Pathophysiology of DM Dr Reem Murad According to


















- Slides: 38

Pathophysiology of DM Dr: Reem Murad

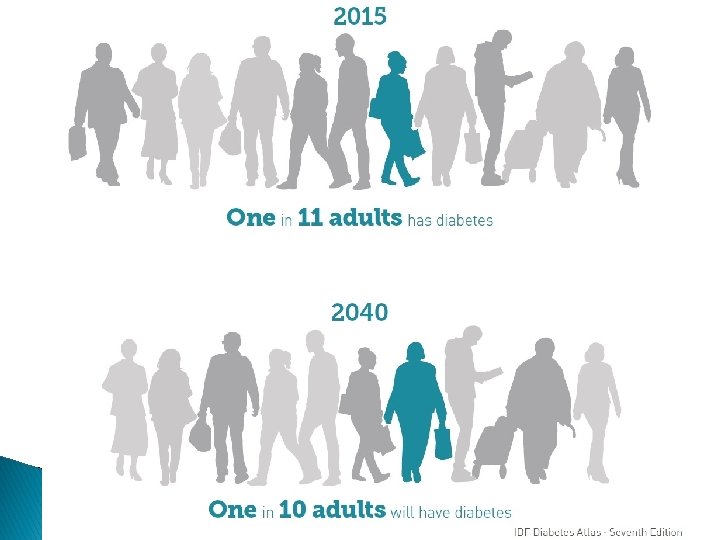
� According to the latest estimates of the WHO, 422 million people suffer from diabetes worldwide – and the number is growing steadily.


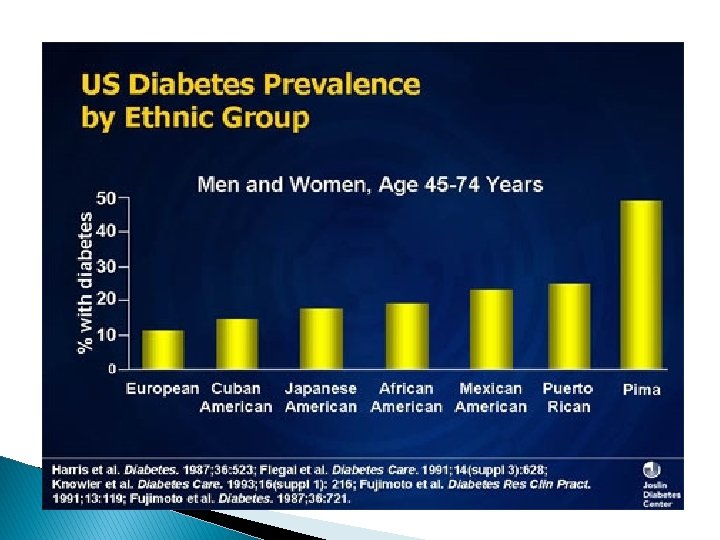
Epidemiology of Type 2 Diabetes





�I am going to talk about the pathophysiology of type 2 diabetes, because most new treatments are now being designed based on our understanding of the pathophysiology


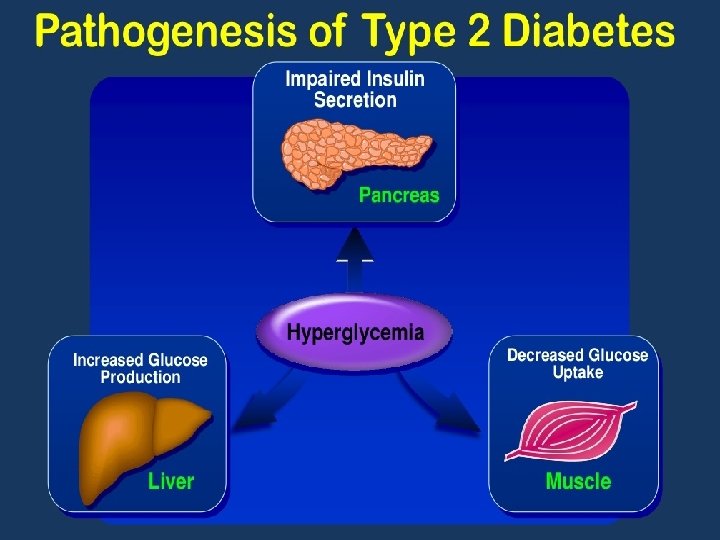
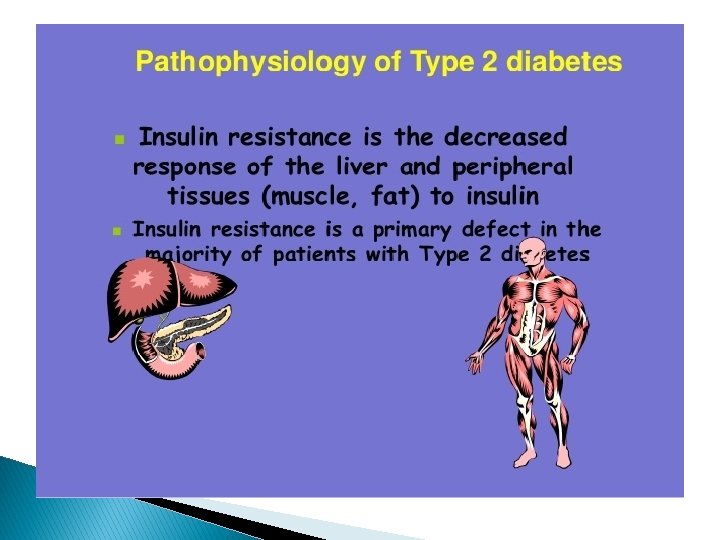
Pathophysiology of Type 2 Diabetes � insulin � And resistance beta-cell dysfunction.

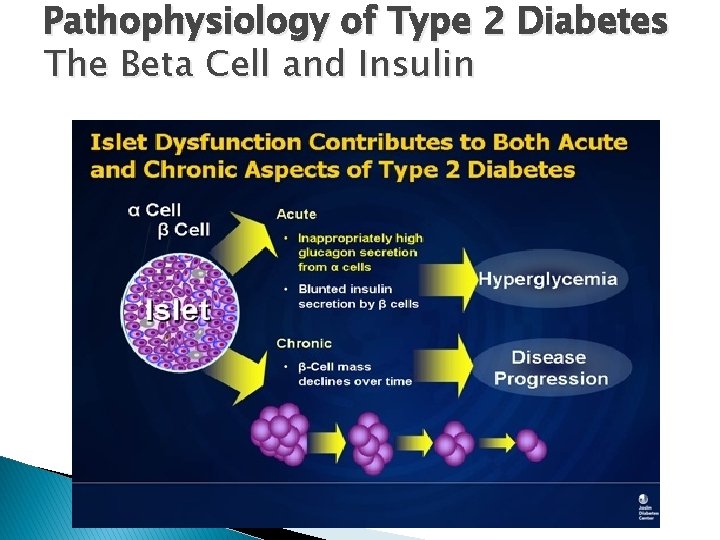
Pathophysiology of Type 2 Diabetes The Beta Cell and Insulin

� Insulin is not only produced when you eat, it is produced continuously. But when you eat, more of it is produced. � Very early in diabetes, the "pacemaker" that controls the secretion is affected, and we see disturbances in the frequency and the amplitude of insulin secretion bursts.

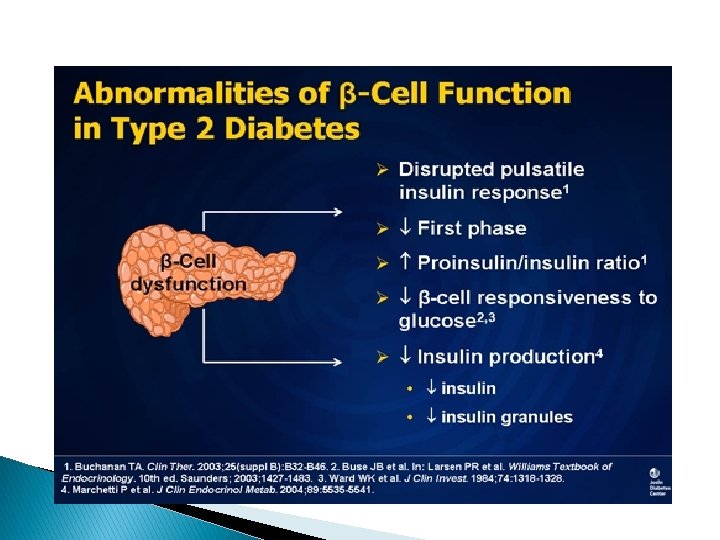
Insulin is produced in 2 phases. � In the first phase, there is preformed insulin, ready to be released very rapidly � In the second phase, more insulin is secreted because you have just eaten and your blood glucose goes higher � In diabetics: The beta cell itself does not respond to glucose as easily; � it becomes a little resistant. � Ultimately, these beta cells die.


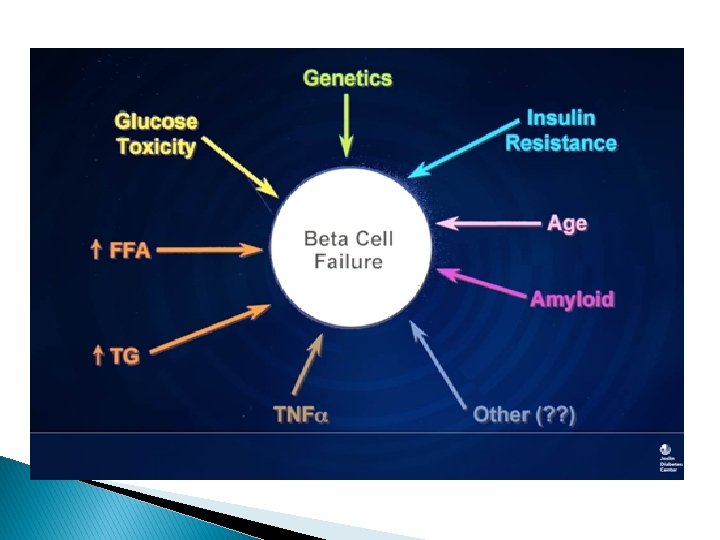
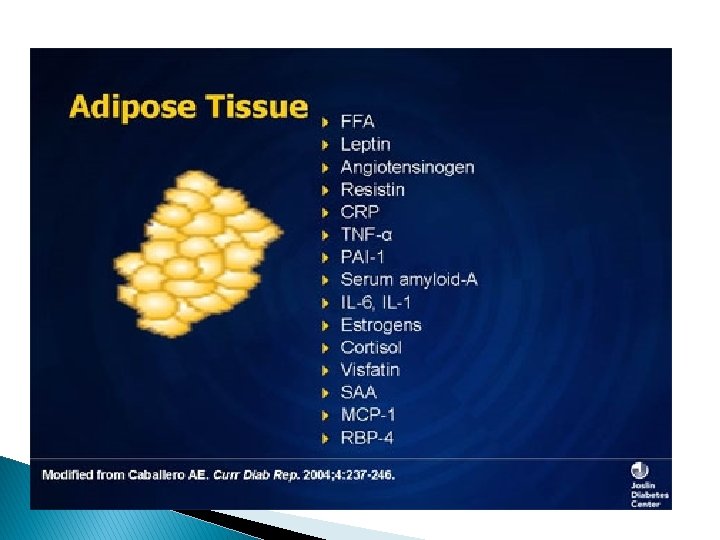
why did the beta cell die? � In type 2 diabetes, many players come together to attack a beta cell, especially if one is genetically prone to diabetes. � There is the effect of aging, � the deposition of amyloid � the adverse effect of cytokines, eg, tumor necrosis factor alpha, as well as free fatty acids, high triglycerides, � and genetic factors.


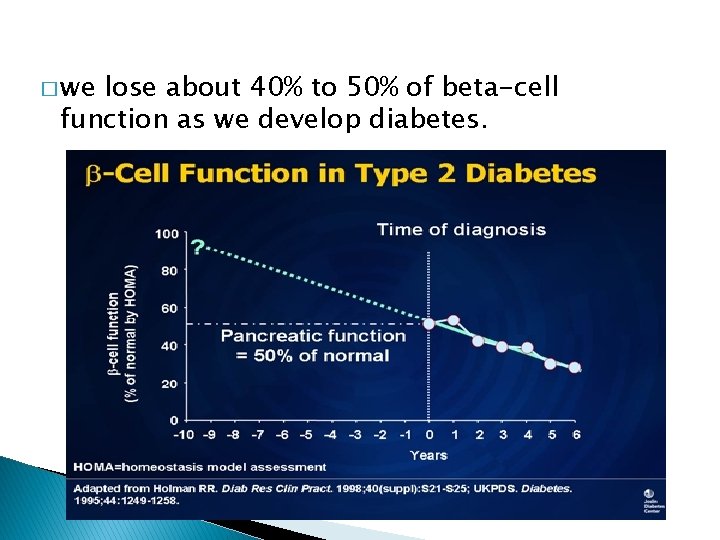
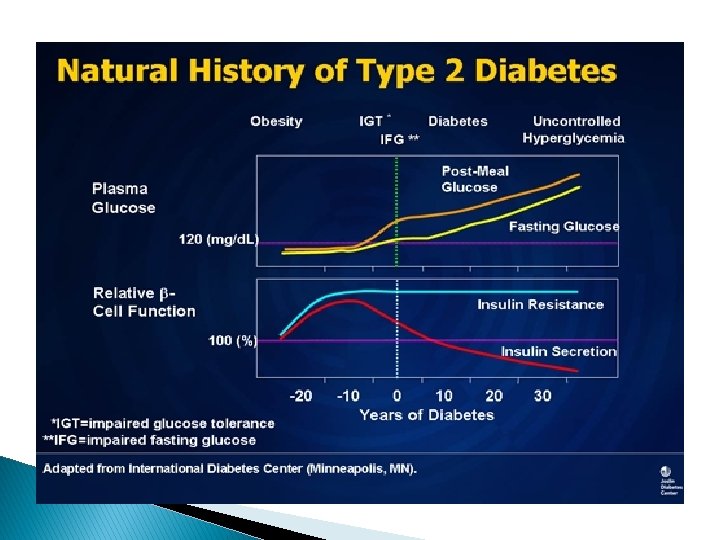
� we lose about 40% to 50% of beta-cell function as we develop diabetes.

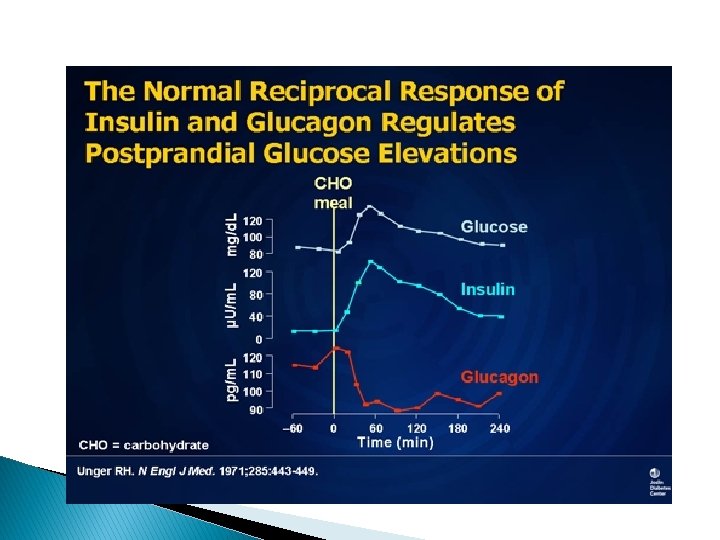
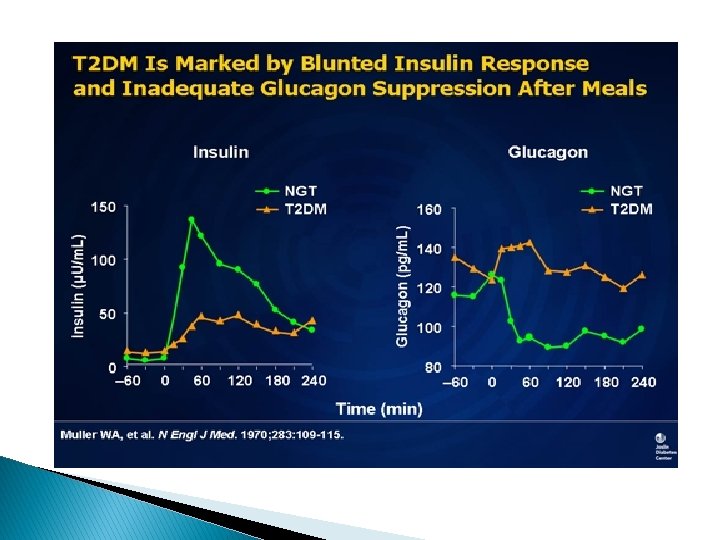
The Alpha Cell and Glucagon � Normally, if you eat a meal and your glucose rises, insulin will also increase and glucagon is suppressed, which is produced by the alpha cells



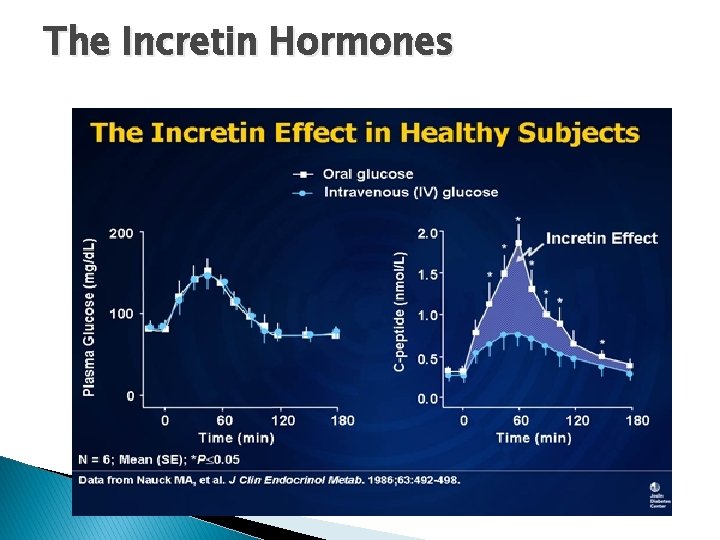
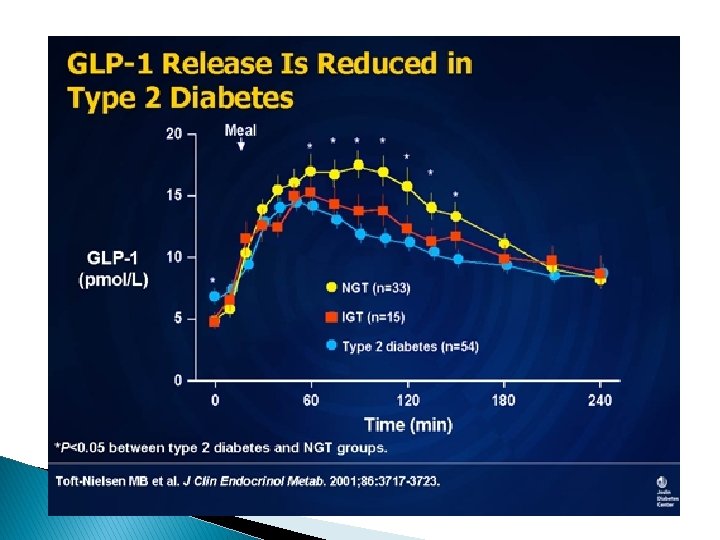
The Incretin Hormones � Incretin hormones are produced by the gastrointestinal (GI) tract in response to incoming nutrients. and have the ability to stimulate insulin release very quickly � There are 2 hormones that we are concerned with � One is glucagon-like peptide 1 (GLP-1 (This is a gut glucagon) � The second is glucose-dependent insulinotropic polypeptide (GIP). � These two are very important early stimulators of insulin secretion, even before glucose comes into the picture

The Incretin Hormones



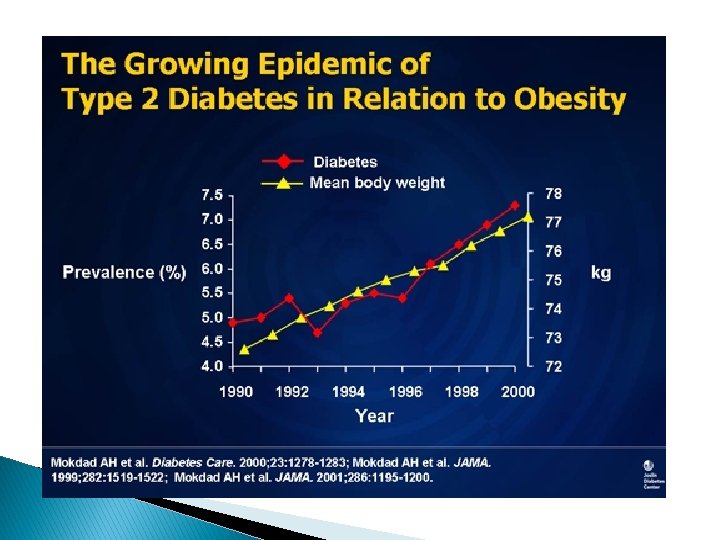
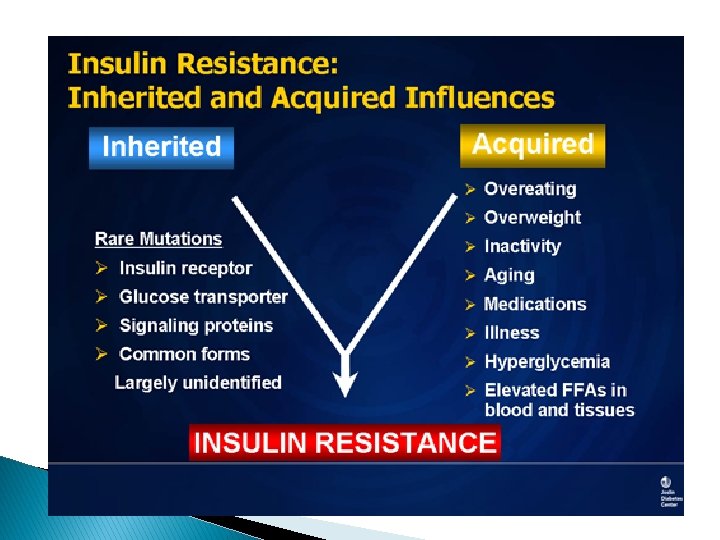
Insulin Resistance and Type 2 Diabetes � Insulin resistance is probably the earliest abnormality � One of the most common causes of insulin resistance is obesity � As time goes on, beta cells cannot keep producing this insulin. As their function starts to decline,




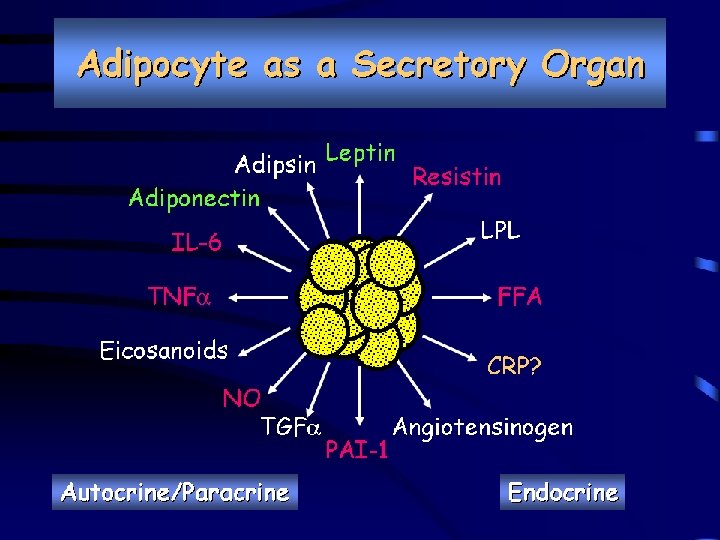
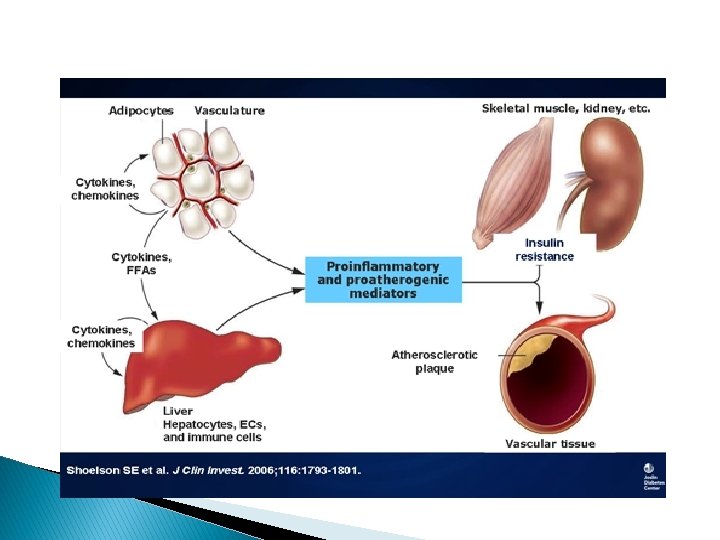
Obesity and Insulin Resistance fat distribution � visceral adiposity � in the liver causing fatty liver � leaking of the FFA from the adipocytes into muscle and interfere muscle insulin action.






Glucose toxicity � When a beta cell in a patient with diabetes is exposed to higher blood glucose, its own ability to make insulin is suppressed. � it makes insulin resistance even worse. Now you have beta cells working even harder and struggling.

Risk factor : non modianittiable

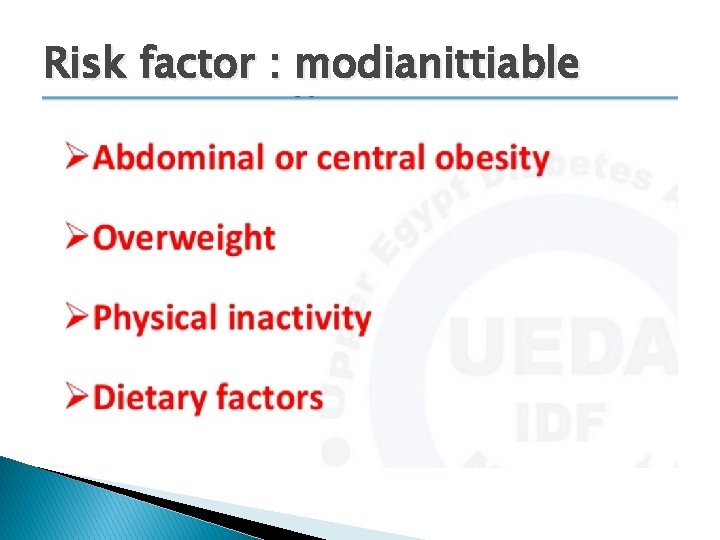
Risk factor : modianittiable