Antiinfection immunity J Ochotn Defence against extracellular pathogens






























- Slides: 34

Antiinfection immunity J. Ochotná

Defence against extracellular pathogens

Defence against extracellular pathogens § bacteria (gram-negative, gram-positive cocci, bacilli), unicellular parasites § for their elimination is necessary opsonization (C 3 b, lectins, antibodies. . . ) § neutrophilic granulocytes are chemotactic attracting to the site of the infection (C 5 a, C 3 a and chemotactic products of bacteria) § absorbed bacteria are destroyed by the microbicidal systems (products of NADP-H oxidase, hydrolytic enzymes and bactericidal substances in lysosomes)

§ phagocytes produce proinflammatory cytokines (IL-1, IL-6, TNF) that induce an increase in temperature, metabolic response of the organism and synthesis of acute phase proteins § in later stages of infection are stimulated antigen-specific mechanisms § plasma cells initially produce Ig. M isotype after isotype switching produce Ig. G 1 and Ig. A (opsonization) § s. Ig. A protect against intestinal and respiratory infections by bacteria § bacteria with a polysaccharide capsule may cause T-independent Ig. M antibody production (after the establishment to the bacteria activate the classical complement path)

§ after infection persist Ig. G, Ig. A (protective effect) and memory T and B lymphocytes § in the defense against bacterial toxins apply neutralizing antibodies (Clostridium tetani and botulinum. . . ) § "indirect toxins - bacterial Lipopolysaccharide (LPS) stimulates big number of monocytes to release TNF, which can cause septic shock § extracellular bacterial infections are especially at risk individuals with disorders in the function of phagocytes, complement and antibody production

Defence against intracellular pathogens

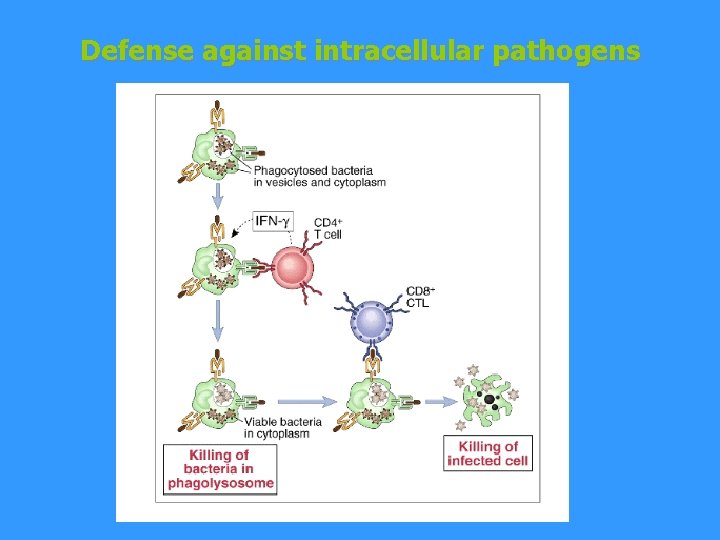
Defense against intracellular pathogens § bacteria, fungi and unicellular parasites § intracellular parasites are resistant to the microbicidal mechanisms of phagocytes § macrophages, which absorbed them, produce IL-12 → TH 1 differentiation, production of IFNg and membrane TNF → activation of macrophages and induction of i. NOS § plasma cells under the influence of IFNg produce Ig. G 2, immune complexes containing Ig. G 2 bind to Fc receptors on macrophages and thus stimulate them -

§ in the defense against intracelular parasites, which escape from phagolysosomes apply TC lymphocytes § intracellular microorganisms infections are at risk individuals with certain disorders of phagocytes and defects of T lymphocytes

Defense against intracellular pathogens

Anti-viral defence

Anti-viral defence § interferons - in infected cells is induced production of IFNa and IFN (prevents viral replication and in uninfected cells cause the anti-virus status); IFNg stimulates the conversion to activated macrophages (i. NOS) § NK cells - ADCC (Antibody-dependent cell-mediated cytotoxicity) = cytotoxic reaction depends on the antibodies; the NK-lymphocyte recognizes cell opsonized with Ig. G by stimulation Fc receptor CD 16 and then activate cytotoxic mechanisms (degranulation) § infected macrophages produce IL-12 (a strong activator of NK cells)

§ in the defense against cytopathic viruses mostly applied antibodies: § s. Ig. A inhibit mucosal adhesion of viruses (defense against respiratory viruses and enteroviruses) § neutralizing Ig. G and Ig. M antibodies activate the classical way of complement, which is capable of some viruses lysis § Ig. A and Ig. G derived in viral infection have a preventive effect in secondary infection

§ effector TC lymphocytes destroy infected cells in direct contact (granzym/perforin; Fas. L) and by produced cytokines (lymfotoxin) § some viruses after infection integrate into the host genome, where persist for years (varicella zoster, EBV, papillomavirus) § by these infections are at risk individuals with T lymphocyte immunodeficiency and with combined immune disorders § increased susceptibility to herpes infections in individuals with dysfunction of NK cells

Defense against parasites

Defense against protozoa parasites §Toxoplasma gondii, Leishmania, Trypanosoma § defense against protozoa parasites is similar to bacteria § extracellular parasites - antibodies § intracellular parasites - TH 1 lymphocytes and activated macrophages

Defense against multicellular parasites

Defense against multicellular parasites § contact of mast cells, basophils and eosinophils with parasite antigens § TH 2 stimulation under the influence of IL-4 (mast cells and other APC stimulated by parasite) § TH 2 stimulate B cells with BCR-specific parasite antigens § isotype switching under the influence of IL-4 to Ig. E § Ig. E bind to Fc RI on mast cells and basophils („antigenspecific receptors“)

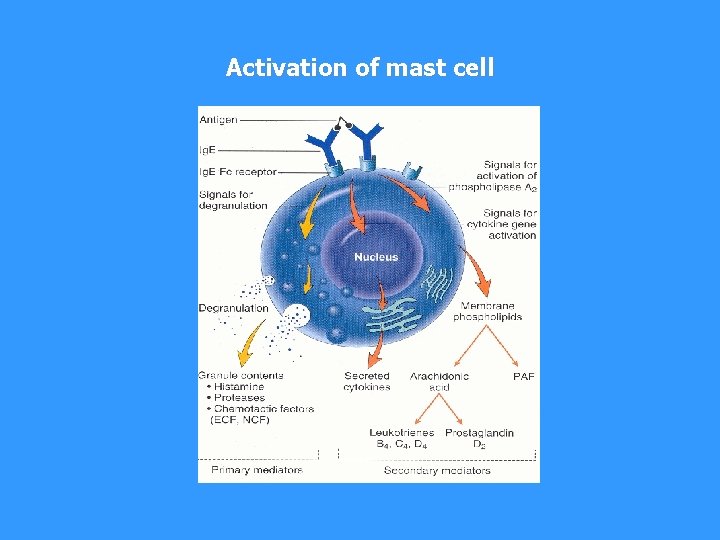
§ establish of multivalent antigen (multicellular parasite) using the Ig. E to highafinity Fc receptor for Ig. E (Fc RI) aggregation of several molecules Fc RI § initiate mast cell degranulation (cytoplasmic granules mergers with the surface membrane and release their contents) § activation of arachidonic acid metabolism (leukotriene C 4, prostaglandin PGD 2) - amplification of inflammatory responses § cytokine production by mast cell (TNF, TGF , IL-4, 5, 6 . . . )

§ in later stages are activated TH 1 and are produced antibodies of other classes § eosinophils fagocyte complexes of parasitic particles with Ig. E via their receptors for Ig. E § eosinophils use against parasites extracellular bactericidal substances released from granules (eosinophil cationic protein, protease)

Activation of mast cell

External regulation of immune response

Causal treatment a) Stem cell transplantation § for serious congenital disorders of the immune system and some lymphoproliferative and myeloproliferative disorders § complications: infectious complications Graft-versus-host disease § obtaining stem cells - collection from shovel hip bone - from umbilical cord blood - from peripheral blood after stimulation with GM-CSF

b) Gene therapy § with a suitable expression vector is introduced functional gene (to replace dysfunctional gen) into the lymphocytes or stem cells § used as a treatment for some cases of SCID

Substitution treatment § autologous stem cell transplantation following chemotherapy and radiotherapy § treatment with intravenous immunoglobulin (derived from plasma of blood donors) § substitution of C 1 inhibitor for hereditary angioedema § substitution of erythropoietin in patients with chronic renal failure § substitution of G-CSF in agranulocytosis

Immunomodulation = medical procedure to adjust the disrupted immune function Non-specific immunosuppressive therapy § nonspecific = affects not only autoreactive and aloreactive lymphocytes, but also other components of immunity (risk of reduction antiinfectious and anti tumor immunity) § used for treatment of autoimmune diseases, severe allergic conditions and for organ transplantation

Non-specific immunosuppressive therapy § corticosteroids - anti-inflammatory, immunosuppressive effects - blocking the activity of transcription factors (AP-1, NFk. B) - suppress the expression of genes (IL-2, IL-1, phospholipase A, MHC gp II, adhesion molecules) - inhibition of histamine release from basophils - higher concentrations induce apoptosis of lymfocytes § immunosuppressants affecting the metabolism of DNA - cyclophosphamide (alkylating agent) - methotrexate (antimetabolite) - azathioprine (purine analogue)

§ immunosuppressant selectively inhibiting T lymphocytes - immunosuppressive ATB: cyclosporine A, tacrolimus, rapamycin (suppressing the expression of IL-2 and IL-2 R in activated T lymphocytes) - monoclonal antibody anti-CD 3 (Immunosuppression after transplantation, treatment of rejection crises) § immunoglobulins in the immunosuppressive indication - Polyspecific intravenous immunoglobulins (Inhibition of B lymphocytes, antiidiotype activity, inhibition of cytokines, neutralization of toxins, inhibition of complement activation. . . )

Anti-inflammatory and antiallergic treatment § nonsteroidal anti-inflammatory drugs § antihistamines - blocking H 1 receptor - reduce the expression of adhesion molecules - reduce the secretion of histamine. . . § inhibitors of inflammatory cytokine - receptor antagonist for IL-1 - monoclonal antibodies against TNF - thalidomide (TNF inhibitor) § enzyme therapy - in the enzyme mixture has a major effect trypsin and bromelain - anti-inflammatory and immunomodulatory effects

Non-specific immunostimulant therapy § synthetic immunomodulators § Methisoprinol (Isoprinosine) - used in viral infections with more severe or relapsing course § bacterial extracts and lysates § Broncho-Vaxom - prevention of recurrent respiratory tract infections § Ribomunyl § products of the immune system § § § IL-2 - renal adenocarcinoma IFNa, IFN - viral hepatitis, some leukemia Erythropoietin – renal failure G-CSF, GM-CSF – neutropenia Transfer factor (blood donors leukocytes undergoing dialysis) Thymus hormones

Antigen-specific immunomodulatory therapy § specific immunomodulation = induce an immune response or tolerance against a specific antigen

a) active immunization = use of antigen to induce an immune response that can later protect against a pathogen bearing the antigen (or similar antigen) § immunization vaccines are made from inactivated or attenuated microorganisms or their antigens (polysaccharide capsule, toxins) § creates long-term immunity § activate cellular and antibody immunity § administration of antigen injectable, oral § prophylaxis § risk of infection or anaphylactic reactions

b) passive immunization § natural - transfer of maternal antibodies in fetal blood § therapeutically - the use of animal antibodies against various toxins (snake toxins, tetanus toxin, botulinum toxin) § prophylaxis - the human immunoglobulin from immunized individuals (hepatitis A, rabies, tetanus) - Anti-Rh. D antibodies - preventing maternal immunization with Rh. D+ fetus § provides a temporary (3 weeks) specific humoral immunity § the risk anaphylactic reactions

c) specific immunosuppression = induction of tolerance to a specific antigen § ongoing clinical studies § induction of tolerance by oral administration of antigen (treatment of certain autoimmune diseases) § allergen immunotherapy (pollen, insect poisons) d) vaccination against cancer § immunization by dendritic cells
