General Principles of Radiotherapy Anita ODonovan Discipline of


















- Slides: 32

General Principles of Radiotherapy Anita O’Donovan Discipline of Radiation Therapy, School of Medicine, Trinity College Dublin Email: anita. odonovan@tcd. ie @anitaodonovan 1

Disclosure No conflicts of interest to declare

Objectives • What is radiotherapy? • How does it work? • Patient pathway through radiotherapy • Advances in radiation therapy

Objectives • What is radiotherapy? • How does it work? • Patient pathway through radiotherapy • Advances in radiation therapy

What is Radiotherapy? Radiation therapy uses high-energy X-rays to destroy or damage cancer cells Goal: to target radiation to cancer cells while keeping the dose to normal cells as low as possible Radical Vs Palliative Vs Prophylactic Vs Abscopal

Different Modalities • External Beam Radiotherapy • Internal – Brachytherapy (Interstitial/Intracavitary) Ø Dose is measured in Gray (Gy) Ø Prescribed by Radiation Oncologist as Total Dose/Fraction Dose e. g. 50 Gy/25# (conventional fractionation) Ø 50% of cancer patients require RT at some stage of their cancer journey

Objectives • What is radiotherapy? • How does it work? • Patient pathway through radiotherapy • Advances in radiation therapy

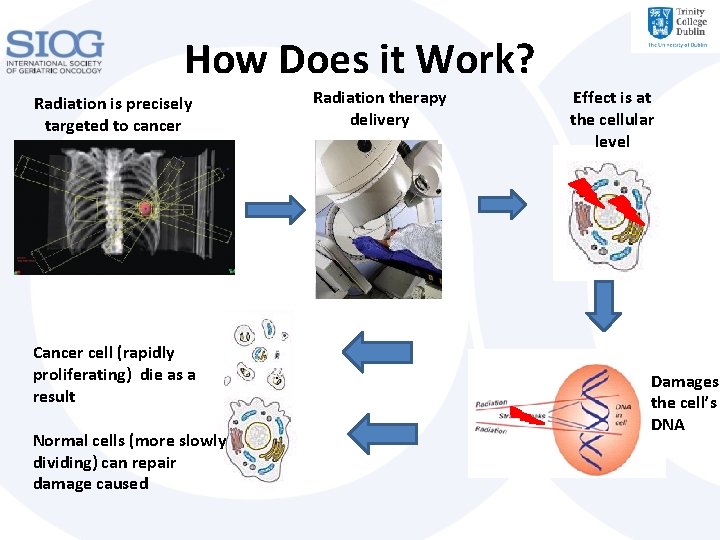
How Does it Work? Radiation is precisely targeted to cancer Cancer cell (rapidly proliferating) die as a result Normal cells (more slowly dividing) can repair damage caused Radiation therapy delivery Effect is at the cellular level Damages the cell’s DNA

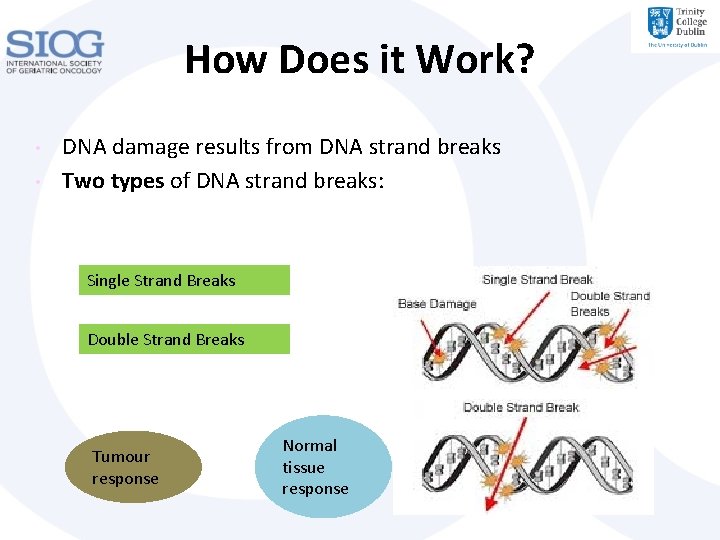
How Does it Work? • • DNA damage results from DNA strand breaks Two types of DNA strand breaks: Single Strand Breaks Double Strand Breaks Tumour response Normal tissue response

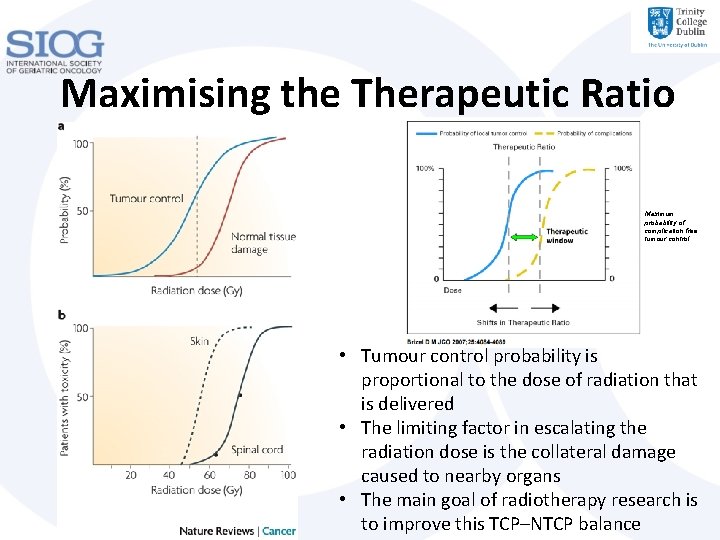
Maximising the Therapeutic Ratio Maximum probability of complication free tumour control • Tumour control probability is proportional to the dose of radiation that is delivered • The limiting factor in escalating the radiation dose is the collateral damage caused to nearby organs • The main goal of radiotherapy research is to improve this TCP–NTCP balance

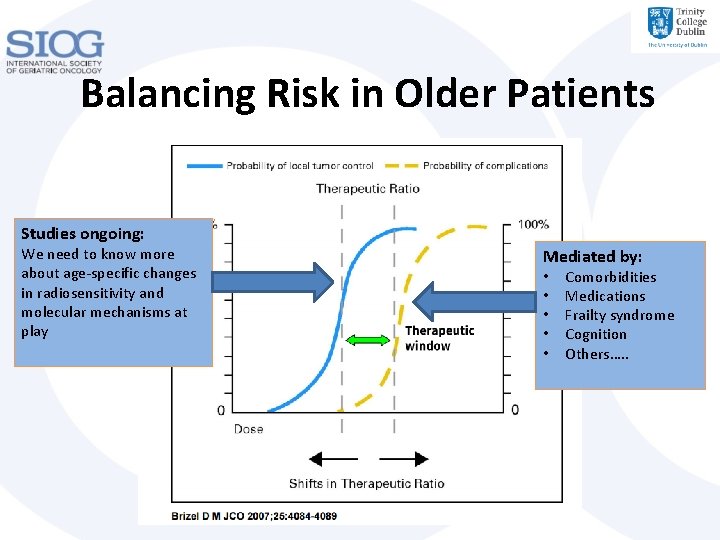
Balancing Risk in Older Patients Studies ongoing: We need to know more about age-specific changes in radiosensitivity and molecular mechanisms at play Mediated by: • • • Comorbidities Medications Frailty syndrome Cognition Others…. .

Toxicity • Acute/Early: up to 90 days following the start of radiotherapy • Late: beyond 90 days after the onset of radiotherapy • Minimised by 2 main mechanisms: – Geometric avoidance (how our beams hit the target) – Biological sparing (fractionation) Accurate dose delivery matters!

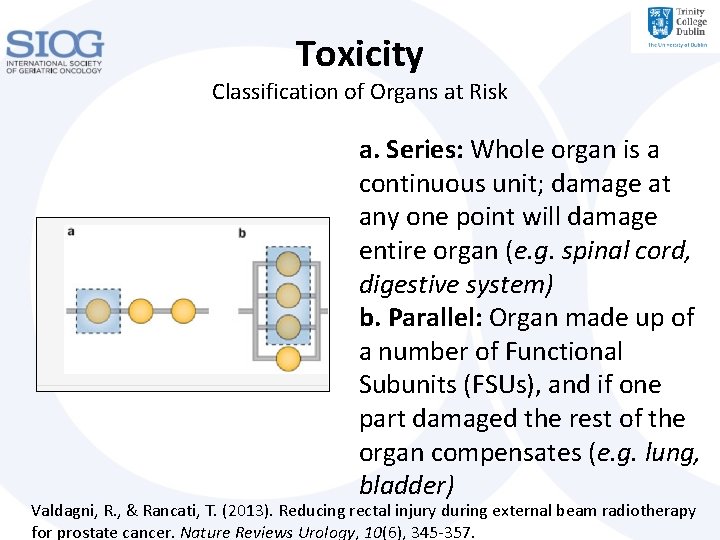
Toxicity Classification of Organs at Risk a. Series: Whole organ is a continuous unit; damage at any one point will damage entire organ (e. g. spinal cord, digestive system) b. Parallel: Organ made up of a number of Functional Subunits (FSUs), and if one part damaged the rest of the organ compensates (e. g. lung, bladder) Valdagni, R. , & Rancati, T. (2013). Reducing rectal injury during external beam radiotherapy for prostate cancer. Nature Reviews Urology, 10(6), 345 -357.

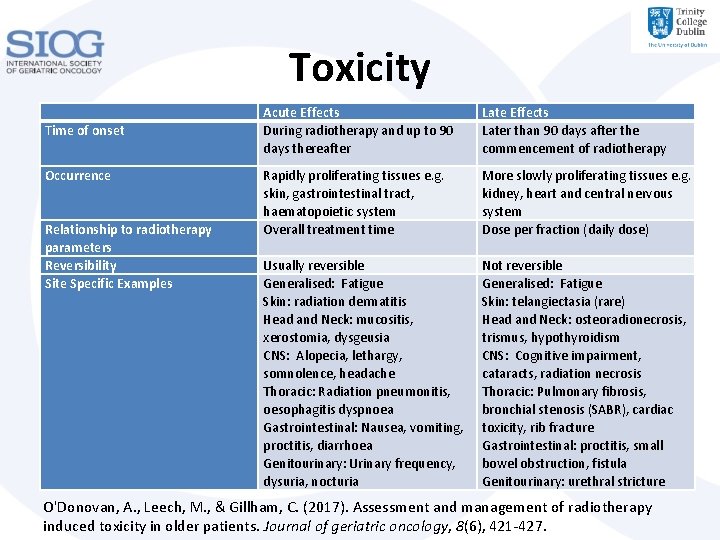
Toxicity Time of onset Acute Effects During radiotherapy and up to 90 days thereafter Late Effects Later than 90 days after the commencement of radiotherapy Occurrence Rapidly proliferating tissues e. g. skin, gastrointestinal tract, haematopoietic system Overall treatment time More slowly proliferating tissues e. g. kidney, heart and central nervous system Dose per fraction (daily dose) Usually reversible Generalised: Fatigue Skin: radiation dermatitis Head and Neck: mucositis, xerostomia, dysgeusia CNS: Alopecia, lethargy, somnolence, headache Thoracic: Radiation pneumonitis, oesophagitis dyspnoea Gastrointestinal: Nausea, vomiting, proctitis, diarrhoea Genitourinary: Urinary frequency, dysuria, nocturia Not reversible Generalised: Fatigue Skin: telangiectasia (rare) Head and Neck: osteoradionecrosis, trismus, hypothyroidism CNS: Cognitive impairment, cataracts, radiation necrosis Thoracic: Pulmonary fibrosis, bronchial stenosis (SABR), cardiac toxicity, rib fracture Gastrointestinal: proctitis, small bowel obstruction, fistula Genitourinary: urethral stricture Relationship to radiotherapy parameters Reversibility Site Specific Examples O'Donovan, A. , Leech, M. , & Gillham, C. (2017). Assessment and management of radiotherapy induced toxicity in older patients. Journal of geriatric oncology, 8(6), 421 -427.

Objectives • What is radiotherapy? • How does it work? • Patient pathway through radiotherapy • Advances in radiation therapy

Patient Pathway

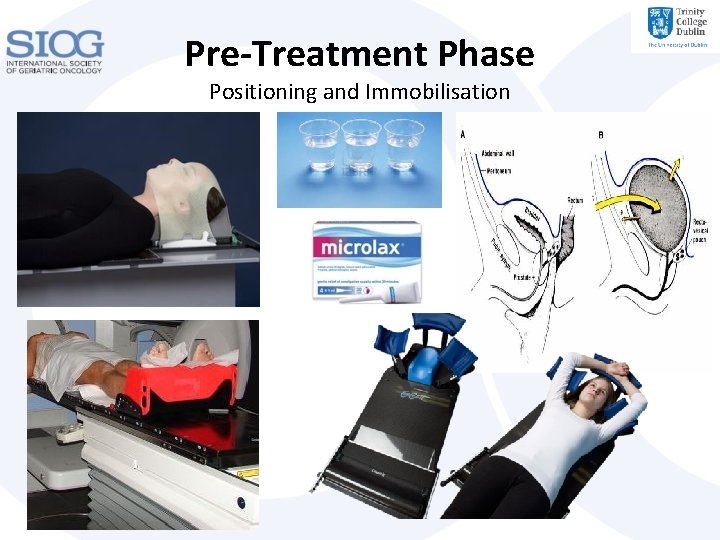
Pre-Treatment Phase Positioning and Immobilisation Ed. ac. uk

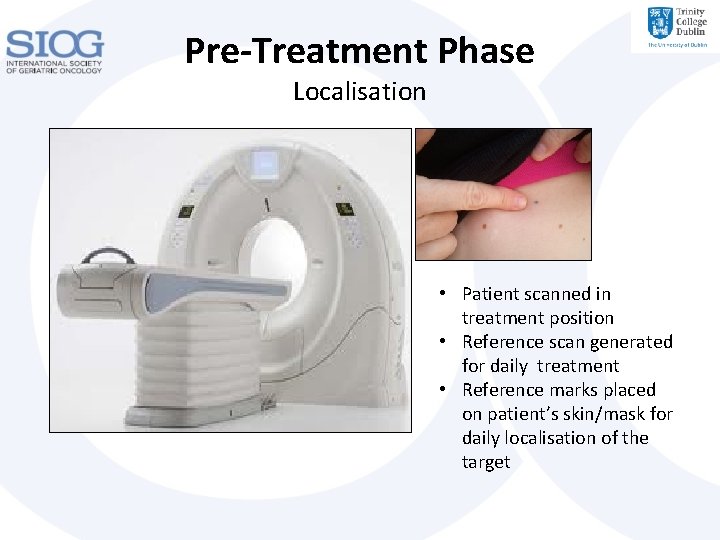
Pre-Treatment Phase Localisation • Patient scanned in treatment position • Reference scan generated for daily treatment • Reference marks placed on patient’s skin/mask for daily localisation of the target

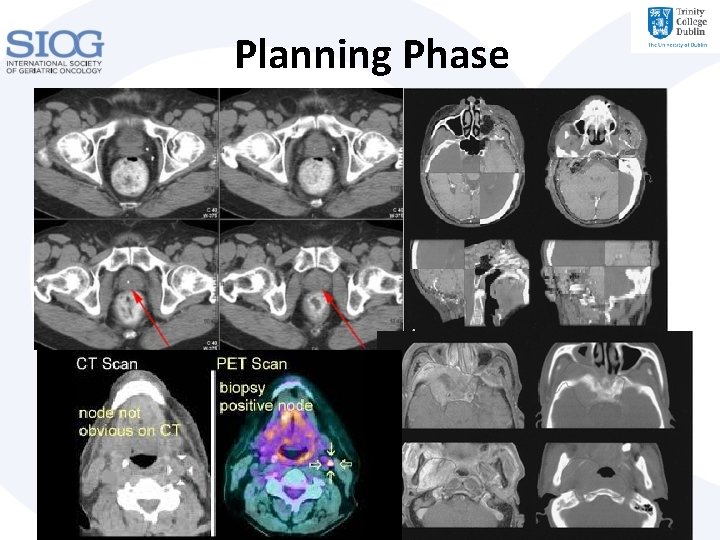
Planning Phase

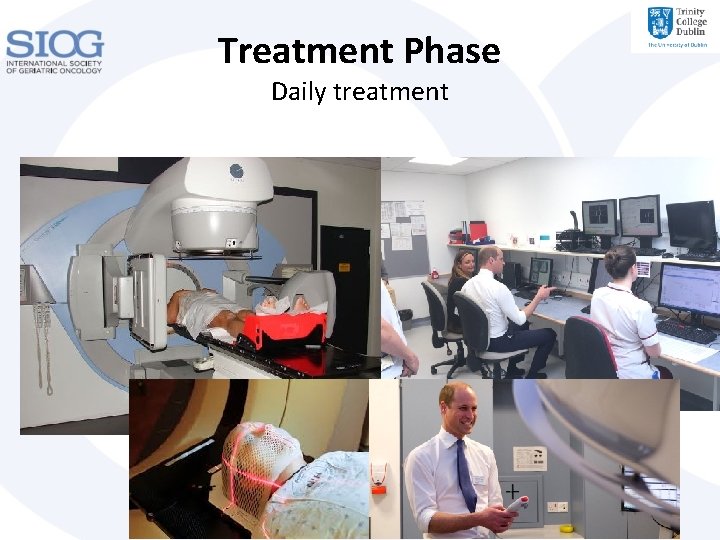
Treatment Phase Daily treatment

Treatment Phase Linear Accelerator

Fractionation Schedules • Conventional: 1. 8 -2 Gy/day/5 days per week • Single fraction: usually palliative setting where late effects are not a concern e. g. 8 Gy for bone metastases • Hypofractionation: ↑dose/fraction; ↓overall dose & OTT • Hyperfractionation: ↓ dose/fraction; ↑overall dose; OTT unchanged • Accelerated fractionation: conventional dose/fraction & overall dose; OTT significantly reduced • Split course: Conventional fractionation schedule with treatment gap of 1 -2 weeks to overcome toxicity; ↑OTT *OTT=Overall Treatment Time

Objectives • What is radiotherapy? • How does it work? • Patient pathway through radiotherapy • Advances in radiation therapy

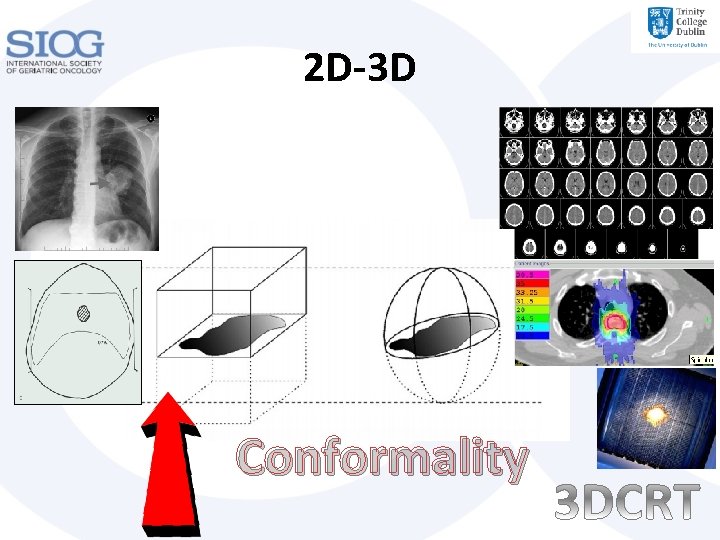
2 D-3 D Conformality

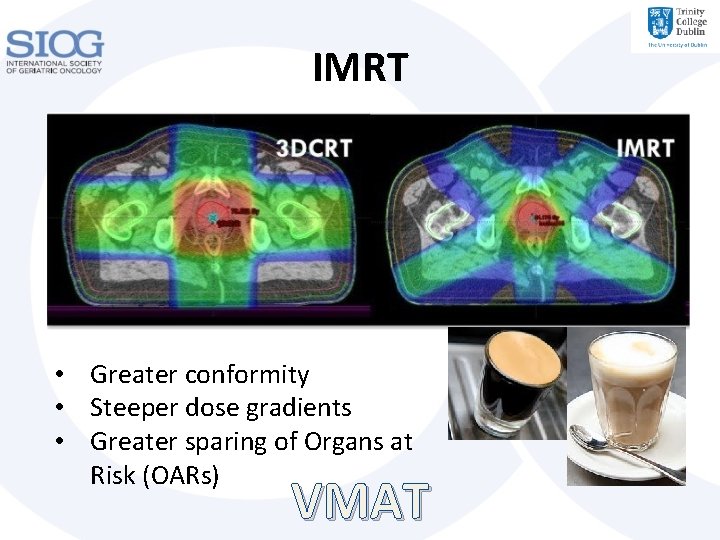
IMRT • Greater conformity • Steeper dose gradients • Greater sparing of Organs at Risk (OARs) VMAT

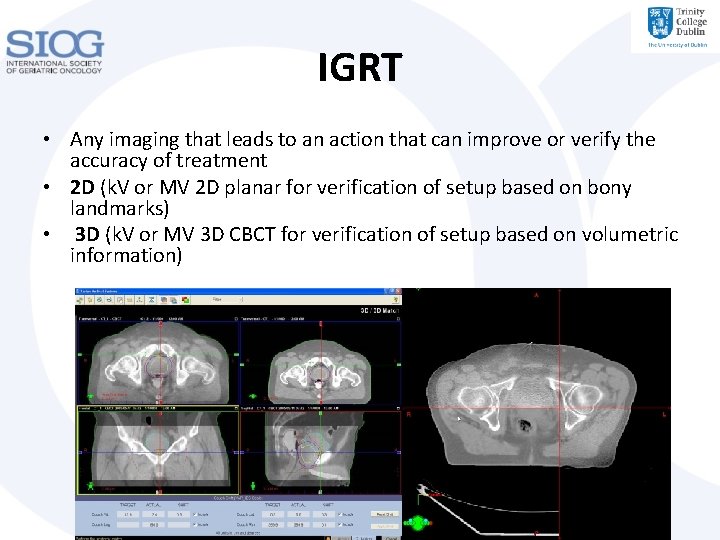
IGRT • Any imaging that leads to an action that can improve or verify the accuracy of treatment • 2 D (k. V or MV 2 D planar for verification of setup based on bony landmarks) • 3 D (k. V or MV 3 D CBCT for verification of setup based on volumetric information)

Proton Therapy Thariat, J. , et al. "Using Proton Beam Therapy in the Elderly Population: A Snapshot of Current Perception and Practice. " International Journal of Radiation Oncology*Biology*Physics. http: //provisionproton. com/static/uploads/VV-button-Pv. C. jpg

Stereotactic • Stereotactic: refers to precise positioning in three-dimensional space i. e. focal irradiation • Much smaller treatment volumes than conventional radiotherapy=less toxicity • SRS (single fraction) Vs SRT (Generally 2 -6 fractions) • 3 Main Types: ØGamma knife (cranial only) ØCyberknife (cranial and extra-cranial) ØLinear accelerator (cranial and extra-cranial)

Stereotactic Cyberknife

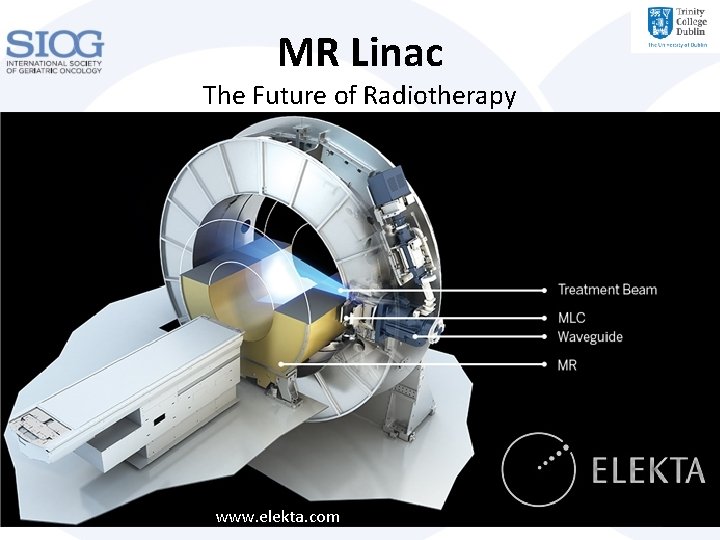
MR Linac The Future of Radiotherapy www. elekta. com

Objectives • What is radiotherapy? • How does it work? • Patient pathway through radiotherapy • Advances in radiation therapy

Thank You! Email: anita. odonovan@tcd. ie @anitaodonovan 1