Neisseria Meningitidis Dr Ajay Poudel Department of Microbiology

Neisseria Meningitidis Dr. Ajay Poudel Department of Microbiology, CMC

• Also known as Meningococcus, Diplococcus intracellularis meningitidis • Meningococcal meningitis /cerebrospinal meningitis/ cerebrospinal fever • Septicaemia • First isolated by Weichselbaum in 1887 from spinal fluid of a case of meningitis
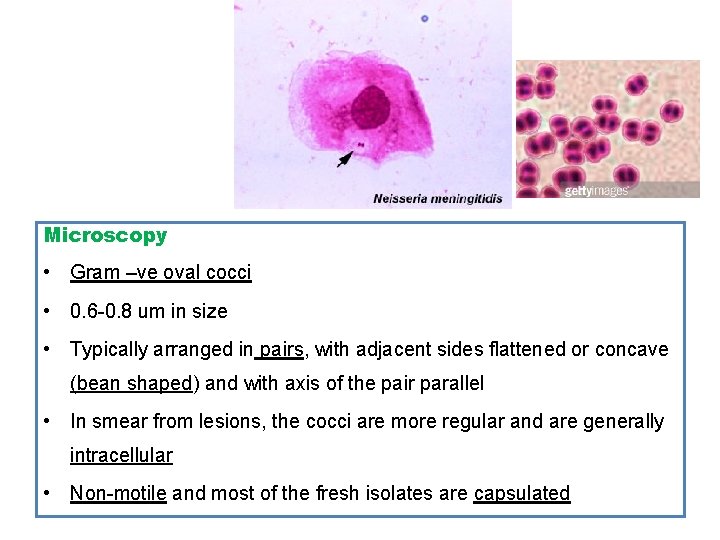
Microscopy • Gram –ve oval cocci • 0. 6 -0. 8 um in size • Typically arranged in pairs, with adjacent sides flattened or concave (bean shaped) and with axis of the pair parallel • In smear from lesions, the cocci are more regular and are generally intracellular • Non-motile and most of the fresh isolates are capsulated

Cultural characteristics • Fastidious do not grow on ordinary culture media. • Strict aerobes, no growth occur anaerobically. • The optimum temperature for growth is 35 -36°C & optimum p. H 7. 47. 6 • Growth is facilitated by 5 -10% CO 2. Non selective media • Blood agar, Chocolate agar, Muller-Hinton agar. Selective media • Modified Thayer Martin medium
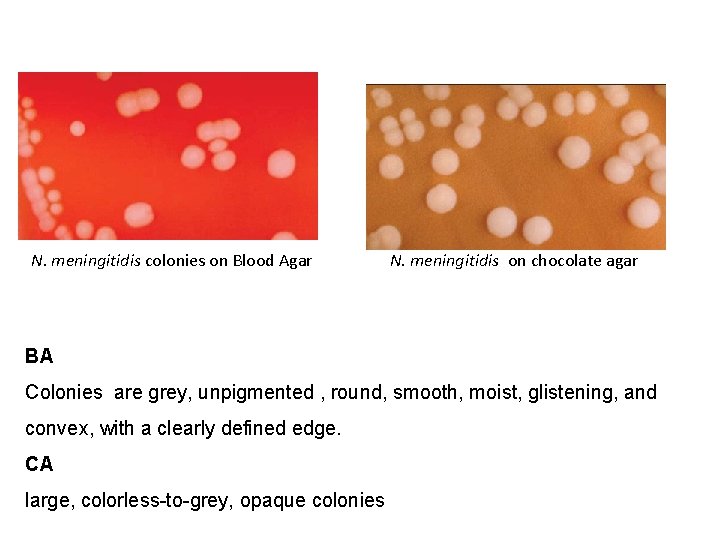
N. meningitidis colonies on Blood Agar N. meningitidis on chocolate agar BA Colonies are grey, unpigmented , round, smooth, moist, glistening, and convex, with a clearly defined edge. CA large, colorless-to-grey, opaque colonies

Biochemical Reactions • Catalase test: +ve • Oxidase test: +ve • Acid production but not gas from glucose and maltose

Antigenic properties and classification • Based on capsular polysaccaride antigens: 13 serogroups • Serogroups A, B, C, W 135 and Y are the 5 most common causes of bacterial meningitis. • Serogroup A has been the most common cause of epidemics in Africa and Asia. • Serogroups are further classified into serotypes and subtypes based on outer membrane proteins and polysaccharides

Virulence factors 1. Adhesion factors • Pilli to attach to the mucosa of oropharynx • Pilli also mediate to attach to meningeal tissue 2. Capsule: Capsular polysachharide is antiphagocytic 3. Lipopolysachharide (LPS, endotoxin): very potent, ten times more than most other endotoxins 4. Ig. A protease: cleaves Ig. A on mucosa and protect from secretory Ig. A

Transmission • Through droplets of respiratory or throat secretions from carriers. • Close and prolonged contact – such as kissing, sneezing or coughing, or living in close quarters (such as a dormitory, sharing eating or drinking utensils) with an infected person (a carrier) – facilitates the spread of the disease. • The average incubation period is 4 days, but can range between 2 and 10 days. • 10% to 20% of the population carries Neisseria meningitidis - upper respiratory tract
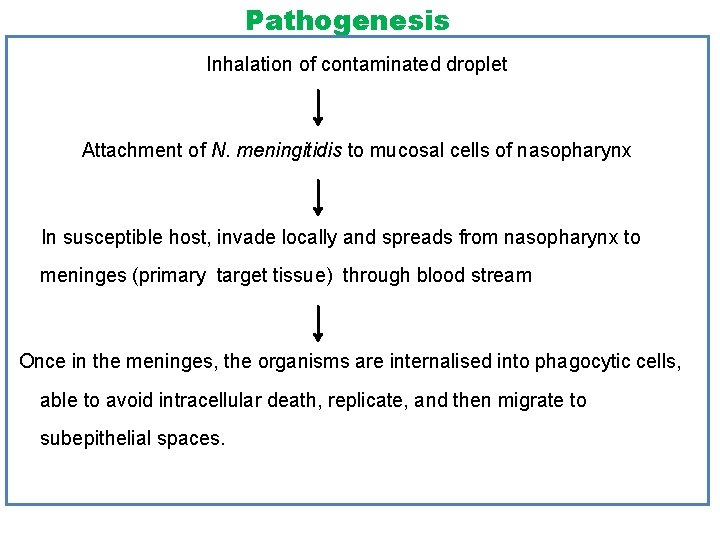
Pathogenesis Inhalation of contaminated droplet Attachment of N. meningitidis to mucosal cells of nasopharynx In susceptible host, invade locally and spreads from nasopharynx to meninges (primary target tissue) through blood stream Once in the meninges, the organisms are internalised into phagocytic cells, able to avoid intracellular death, replicate, and then migrate to subepithelial spaces.

Clinical syndrome 1. 2. A febrile illness – self –limiting is the modest form of meningococcal infection. – Blood culture may be positive Meningitis (cerebrospinal fever): – After reaching CNS, a suppurative lesion of the meninges set up Involving the surface of the spinal cord as well as the base and cortext of brain 3. Meningococcal septicaemia – Bacterial endotoxin probably plays role – Acute adrenal insufficiency (Waterhouse- Frederichsen syndrome) may occur during fulminating meningococcal septicaemia 4. Other syndrome: – Pneumonia, arthritis, and urethritis – A repiratory tract infection usually preceeds menigococcal pneumonia
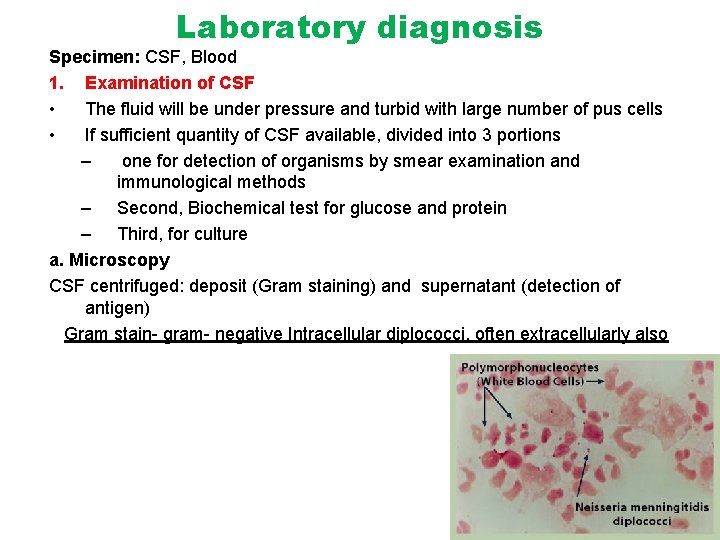
Laboratory diagnosis Specimen: CSF, Blood 1. Examination of CSF • The fluid will be under pressure and turbid with large number of pus cells • If sufficient quantity of CSF available, divided into 3 portions – one for detection of organisms by smear examination and immunological methods – Second, Biochemical test for glucose and protein – Third, for culture a. Microscopy CSF centrifuged: deposit (Gram staining) and supernatant (detection of antigen) Gram stain- gram- negative Intracellular diplococci, often extracellularly also

B. Biochemical tests: Glucose markedly diminished and may even absent in CSF while CSF protein is markedly raised C. Immunological methods: • Supernatant is tested for detection of soluble polysachharide antigen of N. meningitidis by counter immunoelectrophoresis or by agglutination of the latex particle coated with specific antibodies • This test is particularly useful at a later stage of disease when organism are scanty or absent due to therapy

Culture: a. CSF: – inoculated into CA and incubated at 35 -370 C in 5 -10% C 02 and high humidity – Colonies are tested by biochemical and agglutination reactions – Direct slide agglutination of isolated organism may be done with specific antisera B. Blood: – blood culture is positive over 40% cases of meningococcal meningitis – Blood culture s are incubated upto 7 days, with daily subculture c. Nasopharyngeal swab – To detect carrier d. Other cultures : joint fluid, tracheal aspirate or urethral discharge by gram stain and culture depending on patient’s symptoms

Detection of Antigens • Meningococcal antigens in blood and CSF can be found in active disease by PCR (detection of meningococcal DNA) • Capsular polysachharide by CIE and latex agglutination test Serogrouping Helps in epidemiological study
Vaccination: • Contains group- specific capsular polysachharide • Meningococcal polysaccharide vaccines are available in either bivalent (groups A and C), trivalent (groups A, C and W), or tetravalent (groups A, C, Y and W) forms to control the disease • Conjugate vaccine constituted by different serogrops and diptheria toxoid

Thank you
- Slides: 17