Nutrition in the Patient with Anorexia and Cachexia

















- Slides: 21

Nutrition in the Patient with Anorexia and Cachexia Jeanette N. Keith, M. D. Associate Professor of Medicine Departments of Nutrition Sciences and Medicine University of Alabama at Birmingham

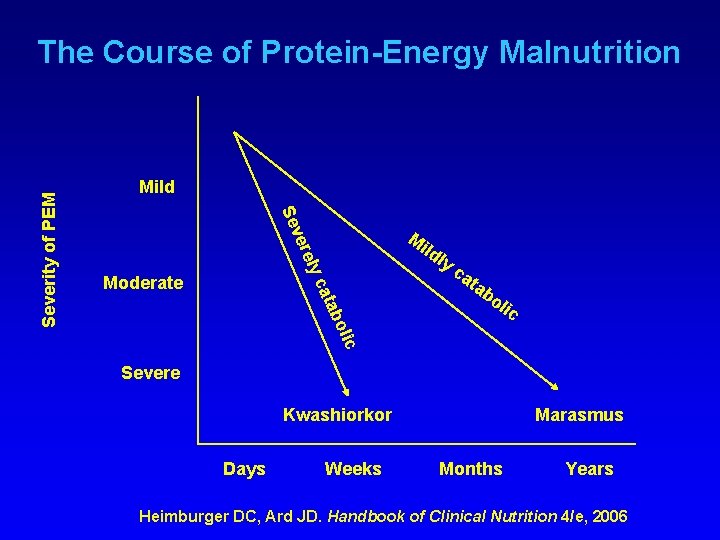
Protein-Energy Malnutrition Two major types • Marasmus • Kwashiorkor (AKA: Protein Calorie Malnutrition) Heimburger DC, Ard JD. Handbook of Clinical Nutrition 4/e, 2006

Marasmus Clinical setting Decreased energy intake Time course to develop Months or years Clinical features Starved appearance Weight < 80% standard for height Triceps skinfold < 3 mm Mid-arm muscle circumference < 15 cm Creatinine-height index <60% standard Laboratory findings Clinical course Reasonably preserved responsiveness to short term stress Mortality Low, unless related to underlying disease Heimburger DC, Ard JD. Handbook of Clinical Nutrition 4/e, 2006

Kwashiorkor Clinical setting Time course to develop Clinical features Laboratory findings Clinical course Mortality Decreased protein intake during stress state Weeks Well-nourished appearance Easy hair pluckability Edema Serum albumin < 2. 8 g/dl TIBC < 200 μg/dl Lymphocytes < 1500/mm 3 Anergy Infections Poor wound healing, pressure sores, skin breakdown High Heimburger DC, Ard JD. Handbook of Clinical Nutrition 4/e, 2006

Minimum Diagnostic Criteria Kwashiorkor • Serum albumin < 2. 8 g/dl • At least one of the following: Marasmus • Triceps skinfold < 3 mm • Mid-arm muscle circumference < 15 cm • Poor wound healing, decubitus ulcers, or skin breakdown • Easy hair pluckability • Edema Heimburger DC, Ard JD. Handbook of Clinical Nutrition 4/e, 2006

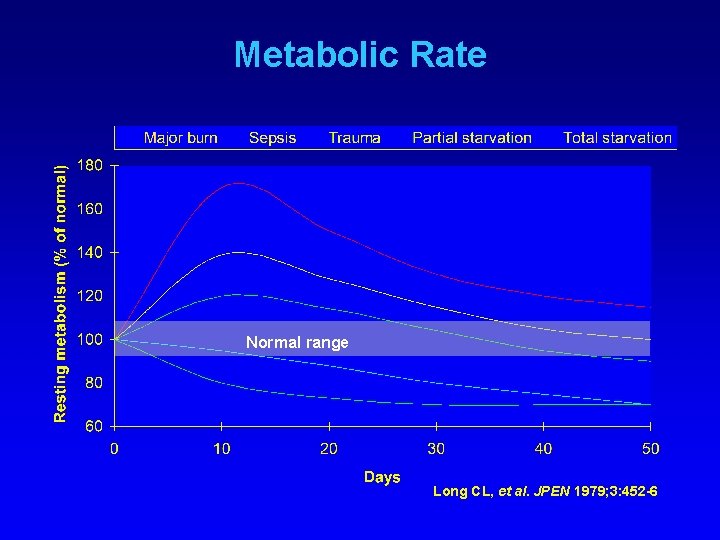
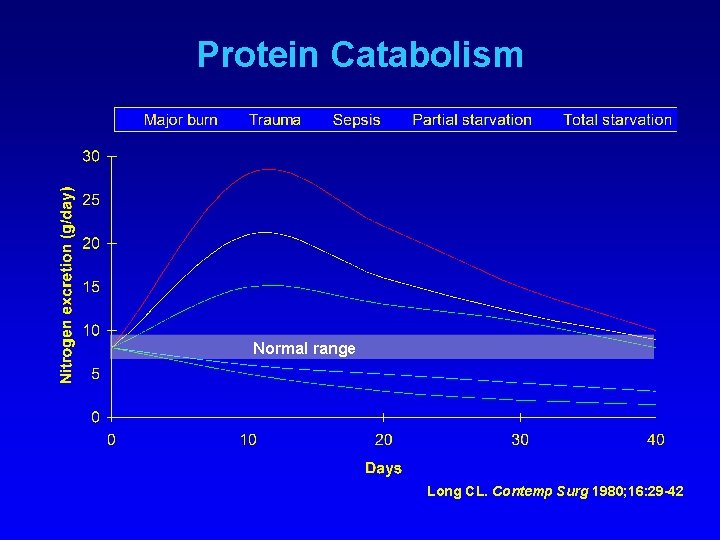
Physiology of Starvation & Stress Physiologic characteristics Hypometabolic, non-stressed patient (cachectic, marasmic) Hypermetabolic, stressed patient (kwashiorkor-risk) Cytokines, catecholamines, glucagon, cortisol, insulin ↓ ↑ Metabolic rate ↓ ↓ ↑ ↑ ↑ Normal Abnormal Proteolysis, gluconeogenesis Urea excretion Fat catabolism, fatty acid utilization Adaptation to starvation Heimburger DC, Ard JD. Handbook of Clinical Nutrition 4/e, 2006

Metabolic Rate Normal range Long CL, et al. JPEN 1979; 3: 452 -6

Protein Catabolism Normal range Long CL. Contemp Surg 1980; 16: 29 -42

Mild Se M ver ild ly ely Moderate ca ta bo lic abo cat Severity of PEM The Course of Protein-Energy Malnutrition Severe Kwashiorkor Days Weeks Marasmus Months Years Heimburger DC, Ard JD. Handbook of Clinical Nutrition 4/e, 2006

Case Presentation • 27 -year old female with a 35 pound weight loss in the last six months presents to your morning clinic with her mother • In the last two weeks, she has lost an additional 10 pounds. She reports decreased po intake, mild epigastric discomfort and bloating • The patient’s main concern is the loss of appetite, and fatigue • She is 5’ 7” tall and weighs 67 pounds, (BP 90/40, P 60, R 18, T 97. 8)

Case Presentation • The patient’s mother calls you at 6 pm stating that her daughter is having palpitations and is on her way to the emergency room. • The ER staff pages you. Her ECG reveals torsade des pointes and her potassium is 1. 9. • She is admitted to the Cardiology service and you are consulted for feeding recommendations.

Case Presentation • What do you recommend now? – Immediate placement of a PICC catheter for TPN initiation. – Have the inpatient team place a dobhoff and begin tube feedings – Call GI procedures to arrange for PEG placement and enteral feedings. – Call Dietary for a 1600 kcal diet and begin a calorie count – Intravenous fluids while correcting the potassium and awaiting other lab studies.

Case Presentation • The patient’s potassium is now normal but her course has been complicated by recurrent vomiting. • EGD reveals a decreased gastric motility and a dilated duodenum bulb with normal motility in the second portion of the duodenum. • What do you recommend next? – Advance her diet to clear liquids – Begin TPN – Place a post-pyloric feeding tube and begin enteral nutrition

Case Presentation • You place a post pyloric feeding tube for enteral nutrition. • What weight do you use for caloric provision? – Ideal Body Weight – Actual Weight – Adjusted Body Weight • How many calories per kilogram per day do you recommend? – – 35 -40 kcal/kg/d 25 -30 kcal/kg/d 15 -20 kcal/kg/d 20 -30 kcal/kg/d

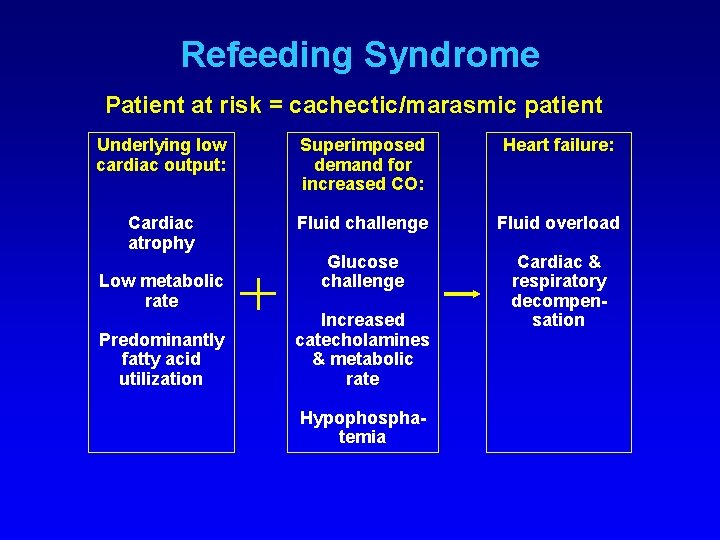
Case Presentation • On the morning after beginning her enteral feeding, the patient complains of palpitations and pain in her hands. • On exam, her hands are swollen and she has pedal edema. Pulmonary exam reveals rales. • Her potassium is now 2. 9, phophorus is 1. 8 and magnesium is 1. 4. • Diagnosis?

Refeeding Syndrome Patient at risk = cachectic/marasmic patient Underlying low cardiac output: Superimposed demand for increased CO: Heart failure: Cardiac atrophy Fluid challenge Fluid overload Glucose challenge Cardiac & respiratory decompensation Low metabolic rate Predominantly fatty acid utilization Increased catecholamines & metabolic rate Hypophosphatemia

Case Presentation • The patient is admitted to inpatient psychiatry for the treatment of anorexia/bulimia nervosa. • After 4 weeks on tube feedings, she was successfully transitioned to oral diet. • At discharge, her weight was 99 pounds.

Selective Refeeding Approaches • Hypometabolic, cachectic/marasmic patient – Aim = rebuild cautiously to avoid hypophosphatemia & repletion heart failure – Refeed gradually with » a portion of fuel as fat » ADEQUATE PHOSPHORUS – Days 1 -2 – BEE x 0. 8 – Days 3 -4 – BEE x 1. 0 – Days 4 -6 – BEE x 1. 1 -1. 4 – Days 7+ – BEE x 2 if weight gain is desired

Selective Refeeding Approaches • Hypermetabolic, stressed patient – Aim = Replace catabolic losses – Refeed aggressively but not excessively – Can often achieve calorie & protein goals within 48 hours • Patient with mixed marasmic/kwashiorkor (starved but also stressed) – Metabolism is accelerated by stress – Therefore, generally feed as you would a patient with kwashiorkor – But watch carefully for refeeding syndrome

Key Points To Remember • The metabolic response to starvation for the hypometabolic patient is to reduce their metabolic rate and use fat as the primary fuel source • Visceral protein stores are preserved in early in the clinical course of the hypometabolic, starved state • In underweight patients, use the actual body weight to avoid overfeeding. • Monitor for re-feeding syndrome with oral, enteral or parenteral nutrition.

Take Home Points • The stressed hypermetabolic patient is more likely to suffer the consequences of underfeeding. • The starved, unstressed patient is at risk for the complications of overfeeding and rapid re-feeding. • If protein calorie malnutrition (kwashiorkor-type) predominates, vigorous nutrition therapy is urgent. • If marasmus predominates, feeding should be more cautious.