Polypharmacy Anticoagulation AF meets PCI David J Moliterno









- Slides: 20

Polypharmacy Anticoagulation: AF meets PCI David J. Moliterno, MD Professor and Chairman Department of Internal Medicine The University of Kentucky Linda and Jack Gill Heart Institute

Conflict of Interest/Disclosure “Polypharmacy Anticoagulation: AF Meets PCI? ” DSMB: Jannsen Pharmaceuticals (GEMINI Study) Research Grant: Merck (Steering Committee: TRACER and TRA 2 P) Astra Zeneca (Steering Committee: TWILIGHT Study)

Optimal Anticoagulation—does it exist? Bleeding Thrombosis intensity x duration

Atrial Fibrillation § Most common sustained cardiac arrhythmia § Currently affects nearly 2. 3 million Americans, or 1% of US population § Prevalence expected to increase 2. 5 x by 2050 § Lifetime risk of developing AF: 1 in 4 for men and women ≥ 40 years of age § Among ACS-PCI patients, ~5% have AF § AF best managed with OAC among those needing antithrombotic therapy

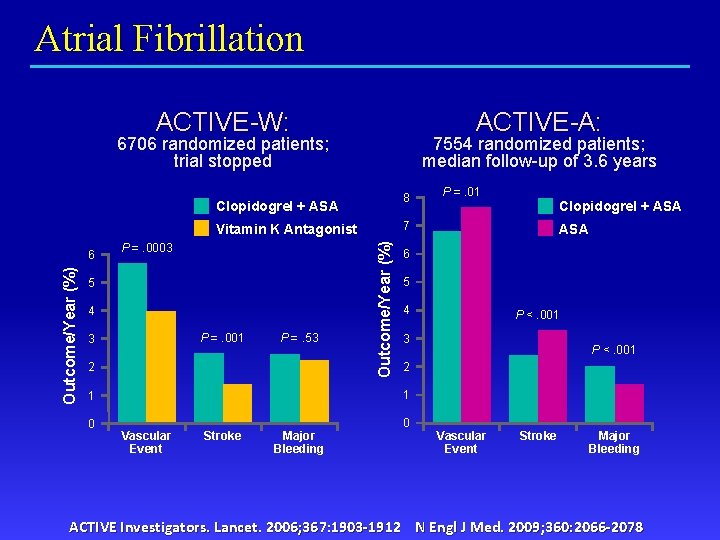
Atrial Fibrillation ACTIVE-W: ACTIVE-A: 6706 randomized patients; trial stopped 7554 randomized patients; median follow-up of 3. 6 years 8 Clopidogrel + ASA 5 4 P =. 001 3 P =. 53 2 Outcome/Year (%) P =. 0003 5 4 P <. 001 2 0 0 Major Bleeding P <. 001 3 1 Stroke ASA 6 1 Vascular Event Clopidogrel + ASA 7 Vitamin K Antagonist 6 P =. 01 Vascular Event Stroke Major Bleeding ACTIVE Investigators. Lancet. 2006; 367: 1903 -1912 N Engl J Med. 2009; 360: 2066 -2078

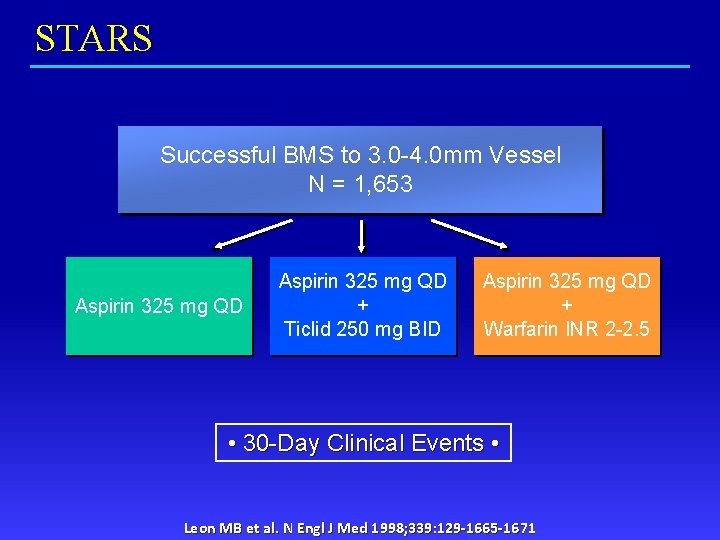
STARS Successful BMS to 3. 0 -4. 0 mm Vessel N = 1, 653 Aspirin 325 mg QD + Ticlid 250 mg BID Aspirin 325 mg QD + Warfarin INR 2 -2. 5 • 30 -Day Clinical Events • Leon MB et al. N Engl J Med 1998; 339: 129 -1665 -1671

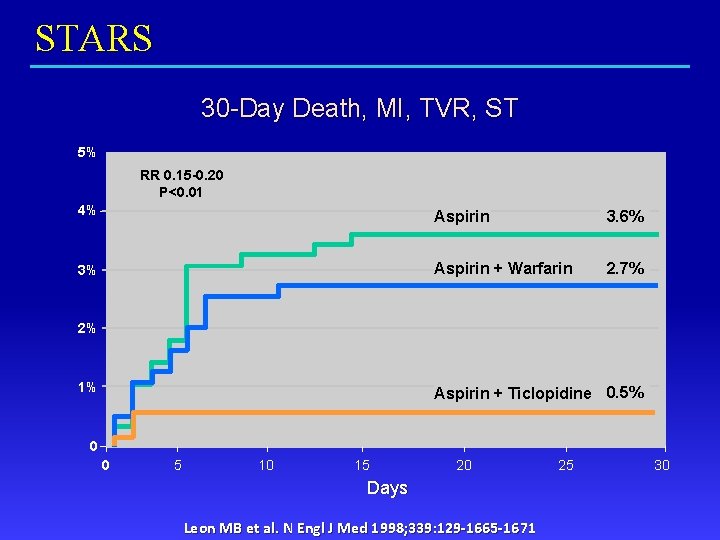
STARS 30 -Day Death, MI, TVR, ST 5% RR 0. 15 -0. 20 P<0. 01 4% Aspirin 3. 6% 3% Aspirin + Warfarin 2. 7% 2% 1% Aspirin + Ticlopidine 0. 5% 0 0 5 10 15 20 Days Leon MB et al. N Engl J Med 1998; 339: 129 -1665 -1671 25 30

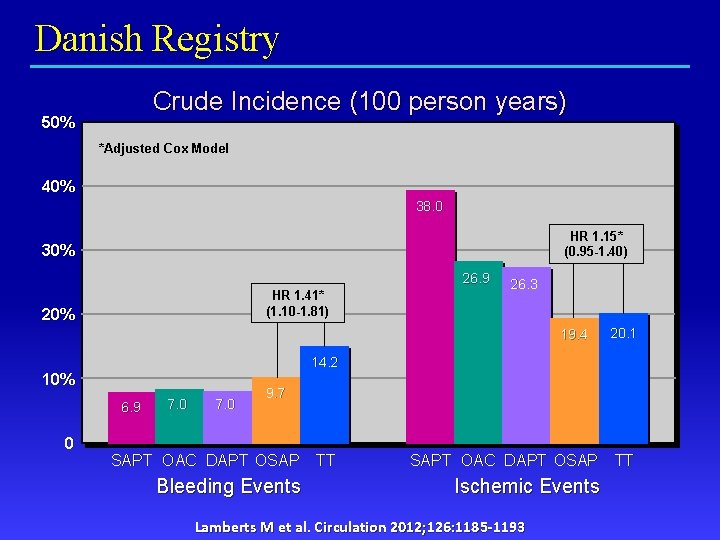
Danish Registry § § Danish National Registry 2000 -2009 11, 480 subjects with AF and new MI or PCI Categorized as single, double, triple therapies Reviewed early and late (1 year) hospitalizations for bleeding and ischemic events Lamberts M et al. Circulation 2012; 126: 1185 -1193

Danish Registry Crude Incidence (100 person years) 50% *Adjusted Cox Model 40% 38. 0 HR 1. 15* (0. 95 -1. 40) 30% 26. 9 HR 1. 41* (1. 10 -1. 81) 20% 26. 3 19. 4 20. 1 14. 2 10% 6. 9 0 7. 0 9. 7 SAPT OAC DAPT OSAP Bleeding Events TT SAPT OAC DAPT OSAP Ischemic Events Lamberts M et al. Circulation 2012; 126: 1185 -1193 TT

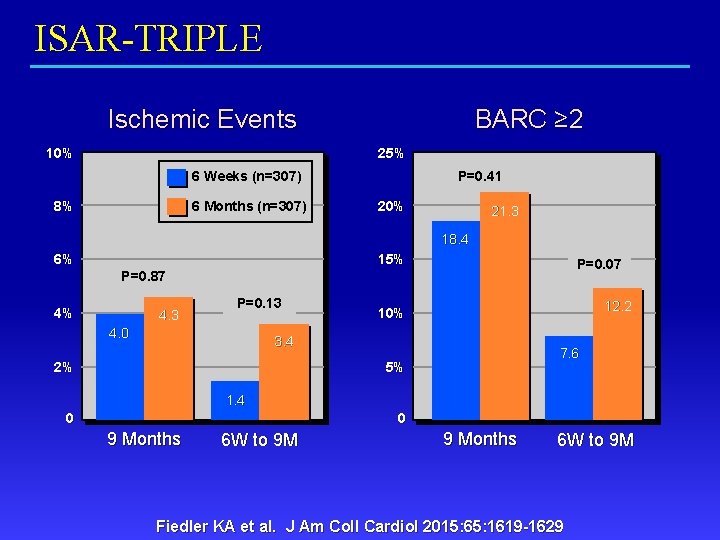
ISAR-TRIPLE Patients receiving OAC undergoing DES N = 614 OAC + ASA 75 -200 mg daily Clopidogrel 300 -600 mg, then 75 mg daily 6 weeks Clopidogrel 300 -600 mg, then 75 mg daily 6 months • 9 -Month Death, MI, CVA, ST, TIMI Major Bleeding • Fiedler KA et al. J Am Coll Cardiol 2015: 65: 1619 -1629

ISAR-TRIPLE Ischemic Events 10% BARC ≥ 2 25% 6 Weeks (n=307) 8% 6 Months (n=307) P=0. 41 20% 21. 3 18. 4 6% 15% P=0. 07 P=0. 87 4% 4. 3 P=0. 13 4. 0 12. 2 10% 3. 4 2% 7. 6 5% 1. 4 0 0 9 Months 6 W to 9 M Fiedler KA et al. J Am Coll Cardiol 2015: 65: 1619 -1629

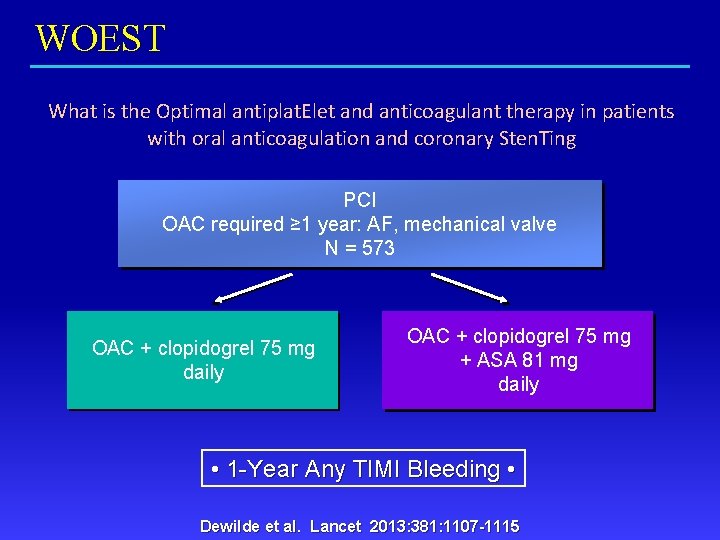
WOEST What is the Optimal antiplat. Elet and anticoagulant therapy in patients with oral anticoagulation and coronary Sten. Ting PCI OAC required ≥ 1 year: AF, mechanical valve N = 573 OAC + clopidogrel 75 mg daily OAC + clopidogrel 75 mg + ASA 81 mg daily • 1 -Year Any TIMI Bleeding • Dewilde et al. Lancet 2013: 381: 1107 -1115

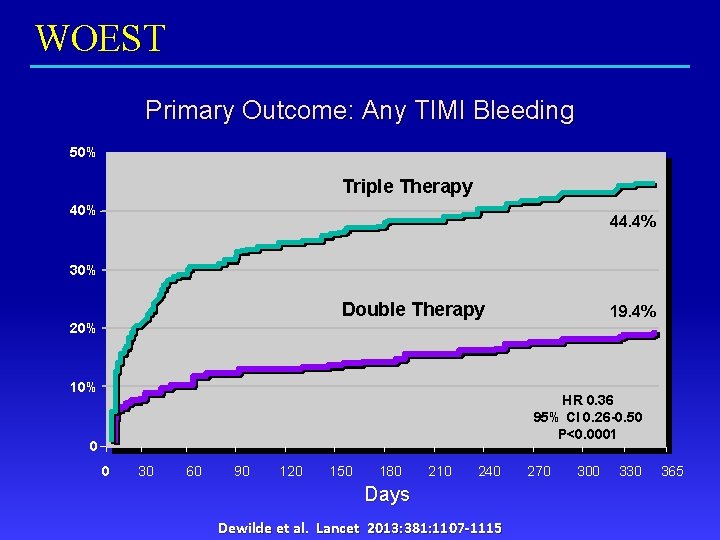
WOEST Primary Outcome: Any TIMI Bleeding 50% Triple Therapy 40% 44. 4% 30% Double Therapy 19. 4% 20% 10% HR 0. 36 95% CI 0. 26 -0. 50 P<0. 0001 0 0 30 60 90 120 150 180 210 240 Days Dewilde et al. Lancet 2013: 381: 1107 -1115 270 300 330 365

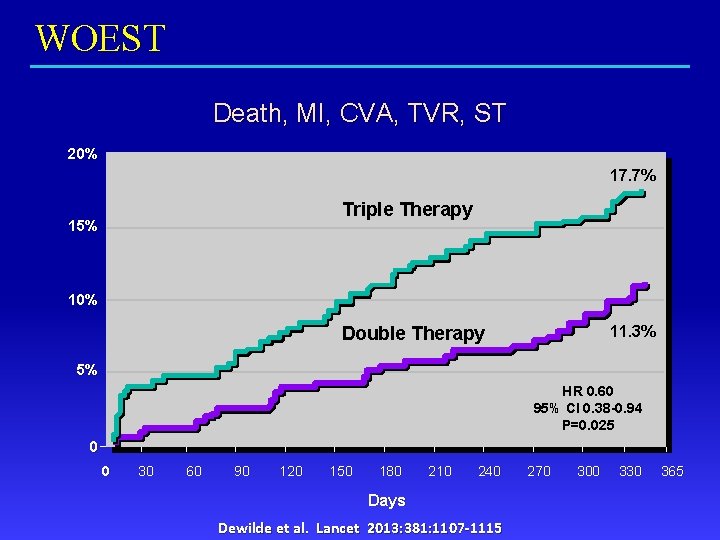
WOEST Death, MI, CVA, TVR, ST 20% 17. 7% Triple Therapy 15% 10% 11. 3% Double Therapy 5% HR 0. 60 95% CI 0. 38 -0. 94 P=0. 025 0 0 30 60 90 120 150 180 210 240 Days Dewilde et al. Lancet 2013: 381: 1107 -1115 270 300 330 365

Algorithm for AF-PCI Considerations § Washout OAC § INR ≤ 2. 0 for radial § INR ≤ 1. 5 for femoral § Withhold NOAC 24 hours (longer if SRI) § Avoid polypharmacy anticoagulation (GPI) § Low-dose ASA § Lower INR target § Shortened-course DAPT § Lifelong OAC (± SAPT) Angiolillo et al. Circ Cardiovasc Intv 2016

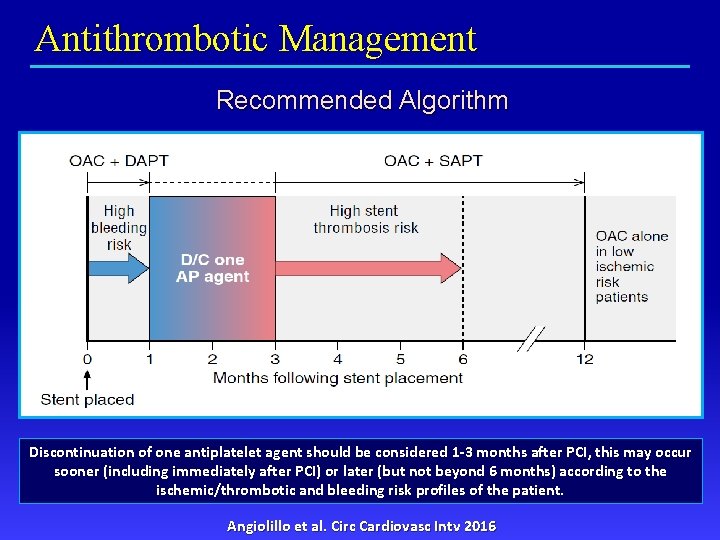
Antithrombotic Management Recommended Algorithm Discontinuation of one antiplatelet agent should be considered 1 -3 months after PCI, this may occur sooner (including immediately after PCI) or later (but not beyond 6 months) according to the ischemic/thrombotic and bleeding risk profiles of the patient. Angiolillo et al. Circ Cardiovasc Intv 2016

Algorithm for AF-PCI Considerations § More frequent follow-up than AF alone or ACS alone or PCI alone § Specific guidance for patient and PCP § Choice, extent, duration of antithrombotic therapy may change for patient or guidelines § Throughout post-PCI course need to reconsider antiplatelet risk-benefit Angiolillo et al. Circ Cardiovasc Intv 2016

Summary § ~5% of ACS patients have pre-existing or soon-tocome AF § Triple therapy is associated with a 40% increased risk of clinically significant bleeding § Small RCT suggest Dual Therapy with OAC and SAPT (clopidogrel) at least as effective and safer § For longer-term care, monotherapy vs “safer” dual § Nanoparticle coated stent trial ongoing § Many ongoing or planned RCT to better understand polypharmacy best practices and how NOACs and newer P 2 Y 12 agents fit in

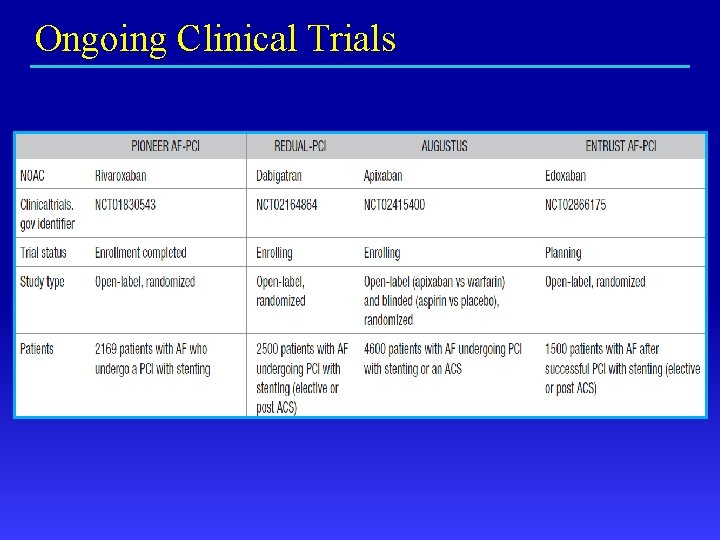
Ongoing Clinical Trials

Polypharmacy Anticoagulation: AF meets PCI David J. Moliterno, MD Professor and Chairman Department of Internal Medicine The University of Kentucky Linda and Jack Gill Heart Institute