MALNUTRITION IN THE ACUTE CARE SETTING Mackenzie Martindale
















- Slides: 21

MALNUTRITION IN THE ACUTE CARE SETTING Mackenzie Martindale, Silvia Lopez-Ross, Nicole Treas Aramark Distance Dietetic Internship Emerging Trends Research Project Spring 2016

Learning Objectives • Understand the meaning of malnutrition • Recognize the prevalence of malnutrition in the acute care setting • Understand the causes and consequences of the problem • Describe role of Registered Dietitian (RD) language in accurate coding of malnutrition • Learn the benefits of diagnosing malnutrition • Use of the Nutrition Focused Physical Exam • Hospital reimbursement for malnutrition

Malnutrition: What is it? Malnutrition is a state of nutrition in which a deficiency, excess, or imbalance of energy, protein and other nutrients cause adverse effects on body structure, function, and the clinical outcome of the patient. Malnutrition can be both undernutrition and overnutrition. § Starvation § Chronic Disease § Acute Disease/Injury § Kwashiorkor § Marasmus White JV, Guenter P, Jensen G, et al. Consensus Statement: Academy of Nutrition and Dietetics and America Society for Parenteral and Enteral Nutrition: Characteristics Recommended for the Identification and Documentation of Adult Malnutrition (Undernutrition), J Acad Nutr Diet. 2012; 112: 730 -783.

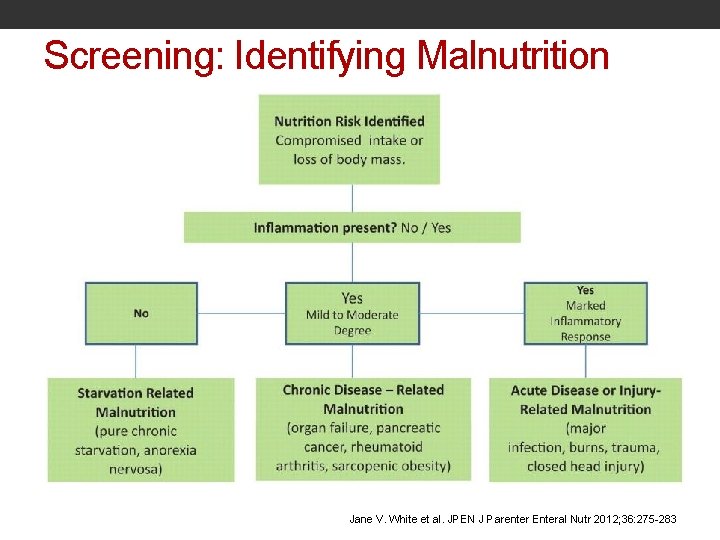
Screening: Identifying Malnutrition Jane V. White et al. JPEN J Parenter Enteral Nutr 2012; 36: 275 -283

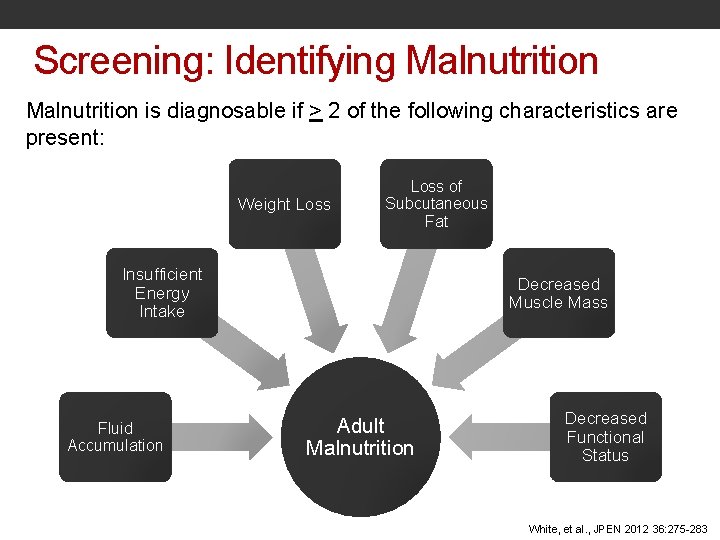
Screening: Identifying Malnutrition is diagnosable if > 2 of the following characteristics are present: Weight Loss of Subcutaneous Fat Insufficient Energy Intake Fluid Accumulation Decreased Muscle Mass Adult Malnutrition Decreased Functional Status White, et al. , JPEN 2012 36: 275 -283

Diagnosing: Types of Malnutrition Starvation Related Malnutrition • Little or no inflammation • Pure chronic starvation e. g. anorexia nervosa Chronic Disease Related Malnutrition • Mild to moderate inflammation • Examples: organ failure, pancreatic cancer Acute Disease Associated Malnutrition • Severe acute systemic inflammatory response e. g. trauma, ARDS, SIRS, severe burns, abdominal surgery White, et al. , JPEN 2012: 36: 275 -283

The Registered Dietitian’s Role • RD’s have the opportunity to: • Increase awareness of hospital malnutrition • Improve patient outcomes by working collaboratively with physicians and nurses on an interdisciplinary health care team to administer the best nutrition interventions. • RD’s can help to properly identify, document, and advocate for patients who enter the hospital with malnutrition or who develop malnutrition during their hospital stay. Todaysdietitian. com. Hospital Malnutrition — Standardized Guidelines Take Center Stage. 2015. Available at: http: //www. todaysdietitian. com/newarchives/010614 p 40. shtml. Accessed December 21, 2015.

Nutrition Assessment (RD) • Medical History • Ex. Congestive Heart Failure, Crohn’s Disease, Gastric Bypass surgery, Dementia, Depression • Nutrition/Diet History • Ex. Meal skipping, food insecurity, ability to feed/prepare meals, decreased appetite • Weight History/Body Changes • Ex. Weight loss parameters, decrease in muscle/fat mass, redistribution of weight, • GI Symptoms • Ex. Malabsorption disorders, chronic diarrhea, nausea/vomiting, abdominal pain • Functional Skills • Ex. Hand grip strength

Nutrition Assessment (RD) Nutrition Focused Physical Exam • Designed to evaluate muscle and/or subcutaneous fat loss • Subcutaneous fat loss: • Orbital fat pads, buccal fat, triceps, ribs • Muscle loss • Temples, clavicle, shoulder, scapula, interosseous, quadriceps/thigh, calf • Vitamin/Mineral deficiencies • Hair, eyes, mouth (oral mucosa), lips, gums, tongue, nails, skin • Fluid Accumulation • Upper body, lower extremities, sacral

Importance of Diagnosing Malnutrition • High prevalence in hospitalized patients • 15 -60% of adults • Consequences of under diagnosing malnutrition: • Poor wound healing • Increased rate of infection • Greater length of stay • Increased readmission for elderly patients • Increased costs to the patient and facility • Increased morbidity and mortality • Suboptimal surgical outcome White JV, Guenter P, Jensen G, et al. Consensus Statement: Academy of Nutrition and Dietetics and America Society for Parenteral and Enteral Nutrition: Characteristics Recommended for the Identification and Documentation of Adult Malnutrition (Undernutrition), J Acad Nutr Diet. 2012; 112: 730 -783.

Albumin and Malnutrition? • Serum albumin does not correlate with weight loss • Levels to not change with consistency or predictability in patients with weight loss, restricted calorie intake, or negative nitrogen balance • Factors effecting serum albumin level include: • Inflammation (more predictable indication) • Fluid accumulation Does serum albumin correlate with weight loss in four models of prolonge protein-energy restriction: anorexia nervosa, non-malabsorptive gastric partitioning bariatric surgery, calorie-restricted diets or starvation? Available at: http: //www. andeal. org/topic. cfm? cat=4302. Academy of Nutrition and Dietetics. Accessed January 3, 2016. Does serum prealbumin correlate with weight loss in four models of prolonge protein-energy restriction: anorexia nervosa, non-malabsorptive gastric partitioning bariatric surgery, calorie-restricted diets or starvation? Available at: http: //www. andeal. org/topic. cfm? cat=4302. Academy of Nutrition and Dietetics. Accessed January 3, 2016. White JV, Guenter P, Jensen G, Malone A, Schofiled M, The Academy Malnutrition Work Group; the ASPEN Malnutrition Task Force; and the ASPEN Board of Directors. Consensus Statement: Academy of Nutrition and Dietetics and America Society for Parenteral and Enteral Nutrition: Characteristics Recommended for the Identification and Documentation of Adult Malnutrition (Undernutrition), J Parenter Enteral Nutr. 2012: 36: 275 -283.

Diagnosing Malnutrition: Why is this important? • Improved reimbursement and benchmarking • Prospective Payment System • MS-DRG • Levels of Severity • Major Complication/Comorbidity (MCC) • Complication/Comorbidity (CC) Condition Acute Myocardial Infarction MS-DRG Contributing Condition Potential Reimbursement 282 No CC/MCC $5, 540 281 +CC $7, 756 280 +MCC $12, 129 Academy of Nutrition and Dietetics: ICD 9 -CM/ICD-10 -CM Codes for MNT, 2014. Access December 20, 2015. Centers for Medicare and Medicaid Services. Acute Care Hospital Inpatient Prospective Payment System: Payment System Fact Sheet Series, 2013. Accessed December 20, 2015. Centers for Medicare and Medicaid Services. Acute Inpatient PPS, FY 2015 Final Rule Tables, 2015. Accessed December 20, 2015.

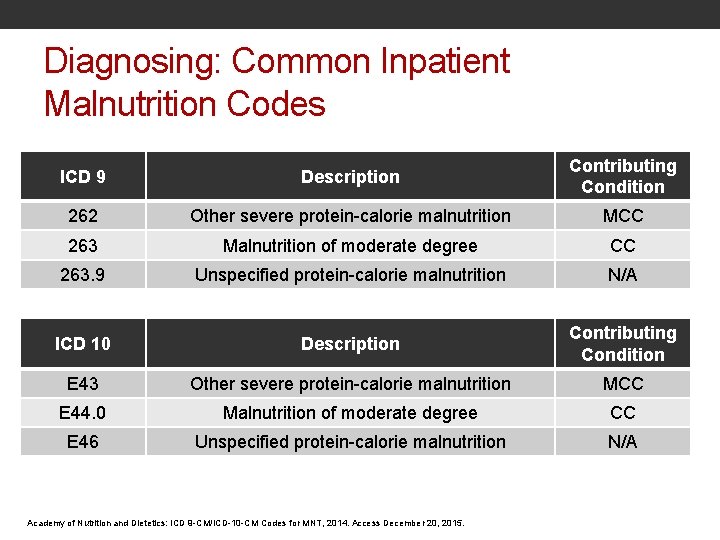
Diagnosing: Common Inpatient Malnutrition Codes ICD 9 Description Contributing Condition 262 Other severe protein-calorie malnutrition MCC 263 Malnutrition of moderate degree CC 263. 9 Unspecified protein-calorie malnutrition N/A ICD 10 Description Contributing Condition E 43 Other severe protein-calorie malnutrition MCC E 44. 0 Malnutrition of moderate degree CC E 46 Unspecified protein-calorie malnutrition N/A Academy of Nutrition and Dietetics: ICD 9 -CM/ICD-10 -CM Codes for MNT, 2014. Access December 20, 2015.

Treatment of Malnutrition in Hospitalized Patients • 1996: Joint Commission mandated nutritional screening within 24 hours of admission • Referral to RD • Encourage PO intake upon admission (if medically feasible) • Allow least restrictive diet if PO intake is decreased • Offer nutritional drink supplements when applicable • Administer EN/TPN as soon as medically feasible (when necessary) Barker LA, Gout BS, Crowe TC. Hospital Malnutrition: Prevalence, Identification and Impact on Patients and the Healthcare System. International Journal of Environmental Research and Public Health. 2011; 8(2): 514 -527. doi: 10. 3390/ijerph 8020514.

Treatment: Desired Outcomes • Improved early identification of patients at-risk for malnutrition • Precise classification and coding of malnourished patients • Earlier and more aggressive interventions for malnourished patients • Increased physician support for nutrition recommendations Kathryn Chiles RD, LD, CNSC

What’s Next? • How we determine if appropriate to complete nutrition focused physical exam: • Meet two other criteria (% PO intake, % Wt. loss, fluid status, functional status) • Current treatment plan and/or goals of care • Challenges within different hospital settings • Inpatient • Outpatient • Intensive Care Unit • Co-managed documentation with physicians • We have to work together as a care team

Review of Key Points • Acute malnutrition in hospitals related to inadequate intake is prevalent • Feeding protocols can successfully reduce calorie deficits when implemented. • However, they are not a “One Size Fits All” approach • Continuous education, monitoring, and modification of protocol • Identify opportunities for multidisciplinary involvement and investment to maximize success • Malnutrition Diagnosis increase hospital reimbursement

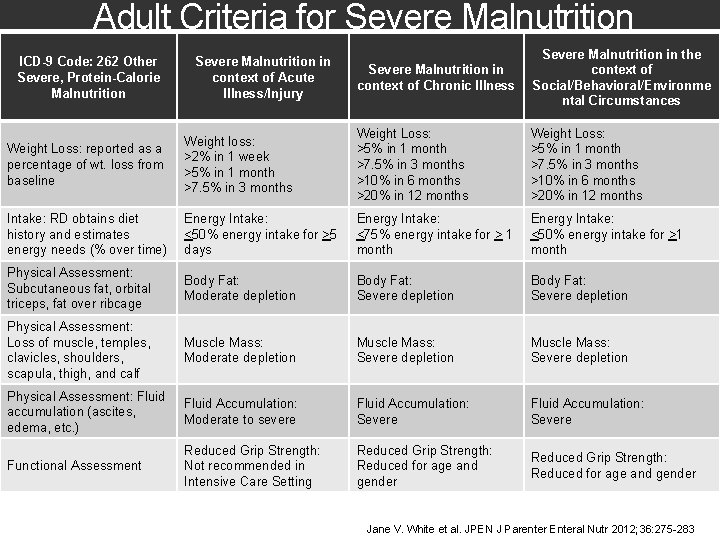
Adult Criteria for Severe Malnutrition in context of Chronic Illness Severe Malnutrition in the context of Social/Behavioral/Environme ntal Circumstances Weight Loss: reported as a percentage of wt. loss from baseline Weight loss: >2% in 1 week >5% in 1 month >7. 5% in 3 months Weight Loss: >5% in 1 month >7. 5% in 3 months >10% in 6 months >20% in 12 months Intake: RD obtains diet history and estimates energy needs (% over time) Energy Intake: <50% energy intake for >5 days Energy Intake: <75% energy intake for > 1 month Energy Intake: <50% energy intake for >1 month Physical Assessment: Subcutaneous fat, orbital triceps, fat over ribcage Body Fat: Moderate depletion Body Fat: Severe depletion Physical Assessment: Loss of muscle, temples, clavicles, shoulders, scapula, thigh, and calf Muscle Mass: Moderate depletion Muscle Mass: Severe depletion Physical Assessment: Fluid accumulation (ascites, edema, etc. ) Fluid Accumulation: Moderate to severe Fluid Accumulation: Severe Functional Assessment Reduced Grip Strength: Not recommended in Intensive Care Setting Reduced Grip Strength: Reduced for age and gender ICD-9 Code: 262 Other Severe, Protein-Calorie Malnutrition Severe Malnutrition in context of Acute Illness/Injury Jane V. White et al. JPEN J Parenter Enteral Nutr 2012; 36: 275 -283

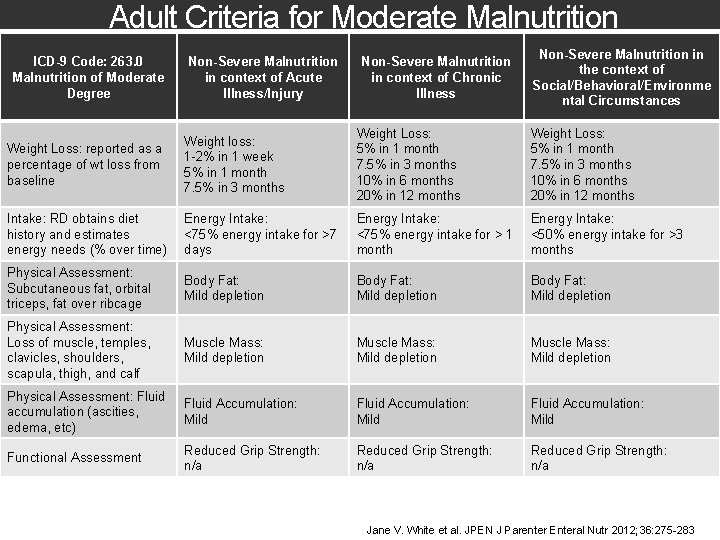
Adult Criteria for Moderate Malnutrition ICD-9 Code: 263. 0 Malnutrition of Moderate Degree Non-Severe Malnutrition in context of Acute Illness/Injury Non-Severe Malnutrition in context of Chronic Illness Non-Severe Malnutrition in the context of Social/Behavioral/Environme ntal Circumstances Weight Loss: reported as a percentage of wt loss from baseline Weight loss: 1 -2% in 1 week 5% in 1 month 7. 5% in 3 months Weight Loss: 5% in 1 month 7. 5% in 3 months 10% in 6 months 20% in 12 months Intake: RD obtains diet history and estimates energy needs (% over time) Energy Intake: <75% energy intake for >7 days Energy Intake: <75% energy intake for > 1 month Energy Intake: <50% energy intake for >3 months Physical Assessment: Subcutaneous fat, orbital triceps, fat over ribcage Body Fat: Mild depletion Physical Assessment: Loss of muscle, temples, clavicles, shoulders, scapula, thigh, and calf Muscle Mass: Mild depletion Physical Assessment: Fluid accumulation (ascities, edema, etc) Fluid Accumulation: Mild Functional Assessment Reduced Grip Strength: n/a Jane V. White et al. JPEN J Parenter Enteral Nutr 2012; 36: 275 -283

Thank you! If you have questions please email us at: martindale-mackenzie@aramark. com (CHI St. Luke’s Medical Center) Treas-nicole 2@aramark. com (Williamsport Regional Medical Center) Lopezross-silvia@aramark. com (Bronx Lebanon Medical Center, Wycoff Hospital)

References White JV, Guenter P, Jensen G, Malone A, Schofiled M, The Academy Malnutrition Work Group; the ASPEN Malnutrition Task Force; and the ASPEN Board of Directors. Consensus Statement: Academy of Nutrition and Dietetics and America Society for Parenteral and Enteral Nutrition: Characteristics Recommended for the Identification and Documentation of Adult Malnutrition (Undernutrition), J Parenter Enteral Nutr. 2012: 36: 275 -283. Etiology-based malnutrition definitions. Adapted with permission from Jensen GL, Bistrian B, Roubenoff R, Heimburger DC. Malnutrition syndromes: a conundrum vs continuum. JPEN J Parenter Enteral Nutr. 2009; 33: 710. Does serum albumin correlate with weight loss in four models of prolonge protein-energy restriction: anorexia nervosa, nonmalabsorptive gastric partitioning bariatric surgery, calorie-restricted diets or starvation? Available at: http: //www. andeal. org/topic. cfm? cat=4302. Academy of Nutrition and Dietetics. Accessed January 3, 2016. Does serum prealbumin correlate with weight loss in four models of prolonge protein-energy restriction: anorexia nervosa, nonmalabsorptive gastric partitioning bariatric surgery, calorie-restricted diets or starvation? Available at: http: //www. andeal. org/topic. cfm? cat=4302. Academy of Nutrition and Dietetics. Accessed January 3, 2016. Barker LA, Gout BS, Crowe TC. Hospital Malnutrition: Prevalence, Identification and Impact on Patients and the Healthcare System. International Journal of Environmental Research and Public Health. 2011; 8(2): 514 -527. doi: 10. 3390/ijerph 8020514.