Accreditation Council for Graduate Medical Education Nuclear Medicine
























- Slides: 32

Accreditation Council for Graduate Medical Education Nuclear Medicine Review Committee Update SNMMI Winter 2016 Jon Baldwin, DO Chair Review Committee for Nuclear Medicine

Disclosures • None

Session Overview • • • RC structure NM program stats Eligibility NAS Updates Milestones/CCC Questions

Current Committee Membership • • Jon Baldwin, DO (AMA) – Chair David Lewis, MD (AMA) – Vice Chair Helena Balon, MD (SNM) Frederick Grant, MD (SNM) Barry Shulkin, MD (ABNM) Kirk Frey, MD (ABNM) Mary Beth Farrell, MS (Public) Adonteng Kwakye, MD(Resident)

RC Meetings • 2 meetings per year • Check RC website for agenda closing dates & meeting dates • Upcoming: April 8, 2016 (agenda closing date: March 7, 2016) • Meeting Length: 1 – 1 ½ days • Program reviews & other Review Committee business

Nuclear Medicine 2015 -2016 • 43 accredited programs • 84/157 (54%) filled vs approved resident positions

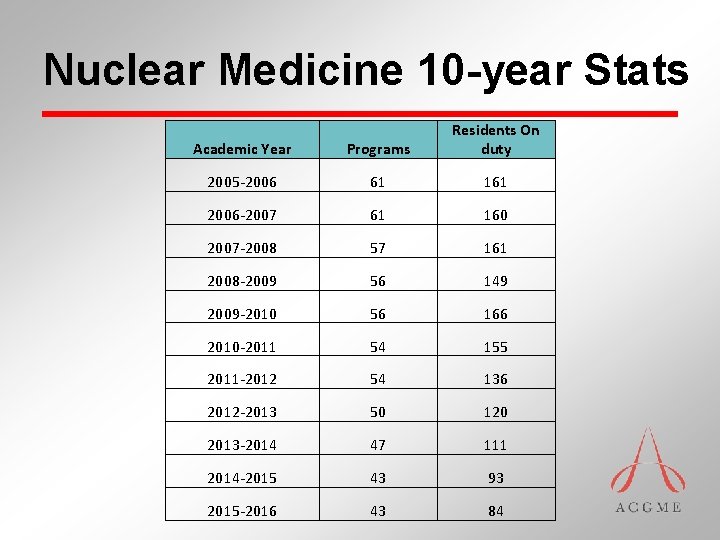
Nuclear Medicine 10 -year Stats Academic Year Programs Residents On duty 2005 -2006 61 161 2006 -2007 61 160 2007 -2008 57 161 2008 -2009 56 149 2009 -2010 56 166 2010 -2011 54 155 2011 -2012 54 136 2012 -2013 50 120 2013 -2014 47 111 2014 -2015 43 93 2015 -2016 43 84

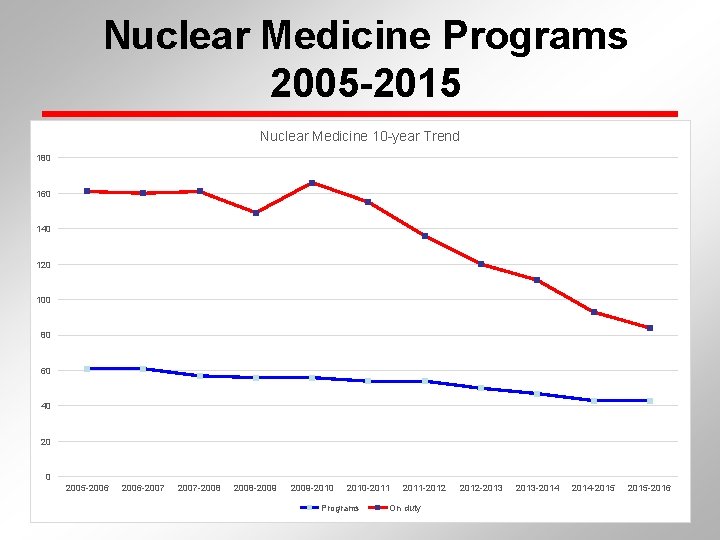
Nuclear Medicine Programs 2005 -2015 Nuclear Medicine 10 -year Trend 180 160 140 120 100 80 60 40 2005 -2006 -2007 -2008 -2009 -2010 -2011 Programs 2011 -2012 On duty 2012 -2013 -2014 -2015 -2016

Eligibility

2016 NM Eligibility FAQ • As AOA-approved programs transition to ACGME accreditation, are there any considerations for nuclear medicine programs considering applicants who have previously completed AOA-approved training? • [Program Requirement: III. A. 1. c)]

2016 NM Eligibility FAQ • Answer: The Review Committee understands that during the transition to a single accreditation system, nuclear medicine programs may wish to consider NM 1 applicants who have completed one year of graduate medical education in an AOA-approved program. Nuclear medicine programs will not jeopardize their accreditation status if they accept these individuals. All programs should check with the American Board of Nuclear Medicine (ABNM) and/or the American Osteopathic Board of Nuclear Medicine (AOBNM) regarding certification eligibility.

NAS Review Discussions

NAS Summary 40% programs Compliant, no feedback 37% programs Minor issues in 1 -2 areas, feedback in the form of AFIs 20% programs Concerns, feedback either as citations and/or AFIs 3% programs Site visits requested for more information Area for Improvement (AFI) • • Areas noted by the Committee for program improvement before it gets worse, “Heads Up” Does not require program response Citations • • Areas of non-compliance with the requirements Requires full program response for Committee review

NAS Most Common Flagged Items • Clinical Experience (Case Logs) • Many data entry discrepancies still occurring • Board Pass Rate • Reminder that the new pass rate is 75% for first time takers for 5 yr period • Pgms below 75% can anticipate feedback from the Review Committee • Resident Survey • Flagged programs with less than 4 residents can anticipate feedback on the multi-year aggregate survey results.

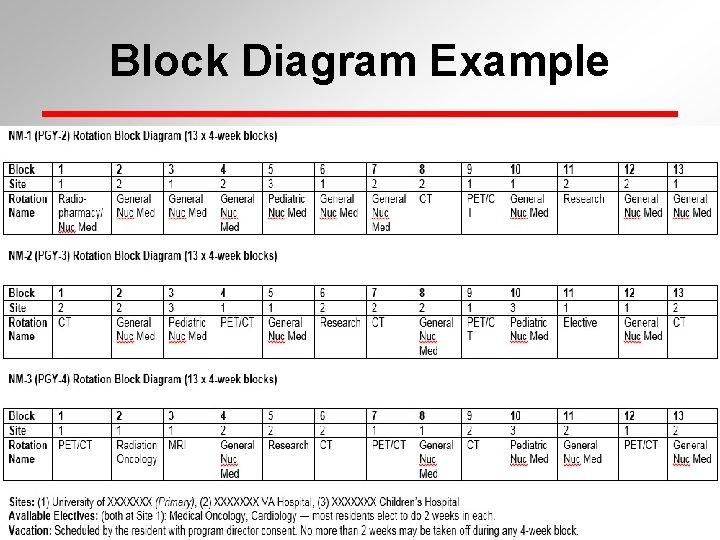
Block Diagram in ADS • Many programs providing inadequate block diagrams • Not representative of a 3 -year curriculum • NM is a three-year specialty. This should be reflected on the block diagram. • Even programs with recruiting practices that only consider NM 2 or NM 3 residents

Block Diagram in ADS • Block diagram should be free of individual resident names or identifiers • If abbreviations are used for rotations or site names, a Key must be provided • Block diagram guide posted on Committee’s webpage


Block Diagram Example

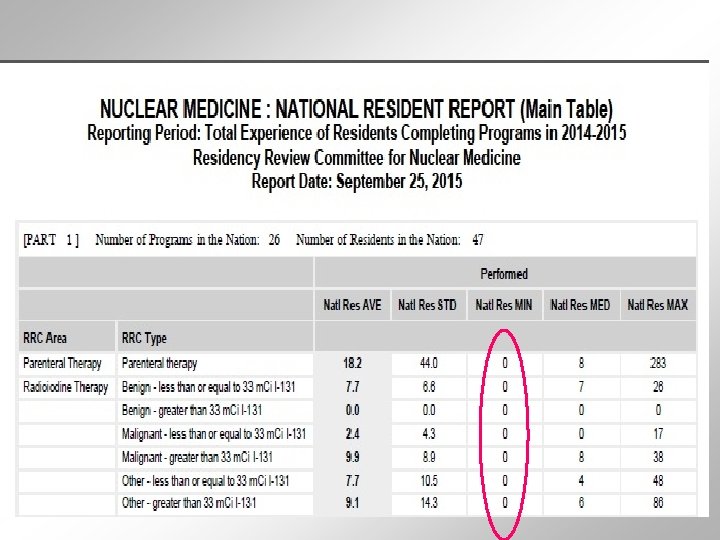
Clinical Experience - Case Logs • All programs are required to use the ACGME Case Log System • Residents must enter all specified procedures performed during their residency education into the ACGME case log system regardless of stated minimums. • Inaccurate data will impede the Committee’s ability to set accurate and realistic future benchmarks for the specialty.

Clinical Experience - Case Logs • Among the graduates of 2015, the minimum number of procedures reported for all procedural categories was “ 0” • The highest procedural category reported was for parenteral therapies at 283


Omission of Data • 5% of programs flagged for not providing data • Faculty Scholarly Activity • No Core Faculty designation • Program Director: • • Must provide complete and accurate information (II. A. 4. h). (1) Review all information before “hitting” the submit button

Milestones

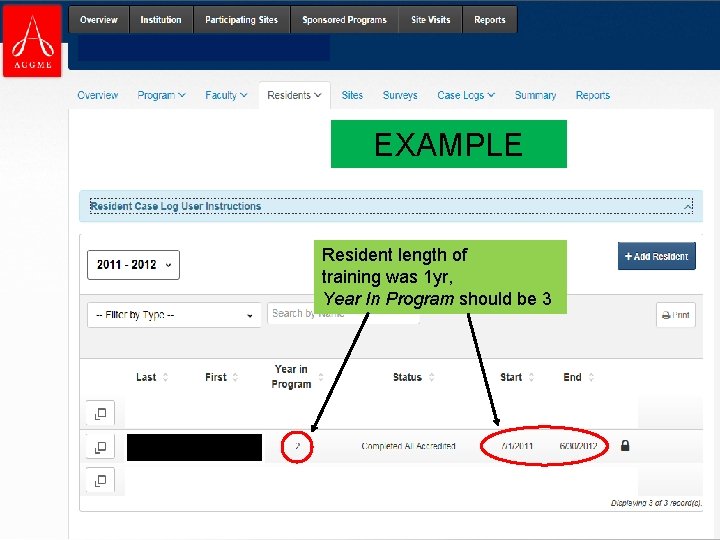
NM Milestones Reporting • Data appears skewed for resident competency progression • Most likely linked to inaccurate resident reporting in ADS • Several residents reported in ADS with inaccurate “Year in Program” compared to their NM year

NM Year Consideration < 12 months of training remaining = NM 3 (or year in program 3) Between 24 and 12 months of training remaining = NM 2 (or year in program 2) Between 36 and 24 months of training remaining = NM 1 (or year in program 1)

EXAMPLE Resident length of training was 1 yr, Year In Program should be 3

Milestones • Milestones designed to help residencies/fellowships produce highly competent physicians to meet the health and healthcare needs of the public • Guide curriculum development • Provide developmental framework for Clinical Competency Committee (CCC) • Residents do not have to achieve level 4 to graduate from the program • The determination of an individual’s readiness for graduation is at the discretion of the program director

Milestones/ Clinical Competency Committee • CCC should help analyze and synthesize resident assessments • Using milestones, CCC should reach consensus judgement regarding resident performance • CCC provides conclusions to program director • Program director has ultimate authority to determine residents’ milestone developmental level at least twice yearly Journal of Graduate Medical Education, September 2015

Clinical Competency Committee • For CCC composition, programs should consider including a physicist or other faculty member who assesses NRC/AU requirements • A Clinical Competency Committee (CCC) Guidebook is posted on the Milestones webpage


ACGME Staff Contact List Executive Director Felicia Davis, MHA 312 -755 -5006 fdavis@acgme. org Associate Executive Director Kate Hatlak, MSEd 312 -755 -7416 khatlak@acgme. org Senior Accreditation Administrator Sara Thomas 312 -755 -5044 sthomas@acgme. org Case Log questions oplog@acgme. org

Questions? Thank you