The Practice of Radiotherapy in Older Patients Anita

















- Slides: 27

The Practice of Radiotherapy in Older Patients Anita O’Donovan Discipline of Radiation Therapy, School of Medicine, Trinity College Dublin

Disclosure No conflict of interest to declare

Role of Radiotherapy • Approximately 50% of all cancer patients require radiotherapy as part of their disease management • An attractive treatment option for older patients, especially where surgery or chemotherapy pose too great a risk

Goals of RT Radical Aim is to cure Palliative Symptom relief & improved Qo. L Prophylactic Prevent or delay the spread of disease

Indications for Palliative Radiotherapy Symptomatic Relief • • • Pain Neurological Haemorrhage Mass effect Ulceration Obstructive symptoms – Airway (SVCO) Underused!

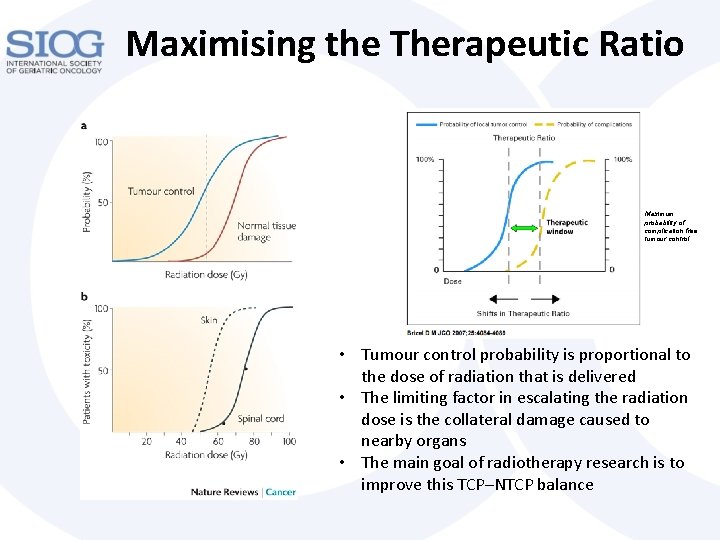
Maximising the Therapeutic Ratio Maximum probability of complication free tumour control • Tumour control probability is proportional to the dose of radiation that is delivered • The limiting factor in escalating the radiation dose is the collateral damage caused to nearby organs • The main goal of radiotherapy research is to improve this TCP–NTCP balance

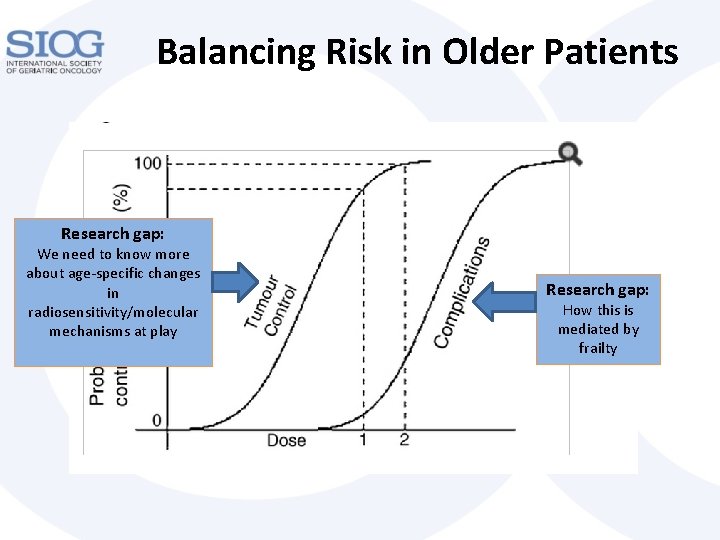
Balancing Risk in Older Patients Research gap: We need to know more about age-specific changes in radiosensitivity/molecular mechanisms at play Research gap: How this is mediated by frailty

Questions to Ask for Older Patients • Will this patient be able to tolerate a course of radiotherapy and associated toxicity? • Or is a more palliative approach suitable? • Are there alternative treatment schedules that might be more suitable for an older patient? • Is every possible attempt being made to reduce toxicity? • Will the patient be able to attend radiotherapy every day? • Does the patient have adequate support? • Does the patient have capacity to consent to treatment? • What are the patient’s wishes if treatment will result in functional decline?

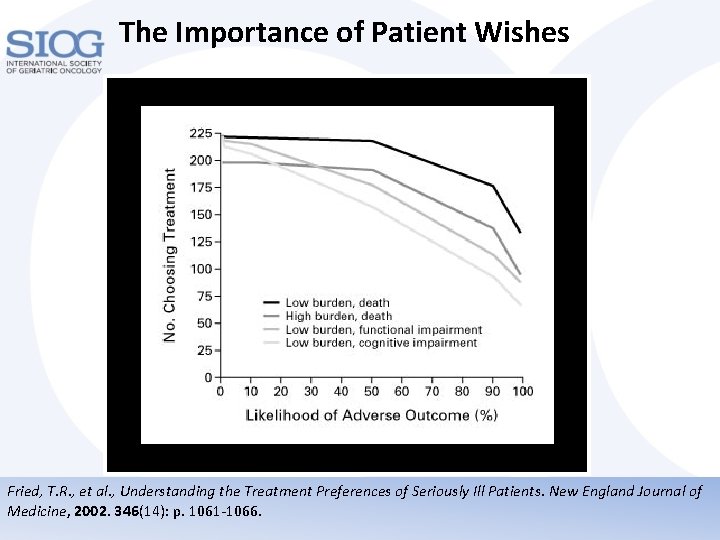
The Importance of Patient Wishes Fried, T. R. , et al. , Understanding the Treatment Preferences of Seriously Ill Patients. New England Journal of Medicine, 2002. 346(14): p. 1061 -1066.

Toxicity • Acute/Early: up to 90 days following the start of radiotherapy • Late: beyond 90 days after the onset of radiotherapy • Minimised by 2 main mechanisms: – Geometric avoidance (how our beams hit the target) – Biological sparing (fractionation) Accurate dose delivery matters!

Hypofractionation: “Low Hanging Fruit in the Radiation Oncologist’s Garden” • Shorter more focussed radiotherapy regimes • Overcome issues of access and social frailty • Suitable for patients with poor mobility and those in active caregiver roles • More convenient option Zietman, Anthony L. , et al. "The Red Journal’s Special Edition on Radiation Therapy in the Elderly. " Red 98. 4 (2017): 713 -968

CGA in Older H&N RT Patients • Deterioration during treatment supports continuous assessment • Screening tools are no substitute for full CGA • CGA deficits closely associated with HRQOL Pottel, L. , Lycke, M. , Boterberg, T. , Pottel, H. , Goethals, L. , Duprez, F. , Van Den Noortgate, N. , De Neve, W. , Rottey, S. , Geldhof, K. , Buyse, V. , Kargar-Samani, K. , Ghekiere, V. and Debruyne, P. R. (2014), Serial comprehensive geriatric assessment in elderly head and neck cancer patients undergoing curative radiotherapy identifies evolution of multidimensional health problems and is indicative of quality of life. European Journal of Cancer Care, 23: 401– 412. doi: 10. 1111/ecc. 12179

Older Patients Don’t Receive Guideline Concordant Care We have no guidelines for the majority of older patients! Mc. Aleese J, Baluch S, Drinkwater K, Bassett P, Hanna GG. The Elderly are Less Likely to Receive Recommended Radical Radiotherapy for Non-small Cell Lung Cancer. Clinical Oncology. 2017 Sep 1; 29(9): 593 -600. Travel dictates patient’s treatment decisions about radiotherapy

Case Study: Prostate Cancer

Hypofractionation: Less is More • CHHi. P (Conventional or Hypofractionated High- dose Intensity Modulated Radiotherapy in Prostate Cancer) (Lancet Oncol 2016; 17[8]: 10471060, PMID: 27339115), • NRG Oncology 0415 trial (J Clin Oncol 2016; 34[20]: 2325 -2330, PMID: 27044935) • Ontario Clinical Oncology Group/Trans-Tasman Radiation Oncology Group trial, PROFIT (PROstate Fractionated Irradiation Trial) (J Clin Oncol 2017 Mar 15. [Epub ahead of print], PMID: 28296582). 4/5 weeks versus 7/8 weeks

Case Study: Breast Cancer

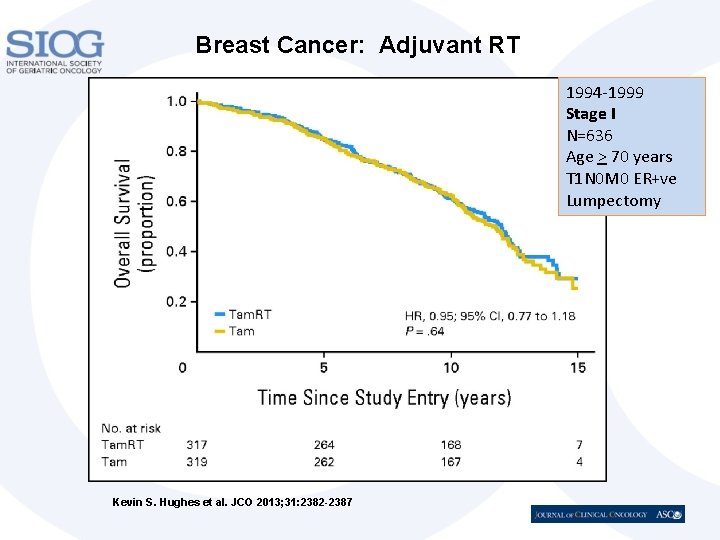
Breast Cancer: Adjuvant RT 1994 -1999 Stage I N=636 Age > 70 years T 1 N 0 M 0 ER+ve Lumpectomy Kevin S. Hughes et al. JCO 2013; 31: 2382 -2387

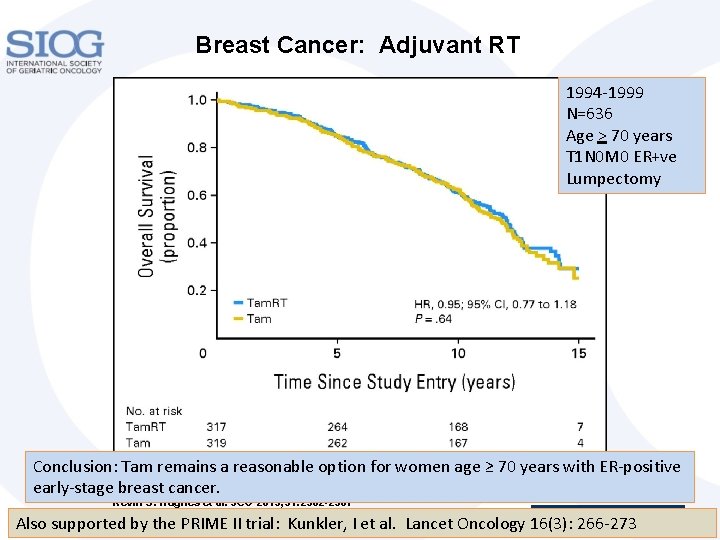
Breast Cancer: Adjuvant RT 1994 -1999 N=636 Age > 70 years T 1 N 0 M 0 ER+ve Lumpectomy Conclusion: Tam remains a reasonable option for women age ≥ 70 years with ER-positive early-stage breast cancer. Kevin S. Hughes et al. JCO 2013; 31: 2382 -2387 Also supported by the PRIME II trial: Kunkler, I et al. Lancet Oncology 16(3): 266 -273

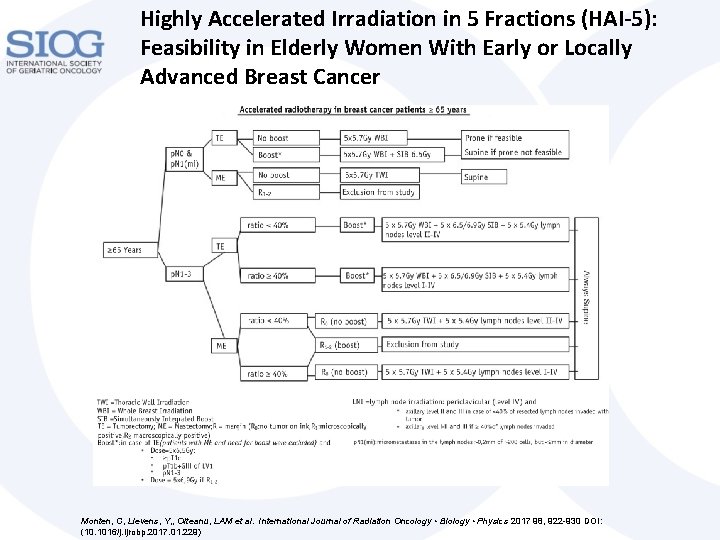
Highly Accelerated Irradiation in 5 Fractions (HAI-5): Fig. 1 Feasibility in Elderly Women With Early or Locally Advanced Breast Cancer Monten, C, Lievens, Y, , Olteanu, LAM et al. International Journal of Radiation Oncology • Biology • Physics 2017 98, 922 -930 DOI: (10. 1016/j. ijrobp. 2017. 01. 229)

Case Study: GBM

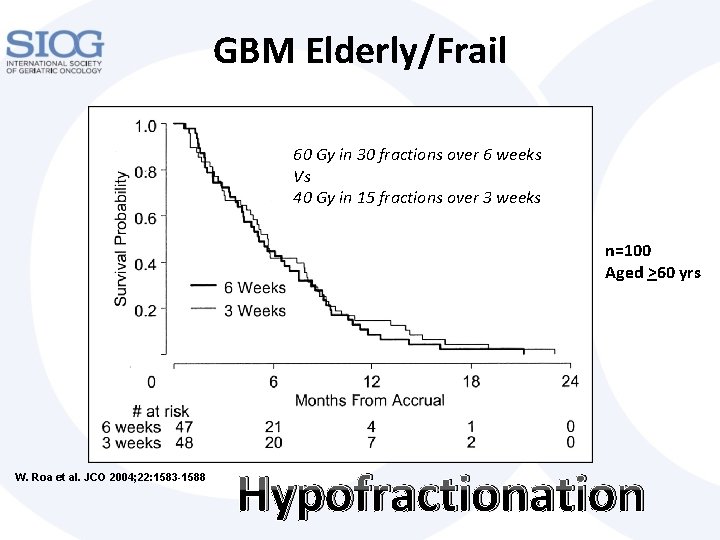
GBM Elderly/Frail 60 Gy in 30 fractions over 6 weeks Vs 40 Gy in 15 fractions over 3 weeks n=100 Aged >60 yrs W. Roa et al. JCO 2004; 22: 1583 -1588 Hypofractionation

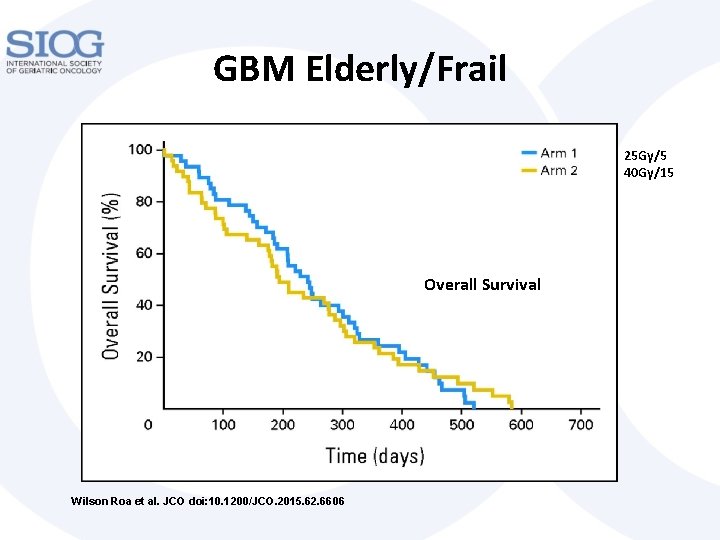
GBM Elderly/Frail 25 Gy/5 40 Gy/15 Overall Survival Wilson Roa et al. JCO doi: 10. 1200/JCO. 2015. 62. 6606

Cranial Irradiation and Dementia • Retrospective study of 1 year survivors treated at MSKCC • N=47 • 5/47 (11%) patients treated with WBRT developed severe dementia: • Schedules used: 6 Gy X 3, 4 Gy X 3, 5 Gy X 3, 3 Gy X 5, 3 Gy X 10, 5 Gy X 3, 3 Gy X 4, 6 Gy X 3, 4 Gy X 3 • 0/15 patients treated with <3 Gy/# had dementia • Dementia associated with high dose/# [Cognitive impairment further reduced by use of hippocampal sparing RT] De. Angelis, L. M. , Delattre, J. Y. , & Posner, J. B. (1989). Radiation‐induced dementia in patients cured of brain metastases. Neurology, 39(6), 789 -789.

Knowledge Gaps in Radiation Therapy

Role of CGA

Key Questions to Ask the RO • Is this the only radiotherapeutic option for this patient? • Is a different fractionation schedule possible/feasible/effective? • What is the anticipated toxicity of treatment? • What efforts can be made to reduce toxicity and manage pre-existing concerns? • What supportive care options will the patient have access to during radiotherapy and during follow-up?

Conclusion: An Integrated Approach Needed “broader than a restricted definition of technical maintenance and quality control of equipment and treatment delivery …. should encompass a comprehensive approach to all activities in the radiotherapy department from the moment a patient enters it until the moment they leave, and also continuing into the follow-up period”(ESTRO, 1998) “Quality geriatric care has been defined as agingsensitive, evidence-based, individualised care that promotes informed decision-making and is continuous across settings” (Barba, 2012)