ECZEMA conti Seborrhoeic eczema Cause Infection of Pityrosporium

ECZEMA conti……. .
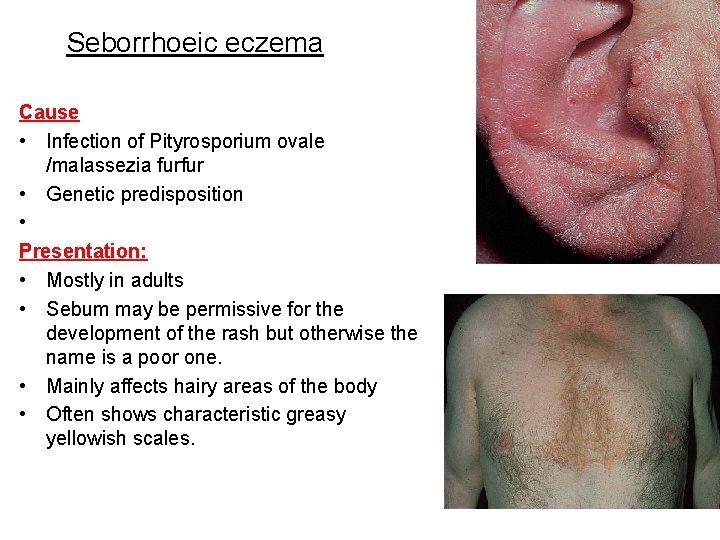
Seborrhoeic eczema Cause • Infection of Pityrosporium ovale /malassezia furfur • Genetic predisposition • Presentation: • Mostly in adults • Sebum may be permissive for the development of the rash but otherwise the name is a poor one. • Mainly affects hairy areas of the body • Often shows characteristic greasy yellowish scales.

Sites : Red scaly/ exudative eruption of the scalp(dandruff in milder form), ears, face, eye lashes and eyebrows. (in severe form resembles psoriasis) Seborrhoeic eczema is a feature of AIDS and can be very severe in this condition. Dry and scaly lesions of presternal and interscapular region and Intertrigenous lesions of armpits, umbilicus and groins or under spectacles and hearing aids Morphology Follicular variant(red follicular papule covered with greasy yellow scales) Eczematous(erythematous scaly, over hairline of scalp, associated with blepharitis and otitis externa) Petaloid(nonexudative annular scaly ) Seborrheic folliculitis(extensive erythematous follicular papules) Flexural (well defined erythema with greasy scales)

• Complications: Invest. bacterial infn candid inf. Rule out HIV Treatment Suppressive treatment rather than curative Topical imidazoles Topical corticosteroids Others: topical agents like 2%sulfur, 2%salicylic acid in aqueous cream and selenium sulfide(1 -2%), lithium prepn systemic therapy: used in HIV induced extensive lesion, antibiotics and antifungul
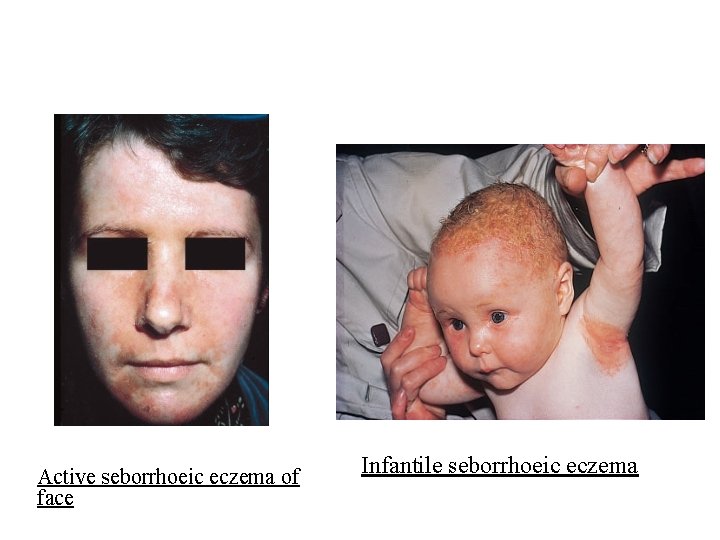
Active seborrhoeic eczema of face Infantile seborrhoeic eczema
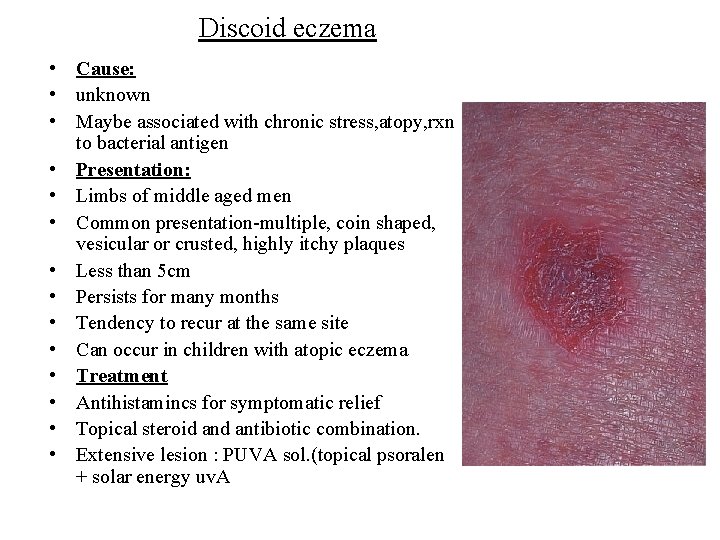
Discoid eczema • Cause: • unknown • Maybe associated with chronic stress, atopy, rxn to bacterial antigen • Presentation: • Limbs of middle aged men • Common presentation-multiple, coin shaped, vesicular or crusted, highly itchy plaques • Less than 5 cm • Persists for many months • Tendency to recur at the same site • Can occur in children with atopic eczema • Treatment • Antihistamincs for symptomatic relief • Topical steroid antibiotic combination. • Extensive lesion : PUVA sol. (topical psoralen + solar energy uv. A
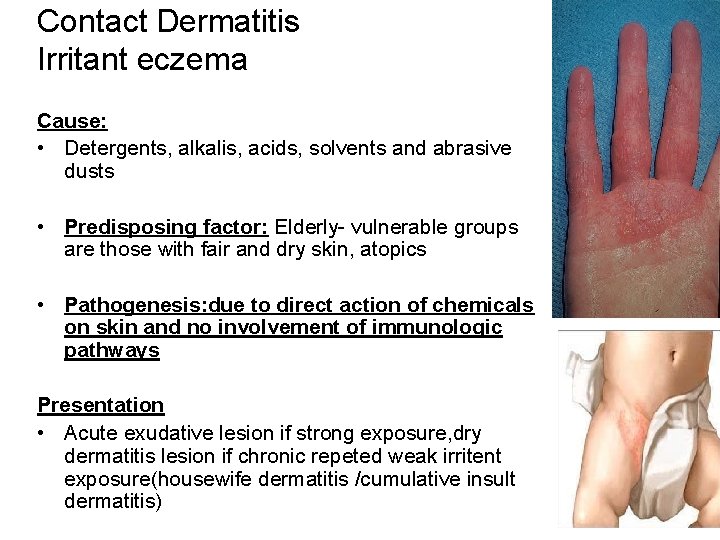
Contact Dermatitis Irritant eczema Cause: • Detergents, alkalis, acids, solvents and abrasive dusts • Predisposing factor: Elderly- vulnerable groups are those with fair and dry skin, atopics • Pathogenesis: due to direct action of chemicals on skin and no involvement of immunologic pathways Presentation • Acute exudative lesion if strong exposure, dry dermatitis lesion if chronic repeted weak irritent exposure(housewife dermatitis /cumulative insult dermatitis)

Children- napkin rashes Prolonged contact of skin with fecal enzymes and ammonia produced by urea-splitting bacteria Overgrowth of yeast Must be differentiated from allergic CD by patch test. Complication: Candida superinfection Treatment Clean the area Avoit irritant exposure Napkin area should be cleaned thoroughly and protective ointments like –Zn and castor oil ointment are useful Topical imidazoles to arrest the growth of yeast Acute cases -moderately potent corticosteroid hasten recovery Chronic –topical steroids , emollients
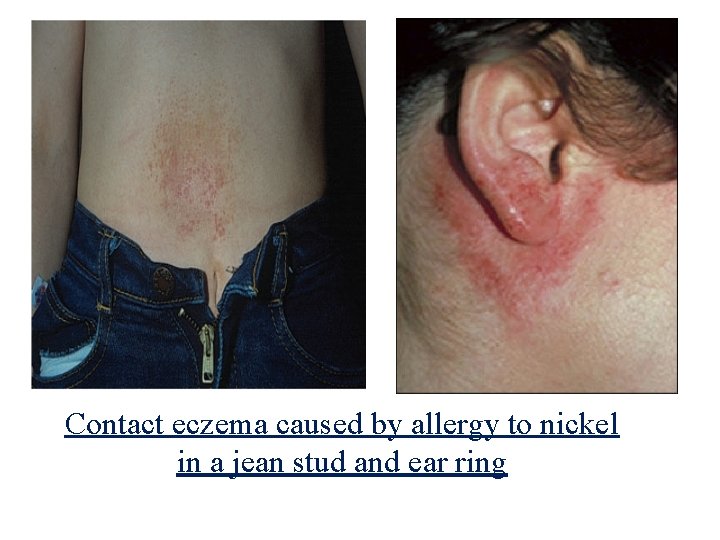
Contact eczema caused by allergy to nickel in a jean stud and ear ring
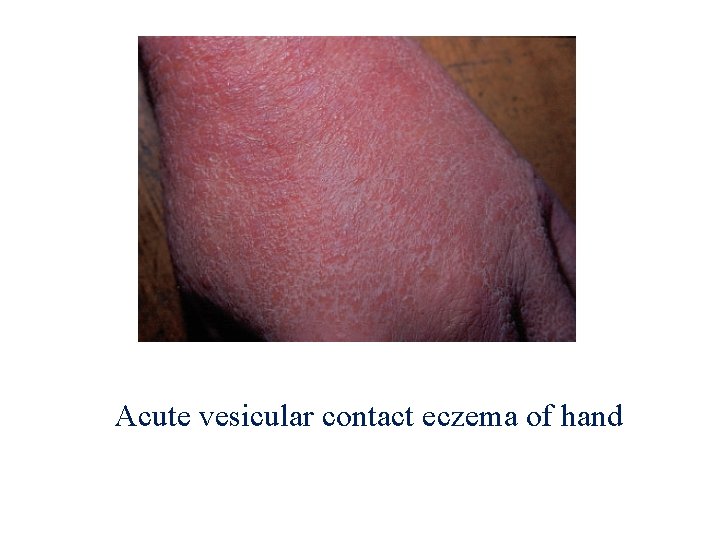
Acute vesicular contact eczema of hand
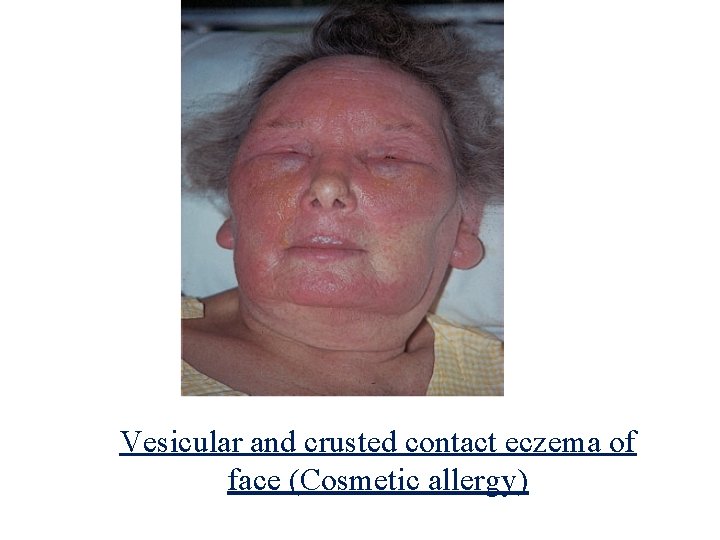
Vesicular and crusted contact eczema of face (Cosmetic allergy)
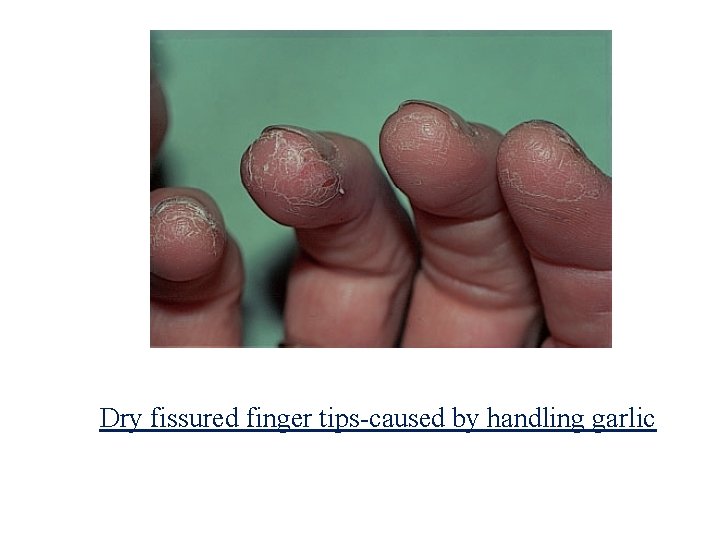
Dry fissured finger tips-caused by handling garlic

Allergic contact dermatitis Etiopathogenesis • • Exposure to allergens/ antigens in single or repeted contact Type IV/ delayed hypersensitivity Specific to one chemical or closely related chemicals All sites are allergic even though lesions manifest only over area of contact • Allergy is permanent
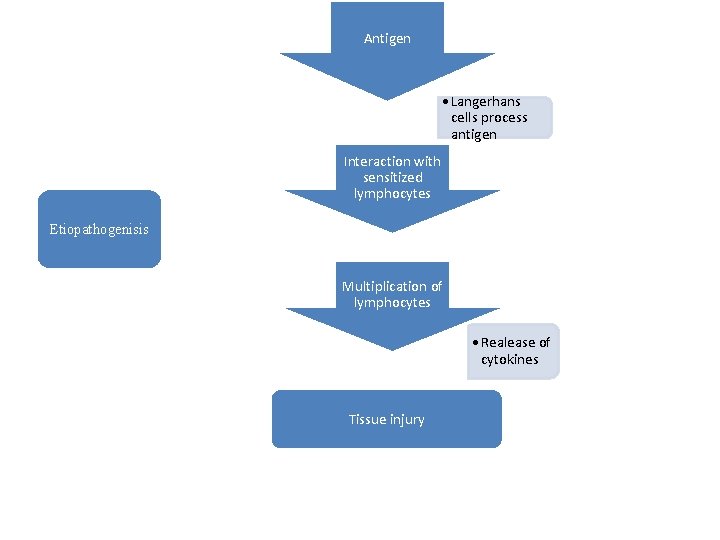
Antigen • Langerhans cells process antigen Interaction with sensitized lymphocytes Etiopathogenisis Multiplication of lymphocytes • Realease of cytokines Tissue injury
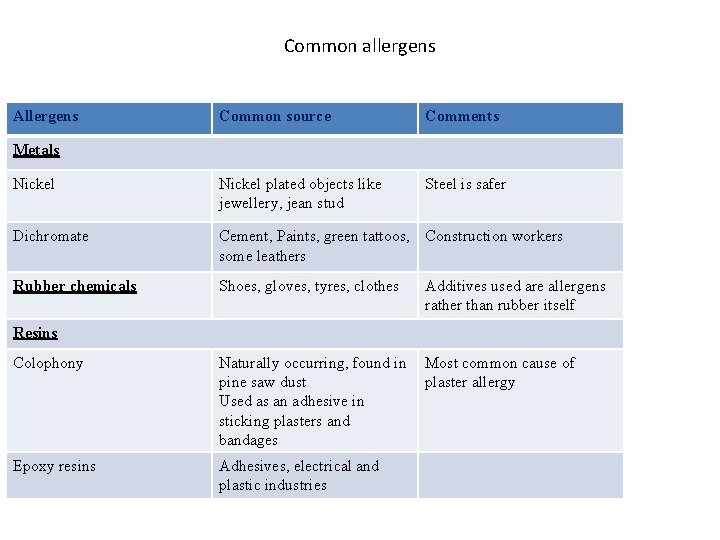
Common allergens Allergens Common source Comments Nickel plated objects like jewellery, jean stud Steel is safer Dichromate Cement, Paints, green tattoos, Construction workers some leathers Rubber chemicals Shoes, gloves, tyres, clothes Additives used are allergens rather than rubber itself Colophony Naturally occurring, found in pine saw dust Used as an adhesive in sticking plasters and bandages Most common cause of plaster allergy Epoxy resins Adhesives, electrical and plastic industries Metals Resins
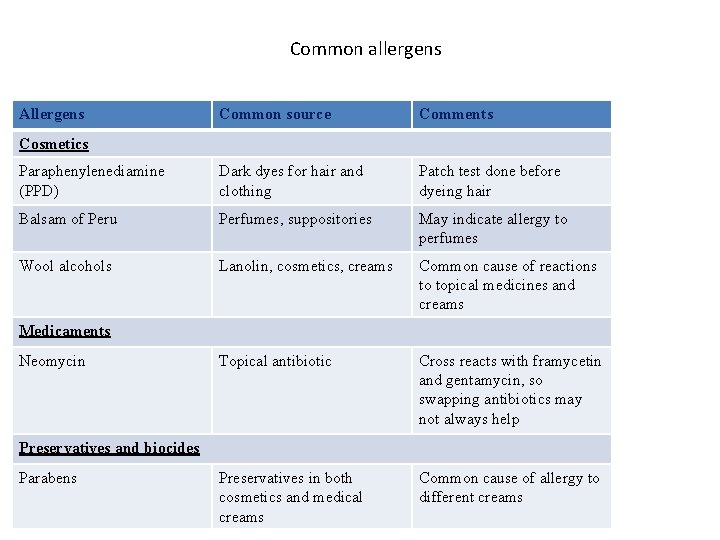
Common allergens Allergens Common source Comments Paraphenylenediamine (PPD) Dark dyes for hair and clothing Patch test done before dyeing hair Balsam of Peru Perfumes, suppositories May indicate allergy to perfumes Wool alcohols Lanolin, cosmetics, creams Common cause of reactions to topical medicines and creams Topical antibiotic Cross reacts with framycetin and gentamycin, so swapping antibiotics may not always help Preservatives in both cosmetics and medical creams Common cause of allergy to different creams Cosmetics Medicaments Neomycin Preservatives and biocides Parabens

Presentation Can manifest as acute or chronic Original site of eruption gives a clue to likely allergen Easily recognizable pattern Usually related to occupation Areas involved: Eyelids, external auditory meatus, hands / feet Investigations: find out allergen from hx and pattern of distribution patch test Treatment Avoid allergens completely Topical corticosteroids and if extensive, oral steroids
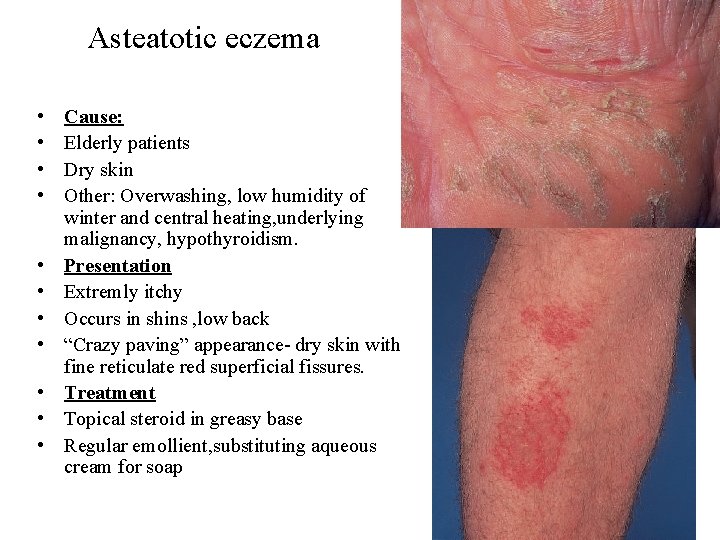
Asteatotic eczema • • • Cause: Elderly patients Dry skin Other: Overwashing, low humidity of winter and central heating, underlying malignancy, hypothyroidism. Presentation Extremly itchy Occurs in shins , low back “Crazy paving” appearance- dry skin with fine reticulate red superficial fissures. Treatment Topical steroid in greasy base Regular emollient, substituting aqueous cream for soap
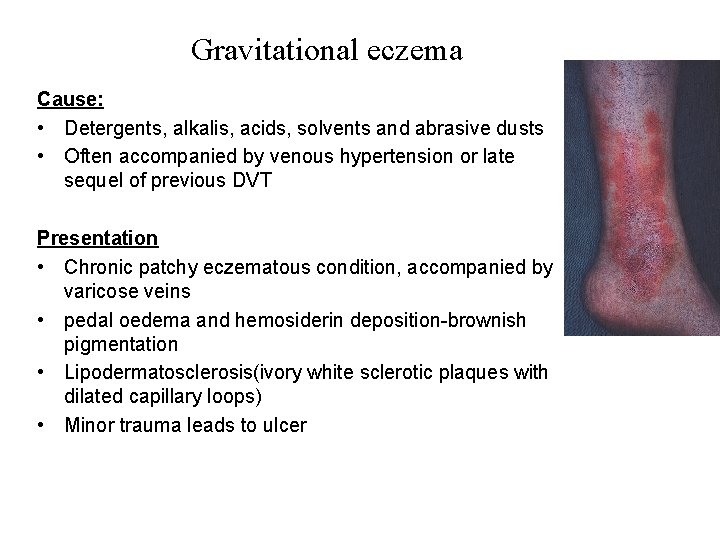
Gravitational eczema Cause: • Detergents, alkalis, acids, solvents and abrasive dusts • Often accompanied by venous hypertension or late sequel of previous DVT Presentation • Chronic patchy eczematous condition, accompanied by varicose veins • pedal oedema and hemosiderin deposition-brownish pigmentation • Lipodermatosclerosis(ivory white sclerotic plaques with dilated capillary loops) • Minor trauma leads to ulcer

• Occurs over lower third of the leg and ulcer over medial mallelus • Severe-spreads to other leg and may become generalized. Complications • Ulceration, infection, alllergic contact dermatitis to topical applications, deformity like inverted campagne bottle, malignancy (rare) Treatment • Elevation of affected limb/ pressure bandages • Mild steroids relieve irritation • Rx infection • Treatment of underlying cause

Lichen simplex/ localized neurodermatitis Cause: • Damage to the skin due to repeated scratching and rubbing and licking lips, usually as a habit or in response to stress , may be associated with atopy • Presentation • Single and sometime multiple, fixed itchy lichenified plaque • Common areas-nape of neck in female, legs in male, anogenital areas in both sexes. • Treatment • Topical steroid , keratolytic agents • antihistaminics • Helps break scratch-itch cycle
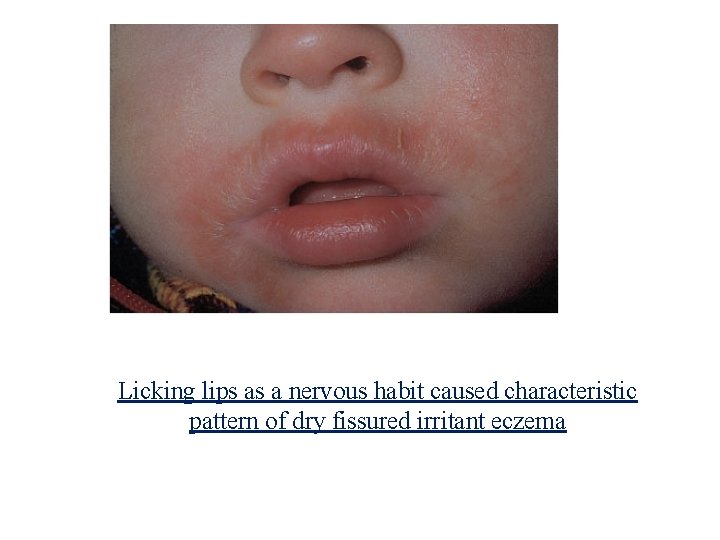
Licking lips as a nervous habit caused characteristic pattern of dry fissured irritant eczema
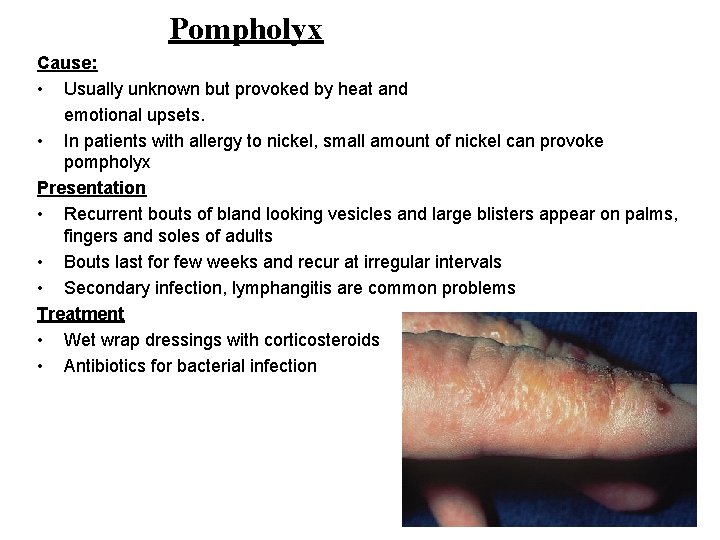
Pompholyx Cause: • Usually unknown but provoked by heat and emotional upsets. • In patients with allergy to nickel, small amount of nickel can provoke pompholyx Presentation • Recurrent bouts of bland looking vesicles and large blisters appear on palms, fingers and soles of adults • Bouts last for few weeks and recur at irregular intervals • Secondary infection, lymphangitis are common problems Treatment • Wet wrap dressings with corticosteroids • Antibiotics for bacterial infection

Topical Steroid Classification • • • • Group I is the strongest, or superpotent. Group VII is the weakest and mildest. Topical Steroid Group I Very potent - up to 600 times stronger than hydrocortisone. Betamethasone diproprionate, Halbetasol proprionate Topical Steroid Group II Fluocinonide, Halcinonide Topical Steroid Group III Triamcinolone acetonide, Fluticasone proprionate, Betamethasone diproprionate Topical Steroid Group IV Fluocinolone acetonide, Hydrocortisone Valerate Hydrocortisone butyrate Topical Steroid Group V Triamcinolone acetonide, Fluticasone propionate, Hydrocortisone valerate Topical Steroid Group VI Prednicarbate, Triamcinolone acetonide, Fluocinolone acetonide Topical Steroid Group VII The weakest class of topical steroids. Has poor lipid permeability, and can not penetrate mucous membranes well. Hydrocortisone 2. 5% , Hydrocortisone 1%

Common side effects of long term steroid use • • Thinning of skin- striae, fragility, purpura Vulnerable to infections Systemic absorption- Suppression of hypothalamic-adrenal axis Cushingoid features(centralized obesity, moon face, flushed cheek double chin, buffalo hump, hypertension, demineralization of bones and short stature)
- Slides: 25