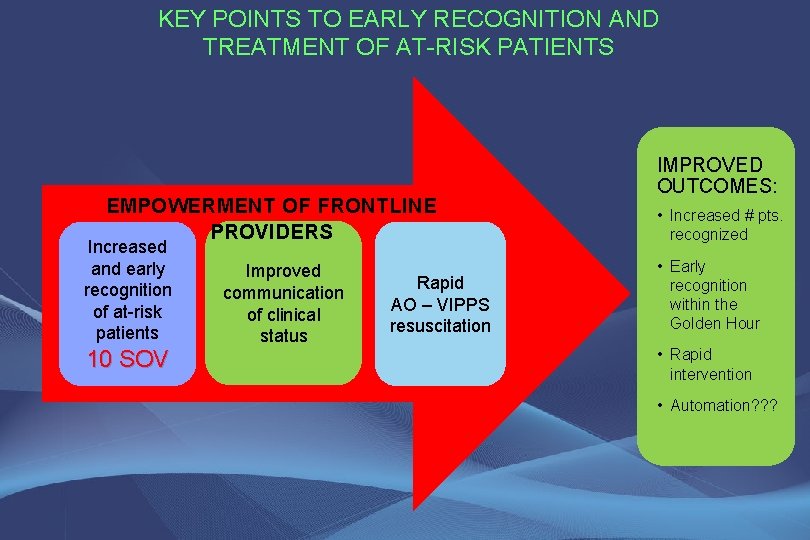
KEY POINTS TO EARLY RECOGNITION AND TREATMENT OF AT-RISK PATIENTS EMPOWERMENT OF FRONTLINE PROVIDERS Increased and early recognition of at-risk patients 10 SOV Improved communication of clinical status Rapid AO – VIPPS resuscitation IMPROVED OUTCOMES: • Increased # pts. recognized • Early recognition within the Golden Hour • Rapid intervention • Automation? ? ?

DON’T BE SHOCKED! Thank You for Attending 49