TRANSFUSION REACTIONS IMMEDIATE HEMOLYTIC TRANSFUSION REACTION Intravascular lysis









- Slides: 11

TRANSFUSION REACTIONS

IMMEDIATE HEMOLYTIC TRANSFUSION REACTION • • Intravascular lysis of transfused rbcs by complement, Ig. M Causes: Ø Transfusion of ABO-incompatible blood Ø Transfusion of ABO-incompatible plasma Ø Non-ABO antibodies • Clinical manifestations: Ø Fever (but most febrile reactions not hemolytic) Ø Back pain Ø Dark or red urine (hemoglobinuria) Ø Bronchospasm Ø Shock Ø DIC Ø Organ failure (esp kidneys) Ø Death

IMMEDIATE HEMOLYTIC TRANSFUSION REACTION Evaluation of suspected cases • • • Check blood product/paperwork to ensure correct product given Notify blood bank/transfusion service Obtain blood and urine samples: Ø Plasma and urine hemoglobin Ø Direct Coombs test Ø Repeat crossmatch/antibody screen Ø Repeat ABO/Rh typing

IMMEDIATE HEMOLYTIC TRANSFUSION REACTION Management • Stop transfusion immediately • IV crystalloid or colloid • Maintain BP, heart rate • Maintain airway • Diuresis Ø fluid, • loop diuretic (mannitol may cause volume overload) Monitor renal and coagulation status

DELAYED HEMOLYTIC TRANSFUSION REACTION • Ig. G-mediated lysis of transfused red cells (usually extravascular, non-ABO) • Usually begins 5 -10 days after transfusion • Jaundice, falling Hct, positive direct Coombs test, fever • Not generally life-threatening

FEBRILE, NONHEMOLYTIC TRANSFUSION REACTION • Cause: cytokines released by leukocytes during • • storage; antibodies to HLA antigens on transfused or donor PMNS Incidence: ≤ 0. 5% of units transfused More common in multiply transfused recipients Fever, chills, respiratory distress in severe reactions Reduced incidence/severity with leukocyte-poor product

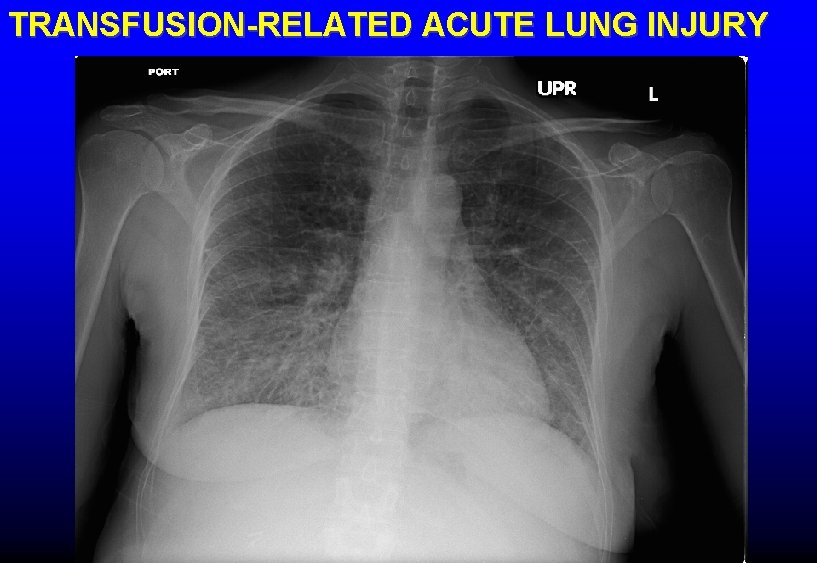
TRANSFUSION-RELATED ACUTE LUNG INJURY (TRALI) • Hypoxemia with bilateral pulmonary infiltrates • No increase in central venous or pulmonary artery • • • pressures Usually begins acutely within 6 hours of transfusion Clinical: acute respiratory distress, fever, chills Pathophysiology: 1. Underlying lung injury (eg, sepsis, pneumonia) causes PMNs to adhere to pulmonary capillaries 2. Mediators in transfused blood product (neutrophil antibodies, cytokines) activate PMNs with resultant capillary injury

TRANSFUSION-RELATED ACUTE LUNG INJURY

TRANSFUSION-RELATED ACUTE LUNG INJURY (TRALI) • Risk: FFP > platelets > RBC • Treatment: stop transfusion (if still in progress); oxygen; ventilatory support if necessary; pulse corticosteroids

OTHER ACUTE NON-INFECTIOUS COMPLICATIONS OF TRANSFUSION • Allergic reactions • Anaphylaxis (Ig. A-deficient recipient) • Lung damage from microaggregates (massive • • • transfusion) Transfusion-associated circulatory overload (“TACO”) Bacterial infection (mainly with platelet transfusion) Hypothermia (rapid infusion of refrigerated blood) Citrate toxicity/hypocalcemia (massive transfusion or apheresis) Graft-vs-host disease Air embolism

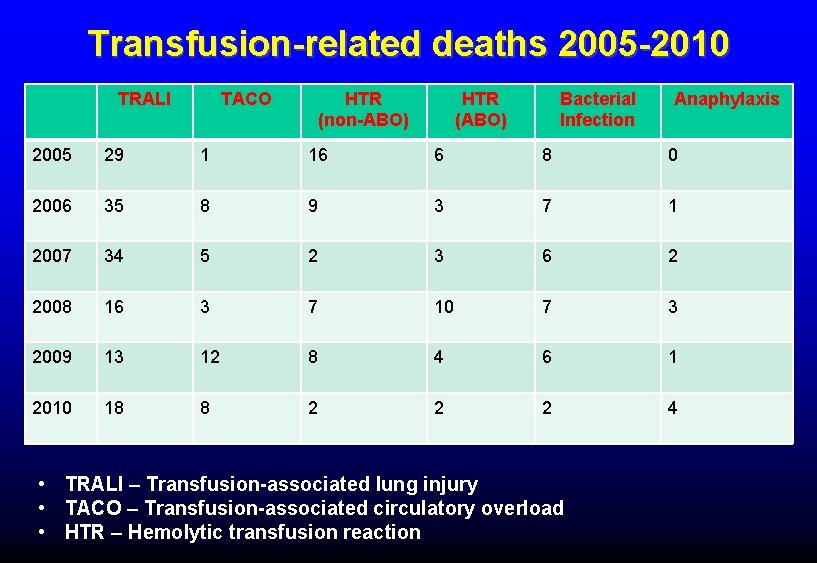
Transfusion-related deaths 2005 -2010 TRALI TACO HTR (non-ABO) HTR (ABO) Bacterial Infection Anaphylaxis 2005 29 1 16 6 8 0 2006 35 8 9 3 7 1 2007 34 5 2 3 6 2 2008 16 3 7 10 7 3 2009 13 12 8 4 6 1 2010 18 8 2 2 2 4 • TRALI – Transfusion-associated lung injury • TACO – Transfusion-associated circulatory overload • HTR – Hemolytic transfusion reaction