Renal GIRFT and Quality Improvement South London Renal








- Slides: 31

Renal GIRFT and Quality Improvement South London Renal Care Alliance October 2019 Will Mc. Kane

Getting it Right First Time (GIRFT) A clinically led programme across 40 specialties: Aims • Reduce unwarranted variation, • Improve the quality of patient outcomes • Deliver operational productivity improvements Cross Cutting themes: CC, OP, Pathology. . 2

Where are we? • 52 visits complete • Paid a price in terms of timeliness of reports • Excellent clinical engagement • Less consistent senior executive engagement • Working on National Report • February 2020 • Co-badged with RA/BRS/RCP

Emerging themes • Data • The “predictable three” • Vascular Access • Access to Transplantation • Home therapies • Prevalence • PD Access and peritonitis • Staffing • AKI requiring nephrology input • Infection • Hospitalisation • Medicines management • Procurement

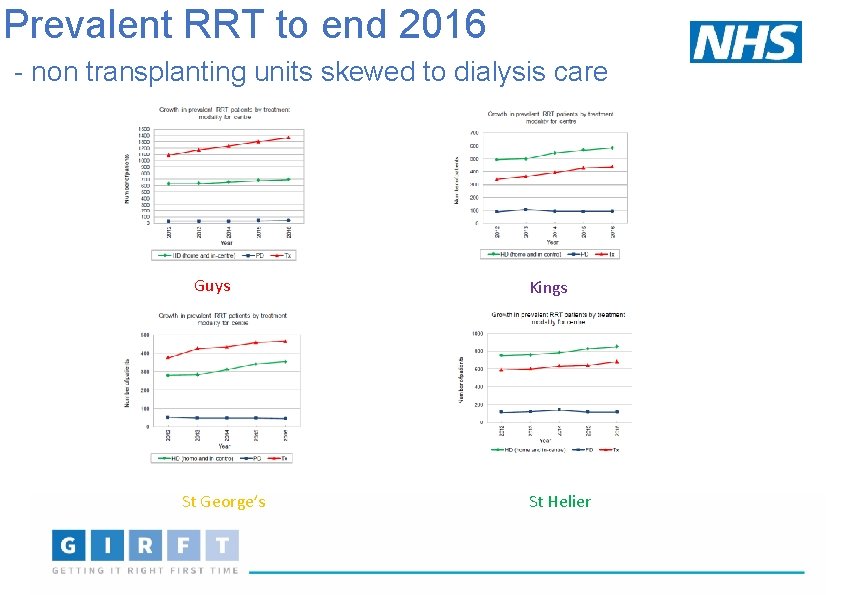
Prevalent RRT to end 2016 - non transplanting units skewed to dialysis care Guys St George’s Kings St Helier

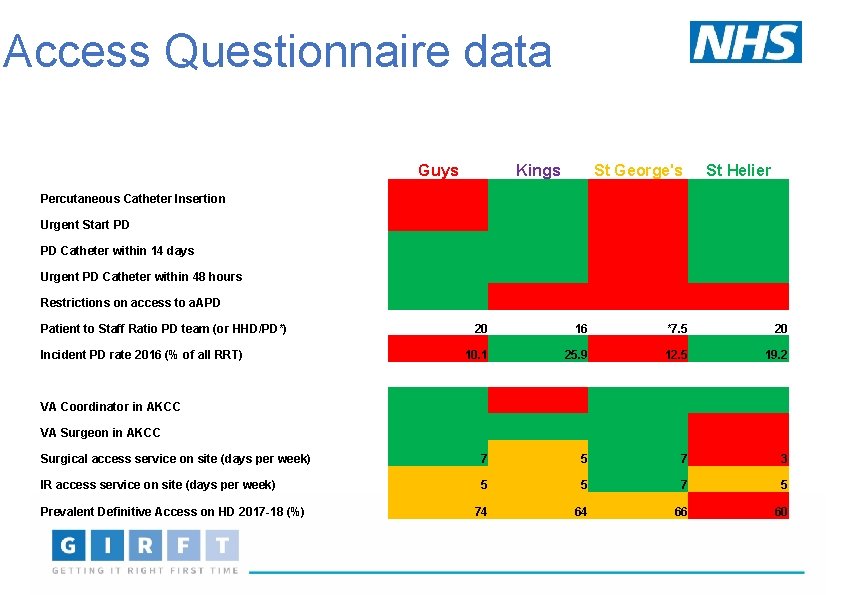
Access Questionnaire data Guys Kings St George's St Helier Percutaneous Catheter Insertion Urgent Start PD Catheter within 14 days Urgent PD Catheter within 48 hours Restrictions on access to a. APD Patient to Staff Ratio PD team (or HHD/PD*) Incident PD rate 2016 (% of all RRT) 20 16 *7. 5 20 10. 1 25. 9 12. 5 19. 2 VA Coordinator in AKCC VA Surgeon in AKCC Surgical access service on site (days per week) 7 5 7 3 IR access service on site (days per week) 5 5 74 64 66 60 Prevalent Definitive Access on HD 2017 -18 (%)

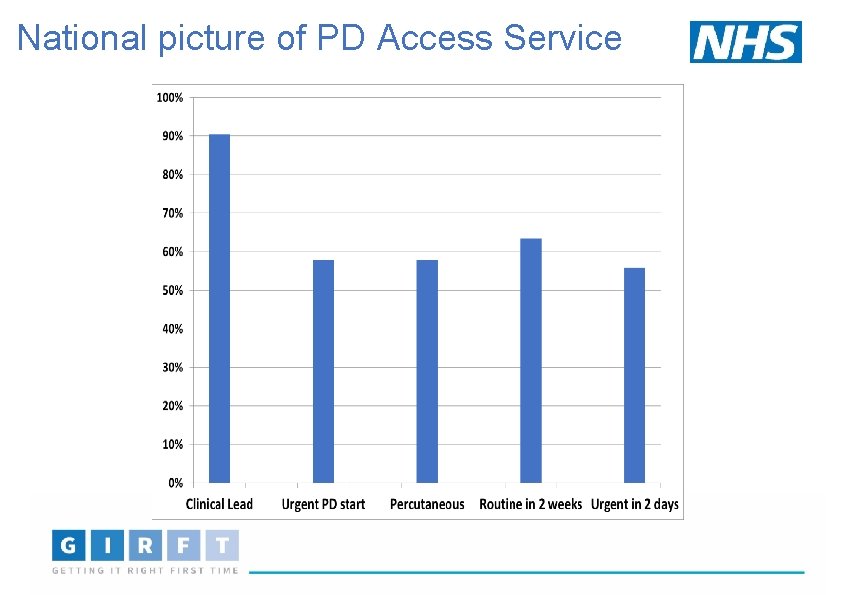
National picture of PD Access Service

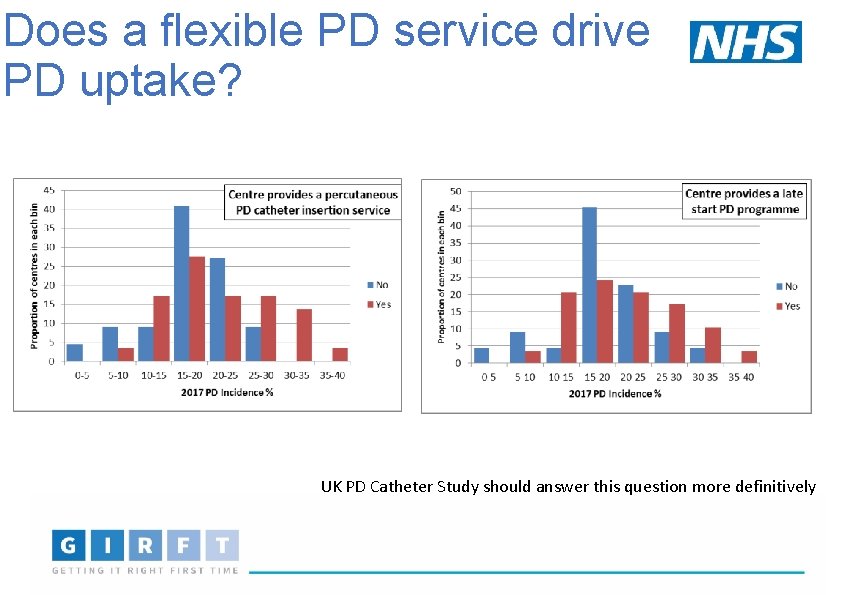
Does a flexible PD service drive PD uptake? UK PD Catheter Study should answer this question more definitively

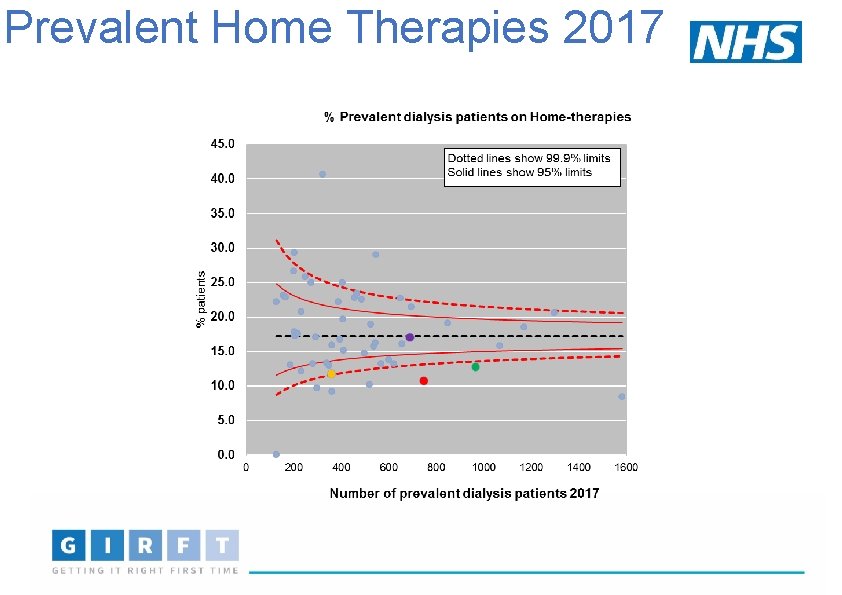
Prevalent Home Therapies 2017

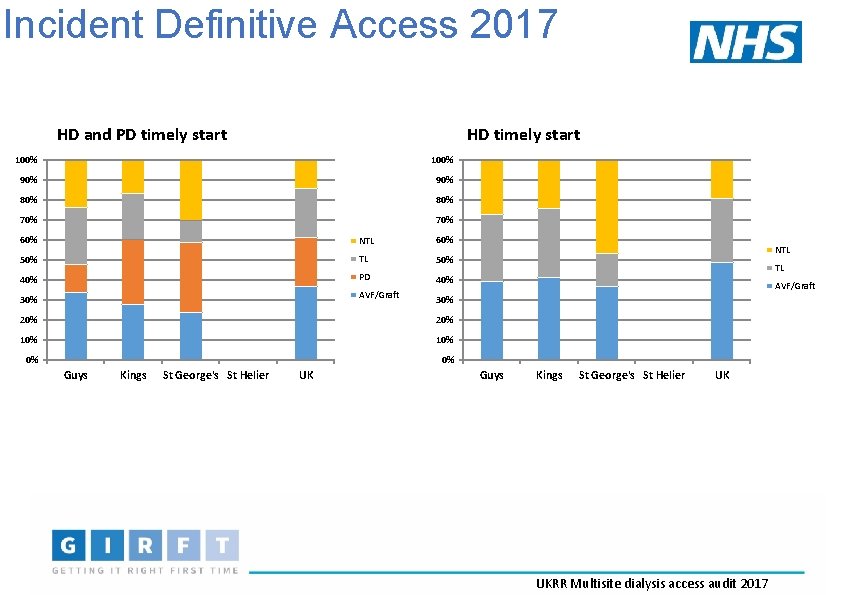
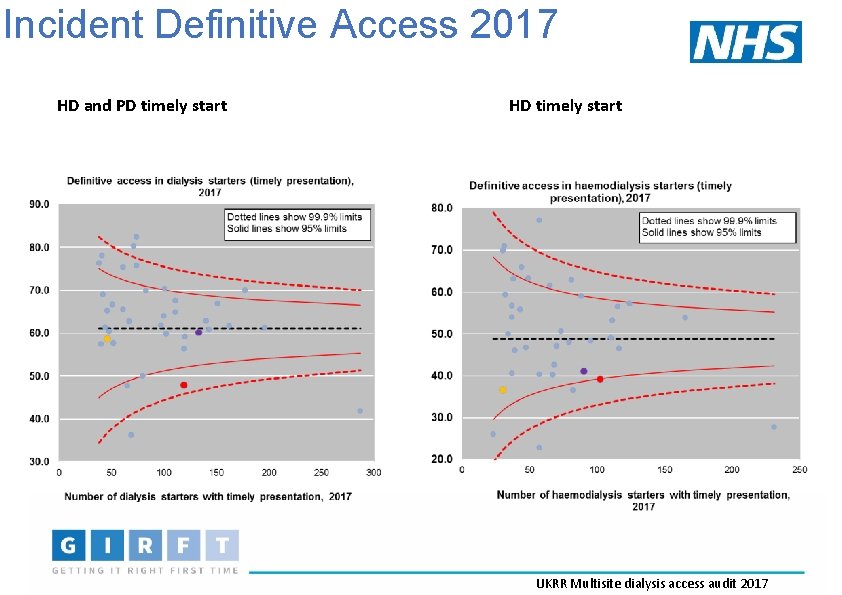
Incident Definitive Access 2017 HD and PD timely start HD timely start 100% 90% 80% 70% 60% NTL 60% 50% TL 50% 40% PD 40% AVF/Graft 30% 20% 10% 0% 0% Kings St George's St Helier UK TL AVF/Graft 30% 20% Guys NTL Guys Kings St George's St Helier UK UKRR Multisite dialysis access audit 2017

Incident Definitive Access 2017 HD and PD timely start HD timely start UKRR Multisite dialysis access audit 2017

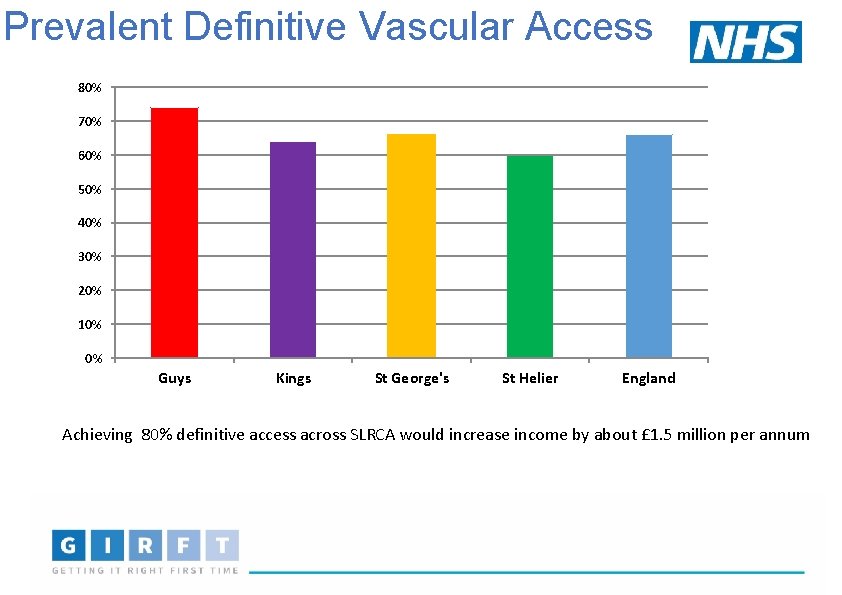
Prevalent Definitive Vascular Access 80% 70% 60% 50% 40% 30% 20% 10% 0% Guys Kings St George's St Helier England Achieving 80% definitive access across SLRCA would increase income by about £ 1. 5 million per annum

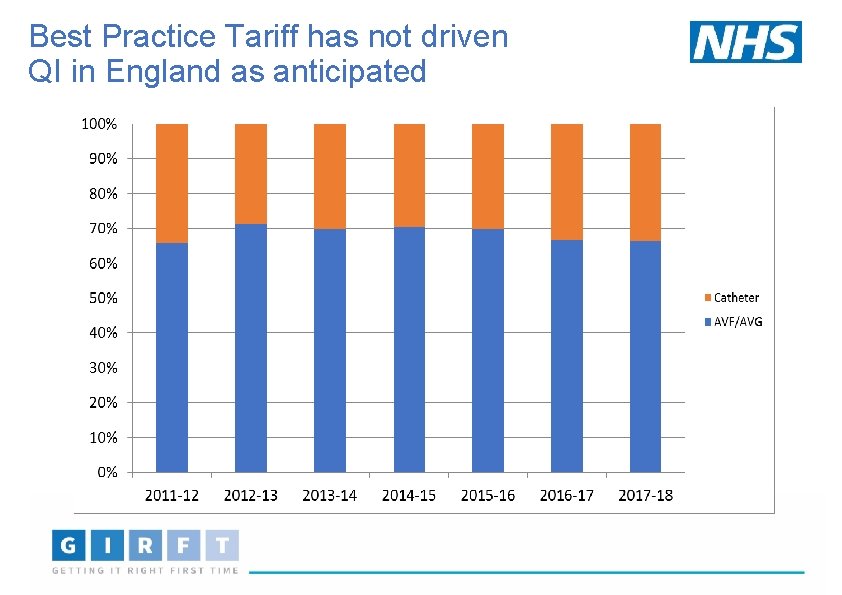
Best Practice Tariff has not driven QI in England as anticipated

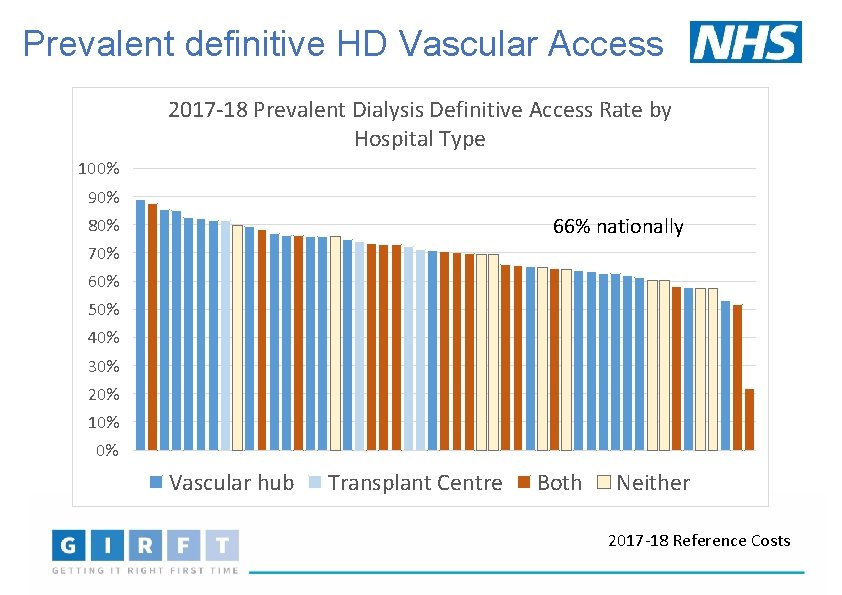
Prevalent definitive HD Vascular Access 2017 -18 Prevalent Dialysis Definitive Access Rate by Hospital Type 100% 90% 66% nationally 80% 70% 60% 50% 40% 30% 20% 10% 0% Vascular hub Transplant Centre Both Neither 2017 -18 Reference Costs

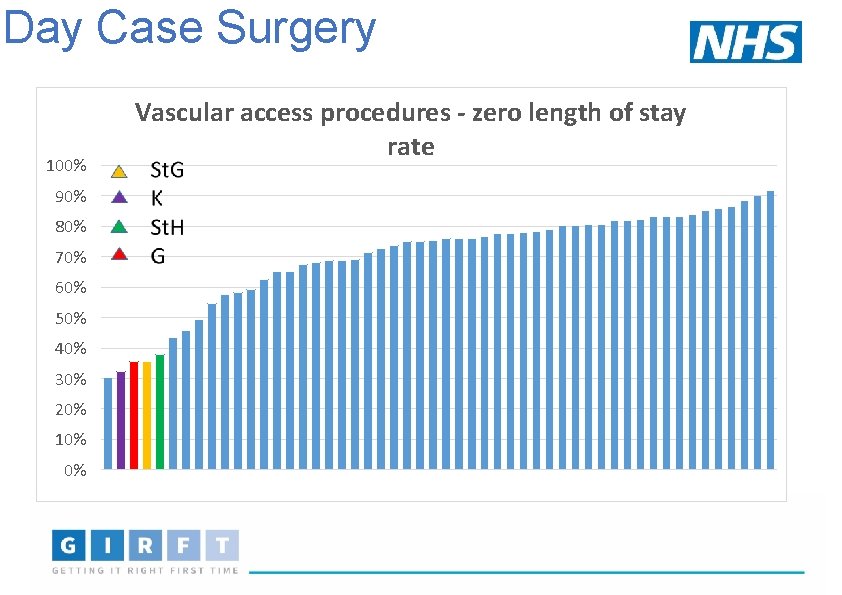
Day Case Surgery 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Vascular access procedures - zero length of stay rate

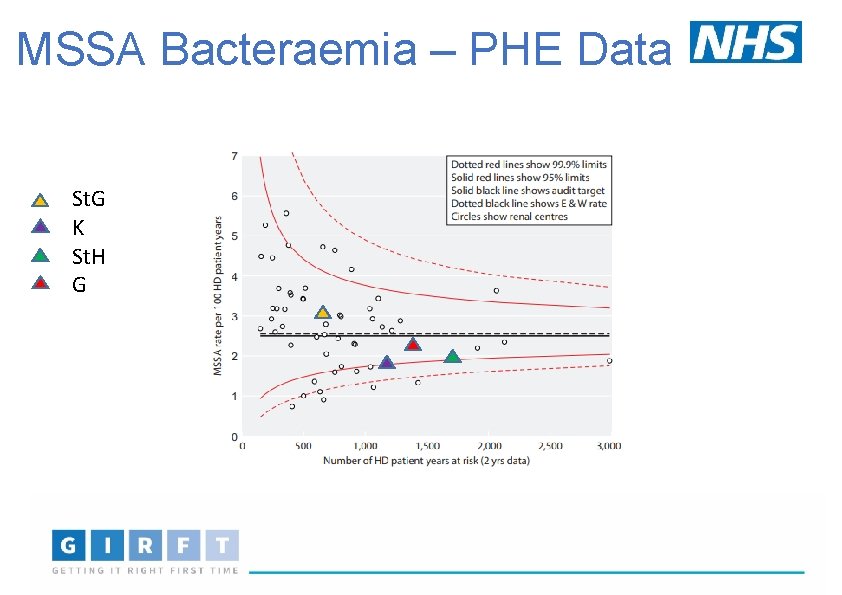
MSSA Bacteraemia – PHE Data St. G K St. H G

Equity of access to transplantation • At a national level 3 major listing inequities: • Patients in non-transplanting centres: • less likely to get listed • OR 0. 68, 95% CI 0. 62– 0. 74 at 2 years • Less likely to get a LD Tx • OR 0. 65, 95% CI 0. 58– 0. 74 • Females less likely to get listed • OR 0. 84, 95% CI 0. 75– 0. 93 UKRR 2017

Equity of access to transplantation • We will not solve this unless we have collaborative transplant networks • Transplant centres recognise their responsibilities to the whole network • Renal centres adequately staffed • What data is most helpful to assess this and to drive QI? • Interpret NHSBT transplant rates PMP with caution • Pre-emptive listing as a proportion of those listed is a valid metric, but interpret with caution

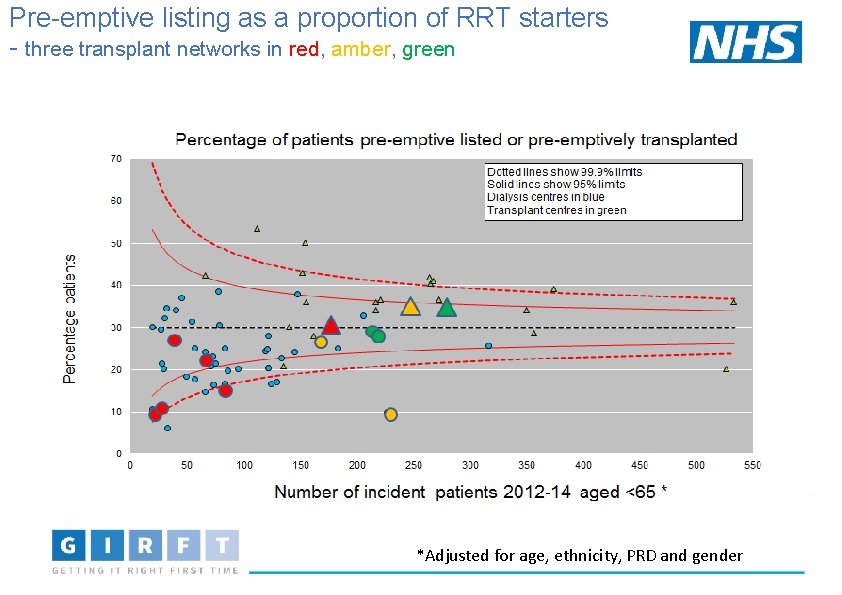
Pre-emptive listing as a proportion of RRT starters - three transplant networks in red, amber, green *Adjusted for age, ethnicity, PRD and gender

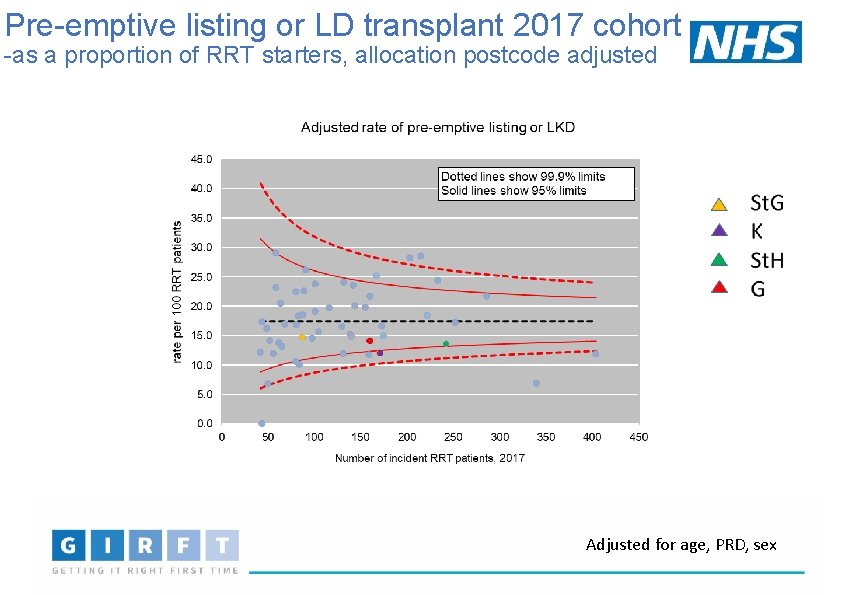
Pre-emptive listing or LD transplant 2017 cohort -as a proportion of RRT starters, allocation postcode adjusted Adjusted for age, PRD, sex

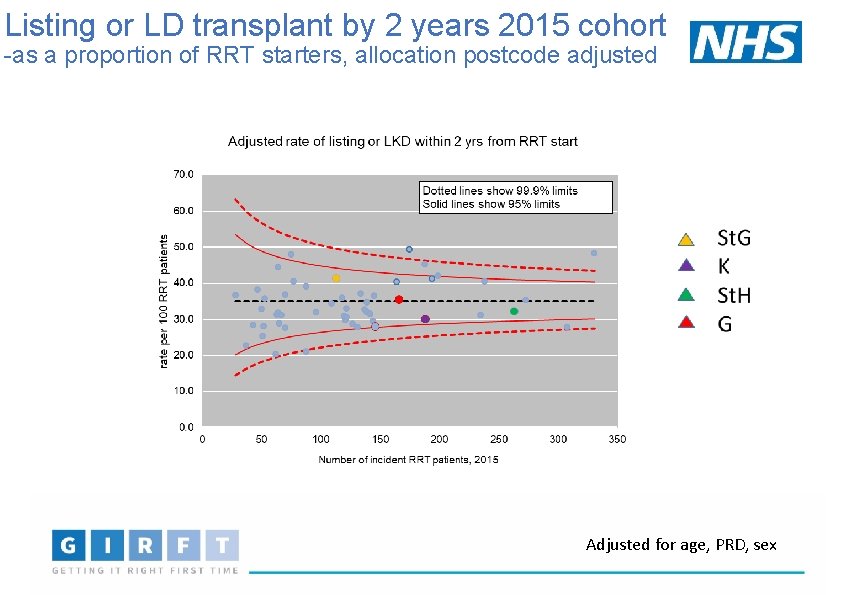
Listing or LD transplant by 2 years 2015 cohort -as a proportion of RRT starters, allocation postcode adjusted Adjusted for age, PRD, sex

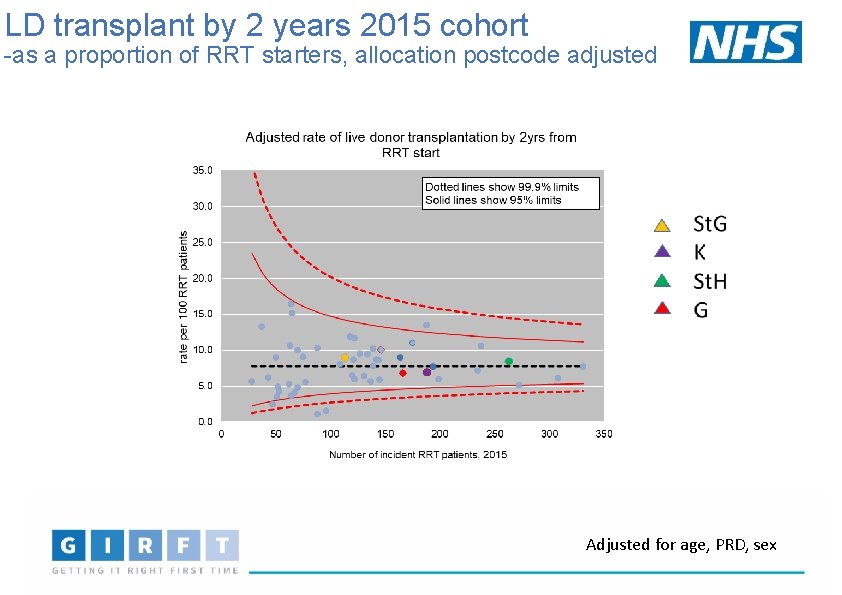
LD transplant by 2 years 2015 cohort -as a proportion of RRT starters, allocation postcode adjusted Adjusted for age, PRD, sex

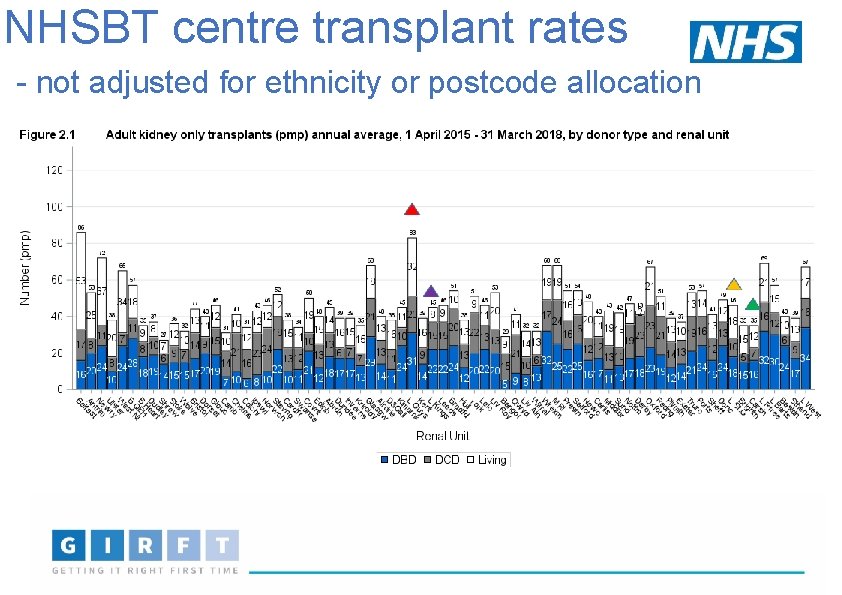
NHSBT centre transplant rates - not adjusted for ethnicity or postcode allocation

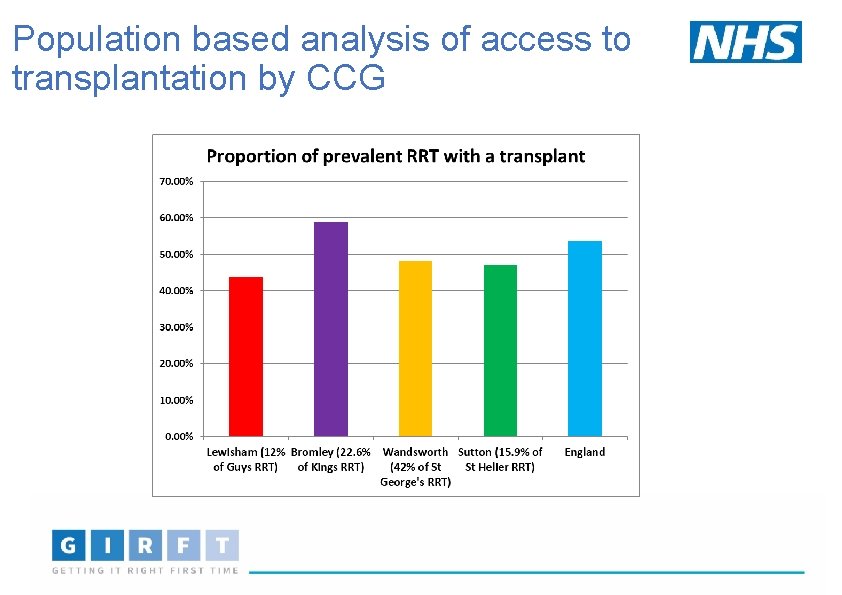
Population based analysis of access to transplantation by CCG

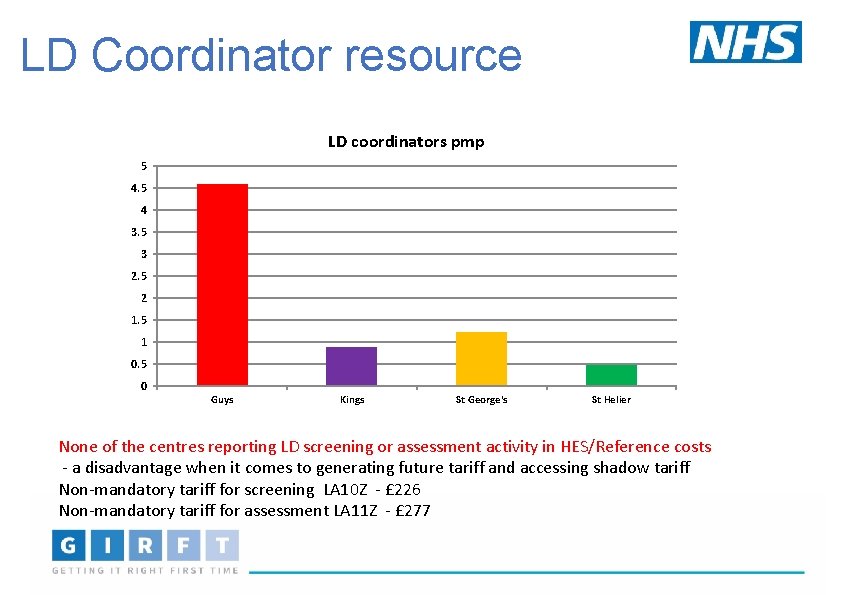
LD Coordinator resource LD coordinators pmp 5 4 3. 5 3 2. 5 2 1. 5 1 0. 5 0 Guys Kings St George's St Helier None of the centres reporting LD screening or assessment activity in HES/Reference costs - a disadvantage when it comes to generating future tariff and accessing shadow tariff Non-mandatory tariff for screening LA 10 Z - £ 226 Non-mandatory tariff for assessment LA 11 Z - £ 277

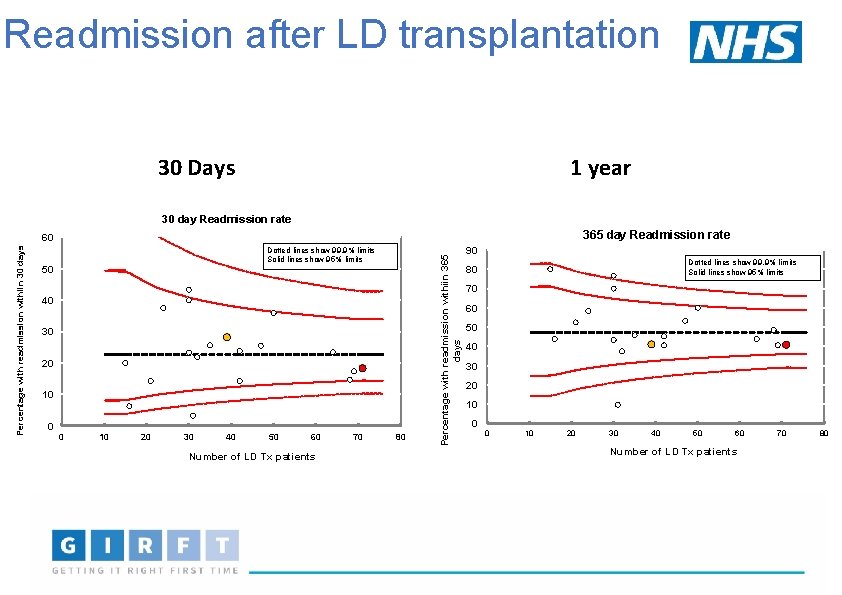
Readmission after LD transplantation 1 year 30 Days 30 day Readmission rate 365 day Readmission rate Dotted lines show 99. 9% limits Solid lines show 95% limits 50 40 30 20 10 0 0 10 20 30 40 50 60 Number of LD Tx patients 70 80 Percentage with readmission withiin 365 days Percentage with readmission withiin 30 days 60 90 Dotted lines show 99. 9% limits Solid lines show 95% limits 80 70 60 50 40 30 20 10 0 0 10 20 30 40 50 60 Number of LD Tx patients 70 80

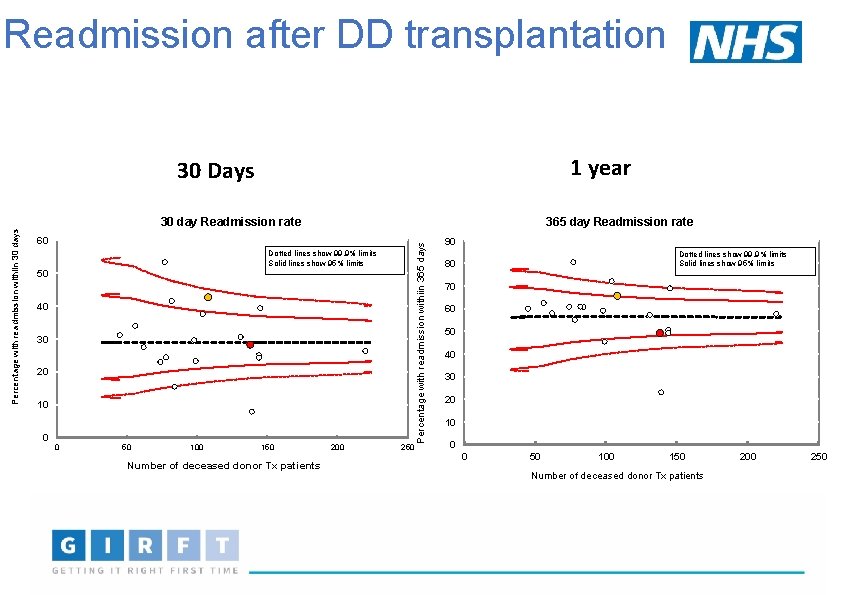
Readmission after DD transplantation 1 year 30 Days 365 day Readmission rate 60 Dotted lines show 99. 9% limits Solid lines show 95% limits 50 40 30 20 10 0 0 50 100 150 Number of deceased donor Tx patients 200 250 Percentage with readmission withiin 365 days Percentage with readmission withiin 30 days 30 day Readmission rate 90 Dotted lines show 99. 9% limits Solid lines show 95% limits 80 70 60 50 40 30 20 10 0 0 50 100 150 Number of deceased donor Tx patients 200 250

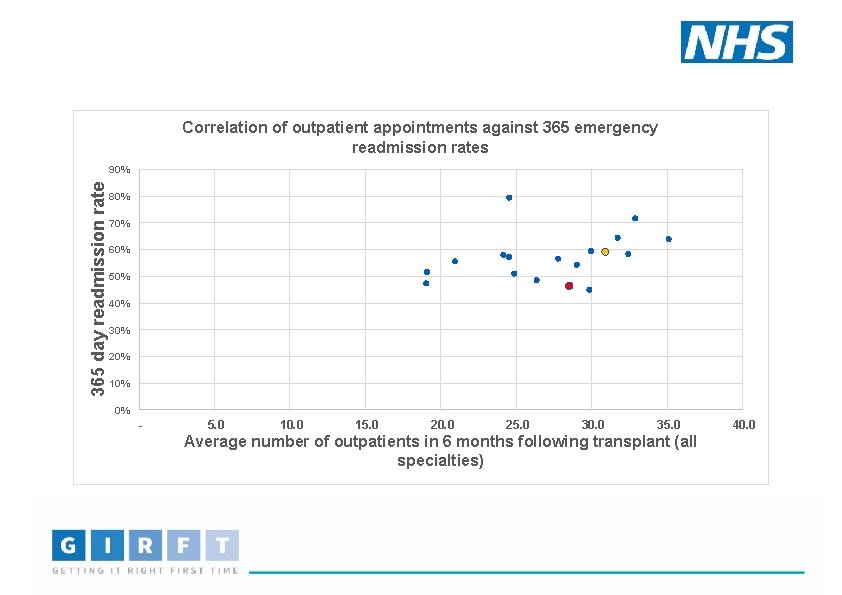
Correlation of outpatient appointments against 365 emergency readmission rates 365 day readmission rate 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% - 5. 0 10. 0 15. 0 20. 0 25. 0 30. 0 35. 0 Average number of outpatients in 6 months following transplant (all specialties) 40. 0

What next? • GIRFT data has set the scene • Variation • • Workforce On site access surgery and IR Infrastructure for PD Day case surgery • Evidence of improved equity in access to transplantation • Work in progress • Transplant First • Areas where a coordinated network approach could help • Making sure that patients have equal access to the resources within South London • May require • • Some changes in working practices Innovative models of care delivery for dialysis access

Renal Co-Leads and core project team 30

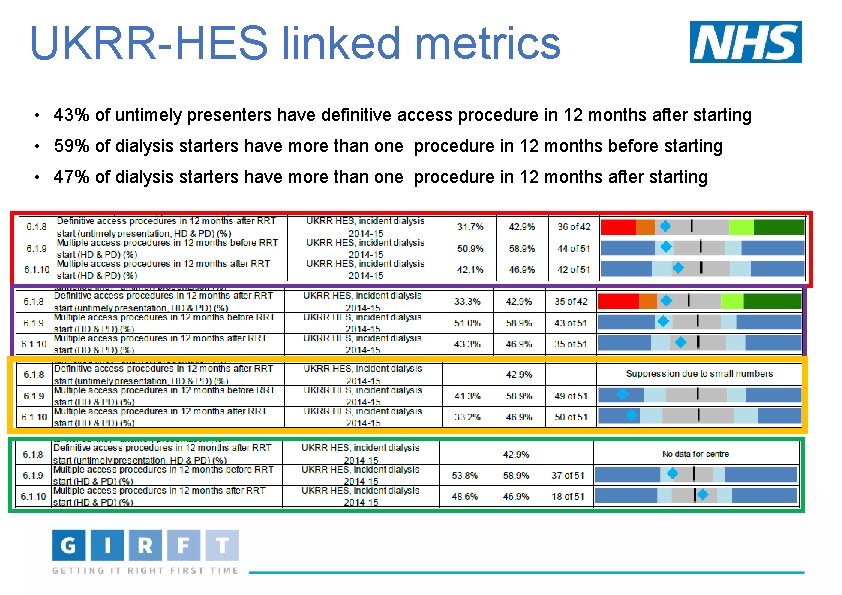
UKRR-HES linked metrics • 43% of untimely presenters have definitive access procedure in 12 months after starting • 59% of dialysis starters have more than one procedure in 12 months before starting • 47% of dialysis starters have more than one procedure in 12 months after starting