Hadron Radiotherapy Pavel Kundrt Institute of Physics Academy















- Slides: 30

Hadron Radiotherapy Pavel Kundrát Institute of Physics, Academy of Sciences of the Czech Republic, Prague Pavel. Kundrat@fzu. cz

Outline l l Introduction Hadron radiotherapy l l Principles Technical requirements Existing centres Treatment planning, mathematical modelling

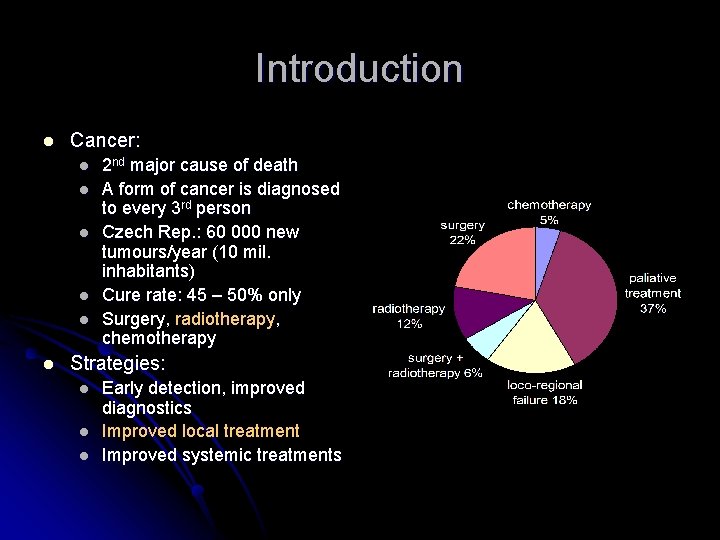
Introduction l Cancer: l l l 2 nd major cause of death A form of cancer is diagnosed to every 3 rd person Czech Rep. : 60 000 new tumours/year (10 mil. inhabitants) Cure rate: 45 – 50% only Surgery, radiotherapy , Surgery, chemotherapy Strategies: l l l Early detection, improved diagnostics Improved local treatment Improved systemic treatments

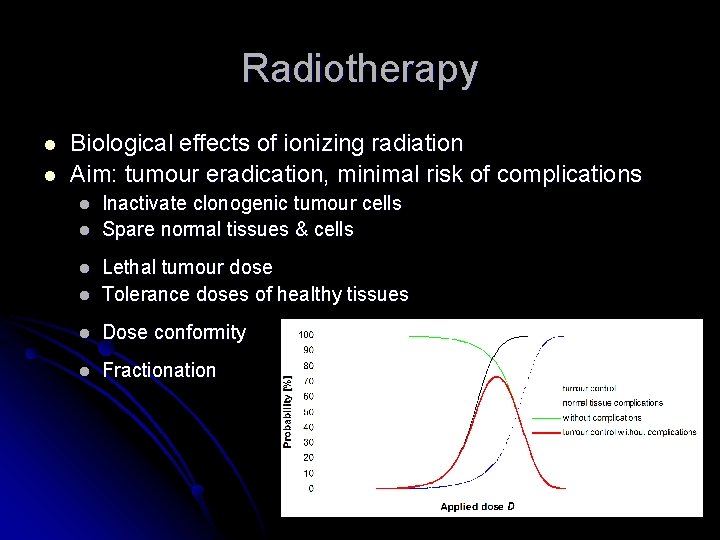
Radiotherapy l l Biological effects of ionizing radiation Aim: tumour eradication, minimal risk of complications l l Inactivate clonogenic tumour cells Spare normal tissues & cells l Lethal tumour dose Tolerance doses of healthy tissues l Dose conformity l Fractionation l

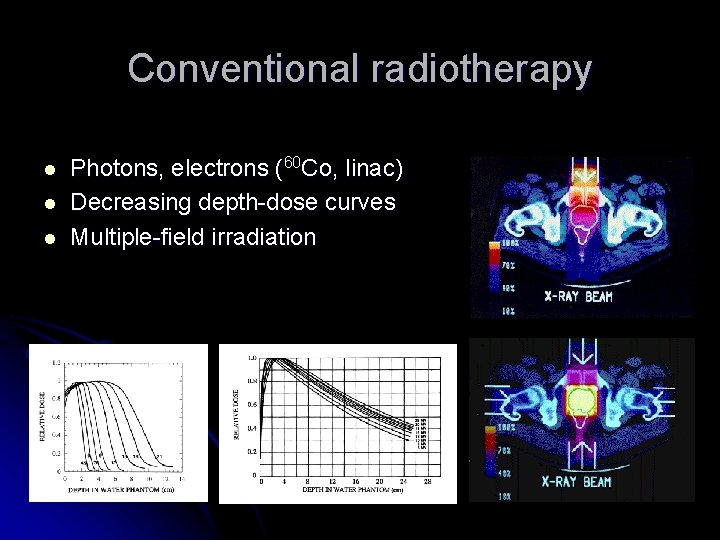
Conventional radiotherapy l l l Photons, electrons (60 Co, linac) Decreasing depth-dose curves Multiple-field irradiation

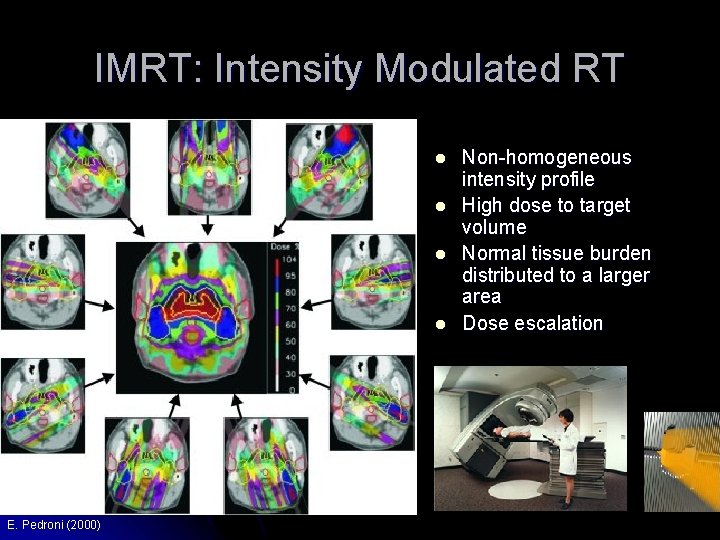
IMRT: Intensity Modulated RT l l E. Pedroni (2000) Non-homogeneous intensity profile High dose to target volume Normal tissue burden distributed to a larger area Dose escalation

Hadron radiotherapy

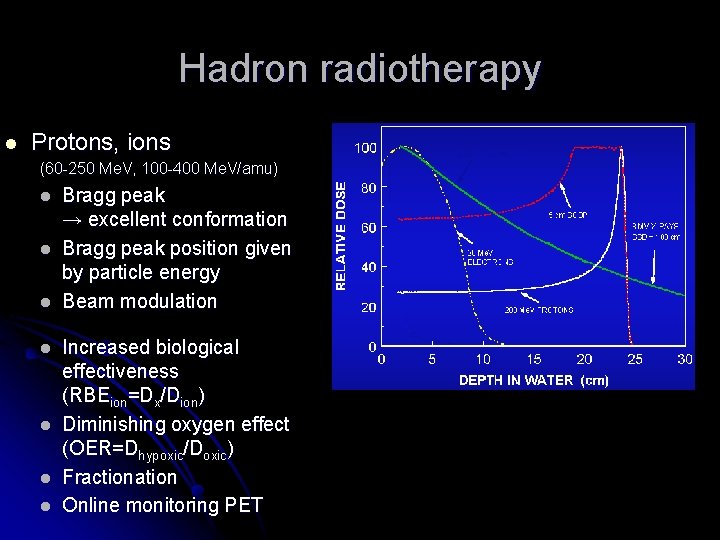
Hadron radiotherapy l Protons, ions (60 -250 Me. V, 100 -400 Me. V/amu) l l l l Bragg peak → excellent conformation Bragg peak position given by particle energy Beam modulation Increased biological effectiveness (RBEion=Dx/Dion) Diminishing oxygen effect (OER=Dhypoxic/Doxic) Fractionation Online monitoring PET

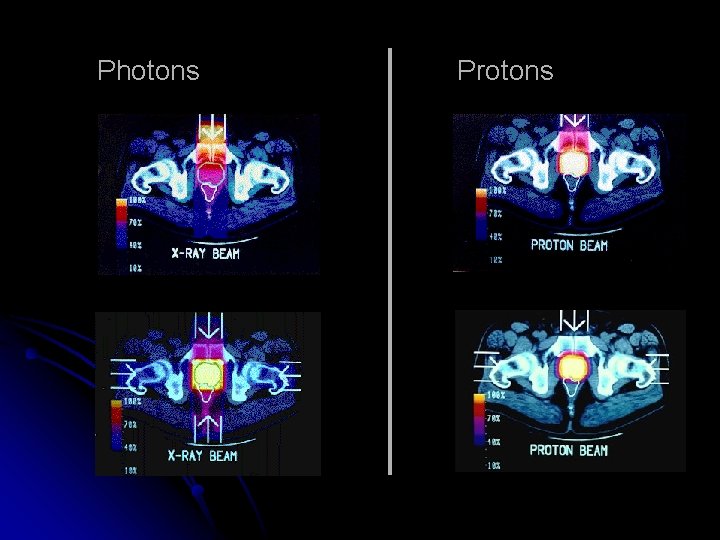
Photons Protons

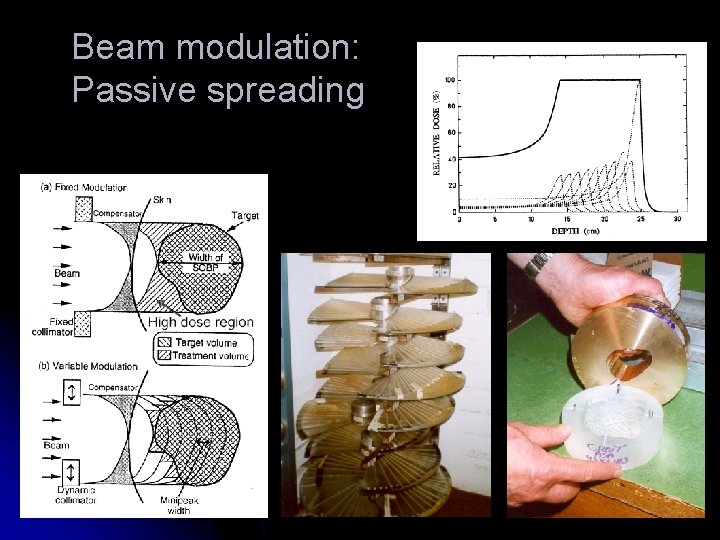
Beam modulation: Passive spreading

Beam modulation: Active scanning

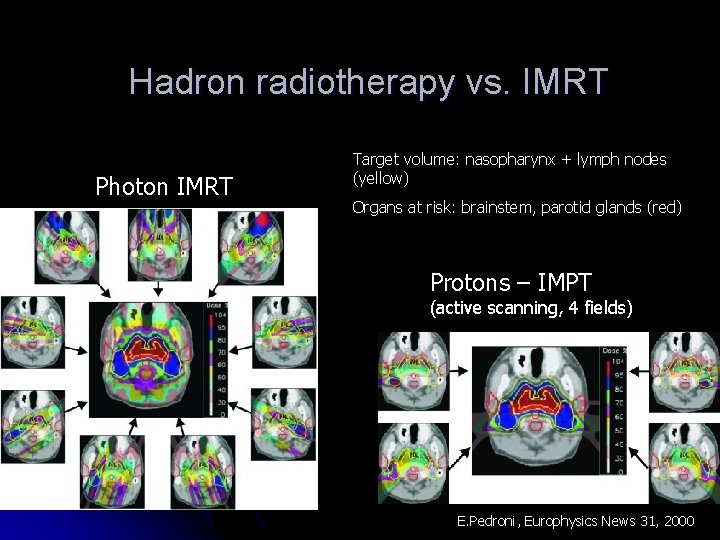
Hadron radiotherapy vs. IMRT Photon IMRT Target volume: nasopharynx + lymph nodes (yellow) Organs at risk: brainstem, parotid glands (red) Protons – IMPT (active scanning, 4 fields) E. Pedroni, Europhysics News 31, 2000

Hadrontherapy: Technical requirements l Range in tissue l l l l l Protons Ions 220 – 250 Me. V up to 400 Me. V / amu Shift in Bragg peak position (1 – 3 mm) → energy shifts (0. 5 – 1 Me. V) Field size Dose rate → particle fluence Accelerators l l 2 – 3. 5 cm 2 – 10 cm 2 – 25 cm Energy l l Eye tumours Head & neck tumours Deep seated tumours Cyclotron (IBA, Accel) Synchrotron (PIMMS, PRAMES, Optivus, Mitsubishi, Hitachi) Fixed beams (horizontal, vertical), gantry Beam modulation - passive spreading, active scanning

Hadrontherapy worldwide l Nuclear physics centres l head & neck tumours eye tumours NSCLC lung cancer prostate cancer Berkeley, Harvard (USA), Dubna, Moscow (Russia), PSI (Switzerland), Nice, Orsay (France) → medical facilities Loma Linda (CA, USA) 1991 HIMAC Chiba (Japan) 1994 NCC Kashiwa (Japan) 1998 NPTC Boston (USA) 2001 Wan Jie PTC (China) 2004 RPTC Munich (Germany) 2006 l l l Approx. 25 centres + 20 in planning (USA, Europe, Japan) Almost 50000 patients (protons + ions) Potential patients: 1000 -3000 per year / 10 mil. inhabitants Main indications: l Clinical results: 5 yrs. local control photon vs. hadron RT chordomas 17 -50% vs. 73 -83% chondrosarcomas 50 -60% vs. 90 -98% l Costs: initial costs 70 -120 mil. € (1000 pt/y) about 20 000 € / patient approx. 2 -3 x more expensive than photon RT, about the same as surgery, by far less expensive than chemotherapy l Particle Therapy Co-Operative Group (PTCOG) http: //ptcog. web. psi. ch/

Proton therapy facilities (1) l NPTC Boston 2001 l l IBA proton cyclotron, 230 Me. V Compact design (6 m diameter) Fixed energy + energy degrader Kashiwa, Japan 1998 Wan Jie PTC, China 2004 MPRI Bloomington, USA 2006 Florida PT Inst, USA 2006 Beijing, China 2007 NCC, Seoul, Korea 2006 [NPTC Boston, 2001] [IBA]

Proton therapy facilities (2) l RPTC Munich l l Superconducting cyclotron Accel, 250 Me. V protons 4 gantries (Schär AG), 1 fixed beam Plan: 4000 patients / year Tests & commissioning; operating in 2006? l PSI Villigen – PROSCAN l Synchrotrons – Loma Linda (>10000 pts since 1991), MD Anderson CC Optivus, Mitsubishi, Hitachi [Accel/Schär]

Ion therapy l Rationale: l l l Cyclotrons: ongoing research (IBA 400 Me. V/amu superconducting cyclotron) Synchrotrons: PIMMS, HICAT, Siemens, Mitsubishi l l Pulsed beam Variable energy Active scanning PIMMS: 23 m diameter l l l Physical selectivity Increased biological effectiveness, diminishing oxygen effects (→ radioresistant tumours) Online dose monitoring (PET) Hypofractionation Protons 60 -250 Me. V Carbon 120 -400 Me. V/amu Several projects within the EU

HICAT Heidelberg l l l Heavy Ion Cancer Therapy Centre p 48 -220 Me. V He 72 -330 Me. V/amu C 88 -430 Me. V/amu O 102 -430 Me. V/amu Linac: 5 m, 7 Me. V/amu Synchrotron, 20 m diameter Gantry 20 m x 13 m diameter (120 t), active scanning Preclinical operation 2006, clinical - 2007

Other p + ion hadrontherapy centres in Europe l PIMMS design l l l CNAO Pavia (Italy) 2007 ETOILE Lyon (France) Med. Austron Wiener Neustadt (Austria) Karolinska, Stockholm (Sweden) Prague? ENLIGHT network

ENLIGHT l European Network for Light Ion Hadron Therapy, European Commission, QLG 1 -CT-2002 -01574, 2002 -2005 ESTRO, CERN, EORTC, GSI Darmstadt, DKFZ Heidelberg, GHIP Heidelberg, TERA, Karolinska Institutet, ETOILE Project, Med-Austron, FZR Rossendorf, Linköping University, Hospital Virgen de la Macarena, Charles University in Prague l Workpackages: l l Epidemiology and patient selection Design and conduct of clinical trials Preparation, delivery and dosimetry of ion beams l l l l Preparation of Ion Beams Dosimetry of Ion Beams Treatment Planning Accelerator Technology Radiation biology In-situ monitoring with positron emission tomography Health-Economic Assessment ENLIGHT++ proposal (2006)

Summary – Hadron therapy l l l Excellent dose conformity Proven clinical benefits in several tumours/locations Approx. 1000 – 3000 pts/year/10 mil. inhabitants would benefit from HT Ion therapy: radioresistant tumours Costs: initial ~ 70 -120 M€, per pt ~ 20 k€

Biological effects of ionizing radiation: Mechanism and its modelling

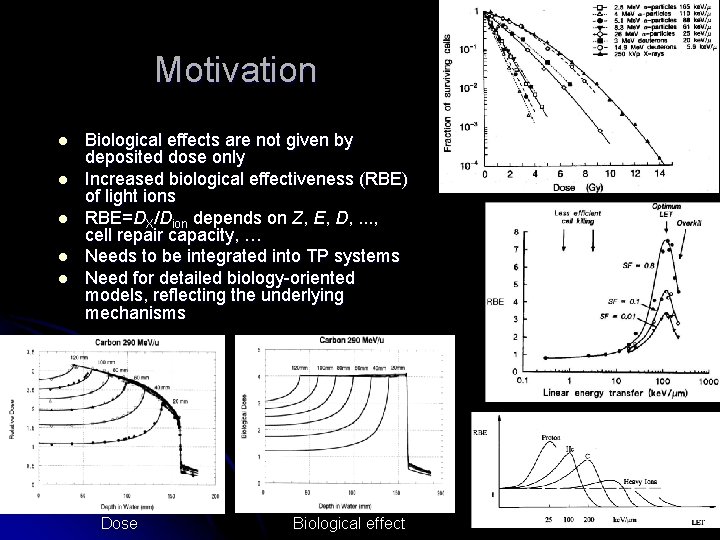
Motivation l l l Biological effects are not given by deposited dose only Increased biological effectiveness (RBE) of light ions RBE=DX/Dion depends on Z, E, D, . . . , cell repair capacity, … Needs to be integrated into TP systems Need for detailed biology-oriented models, reflecting the underlying mechanisms Dose Biological effect

Radiobiological mechanism l Physical phase (10 -18 – 10 -10 s) l l Energy transfer, excitations, ionizations, radical formation Chemical phase (10 -10 – 10 -3 s) l Diffusion, recombination, chemical reactions, DNA damage (base modification, base loss, cross-link, SSB, DSB, LMDS) l Biological phase (seconds – hours, years) l Repair processes (BER, HR, NHEJ), cellular response, apoptosis, necrosis; organ, organism

Probabilistic two-stage model Kundrát P, Lokajíček M, Hromčíková H (2005) Phys. Med. Biol. 50 1433 -1447 Kundrát P (2006) Phys. Med. Biol. (in press), ar. Xiv: physics/0509053 l Mono-energetic particles: l Number of primary particles, k: l l Transferred energy DNA damage induction l l l Pk(D) = [(h. D)k/k!]exp(-h. D) h~σ/LET ε ~ LET Lethal lesions formed by single particles … a „single-particle“ lesions Sublethal lesions … b Lethal if combined from at least 2 particles „combined“ lesions Repair processes l Repair success probability … rk Effect of k particles l Cell survival probability s(D) = Σ Pk(D) qk l l General case: l l Transferred energy Cell survival π1(ε), πk(ε)= ∫ π1(ε’) πk-1(ε-ε’) dε’ s = Σ Pk ∫qk(ε) πk(ε) dε

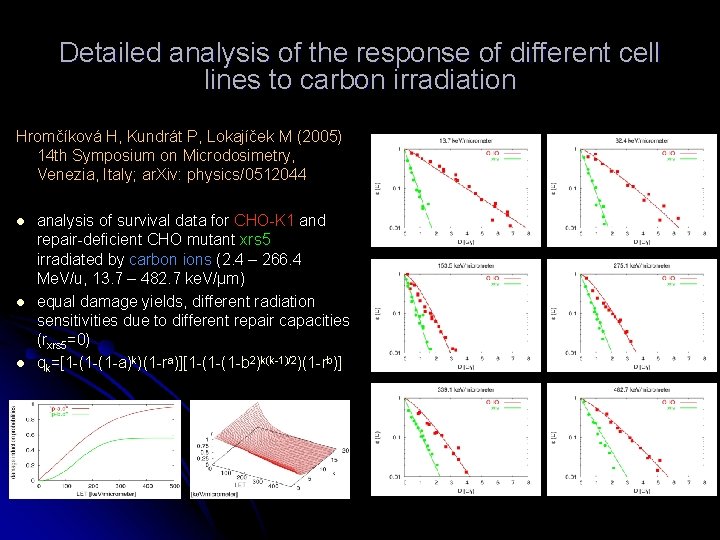
Detailed analysis of the response of different cell lines to carbon irradiation Hromčíková H, Kundrát P, Lokajíček M (2005) 14 th Symposium on Microdosimetry, Venezia, Italy; ar. Xiv: physics/0512044 l l l analysis of survival data for CHO-K 1 and repair-deficient CHO mutant xrs 5 irradiated by carbon ions (2. 4 – 266. 4 Me. V/u, 13. 7 – 482. 7 ke. V/μm) equal damage yields, different radiation sensitivities due to different repair capacities (rxrs 5=0) qk=[1 -(1 -(1 -a)k)(1 -ra)][1 -(1 -(1 -b 2)k(k-1)/2)(1 -rb)]

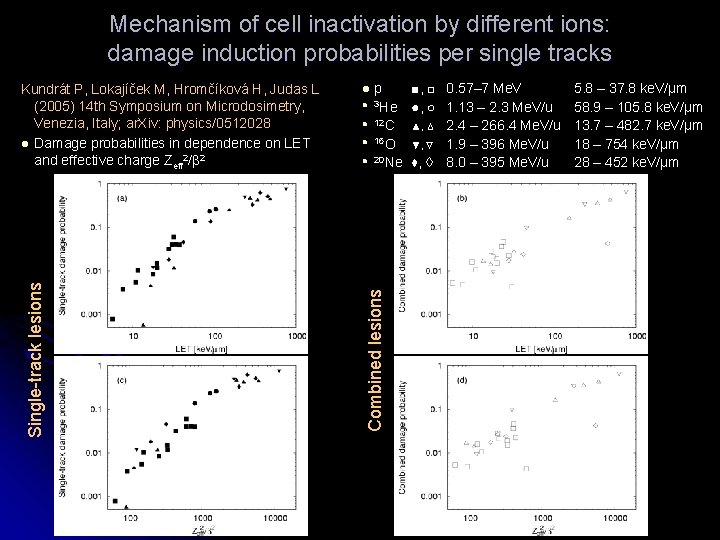
Mechanism of cell inactivation by different ions: damage induction probabilities per single tracks l l l p ■, □ 0. 57– 7 Me. V 3 He ●, ○ 1. 13 – 2. 3 Me. V/u 12 C ▲, Δ 2. 4 – 266. 4 Me. V/u 16 O ▼, 1. 9 – 396 Me. V/u 20 Ne ♦, 8. 0 – 395 Me. V/u Combined lesions Single-track lesions Kundrát P, Lokajíček M, Hromčíková H, Judas L (2005) 14 th Symposium on Microdosimetry, Venezia, Italy; ar. Xiv: physics/0512028 l Damage probabilities in dependence on LET and effective charge Zeff 2/β 2 5. 8 – 37. 8 ke. V/μm 58. 9 – 105. 8 ke. V/μm 13. 7 – 482. 7 ke. V/μm 18 – 754 ke. V/μm 28 – 452 ke. V/μm

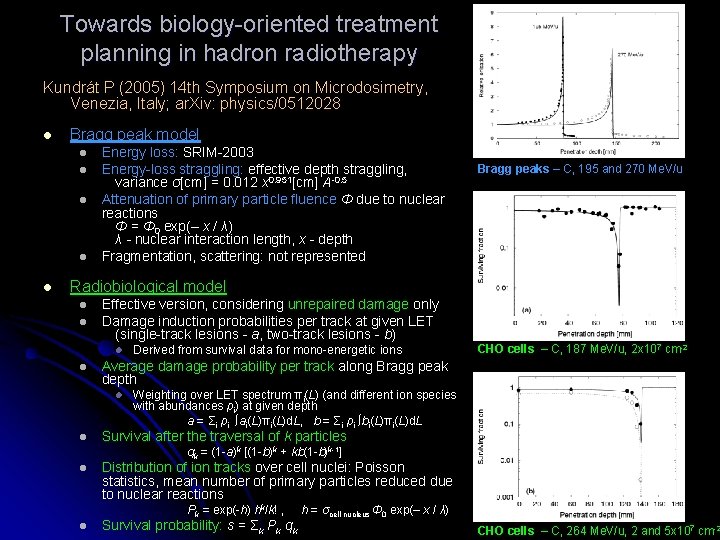
Towards biology-oriented treatment planning in hadron radiotherapy Kundrát P (2005) 14 th Symposium on Microdosimetry, Venezia, Italy; ar. Xiv: physics/0512028 l Bragg peak model l l Energy loss: SRIM-2003 Energy-loss straggling: effective depth straggling, variance σ[cm] = 0. 012 x 0. 951[cm] A-0. 5 Attenuation of primary particle fluence Φ due to nuclear reactions Φ = Φ 0 exp(– x / λ) λ - nuclear interaction length, x - depth Fragmentation, scattering: not represented Bragg peaks – C, 195 and 270 Me. V/u Radiobiological model l l Effective version, considering unrepaired damage only Damage induction probabilities per track at given LET (single-track lesions - a, two-track lesions - b) l l CHO cells – C, 187 Me. V/u, 2 x 107 cm-2 Average damage probability per track along Bragg peak depth l l Derived from survival data for mono-energetic ions Weighting over LET spectrum πi(L) (and different ion species with abundances ρi) at given depth a = Σi ρi ∫ai(L)πi(L)d. L, b = Σi ρi ∫bi(L)πi(L)d. L Survival after the traversal of k particles qk = (1 -a)k [(1 -b)k + kb(1 -b)k-1] l Distribution of ion tracks over cell nuclei: Poisson statistics, mean number of primary particles reduced due to nuclear reactions Pk = exp(-h) hk/k! , h = σcell nucleus Φ 0 exp(– x / λ) l Survival probability: s = Σk Pk qk CHO cells – C, 264 Me. V/u, 2 and 5 x 107 cm-2

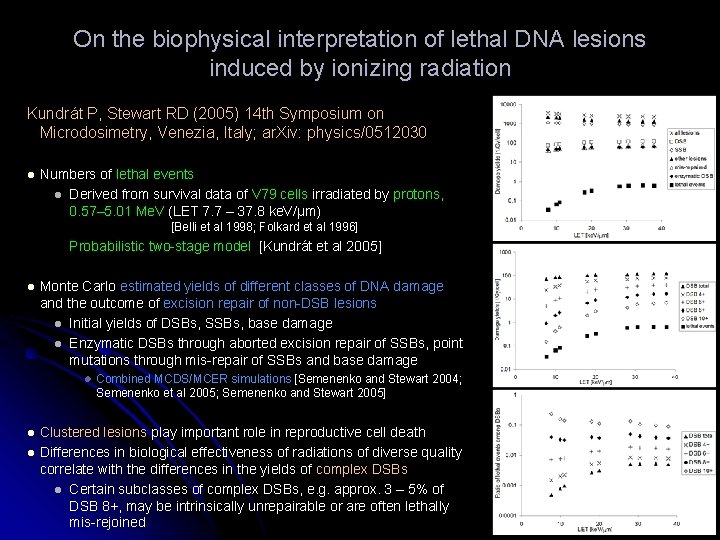
On the biophysical interpretation of lethal DNA lesions induced by ionizing radiation Kundrát P, Stewart RD (2005) 14 th Symposium on Microdosimetry, Venezia, Italy; ar. Xiv: physics/0512030 l Numbers of lethal events l Derived from survival data of V 79 cells irradiated by protons, 0. 57– 5. 01 Me. V (LET 7. 7 – 37. 8 ke. V/µm) [Belli et al 1998; Folkard et al 1996] Probabilistic two-stage model [Kundrát et al 2005] l Monte Carlo estimated yields of different classes of DNA damage and the outcome of excision repair of non-DSB lesions l Initial yields of DSBs, SSBs, base damage l Enzymatic DSBs through aborted excision repair of SSBs, point mutations through mis-repair of SSBs and base damage l l l Combined MCDS/MCER simulations [Semenenko and Stewart 2004; Semenenko et al 2005; Semenenko and Stewart 2005] Clustered lesions play important role in reproductive cell death Differences in biological effectiveness of radiations of diverse quality correlate with the differences in the yields of complex DSBs l Certain subclasses of complex DSBs, e. g. approx. 3 – 5% of DSB 8+, may be intrinsically unrepairable or are often lethally mis-rejoined

Summary – Modelling l P 2 S model l l Biology-oriented model DNA damage & repair Systematic description of survival curves → TCP, NTCP models Future work l l l Relate damage induction to track structure Interpretation of lethal events TCP, NTCP models Pavel. Kundrat@fzu. cz