Cummings Ch 2324 Maxillofacial Trauma Reconstruction of Facial











- Slides: 30

Cummings Ch 23/24 Maxillofacial Trauma Reconstruction of Facial Defects Julianna Pesce October 29, 2014

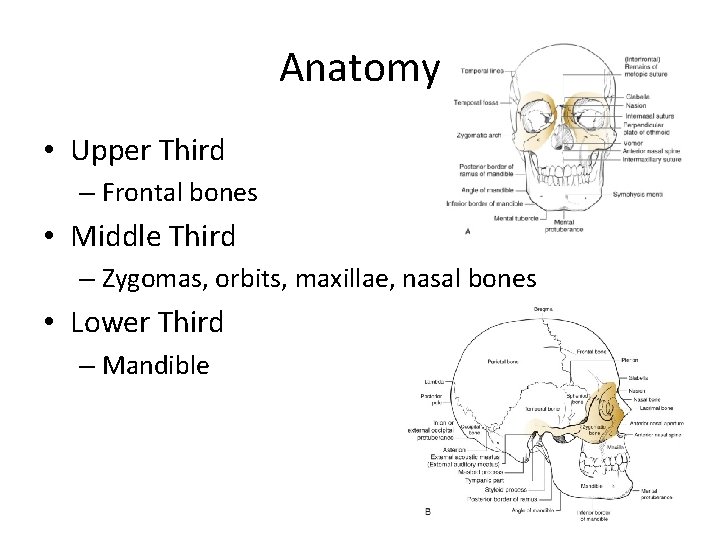
Anatomy • Upper Third – Frontal bones • Middle Third – Zygomas, orbits, maxillae, nasal bones • Lower Third – Mandible

Evaluation and Diagnosis • ABCs – Airway – High rate of c-spine fractures if facial trauma • PE – scalp, forehead – Orbits/vision, zygomas, nasal bones, septum, maxillae – Teeth, mandible, occlusion – Sensation, facial nerve function • CT is workhorse

Frontal Sinus • Anterior/posterior table, comminution, thickness • Sakas and colleagues: the more central and the more severe the fracture, more likely csf leakage

Frontal Sinus Repair • Is exploration necessary? Is obliteration necessary? • Anterior wall for cosmesis • Posterior wall to protect anterior cranial fossa • If nasofrontal ducts involved may lead to infection • Obliteration via cranialization if posterior wall severely comminuted

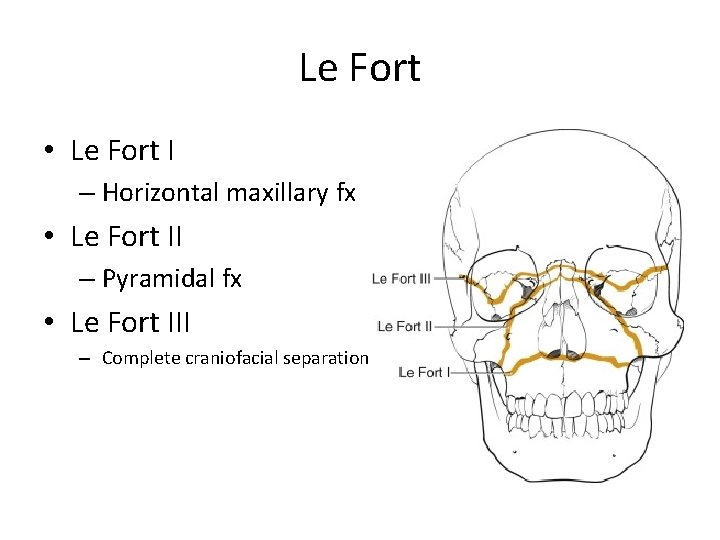
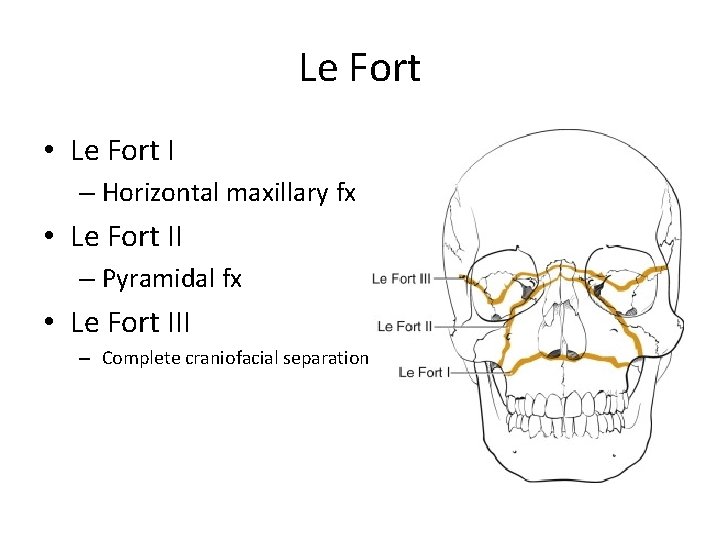
Le Fort • Le Fort I – Horizontal maxillary fx • Le Fort II – Pyramidal fx • Le Fort III – Complete craniofacial separation

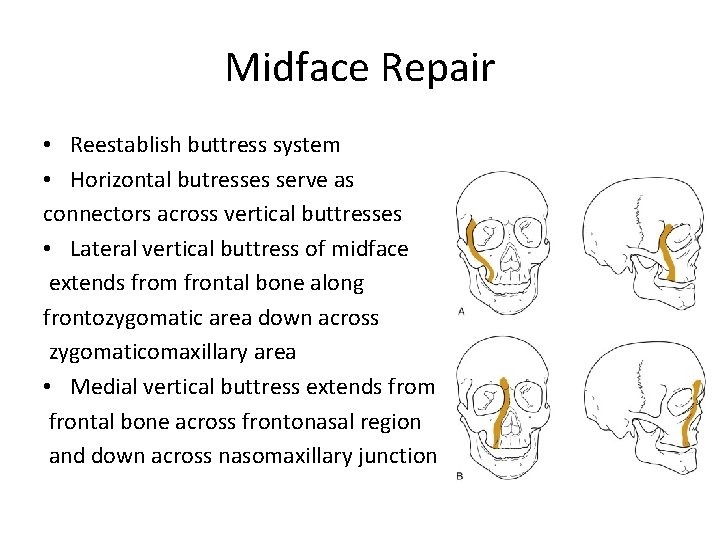
Midface Repair • Reestablish buttress system • Horizontal butresses serve as connectors across vertical buttresses • Lateral vertical buttress of midface extends from frontal bone along frontozygomatic area down across zygomaticomaxillary area • Medial vertical buttress extends from frontal bone across frontonasal region and down across nasomaxillary junction

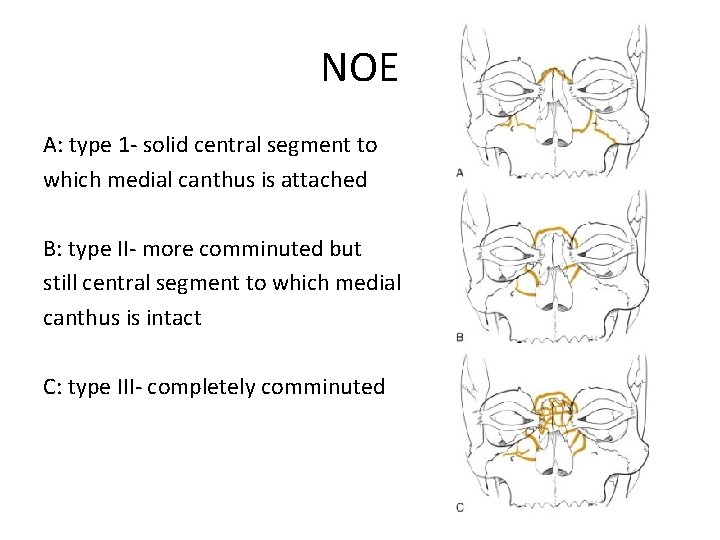
NOE A: type 1 - solid central segment to which medial canthus is attached B: type II- more comminuted but still central segment to which medial canthus is intact C: type III- completely comminuted

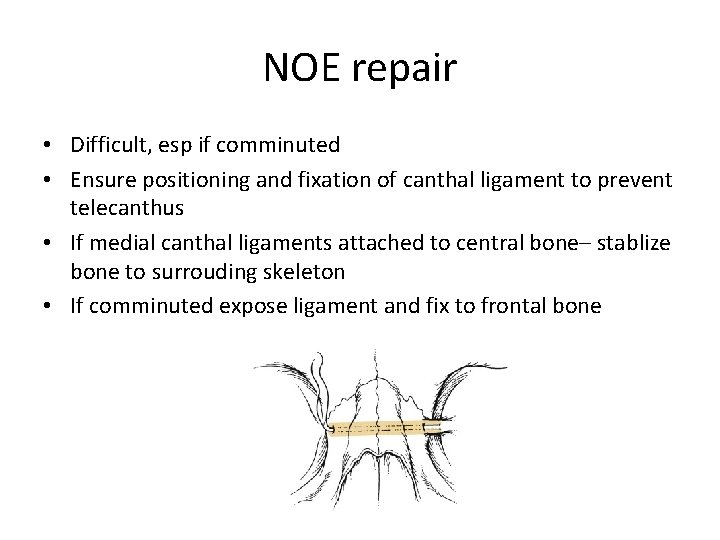
NOE repair • Difficult, esp if comminuted • Ensure positioning and fixation of canthal ligament to prevent telecanthus • If medial canthal ligaments attached to central bone– stablize bone to surrouding skeleton • If comminuted expose ligament and fix to frontal bone

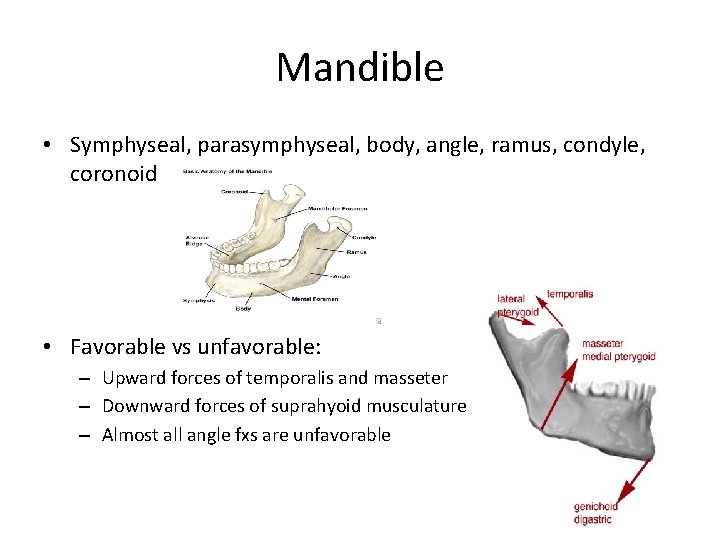
Mandible • Symphyseal, parasymphyseal, body, angle, ramus, condyle, coronoid • Favorable vs unfavorable: – Upward forces of temporalis and masseter – Downward forces of suprahyoid musculature – Almost all angle fxs are unfavorable

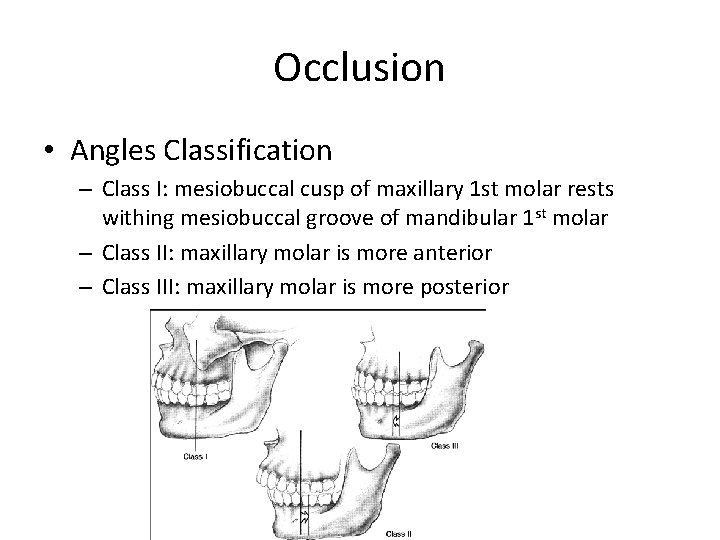
Occlusion • Angles Classification – Class I: mesiobuccal cusp of maxillary 1 st molar rests withing mesiobuccal groove of mandibular 1 st molar – Class II: maxillary molar is more anterior – Class III: maxillary molar is more posterior

Mandible Repair • Occlusion! • Plating if displaced, comminuted, unfavorable • Subcondylar fxs are controversial – MMF – Open reduction if condylar displacement into middle fossa, inability to obtain reduction, lateral extacapsular displacement of condyle, invasion by foreign body • Teeth in fracture line: pull if infected

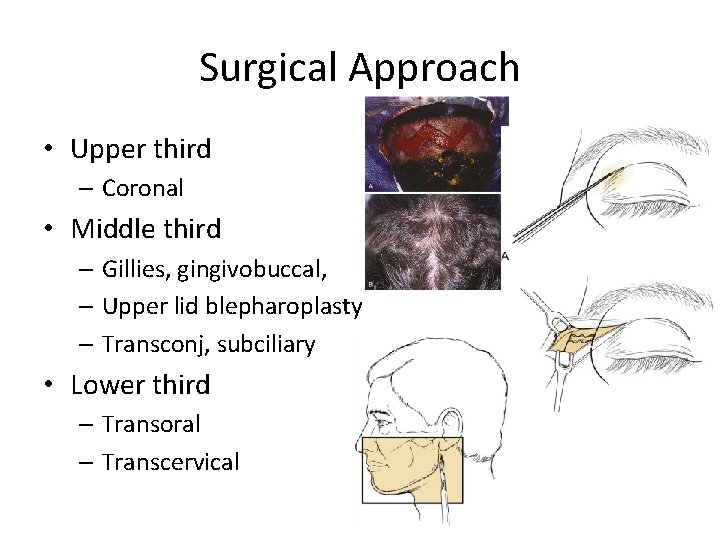
Surgical Approach • Upper third – Coronal • Middle third – Gillies, gingivobuccal, – Upper lid blepharoplasty – Transconj, subciliary • Lower third – Transoral – Transcervical

COCLIA • Review the Le. Fort Fracture levels • When would you obliterate a frontal sinus fracture and what would you use? • What are indications for opening a condyle fracture? • Discuss subciliary vs transconjunctival approach to orbital fractures. �

Le Fort • Le Fort I – Horizontal maxillary fx • Le Fort II – Pyramidal fx • Le Fort III – Complete craniofacial separation

• Frontal sinus fractures and obliteration are controversial • Posterior table displaced more than one table width • Very comminuted fractures • Persistant csf leak • Obliteration with fat, bone, pericranial fat

Condyle • Absolute indications for ORIF – Displacement into middle cranial fossa – Inability to obtain occlusion – Lateral extracapsular dislocation – Foreign body or contaminated open wound • Relative ORIF – Bilateral condylar fracture in edentulous mandible – Bilateral condylar fracture with midface fracture

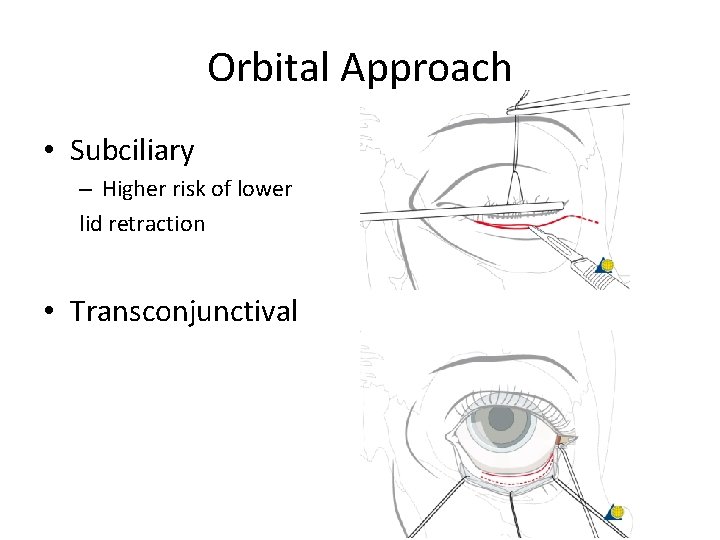
Orbital Approach • Subciliary – Higher risk of lower lid retraction • Transconjunctival

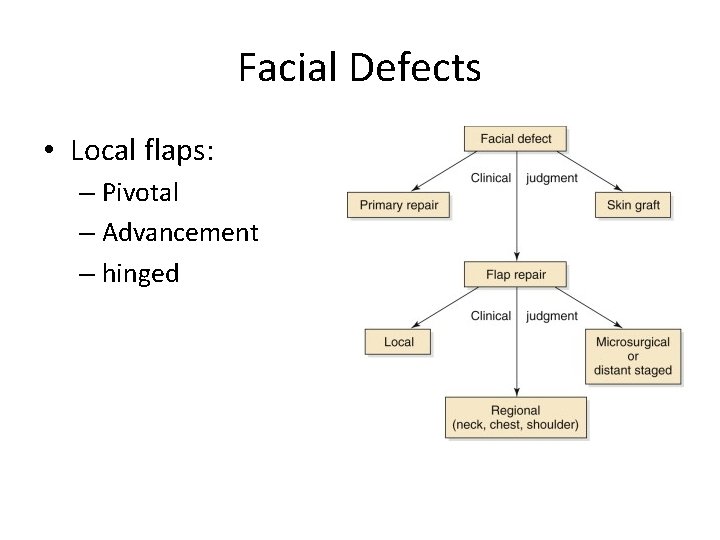
Facial Defects • Local flaps: – Pivotal – Advancement – hinged

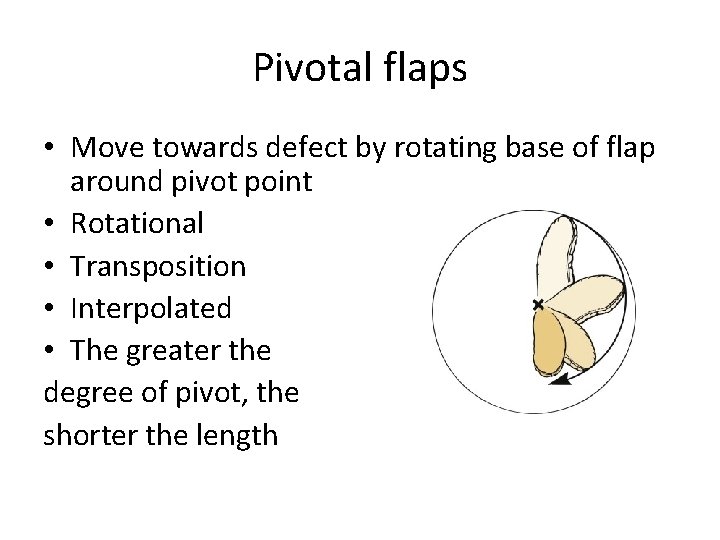
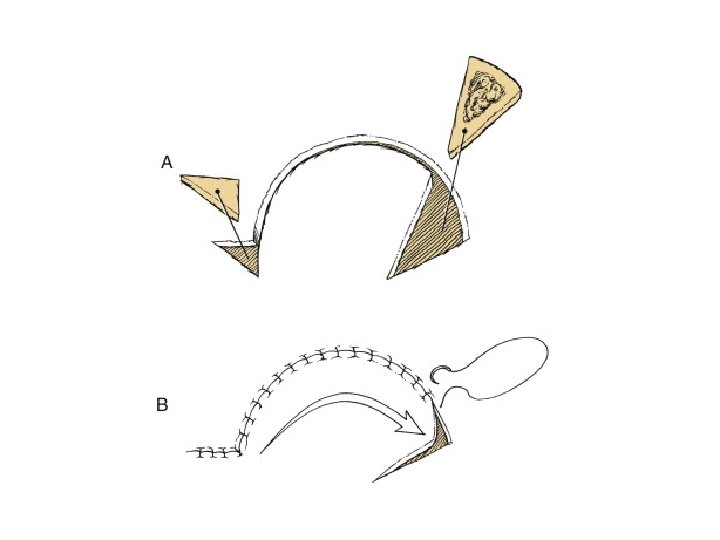
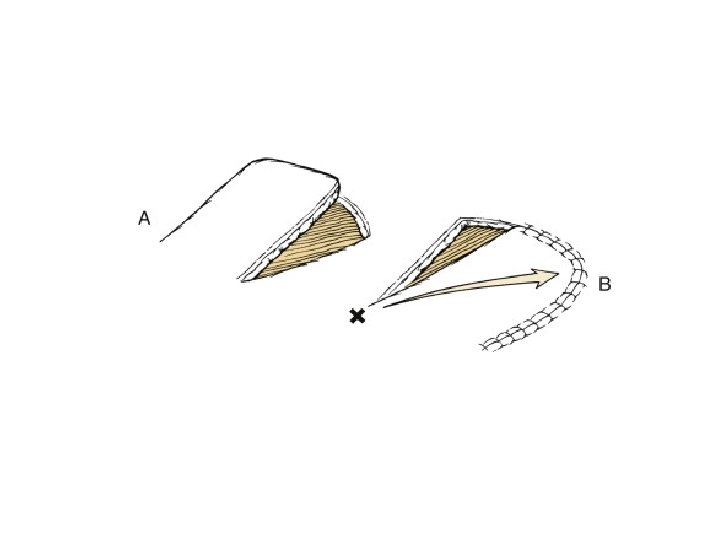
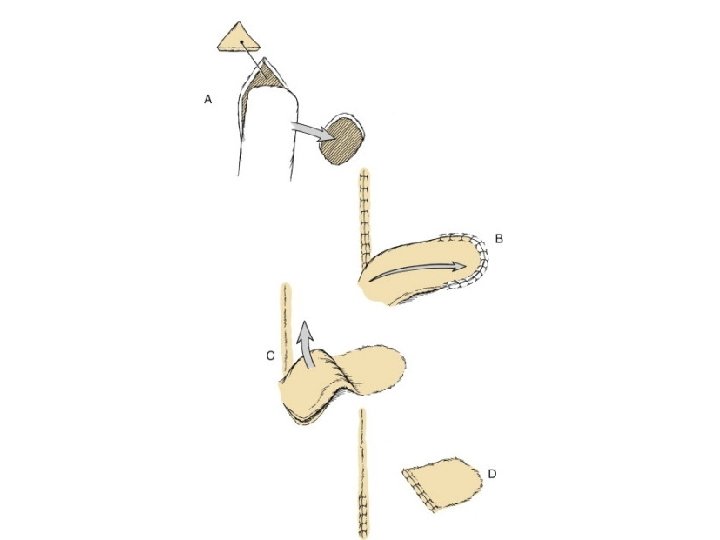
Pivotal flaps • Move towards defect by rotating base of flap around pivot point • Rotational • Transposition • Interpolated • The greater the degree of pivot, the shorter the length




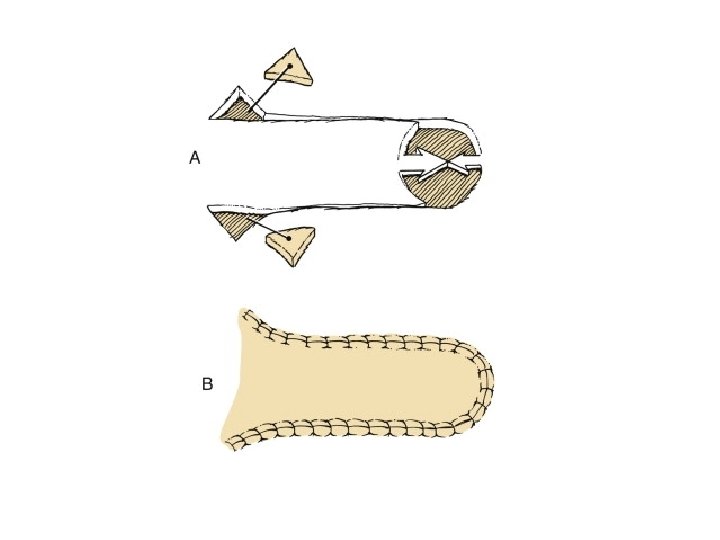
Advancement flaps • Move towards defect by stretching or recoiling the tissue of the flap • Unipedicle • Bipedicle • V-Y and V-V



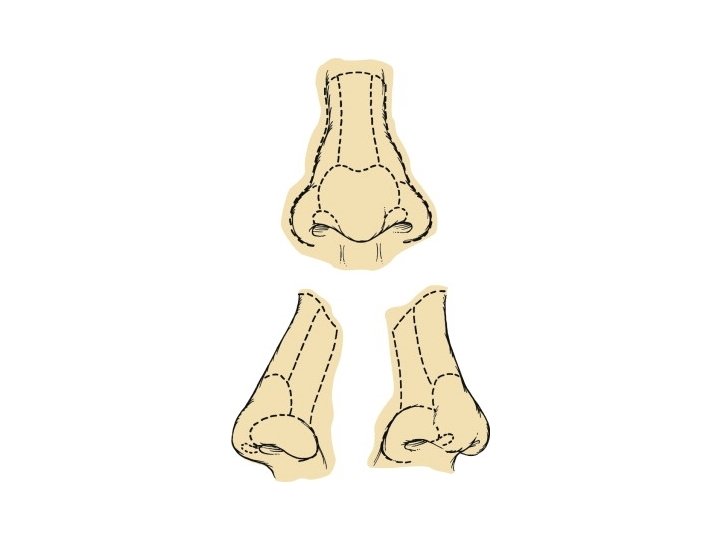
Nasal repair • Small defects with adjacent nasal skin • Full thickness skin graft for shallow defects • Interpolated paramedian forehead flap or melolabial flap for deeper defect • Full thickness requires replacement of internal lining, structural support with cartilage or bone, external coverage with interpolated cheek or forehead flap


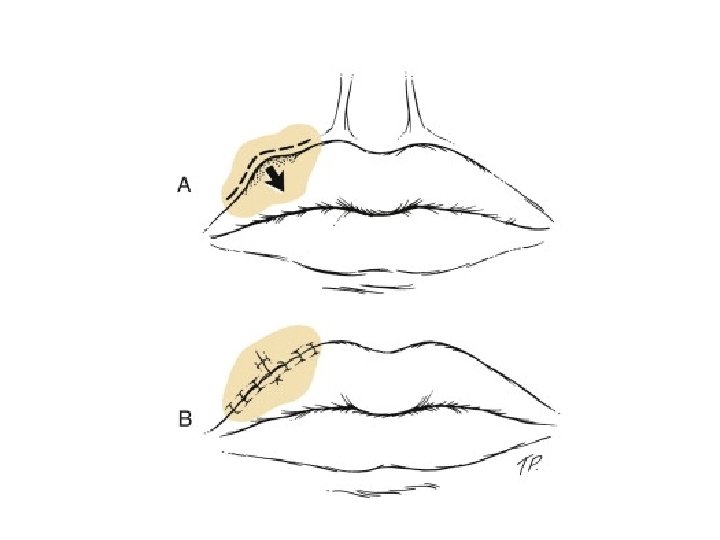
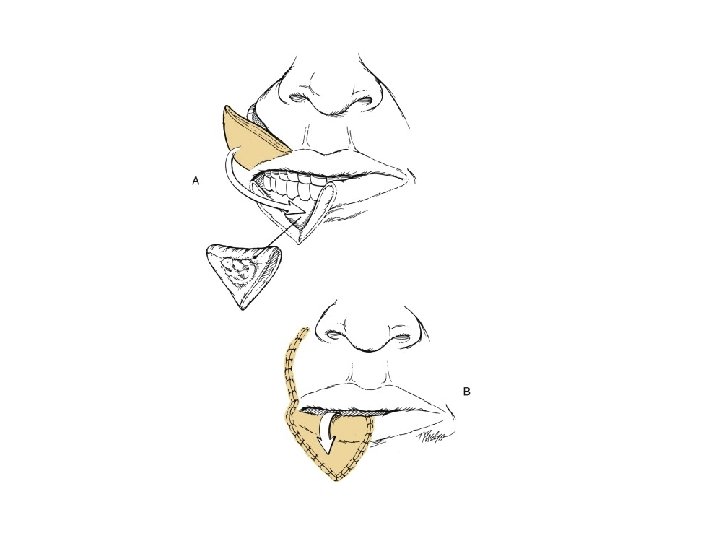
Lip reconstruction • Less than one half with primary wound closure or local flap • ½ to 2/3 require full thickness flap from opposite lip or cheek • Full thickness >2/3 need regional flap or vascularized microsurgical flap
