King Khalid University Hospital Department of Obstetrics Gynecology

King Khalid University Hospital Department of Obstetrics & Gynecology Course 482 Postpartum Haemorrhage

Definition – Any blood loss than has potential to produce or produces hemodynamic instability Incidence – About 5% of all deliveries

Definition l >500 ml after completion of the third stage, 5% women loose >1000 ml at vag delivery l >1000 ml after C/S l >1400 ml for elective Cesarean-hyst l >3000 -3500 ml for emergent Cesarean -hyst

l woman with normal pregnancyinduced hypervolemia increases blood-volume by 30 -60% = 1 -2 L l therfore, tolerates similar amount of blood loss at delivery l hemorrhage after 24 hrs = late PPH

Hemostasis at placental site At term, 600 ml/min of blood flows through intervillous space l Most important factor for control of bleeding from placenta site = contraction and retraction of myometrium to compress the vessels severed with placental separation l Incomplete separation will prevent appropriate contraction l

Etiology of Postpartum Haemorrhage Tone Tissue Trauma Thrombin Uterine atony 95% Retained tissue/clots laceration, rupture, inversion coagulopathy

Predisposing factors- Intrapartum l Operative delivery l Prolonged or rapid labour l Induction or agumentation l Choriomnionitis l Shoulder dystocia l Internal podalic version l coagulopathy

Predisposing Factors- Antepartum l Previous PPH or manual removal l Abruption/previa l Fetal demise l Gestational hypertension l Over distended uterus l Bleeding disorder

Postpartum causes l Lacerations or episiotomy l Retained placental/ placental abnormalities l Uterine rupture / inversion l Coagulopathy

Prevention Be prepared l Active management of third stage l – – – Prophylactic oxytocin 10 U IM 5 U IV bolus 10 -20 U/L N/S IV @ 100 -150 ml/hr Early cord clamping and cutting Gentle cord traction with surapubic countertraction

Remember! Blood loss is often underestimated l Ongoing trickling can lead to significant blood loss l Blood loss is generally well tolerated to a point l

Managementl l l talk to and assess patient Get HELP! Large bore IV access Crystalloid-lots! CBC/cross-match and type Foley catheter

Diagnosis ? Assess in the fundus l Inspect the lower genital tract l Explore the uterus l – Retained placental fragments – Uterine rupture – Uterine inversion l Assess coagulation

Management- Assess the fundus l l l l Simultaneous with ABC’s Atony is the leading case of PPH Bimanual massage Rules out uterine inversion May feel lower tract injury Evacuate clot from vagina and/ or cervix May consider manual exploration at this time
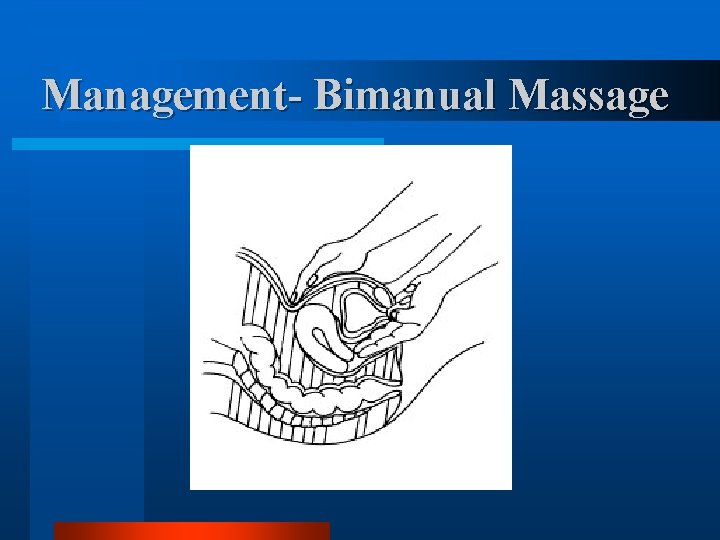
Management- Bimanual Massage

Management- Manual Exploration l Manual exploration will: – Rule out the uterine inversion – Palpate cervical injury – Remove retained placenta or clot from uterus – Rule out uterine rupture or dehiscence
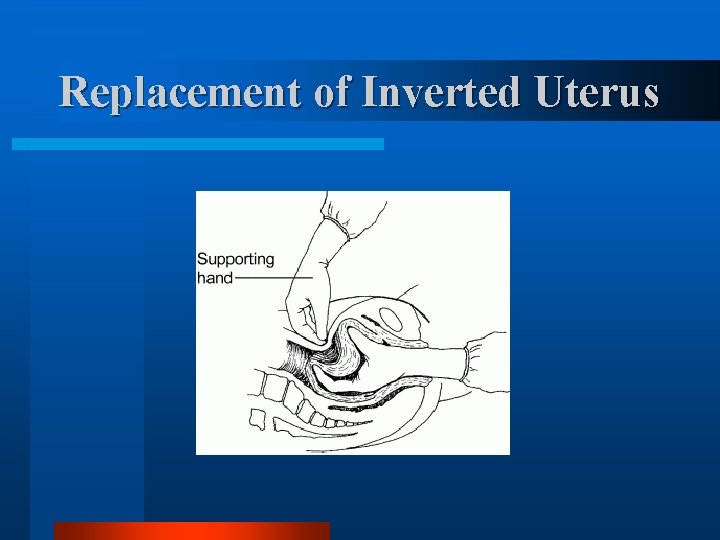
Replacement of Inverted Uterus

Management- Oxytocin l 5 units IV bolus l 20 units per L N/S IV wide open l 10 units intramyometrial given transabdominally
Replacement of Inverted Uterus
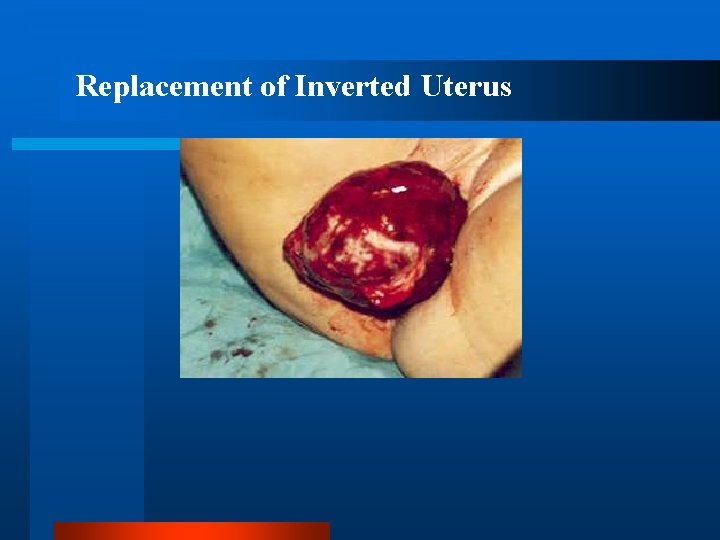
Replacement of Inverted Uterus

Management- Additional Uterotonics l Ergometrine (caution in hypertension) –. 25 mg IM 0 r. 125 mg IV – Maximum dose 1. 25 mg l Hemabate (asthma is a relative contraindication) – 15 methyl-prostaglandin F 2 alfa – O. 25 mg IM or intramyometrial – Maximum dose 2 mg (Q 15 min- total 8 doses) l Cytotec (misoprostol) PG E 1 – 800 -1000 mcg pr


Management- Bleeding with Firm Uterus l Explore the lower genital tract l Requirements • Appropriate analgesia • Good exposure and lighting l Appropriate surgical repair • May temporize with packing

Management – ABC’s ENSURE THAT YOU ARE ALWAYS AHEAD WITH YOUR RESUSCITATION!!!! l Consider need for Foley catheter, CVP, arterial line, etc. l Consider need for more expert help

Management- Evolution Panic l Hysterectomy l l Pitocin l Prostaglandins l Happiness

MANAGEMENT OF PPH

Management- Continued Uterine Bleeding l Consider coagulopathy l Correct coagulopathy – FFP, cryoprecipitate, platelets l If coagulation is normal – Consider embolization – Prepare for O. R.

Surgical Approaches l Uterine vessel ligation l Internal iliac vessel ligation l Hysterectomy



Conclusions l l l l Be prepared Practice prevention Assess the loss Assess the maternal status Resuscitate vigorously and appropriately Diagnose the cause Treat the cause

Summary: Remember 4 Ts l Tone l Tissue l Trauma l Thrombin

Summary: remember 4 Ts “TONE” l Rule out Uterine Atony l l l Palpate fundus. Massage uterus. Oxytocin Methergine Hemabate

Summary: remember 4 Ts “Tissue” l R/O retained placenta l Inspect placenta for missing cotyledons. l Explore uterus. l Treat abnormal implantation. l

Summary: remember 4 Ts “TRAUMA” l R/O cervical or vaginal lacerations. l Obtain good exposure. l Inspect cervix and vagina. l Worry about slow bleeders. l Treat hematomas. l

Summary: remember 4 Ts l “THROMBIN” l Check labs if suspicious.

CONSUMPTIVE COAGULOPATHY (DIC) l. A complication of an identifiable, underlying pathological process against which treatment must be directed to the cause

Pregnancy Hypercoagulability l coagulation factors I (fibrinogen), VII, IX, X l plasminogen; plasmin activity l fibrinopeptide A, bthromboglobulin, platelet factor 4, fibrinogen

Pathological Activation of Coagulation mechanisms Extrinsic pathway activation by thromboplastin from tissue destruction l Intrinsic pathway activation by collagen and other tissue components l Direct activation of factor X by proteases l Induction of procoagulant activity in lymphocytes, neutrophils or platelets by stimulation with bacterial toxins l


Significance of Consumptive Coagulopathy l Bleeding l Circulatory obstruction organ hypoperfusion and ischemic tissue damage l Renal failure, ARDS l Microangiopathic hemolysis

Causes l Abruptio placentae (most common cause in obstetrics) l Sever Hemorrhage (Postpartum hge) l Fetal Death and Delayed Delivery >2 wks l Amniotic Fluid Embolus l Septicemia

Treatment l Identify and treat source of coagulopathy l Correct coagulopathy – FFP, cryoprecipitate, platelets

Fetal Death and Delayed Delivery l l l Spontaneous labour usually in 2 weeks post fetal death Maternal coagulation problems < 1 month post fetal death If retained longer, 25% develop coagulopathy Consumptive coagulopathy mediated by thromboplastin from dead fetus tx: correct coagulation defects and delivery

Amniotic Fluid Embolus l Complex condition characterized by abrupt onset of hypotension, hypoxia and consumptive coagulopathy l 1 in 8000 to 1 in 30 000 pregnancies l “anaphylactoid syndrome of pregnancy”

Amniotic Fluid Embolus l Pathophysiology: brief pulmonary and systemic hypertension transient, profound oxygen desaturation (neurological injury in survivors) secondary phase: lung injury and coagulopathy l Diagnosis is clinical

Amniotic Fluid Embolus l Management: supportive

Amniotic Fluid Embolus Prognosis: l 60% maternal mortality; profound neurological impairment is the rule in survivors l fetal: outcome poor; related to arrest-todelivery time interval; 70% neonatal survival; with half of survivors having neurological impairment

Septicemia l Due to septic abortion, antepartum pyelonephritis, puerperal infection l Endotoxin activates extrinsic clotting mechanism through TNF (tumor necrosis factor) l Treat cause

Abortion Coagulation defects from: l Sepsis (Clostridium perfringens highest at Parkland) during instrumental termination of pregnancy l Thromboplastin released from placenta, fetus, decidua or all three (prolonged retention of dead fetus)

- Slides: 51










































































