Radiation Sources in Radiotherapy External Beam Radiotherapy IAEA

Radiation Sources in Radiotherapy External Beam Radiotherapy IAEA International Atomic Energy Agency Day 7 – Lecture 4

Objective To become familiar with the radiation sources, devices and ancillary equipment used in external beam radiotherapy. IAEA 2

Contents • Treatment planning systems; • Radiotherapy simulators; • Superficial / orthovoltage units; • Cobalt-60 units including Gamma-knife; • Linear accelerators; • Computed Tomography (CT) scanners for radiotherapy; • Multileaf Collimators (MLC). IAEA 3

Clinical Objectives To deliver a dose and dose distribution that is adequate for tumor control but which also minimizes complications in normal tissue. Note: It is not the role of the Regulatory Body to evaluate the clinical decisions of medical practitioners authorized to prescribe radiotherapy treatments. IAEA 4
Treatment Planning Prescription Planning IAEA Treatment Very important for optimization of protection in medical exposures

Treatment Planning • About 1/3 of problems are directly related to treatment planning; • Problems may affect an individual patient or cohort of patients. IAEA Safety Report Series 17; 2000 “Lessons learned from accidental exposures in radiotherapy” IAEA 6
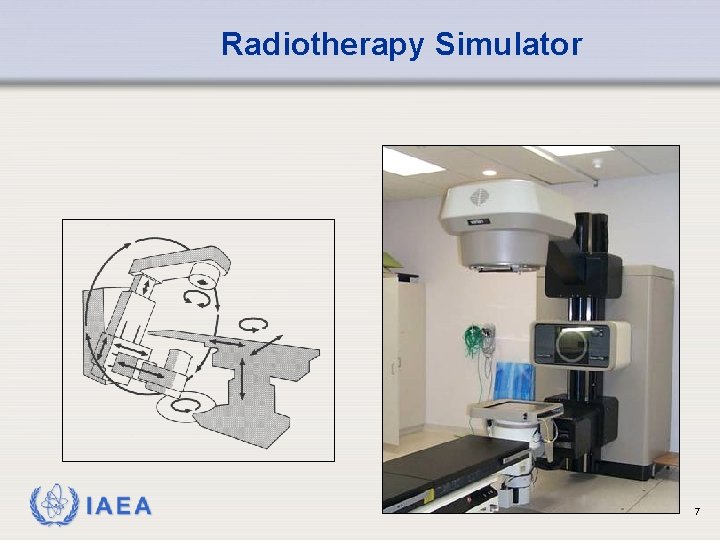
Radiotherapy Simulator IAEA 7

External Beam Equipment Therapeutic x-ray equipment operates in the range of: • 10 k. Vp - 150 k. Vp (superficial); • 150 k. Vp - 400 k. Vp (orthovoltage / deep); Radioactive sources ( γ ray equipment). • Cobalt 60 & Caesium 137 Megavoltage electron accelerators for X and electron therapy • Linear accelerator IAEA 8

Typical Radiation Levels Cobalt-60 teletherapy • Source activity may be around 400 TBq (~10, 000 Ci); • Average radiation leakage (beam off) should not exceed 0. 02 m. Gy/h at 1 m i. e. it would take 50 hours exposure for 1 m. Sv; • In general, minimize the time spent in the treatment room. IAEA 9

Typical radiation levels (cont) Linear accelerator turned off • There is no useful radiation beam when turned off; • However, immediately after higher energy beams (> 10 Me. V) are turned off there may be induced radioactivity but typically with very short half lives (seconds to minutes); • It is suggested that room entry be briefly delayed, especially after long exposures. IAEA 10

Superficial and Orthovoltage x-ray equipment Superficial • 40 k. Vp to 120 k. Vp Orthovoltage (“deep”) • 150 k. Vp to 400 k. Vp • treat small skin lesions to a depth of ~ 5 cm • treat skin lesions, bone metastases to a depth of ~ 20 cm • maximum applicator size typically < 7 cm diameter • use applicators or diaphragm • typical SSD < 30 cm • beam quality (HVL) typically 0. 5 to 8 mm Al IAEA • SSD 30 to 60 cm • beam quality (HVL) typically 0. 2 to 5 mm Cu 11
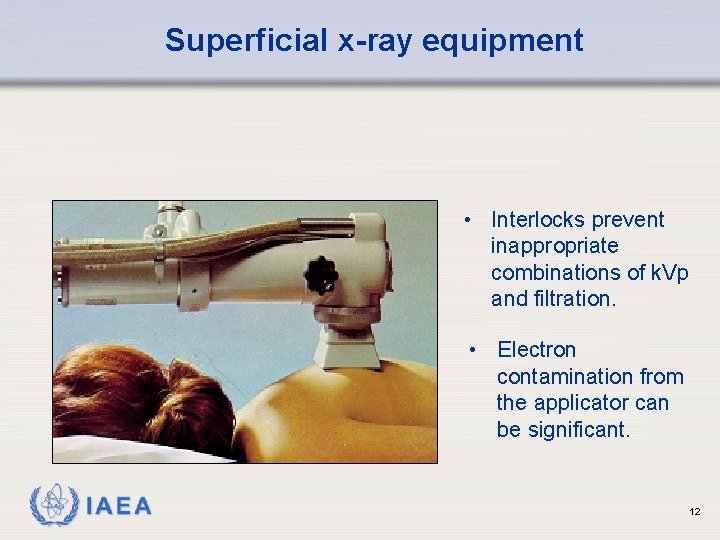
Superficial x-ray equipment • Interlocks prevent inappropriate combinations of k. Vp and filtration. • Electron contamination from the applicator can be significant. IAEA 12

Superficial x-ray equipment (cont) • Dose is highly dependent on source -skin distance, filtration and applicator area. IAEA 13

Superficial x-ray equipment (cont) Provides a range of k. Vp, m. A and filtration Filters are used to absorb low energy photons which otherwise may unnecessarily increase skin dose. IAEA 14

Issues with Superficial radiotherapy • Short focus to skin distance (FSD) and hence high output and large influence of inverse square law • Calibration difficult due to strong dose gradient i. e. dose fall off and electron contamination IAEA

Issues with superficial therapy • Dose determined by a timer • on/off effects must be considered • Photon beams may be contaminated with electrons scattered from the applicator IAEA Control panel
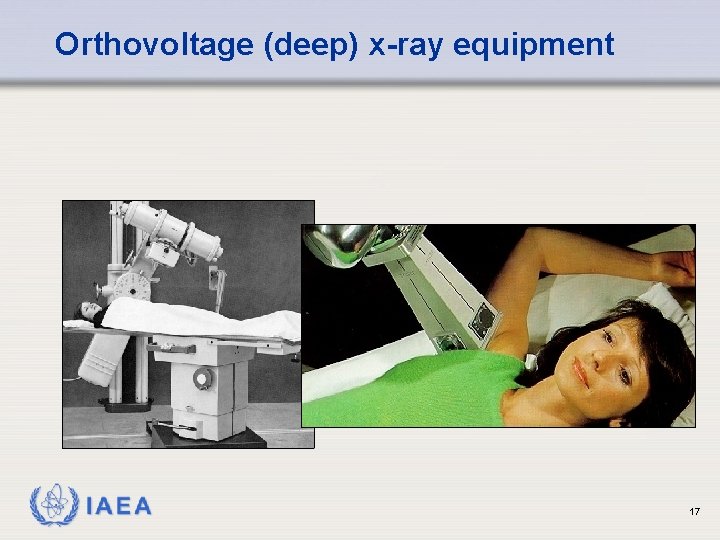
Orthovoltage (deep) x-ray equipment IAEA 17
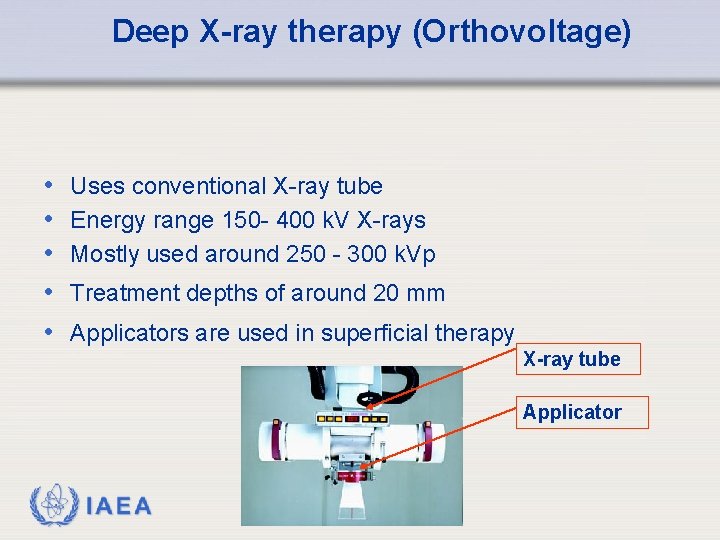
Deep X-ray therapy (Orthovoltage) • • • Uses conventional X-ray tube Energy range 150 - 400 k. V X-rays Mostly used around 250 - 300 k. Vp Treatment depths of around 20 mm Applicators are used in superficial therapy X-ray tube Applicator IAEA

Deep X-ray therapy (Orthovoltage) • Penetration sufficient for palliative treatment of bone lesions relatively close to the surface (ribs, spinal cord) • Largely replaced by megavoltage treatment modalities for treatment of other lesions IAEA

Disadvantages of deep x-ray • Higher dose to bone - photoelectric absorption • Maximum dose on the surface hence higher skin dose • Treatment to a depth of only a few centimeters possible • Low energy, hence high scattered radiation and larger penumbra IAEA

Gamma ray equipment IAEA 21
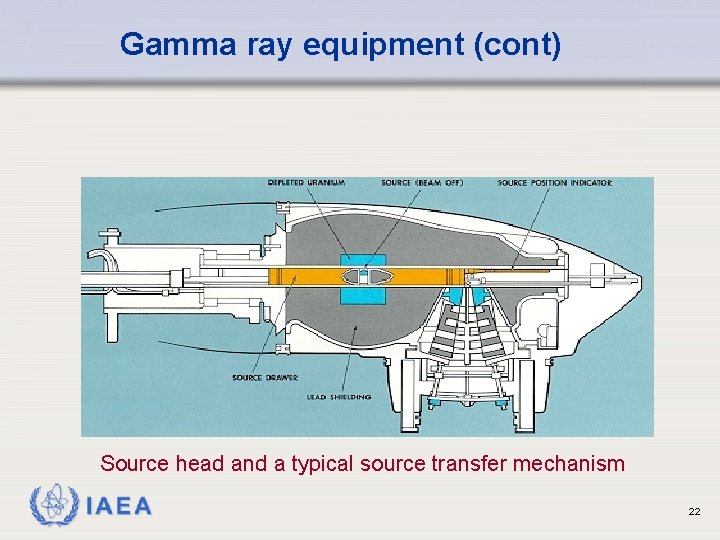
Gamma ray equipment (cont) Source head and a typical source transfer mechanism IAEA 22

Why prefer Cobalt unit over Orthovoltage? IAEA

GAMMA KNIFE • The gamma knife device contains 201 cobalt-60 sources of • • approximately 30 curies each It is placed in a circular array in a heavily shielded assembly. The device aims gamma radiation through a target point in the patient's brain. The patient wears a specialized helmet that is surgically fixed to their skull so that the brain tumor remains stationary at target point of the gamma rays. Therefore it is also known as the stereotactic surgery. IAEA
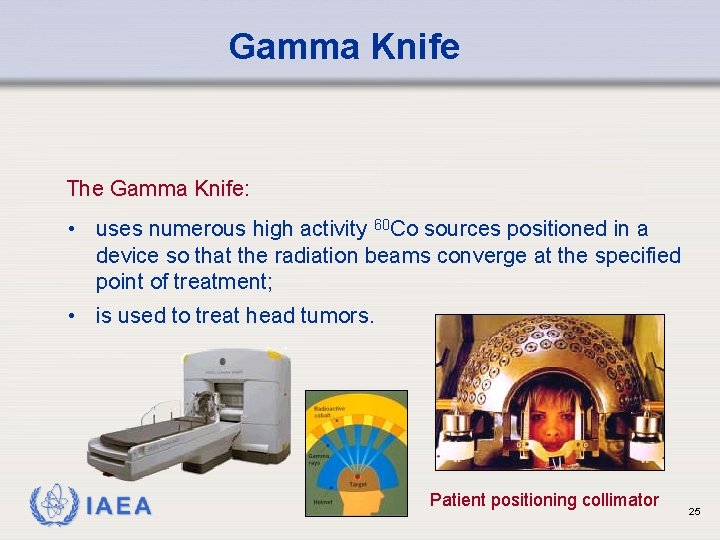
Gamma Knife The Gamma Knife: • uses numerous high activity 60 Co sources positioned in a device so that the radiation beams converge at the specified point of treatment; • is used to treat head tumors. IAEA Patient positioning collimator 25

Linear Accelerator Modern accelerators have a number of treatment options e. g. • X-rays or electrons (dual mode); • 2 X-ray energies; • 5 or more electron energies. IAEA 26
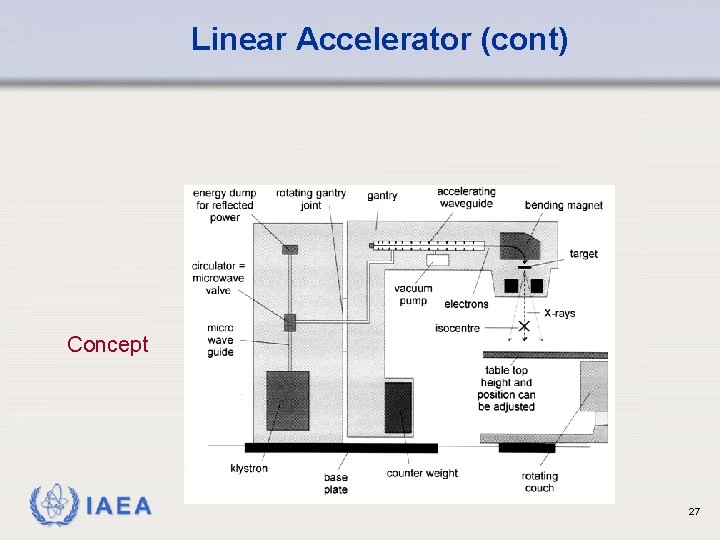
Linear Accelerator (cont) Concept IAEA 27

Linear Accelerator (cont) Radiation exposure: • is controlled by two independent integrating transmission ionization chamber systems; • one of these is designated as the primary system and should terminate the exposure at the correct number of monitor units; • these also steer the beam. IAEA 28

Linear Accelerator (cont) • the other system is termed the secondary system and is usually set to terminate the exposure after an additional 0. 4 Gy; • most modern accelerators also have a timer which will terminate the exposure if both ionization chamber systems fail. IAEA 29

Linear Accelerator (cont) Complex head structure to handle multiple energies and multiple modalities. IAEA 30

Linear Accelerator (cont) Complex control system IAEA 31

Linear Accelerator (cont) Verification systems All accelerator manufacturers produce computer controlled verification systems which provide an additional check that the settings on the accelerator console: • are correct for proper accelerator function; and • correspond exactly with the parameters determined for the individual patient during the treatment planning process IAEA 32

Linear Accelerator (cont) X-ray Collimators Rectangular (conventional) • The transmission through the collimators should be less than 2% of the primary (treatment) beam. Multi-leaf collimators (MLC) • the transmission through the collimators should be less than 2% of the primary (treatment) beam. • The transmission between the leaves should be checked to ensure that it is less than the manufacturer’s specification. IAEA 33

Linear Accelerator (cont) Electron applicators may be: • open sided for modern accelerators using double scattering foils or scanned beams; • enclosed for older accelerators usingle scattering foils. Both types should be checked for leakage: • adjacent to the open beam; • on the sides of the applicators. IAEA 34

Linear Accelerator (cont) Neutrons: - • should be considered if the x-ray energy is greater than 10 MV Issues which need to be considered when neutrons are presents include: • neutron activation • shielding problems IAEA

A comparison: Cobalt unit Vs Linac IAEA

General Safety Requirements • Clear indication shall be provided at the control console and in the treatment room to show when the equipment is in operation. • Dual interlocks shall be provided on all doors to the treatment room such that opening a door will interrupt the treatment. It should only be possible to resume treatment from the control console. IAEA 37

General Safety Requirements Warning Signals and Signs IAEA 38

General Safety Requirements “Fail safe” systems There shall be at least two independent “fail safe” systems for terminating the irradiation. These could be: • two independent integrating in-beam dosemeters; • two independent timers; • an integrating dose meter and timer. Each system shall be capable of terminating the exposure. IAEA 39

General Safety Requirements Collimation The exposure shall be limited to the area being examined or treated by the use of collimating devices aligned with the radiation beam. Exposure rates outside the examination or treatment area due to leakage or scatter shall be kept as low as reasonably achievable. IAEA 40
- Slides: 40