EASTERN CAPE DEPARTMENT OF HEALTH Parliamentary Budget Hearings

EASTERN CAPE DEPARTMENT OF HEALTH Parliamentary Budget Hearings Tuesday, 08 June 2004

INDEX 1. 2. 3. 4. 5. 6. 7. 8. 9. 10 Overview Organisational Establishment Revised Service Delivery Model Where do we want to be Achievements according to Ten Point Plan Major challenges Alignment of goals with National and Provincial imperative Priorities Finance Information Conclusion Page 3 4 5 -6 7 -9 10 – 20 21 -23 24 -29 30 -34 u 2
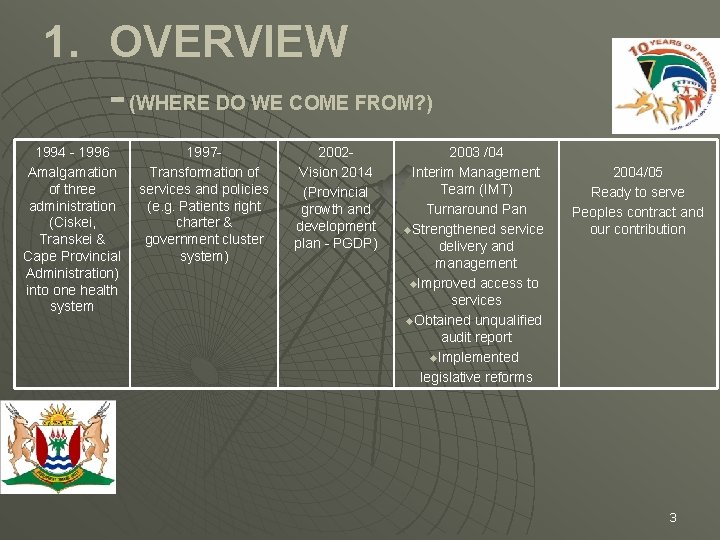
1. OVERVIEW - (WHERE DO WE COME FROM? ) 1994 - 1996 Amalgamation of three administration (Ciskei, Transkei & Cape Provincial Administration) into one health system 1997 Transformation of services and policies (e. g. Patients right charter & government cluster system) 2002 Vision 2014 (Provincial growth and development plan - PGDP) 2003 /04 Interim Management Team (IMT) Turnaround Pan u. Strengthened service delivery and management u. Improved access to services u. Obtained unqualified audit report u. Implemented legislative reforms 2004/05 Ready to serve Peoples contract and our contribution 3
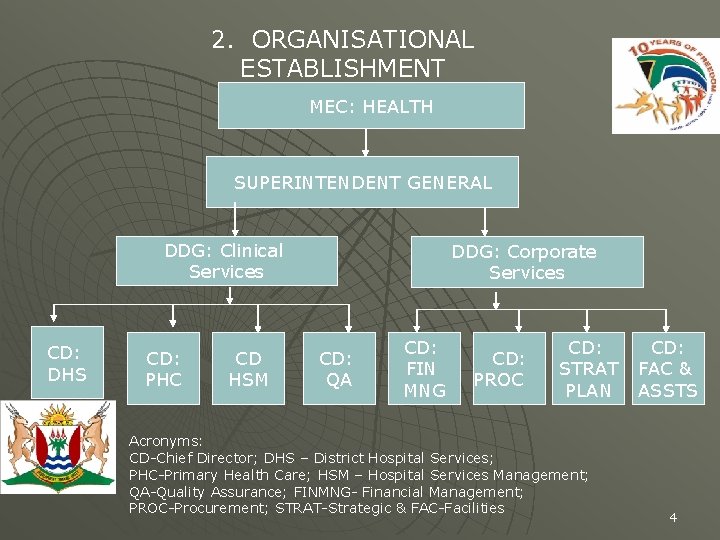
2. ORGANISATIONAL ESTABLISHMENT MEC: HEALTH SUPERINTENDENT GENERAL DDG: Clinical Services CD: DHS CD: PHC CD HSM DDG: Corporate Services CD: QA CD: FIN MNG CD: PROC CD: STRAT PLAN Acronyms: CD-Chief Director; DHS – District Hospital Services; PHC-Primary Health Care; HSM – Hospital Services Management; QA-Quality Assurance; FINMNG- Financial Management; PROC-Procurement; STRAT-Strategic & FAC-Facilities CD: FAC & ASSTS 4
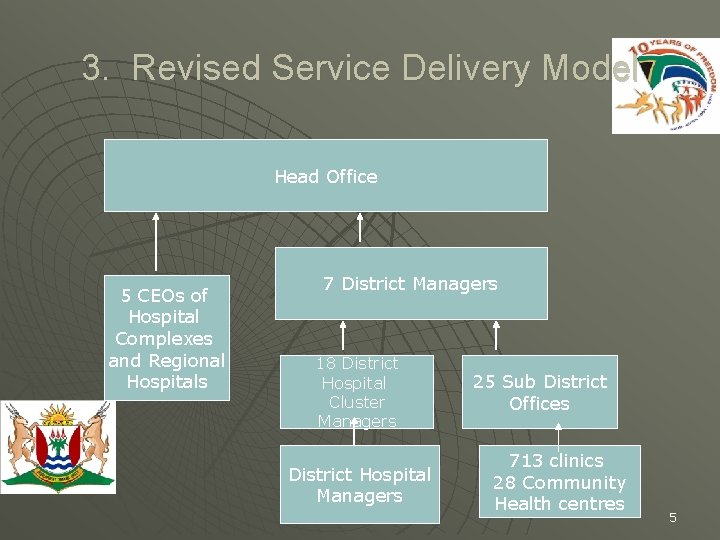
3. Revised Service Delivery Model Head Office 5 CEOs of Hospital Complexes and Regional Hospitals 7 District Managers 18 District Hospital Cluster Managers District Hospital Managers 25 Sub District Offices 713 clinics 28 Community Health centres 5

SERVICE DELIVERY MODEL The role of Head Office will be focused on programs coordination, integration and policy formulation, monitoring and evaluation. u. Our PHC services are provided through 713 clinics and 28 Community Health Centres, and these are managed by 27 Local Service Area (LSA) managers. Patients that need high level of care will be referred to Level 1 hospitals u 18 Clusters of 47 district hospitals as well as 18 provincial aided and 4 privately run hospitals provide level 1 services. Clustering will allow for sharing of resources including professional staff. u The three complexes and two regional hospitals provide levels 2 and 3 services. u. The 7 district managers have responsibility over 18 CEOs in the clusters and 25 LSA managers. They report to head office. u. The 2 regional and 3 complex CEOs report directly to head office. u

4. WHERE DO WE WANT TO BE? 4. 1 VISION u A health service to the people in the Eastern Cape Province promoting a better quality of life for all. 7

4. 2 MISSION To provide and ensure accessible comprehensive integrated services in the Eastern Cape emphasizing the primary health care approach utilizing and developing all resources to enable all its present and future generation to enjoy health and quality of life. 8

4. 3 VALUES Human Rights, customer satisfaction, service excellence and value for money are ensured through adherence to the following values: u u u Equity of both distribution and quality of services Service excellence including customer satisfaction Fair labour practices Good work ethic and a high degree of accountability Transparency demonstrated through consultations with all stakeholders in the health industry/field 9

5. ACHIEVEMENTS ACCORDING TO THE TEN POINT PLAN (WHERE ARE WE NOW? ) 10

5. 1. REORGANISATION OF CERTAIN SUPPORT SERVICES CORPORATE SERVICES CENTRES u The department and the Interim Management Team (IMT) established 11 Corporate Service Centres • 3 Complexes • 7 Districts • Head Office u to provide shared support services • • • HR, Finance, Procurement, Administration & IT 11

5. 2. LEGISLATIVE REFORM u u u Education and Training of Nurses and Midwives Act no. 4 of 2003 Medicines Act 90 of 1997 and Pharmacy Act 88 of 1997 they will be applicable in July 2005 to the State Mental Health Act of 2002 12

5. 3. IMPROVING QUALITY OF CARE u u u Health service awards launched in East London and Umtata aimed at maintaining high standards in institutions A 24 hr call centre has been established with a toll free number of 0800032364 providing opportunity for grievances and suggestions In line with the prevention of blindness (Global vision 2020) we are improving our cataract performance yearly. 13

5. 4. REVITALIZATION OF HOSPITAL SERVICES u u u PE Complex is our flagship in Rationalisation of Services Provincial secondary and tertiary service delivery plans have been developed and these are linked to national modernisation of tertiary services Outreach program focussing on mother and child health as well as anaesthetic training Rationalisation of psychiatric services establishing psychiatric beds in the eastern side of the province Nelson Mandela Academic Hospital functional and awaiting official opening 21 hospital construction projects completed, 14 under construction, equipment procured for 50 hospitals and maintenance done to 88 hospitals 14

5. 5. SPEEDING OF DELIVERY OF AN ESSENTIAL PACKAGE OF SERVICE THROUGH THE DISTRICT HEALTH SYSTEM u u Institutionalisation of the 18 hospital clusters including appointment of management teams for these clusters Clustering will allow sharing of resources 15

5. 6. DECREASING MORBIDITY AND MORTALITY RATES THROUGH STRATEGIC INTERVENTIONS u u u Following implementation of standards in Traditional Circumcision Act (Act no. 6 of 2001) there has been marked decrease in morbidity and mortality resulting from circumcision (statistics) Placement of staff to oversee the ARV treatment plan has been completed; 270 nurses, doctors, pharmacists, dieticians and workers have been trained in the various aspects of disease management 16

5. 7. IMPROVING RESOURCE MOBILIZATION AND UTILISATION For the first time Eastern Cape had an unqualified report u PPP – Kouga Partnership Hospital at Humansdorp being the first colocation PPP in the Province u 17

5. 8. IMPROVING COMMUNICATION AND CONSULTATION WITHIN THE HEALTH SYSTEM AND WITH COMMUNITIES WE SERVE u u Communication unit established at head office and director appointed Hospital boards clinic committees established Three mental health review boards established Weekly slot in local radio station talking about health issues 18

5. 9. IMPROVING HUMAN RESOURCE DEVELOPMENT AND MANAGEMENT u u u u Increased number of community service professionals Induction of community service professionals aimed at presenting our recruitment and retention strategy Learnerships & internships introduced Delegations – human resources and finance have been finalised Implementation of scarce skills and rural allowances Implementation of skills development plan Gradual implementation of the Employment Equity 19

5. 10. STRENGTHENING CO-OPERATION WITH OUR PARTNERS INTERNATIONALLY u u Fred Hollows Foundation training programme to assist in improving prevention of blindness Luxemburg-Aid in infrastructure development (Mnquma – former Transkei Communicable Disease Centre, British Columbia, PEPFAR supporting the implementation of the Comprehensive Treatment Plan Training of rehabilitation technicians in Tanzania 20

6. MAJOR CHALLENGES IN THE DEPARTMENT 21

6. 1 HEALTH CHALLENGES u u u u Management and reduction of communicable disease, Cholera HIV/AIDS, TB and STIs including the Comprehensive Treatment Plan which includes ARV roll-out. Staff recruitment, retention and composition Management of childhood disease including low immunization coverage Cross boundaries movement of people Legislative reforms influenced by cultural factors e. g. circumcision, and recognition of alternative medicine including traditional healing Drug supply Backlog in health infrastructure development 22

6. 2 OTHER CHALLENGES u u Escalating crime calling for more security for staff working in primary health care facilities, establishment of Crisis Centres and counseling facilities for victims of abuse as well as calling for more collaborative endeavors with other sectors The impact of increased motor vehicle accidents on emergency medical services and other services 23

7. ALIGNMENT OF GOALS WITH NATIONAL AND PROVINCIAL IMPERATIVES 24

Alignment of Goals People’s Contract NDo. H PGDP EC Do. H Access to services Strengthen primary health care (both public and private sectors) Improving access to health by prioritising health resources G 1: Ensuring equitable access by all communities to essential package of services through DHS and referral systems O 1. 1: Effective rendering of PHC & EHS in the province 01. 2 : Implementation of programmes to reduce morbidity and mortality 01. 3: Improve equity of access to all services and infrastructure development Sustainable livelihoods 25

Alignment of Goals Continued People’s Contract NDo. H PGDP ECDo. H Access to services Strengthen primary health care (both public and private sectors Equitable health standards between rural and urban areas G 2: Health services to meet quality standards O 2. 1: Set norms and standards for quality assurance 02. 2: Implement monitoring and evaluation systems 02. 3: Revitalize our facilities 02. 4: Strengthen drug distribution and information systems 02. 5: Accreditation of facilities Sustainable livelihoods 26

Alignment of Goals Continued People’s Contract NDo. H Constitutional rights & governance Participation of communities with effective communication. Strengthen social mobilisation PGDP ECDo. H Funding leverage through increased use of PPP’s for hospital management. Participation by the public in the process of socio economic change G 3: Communities become active, responsible partners in health issues which affect them O 3. 1: Strengthen governance structure at all levels for effective participation of civil society 03. 2: Improving external and internal communication to harness service delivery 27

Alignment of Goals Continued People’s Contract NDo. H Access to services Growing economy Human resource development and management – need more coherent strategy PGDP ECDo. H Human resource development -Learnerships and internship programmes -Community Health Worker programme -Decentralisation of powers and functions to district health services G 4: Build capacity in the Dept. to support improved implementation of its goals O 4. 1: Implement programmes for recruitment and retention of essential HR skills 04. 2: Provide ongoing training and skills development for health workers 04. 3: Align skills to service delivery, by standardising nursing education, using PPPs, Section 21, employing medical assistants etc. Implement and maintain results driven PMDS programme 28

Alignment of Goals End People’s Contract NDo. H PGDP ECDo. H A growing economy Sustainable livelihoods Access to services Crime & Corruption Enabling factor – relates to all health priorities e. g. Affordable medicines, including traditional medicines Decentralisation of powers and functions to district health office G 5: Effective and efficient utilisation of the Depts. Finance and assets to achieve effective service delivery O 5. 1: Equitable resource allocation across the province 05. 2: Rationalise and integrate health services 05. 3: Ensure effective cash flow forecasting, efficient financial and asset management as well as financial controls Health infrastructure planning 29

8. PRIORITIES FOR DEPARTMENT OF HEALTH IN NEXT 3 YEARS 30

8. 1 CLINICAL SERVICES (PHC) u u u Roll out Comprehensive Plan to target 147 200 cumulative clients by 2008 including 2700 in 2004/05. Accreditation of Ukhahlamba and Alfred Nzo phase 1 sites will be finalized by end July 2004 Collaborative project with DWAF and Municipalities on water and sanitation Expanded Programme of Immunisation campaign in July 2004 R 1 million set aside for food gardens to benefit 4000 clients Commenced a programme on training professionals on maternity and child health services Finalise transfer of 174 Environmental Health Professionals to municipalities 31

8. 2 CLINICAL SERVICES (HOSPITAL) u u 80 New EMS vehicles were purchased between November 2003 and March 2004 for deployment. An Air Ambulance service has been implemented Finalise recruitment of management in the District Hospital Clusters and implementation of clinical programmes Aligning our service delivery plans with MTS NMAH commissioned and awaiting official opening in 2004/05 32

8. 3 CLINICAL SERVICES (QUALITY OF CARE) u u u Implementation of fully-fledged call centre to be able to monitor and provide feedback in all our customer complaints Will establish clinical audit on target clinical programmes to ensure on-going monitoring and quality Will implement accreditation programme targeting 40 hospitals over the next 3 years (and targeting 5 accredited hospitals) 33

8. 4 SUPPORT SERVICES u Infrastructure -Roll-out revitalisation programme with 4 Hospitals at different phases of development (St Elizabeth, Frontier, Mary Terese and Rietvlei) -Building of 46 clinics (including 13 in 2004/05) over the next 3 years -Replacing 47 clinic over next 3 years u u Roll-out Corporate Service Centres to all districts (functional by March 2005) Implementation of good finance governance and management principles • • Audit committee Internal Audit Risk assessment and management Decentralized pre-audit function 34

Support Services continued u Enhance HRM in the department • • • u Robust recruitment and retention strategy Roll-out PMDS to all levels Learnership and internship programmes and targeting 1000 school leavers training as Nursing assistants and /or Community Health Workers Mobilization of resources • Finalization of Drug PPP • Implementation Humansdorp PPP • Development of Port Alfred and Settlers PPP’s 35
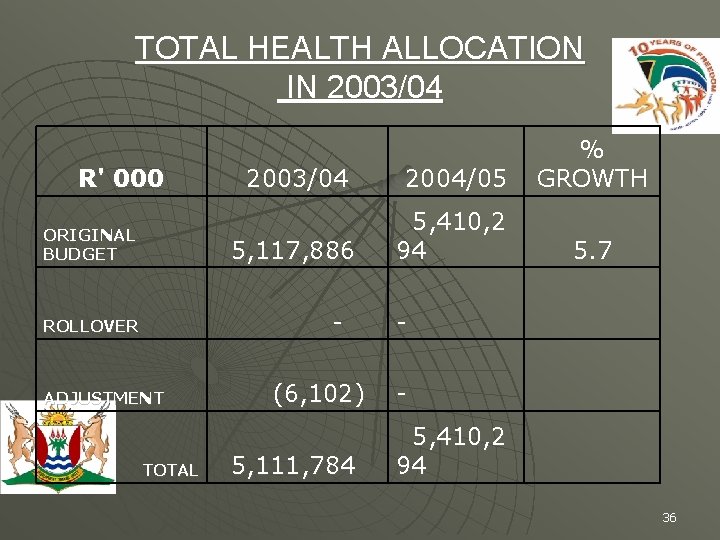
TOTAL HEALTH ALLOCATION IN 2003/04 R' 000 ORIGINAL BUDGET 2003/04 2004/05 % GROWTH 5, 117, 886 5, 410, 2 94 5. 7 - ROLLOVER ADJUSTMENT TOTAL (6, 102) 5, 111, 784 5, 410, 2 94 36

6. BUDGET Trends in Provincial Public Health expenditure by Budget Programme in current prices (R thousand) Programme Health Administration 7 District Health Services 1 Emergency Medical Services 4 Provincial Hospital Services 8 Health Sciences and Training 6 Health Care Support Services 65 Health Facilities Management 2 Total 2001/02 2002/03 2003/04 2004/05 2005/06 2006/07 (Actual) (Estimate) Budget MTEF 53 168, 94 2, 124, 75 87, 31 1, 237, 95 76, 75 6, 7 189, 96 3, 892, 4 7 1 4 0 4 68 8 42 191, 70 2, 250, 81 122, 46 1, 519, 75 96, 12 9, 1 303, 21 4, 493, 2 10 46 88 85 84 27 06 46 215, 1 2, 518, 3 194, 4 1, 699, 4 122, 8 23, 0 468, 8 5, 242, 1 86 02 65 44 26 07 64 94 260, 5 2, 684, 1 65, 3 1, 703, 2 163, 5 21, 6 511, 8 5, 410, 2 76 94 23 40 10 73 75 91 302, 1 3, 058, 5 86, 9 1, 940, 6 171, 3 26, 8 624, 3 6, 210, 8 37 57 06 50 86 07 29 72 315, 6 3, 318, 5 90, 3 2, 016, 8 177, 8 27, 9 675, 3 6, 622, 4 37
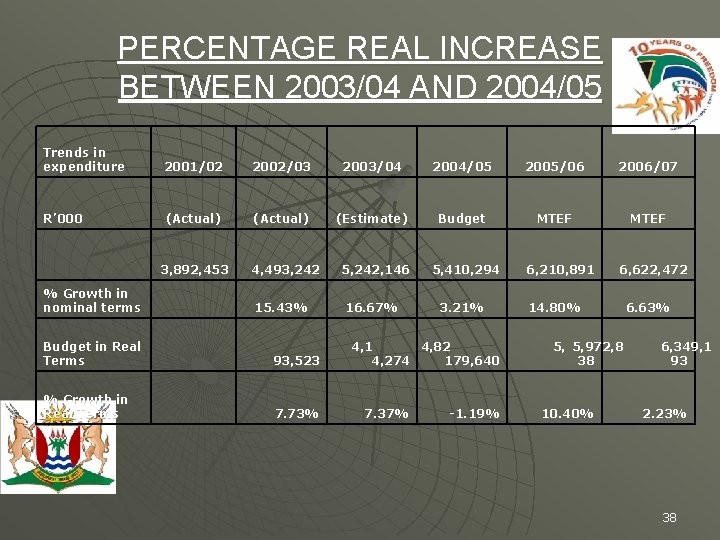
PERCENTAGE REAL INCREASE BETWEEN 2003/04 AND 2004/05 Trends in expenditure 2001/02 2002/03 2003/04 2004/05 2005/06 2006/07 R’ 000 (Actual) (Estimate) Budget MTEF 3, 892, 453 % Growth in nominal terms 4, 493, 242 15. 43% Budget in Real Terms 93, 523 % Growth in Real Terms 7. 73% 5, 242, 146 16. 67% 5, 410, 294 3. 21% 4, 1 4, 82 4, 274 179, 640 7. 37% -1. 19% 6, 210, 891 6, 622, 472 14. 80% 5, 5, 972, 8 38 10. 40% 6. 63% 6, 349, 1 93 2. 23% 38
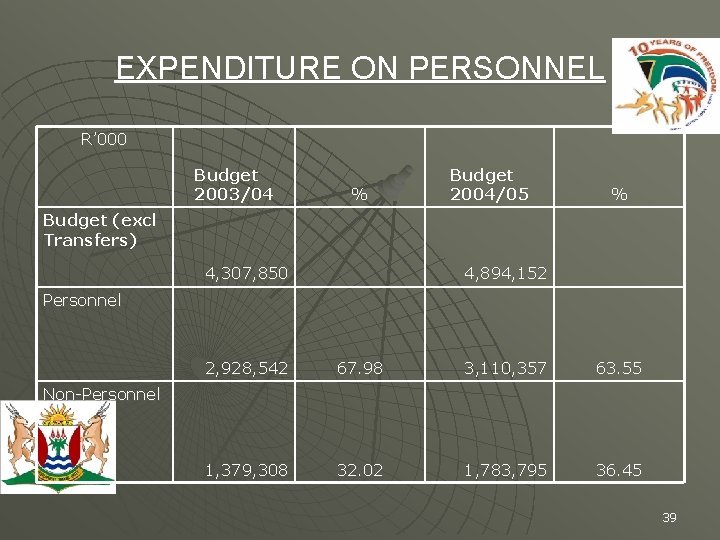
EXPENDITURE ON PERSONNEL R’ 000 Budget 2003/04 % Budget 2004/05 % Budget (excl Transfers) 4, 307, 850 4, 894, 152 Personnel 2, 928, 542 67. 98 3, 110, 357 63. 55 1, 379, 308 32. 02 1, 783, 795 36. 45 Non-Personnel 39
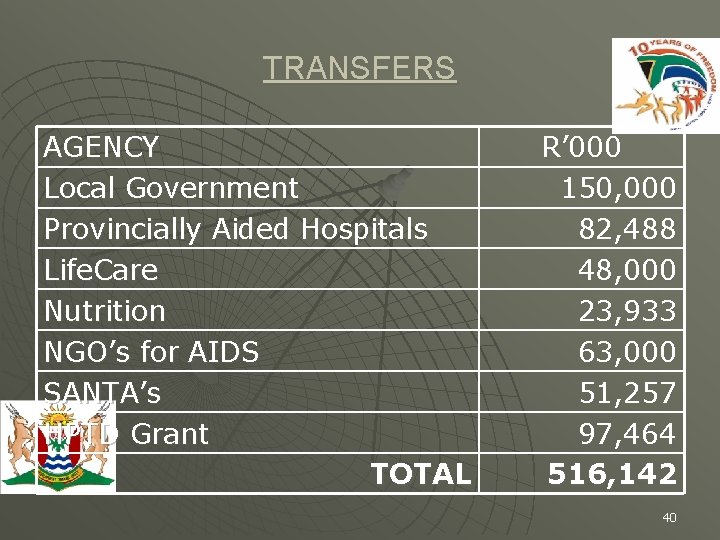
TRANSFERS AGENCY Local Government Provincially Aided Hospitals Life. Care Nutrition NGO’s for AIDS SANTA’s HPTD Grant TOTAL R’ 000 150, 000 82, 488 48, 000 23, 933 63, 000 51, 257 97, 464 516, 142 40
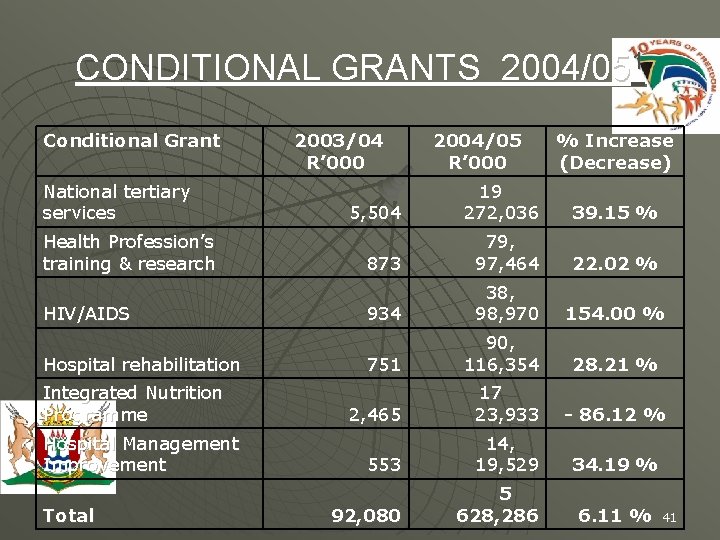
CONDITIONAL GRANTS 2004/051 Conditional Grant National tertiary services Health Profession’s training & research HIV/AIDS Hospital rehabilitation Integrated Nutrition Programme Hospital Management Improvement Total 2003/04 R’ 000 2004/05 R’ 000 % Increase (Decrease) 5, 504 19 272, 036 39. 15 % 873 79, 97, 464 22. 02 % 934 38, 970 154. 00 % 751 90, 116, 354 2, 465 17 23, 933 - 86. 12 % 553 14, 19, 529 34. 19 % 92, 080 5 628, 286 28. 21 % 6. 11 % 41
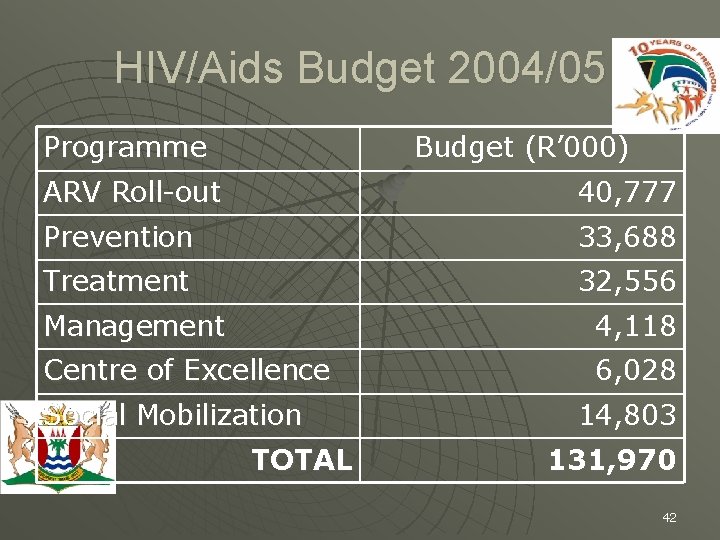
HIV/Aids Budget 2004/05 Programme Budget (R’ 000) ARV Roll-out 40, 777 Prevention 33, 688 Treatment 32, 556 Management 4, 118 Centre of Excellence 6, 028 Social Mobilization TOTAL 14, 803 131, 970 42

2003/04 Expenditure analysis Adjusted Appropriatio n Actual Expenditure R'000 2, 846, 958 2, 815, 673 31, 285 99 Administrative 225, 488 219, 150 6, 338 97 Inventories 569, 141 558, 506 10, 635 98 Equipment 108, 467 97, 782 10, 685 90 716) (49, 112 278) (48, 116 754) (91, 114 Standard item classification Personnel Land buildings Professional and special services 417, 084 298, 501 Transfer payments Total 643, 841 782 Expenditu re as % of revised R'000 allocation Savings (Excess) 466, 800 346, 779 735, 595 5, 111, 2, 146 5, 24 364) (130, 103 43
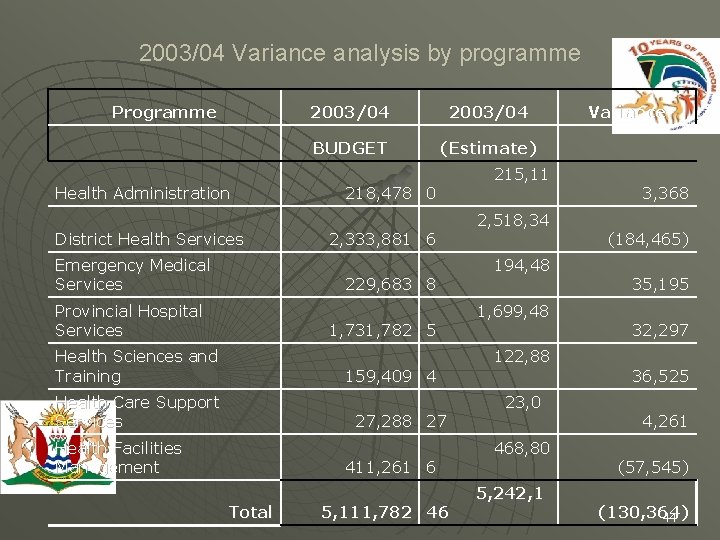
2003/04 Variance analysis by programme Programme Health Administration District Health Services Emergency Medical Services 2003/04 BUDGET (Estimate) 218, 478 0 2, 333, 881 6 229, 683 8 Provincial Hospital Services 1, 731, 782 5 Health Sciences and Training 159, 409 4 Health Care Support Services 27, 288 27 Health Facilities Management 411, 261 6 Total 5, 111, 782 46 215, 11 2, 518, 34 194, 48 1, 699, 48 122, 88 23, 0 468, 80 5, 242, 1 Variance 3, 368 (184, 465) 35, 195 32, 297 36, 525 4, 261 (57, 545) (130, 364) 44
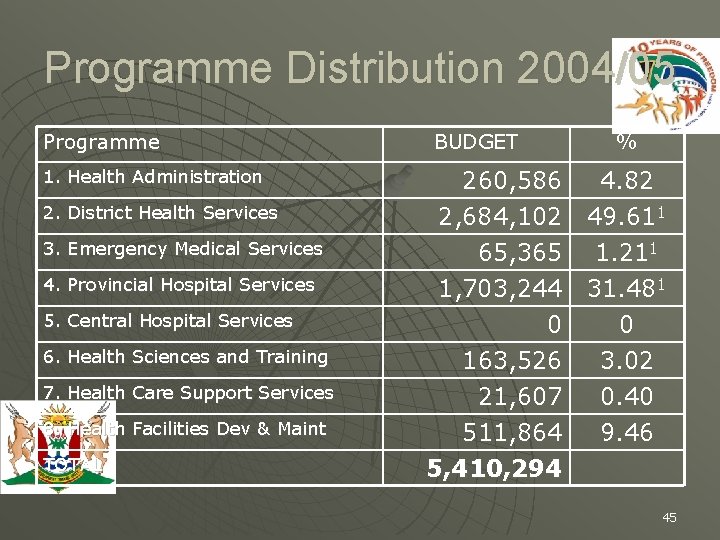
Programme Distribution 2004/05 Programme 1. Health Administration 2. District Health Services 3. Emergency Medical Services 4. Provincial Hospital Services 5. Central Hospital Services 6. Health Sciences and Training 7. Health Care Support Services 8. Health Facilities Dev & Maint TOTAL BUDGET % 260, 586 4. 82 2, 684, 102 49. 611 65, 365 1. 211 1, 703, 244 31. 481 0 0 163, 526 3. 02 21, 607 0. 40 511, 864 9. 46 5, 410, 294 45
EXPENDITURE AMOUNT PER CAPITA Expenditure per capita for the Eastern Cape Department of Health 2003/04 Population 6, 436, 7631 Per capita (total Budget) R 814. 41 Per Capita (Excluding Conditional Grants R 725. 51 In terms of the Inter Governmental Fiscal Review (IGFR) 2003 this province at R 769. 00 received the third lowest per capita allocation in South Africa. (1) Census data 2001 46

Programme Analysis u The proportion of the budget transferred to Local Government • 2. 8 % was transferred. u The total amount for donor funding was • Approx. R 26 million in kind where the USAID sponsored the Equity Project who rendered technical support and training. 47

Programme Analysis (cont) R’ 000 u Proportion of the Budget spent on District Health Services: • R 2, 684, 102 or 49. 6 % u Proportion of the Budget spent on Community Health Services and Primary Health Services • R 1, 200, 057 or 22. 18 % which is 45% of District Health Services budget 48

Cost Pressures Transport management R 37 m short u Laboratory services R 44 m short u Land buildings especially maintenance R 43 m short u Nutrition budget of R 23 m not enough to cover patients with HIV and TB u 49

7. CONCLUSION u u u Various restructuring programs have been put in place, and now we are in a process to deepen implementation. We have started the roll-out of the Plan and we will increase the pace and capacity to absorb the demand We are continuously seized with the challenge to increase the access and thereby drastically reducing the morbidity and mortality, and any other curable diseases Even though significant improvements have been made on PPTV it remains a challenge Demand for services continues to outweigh our resources We remain committed to strengthen our links with partners in civil society 50

u WE ARE READY TO DELIVER u ENKOSI!!! 51
- Slides: 51