Immunization By Reem Habboush Ansam Sabah Shaher Homaydein

Immunization By: Reem Habboush Ansam Sabah Shaher Homaydein

Outline: �Objectives �Definition of Immunity �Types of immunity � vaccination �Routs of administration �Vaccines on schedule �The process �General precautions to be taken �Adolescents vaccines �Vaccinations for special health status persons �Vaccines Adverse Reactions

Objectives: �At the end of this lecture, the students will be able to: 1. Define core concepts (immunization, vaccination) 2. Identify types of vaccination clearly. 3. List 2 -3 of general precautions should be taken correctly. 4. Summarize the steps of vaccination process. 5. Identify vaccines adverse reactions.

Immunization: �Immunization is the process of inducing immunity artificially by either vaccination (active immunization) or administration of antibody (passive immunization).
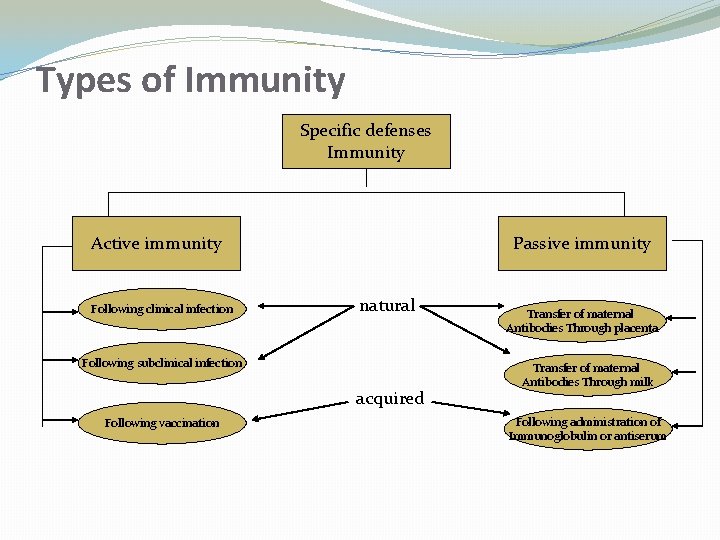
Types of Immunity Specific defenses Immunity Active immunity Following clinical infection Passive immunity natural Following subclinical infection acquired Following vaccination Transfer of maternal Antibodies Through placenta Transfer of maternal Antibodies Through milk Following administration of Immunoglobulin or antiserum

Active immunity �Resistance developed in response to stimulus by an antigen (infecting agent or vaccine) and is characterized by the production of antibodies by the host.

Passive immunity �Immunity conferred by an antibody produced in another host. � It may be acquired naturally or artificially (through an antibody-containing preparation).

Vaccination �Vaccination is a method of giving antigen to stimulate the immune response through active immunization. �A vaccine is “antigenic” but not “pathogenic”.

History of vaccination �Historical recordings of attempts of vaccination from 7 th century but not really recognised or successful until: � 1796: Edward Jenner demonstrated that inoculation with cowpox virus produced protection from infection with smallpox. �(Hence “Vaccination”: taken from vacca – the Latin word for cow) � 1860 s-1890 s: Louis Pasteur produced vaccines against chickenpox, cholera, diphtheria, anthrax and rabies

History of vaccination �Early 20 th Century: Toxoid vaccines against diphtheria and tetanus produced. �Post World War 2: successful live viral vaccines developed using cell culture techniques �Present and future: new technologies constantly developing: recombinant protein vaccines, DNA and conjugate vaccines

Types of vaccines �Live attenuated vaccine �Live vaccines �Inactivated (killed vaccines) �Toxoids �Cellular fraction vaccine �Surface antigen (recombinant) vaccines.

Live attenuated vaccines �These vaccines contain a version of living virus that has been weakened so that it does not cause serious disease in people with healthy immune system (example: MMR)

Live vaccines �Live vaccines are made from live infectious agents without any amendment. �The only live vaccine is “Variola” small pox vaccine.

Inactivated (killed) vaccines �Organisms are killed or inactivated by heat or chemicals but remain antigenic. �Usually safe but less effective than live attenuated vaccines. �The only absolute contraindication to their administration is a severe local or general reaction to a previous dose.

Toxoids �They are prepared by detoxifying the exotoxins of some bacteria rendering them antigenic but not pathogenic.

Surface antigen (recombinant) vaccines. �It is prepared by cloning HBs. Ag gene in yeast cells where it is expressed. HBs. Ag produced is then used for vaccine preparations. �Their efficacy and safety also appear to be high.
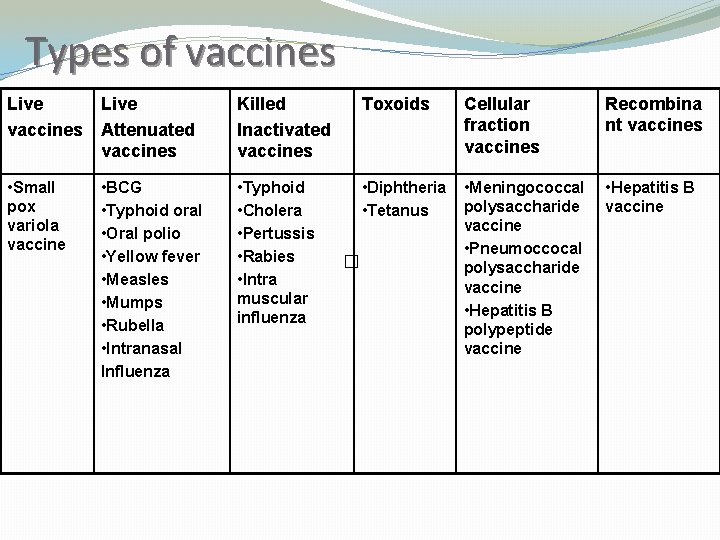
Types of vaccines Live vaccines Attenuated vaccines Killed Inactivated vaccines Toxoids Cellular fraction vaccines Recombina nt vaccines • Small pox variola vaccine • Typhoid • Cholera • Pertussis • Rabies • Intra muscular influenza • Diphtheria • Tetanus • Meningococcal polysaccharide vaccine • Pneumoccocal polysaccharide vaccine • Hepatitis B polypeptide vaccine • Hepatitis B vaccine • BCG • Typhoid oral • Oral polio • Yellow fever • Measles • Mumps • Rubella • Intranasal Influenza �

Diseases Caused by Bacteria Diphtheria Haemophilus influenza type b Meningococcal disease Pertussis Pneumococcal disease Tetanus
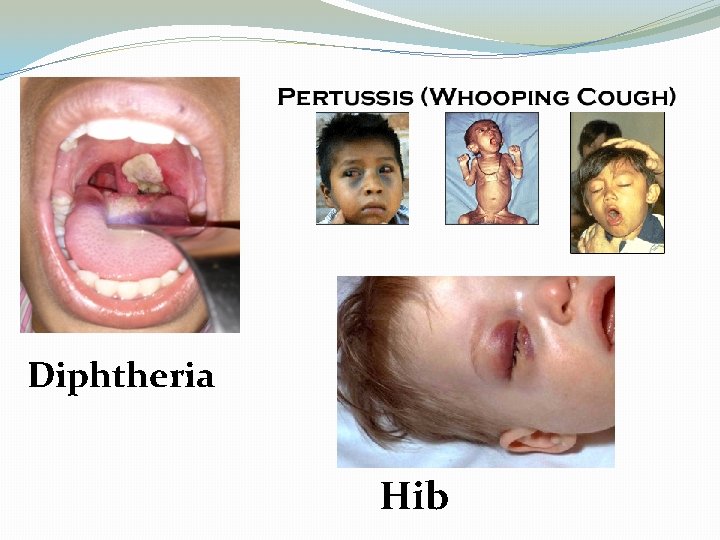
Diphtheria Hib

Diseases Caused by Viruses �Hepatitis A �Hepatitis B �Shingles �Human papillomavirus(HPV) �Influenza �Measles �Mumps �Rotavirus �Chickenpox � Polio
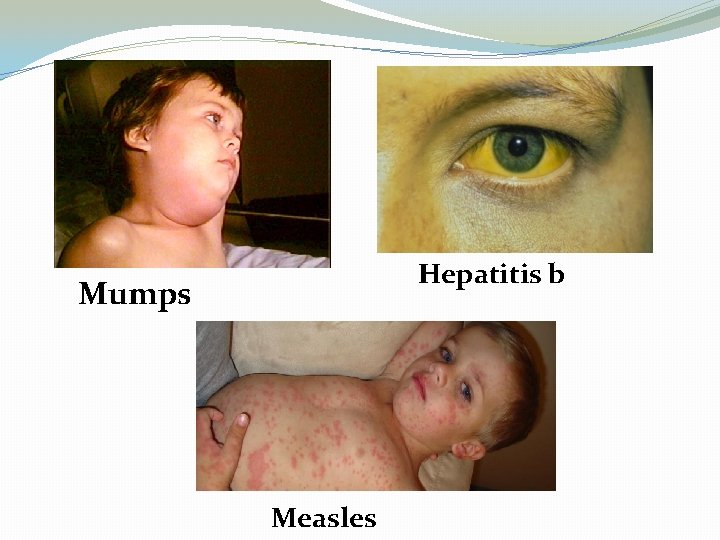
Hepatitis b Mumps Measles

Routes of administration �Deep subcutaneous or intramuscular route (most vaccines) �Oral route (Sabine vaccine, oral BCG vaccine) �Intradermal route (BCG vaccine) �Scarification (small pox vaccine) �Intranasal route (live attenuated influenza vaccine)
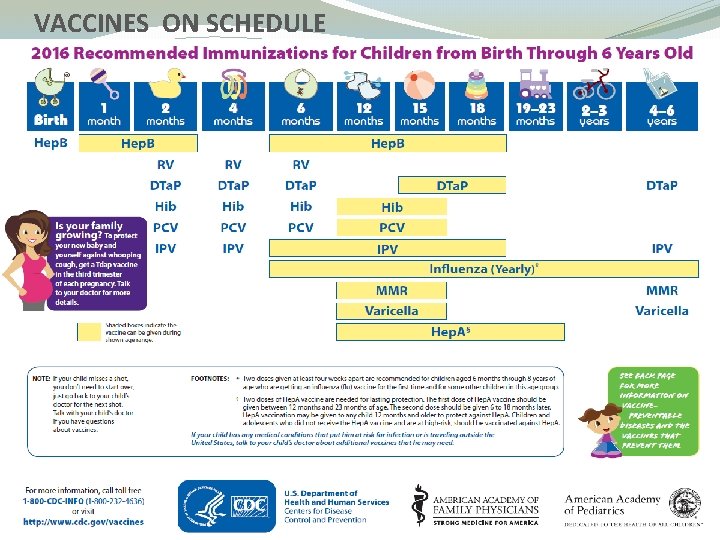
VACCINES ON SCHEDULE


The process (nursing roll): �Assess the patient’s immunization history �Check the recommended immunization schedule �Screen for contraindications and precautions �Educate the parent and patient �Administer all needed vaccines �Document administered vaccines �Inform parents and patients when vaccines are needed next

GENERAL PRECAUTIONS TO BE TAKEN: �The risk of adverse reactions can be reduced by proper sterilization of syringes and needles, by proper selection of the subject and the product. � Measles and BCG vaccines should be reconstituted only with the diluents supplied by the manufacturer.

�Reconstituted vaccine should be discarded at the end of each immunization session and NEVER retained for use in subsequent sessions. In the refrigerator of the immunization centre, no other drug and substances should be stored beside vaccines. �Training of immunization worker and their close supervision to ensure that proper procedures are being followed are essential to prevent complications and deaths following immunization.

Adolescents Vaccines

Four Vaccines Are Recommended for ALL Preteens at age 11 or 12 years q Tetanus-diphtheria-acellular pertussis vaccine (Tdap) q Meningococcal conjugate vaccine (MCV 4) q Human papillomavirus vaccine (HPV) q Influenza (flu) vaccine

Vaccines Recommended for Adolescents q Polio q Hepatitis B q MMR q Hepatitis A

Vaccines Recommended for Adolescents with High-Risk Conditions q Pneumococcal conjugate vaccine (PCV 13) q Pneumococcal polysaccharide vaccine (PPSV 23)

Vaccinations for special health status persons: �Immuno-compromised persons ( Leukemia, lymphoma, HIV, malignancy…) �Hemodialysis and transplantation should receive the following vaccines according to their situation: HBV, Influenza, Pneumococcal vaccines

Vaccine Adverse Reactions �Adverse reaction �extraneous effect caused by vaccine "side effect" �Adverse event � any event following a vaccine � may be true adverse reaction � may be only coincidental

Vaccine Adverse Reactions �Local pain, swelling, redness at site of injection � common with inactivated vaccines � usually mild and self-limited � �Systemic fever, malaise, headache � nonspecific � may be unrelated to vaccine �

Article:

Summary:

Conclusion: �Immunization is one of the most costeffective health interventions. �Investing in vaccines SAVES more money than it costs.

References: �www. pitt. edu. com �medicine. missouri. edu/childhealth �https: //www. cdc. gov/primarycare/. . . /adolescent_vacci nes_module. ppt
- Slides: 38