The Red Eye for primary healthcare providers DR















- Slides: 35

The Red Eye for primary healthcare providers DR CHIN PIK KEE FRCS Ophthal (Edinburgh), M. Med Ophthal (S’pore) Sunway Medical Centre Primary Eye Care Paramedic Workshop, MSJOC 2016; 4 March 2016, Kuching, Sarawak

CAUSES From the harmless to the very serious Infectious • Bacteria, virus, fungus – Conjunctivitis – Keratitis – Uveitis – Retinitis – Choroiditis – Endophthalmitis – Panopthalmitis – Orbital cellulitis Non-infectious • • • Allergy Contact lens wear Glaucoma (some types) Non-infective uveitis Trauma Subconjunctival haemorrhage Growths (e. g. , pterygium) Tumours Carotid-cavernous fistula

HISTORY – Key Points • Any pain? – Superficial foreign body sensation or deep – headache/vomiting, severe enough to disturb sleep • Any discharge? – purulent, watery, or mucoid • Any itch? – allergy • Is vision affected or normal? • Any – contact with red eye? – contact lens wear? – trauma?

EXAMINATION – Key Points • Distribution of conjunctival hyperaemia – Generalised or focal, peripheral or circumcorneal • Any discharge? – purulent, watery or mucoid • Is the cornea clear? • Pupil size and reaction to light • Anterior chamber • Deep or shallow? • Any hypopyon or hyphaema? • Are the eye movements full?

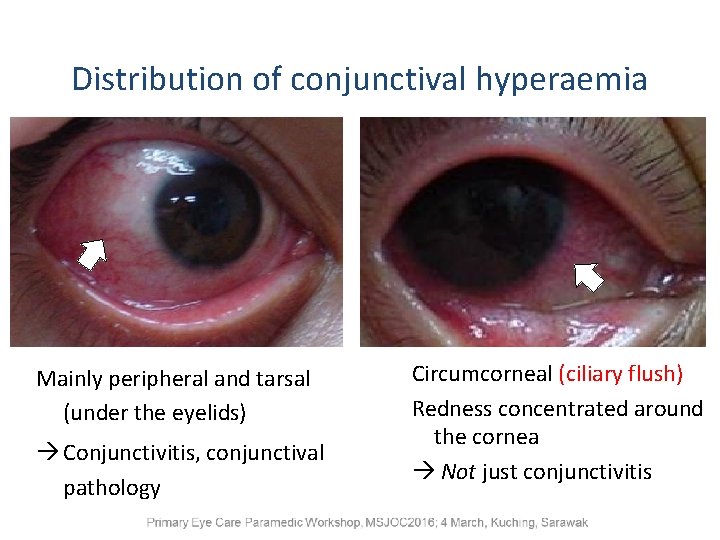
Distribution of conjunctival hyperaemia Mainly peripheral and tarsal (under the eyelids) Conjunctivitis, conjunctival pathology Circumcorneal (ciliary flush) Redness concentrated around the cornea Not just conjunctivitis

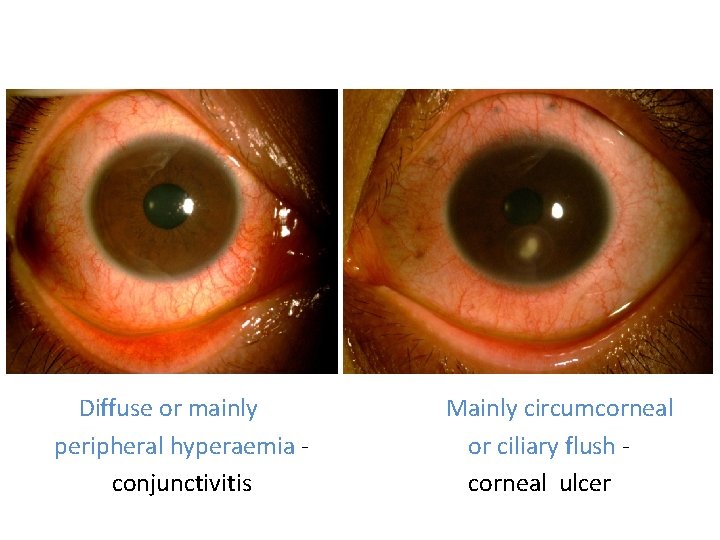
1 Diffuse or mainly peripheral hyperaemia conjunctivitis Mainly circumcorneal or ciliary flush corneal ulcer

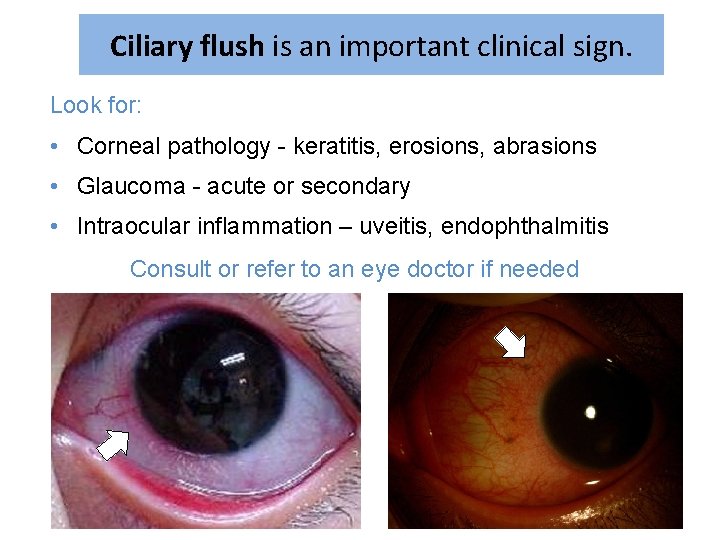
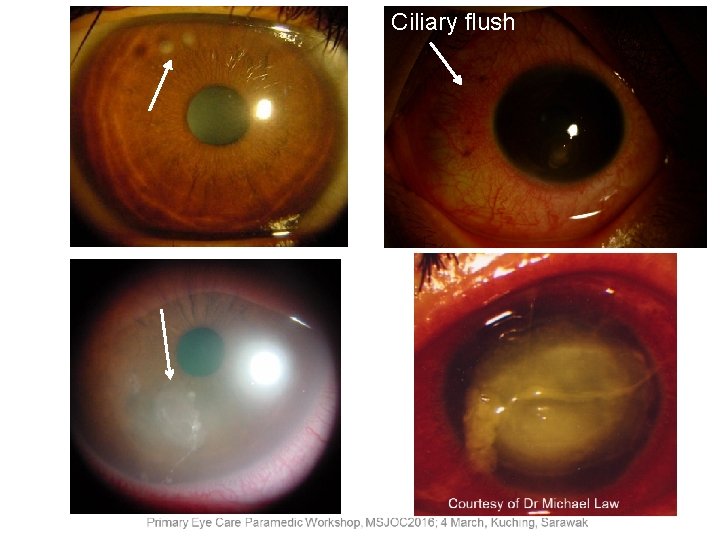
Ciliary flush is an important clinical sign. Look for: • Corneal pathology - keratitis, erosions, abrasions • Glaucoma - acute or secondary • Intraocular inflammation – uveitis, endophthalmitis Consult or refer to an eye doctor if needed

Common Causes of Red Eye • • Acute conjunctivitis – Bacterial, viral Keratitis – Dendritic ulcer – Corneal ulcer Allergic conjunctivitis Acute iritis (uveitis) Subconjunctival haemorrhage Contact lens wear Acute angle-closure glaucoma

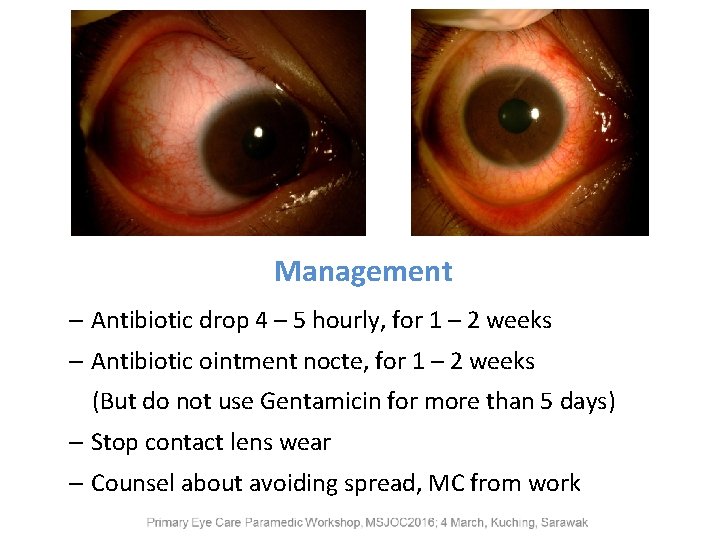
Acute Conjunctivitis • Commonly bacterial or viral • Symptoms • Red eye (one or both), irritation, burning, discharge • Signs – Eyelid redness, swelling – Conjunctival hyperaemia (generalised or peripheral) – Eye discharge • Purulent (usually bacterial) • Watery (viral) • Mild to severe • Uncomplicated or complicated

Management – Antibiotic drop 4 – 5 hourly, for 1 – 2 weeks – Antibiotic ointment nocte, for 1 – 2 weeks (But do not use Gentamicin for more than 5 days) – Stop contact lens wear – Counsel about avoiding spread, MC from work

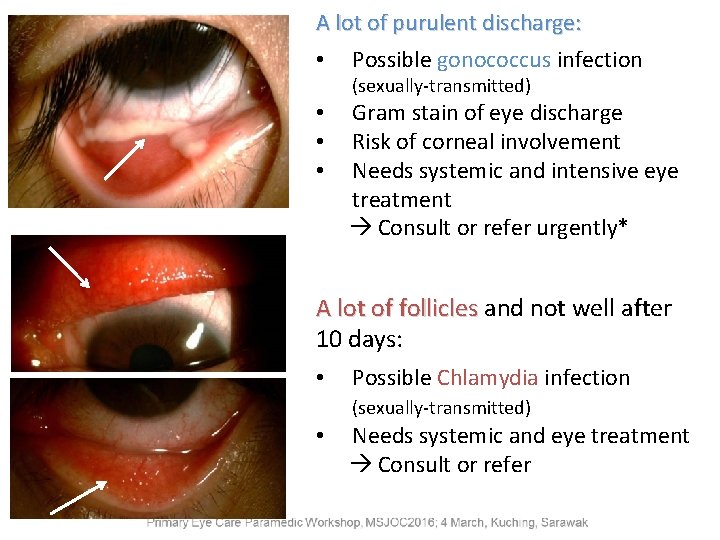
A lot of purulent discharge: • Possible gonococcus infection (sexually-transmitted) • • • Gram stain of eye discharge Risk of corneal involvement Needs systemic and intensive eye treatment Consult or refer urgently* A lot of follicles and not well after 10 days: • Possible Chlamydia infection (sexually-transmitted) • Needs systemic and eye treatment Consult or refer

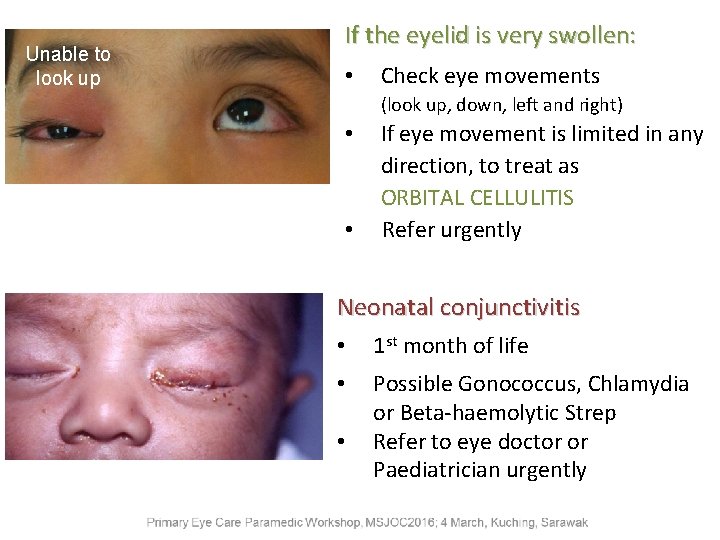
Unable to look up If the eyelid is very swollen: • Check eye movements (look up, down, left and right) • • If eye movement is limited in any direction, to treat as ORBITAL CELLULITIS Refer urgently Neonatal conjunctivitis • 1 st month of life • Possible Gonococcus, Chlamydia or Beta-haemolytic Strep Refer to eye doctor or Paediatrician urgently •

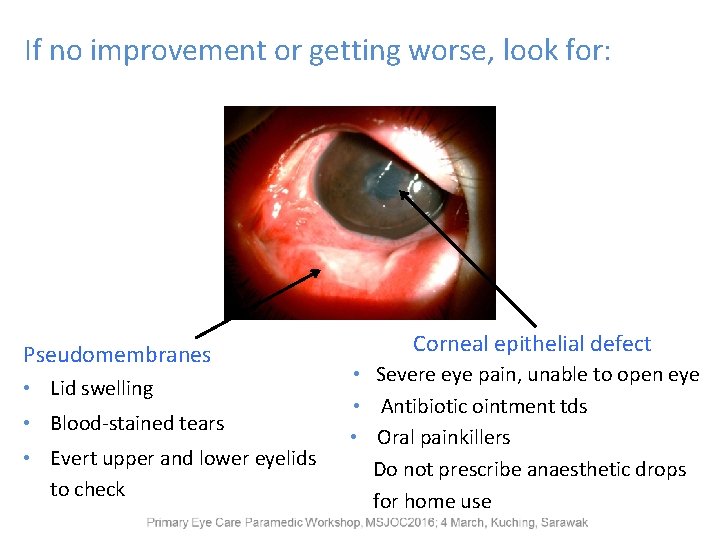
If no improvement or getting worse, look for: Pseudomembranes • Lid swelling • Blood-stained tears • Evert upper and lower eyelids to check Corneal epithelial defect • Severe eye pain, unable to open eye • Antibiotic ointment tds • Oral painkillers Do not prescribe anaesthetic drops for home use

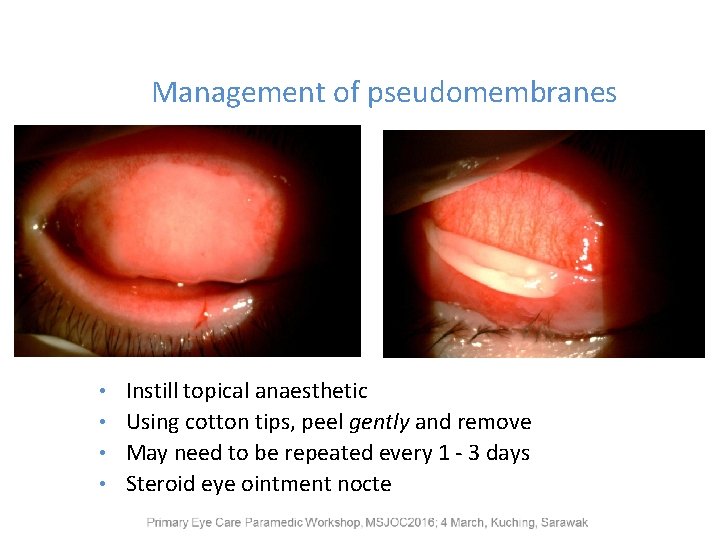
Management of pseudomembranes Instill topical anaesthetic • Using cotton tips, peel gently and remove • May need to be repeated every 1 - 3 days • Steroid eye ointment nocte •

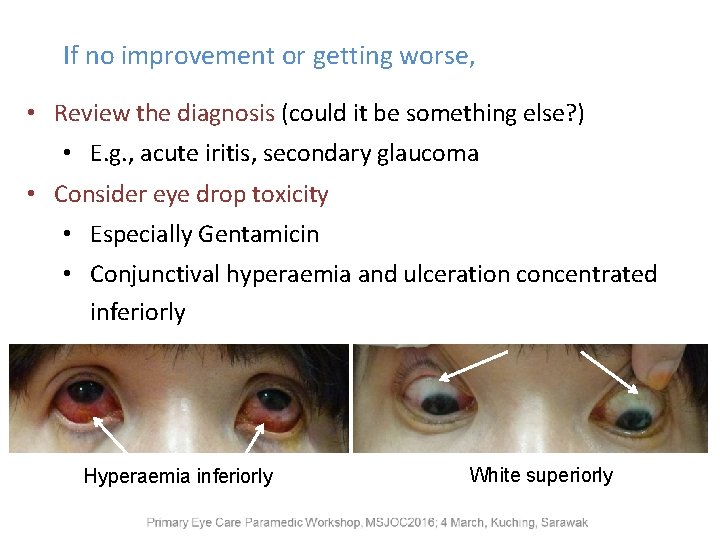
If no improvement or getting worse, • Review the diagnosis (could it be something else? ) • E. g. , acute iritis, secondary glaucoma • Consider eye drop toxicity • Especially Gentamicin • Conjunctival hyperaemia and ulceration concentrated inferiorly Hyperaemia inferiorly White superiorly

Keratitis - Dendritic Ulcer • Herpes simplex keratitis • Symptoms: may be mild – Redness, irritation, photophobia, watering, blurred vision • Signs: – Conjunctival congestion – Ulcer is usually seen only with fluorescein staining

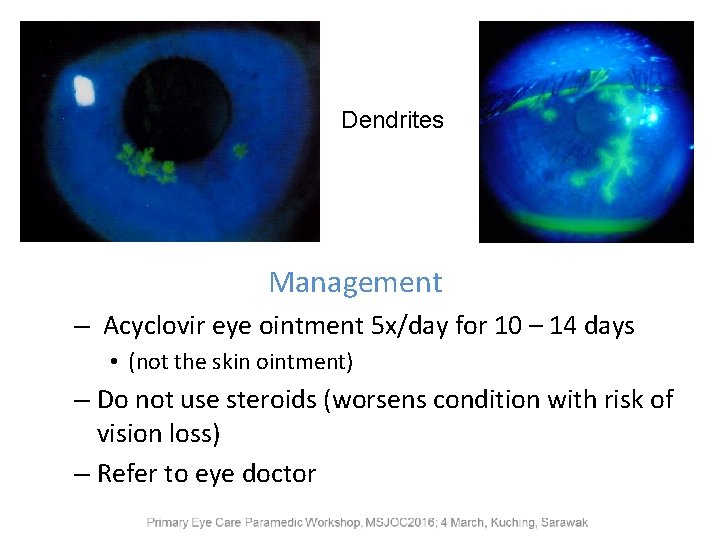
Dendrites Management – Acyclovir eye ointment 5 x/day for 10 – 14 days • (not the skin ointment) – Do not use steroids (worsens condition with risk of vision loss) – Refer to eye doctor

Keratitis - Corneal Ulcer • Corneal infection by bacteria (common), fungus or protozoa, virus (less common) • Risk factors – Trauma – Contact lens wear • Clinical features – Red eye, pain, tearing, photophobia, eyelid swelling – Corneal opacity, stains with fluorescein

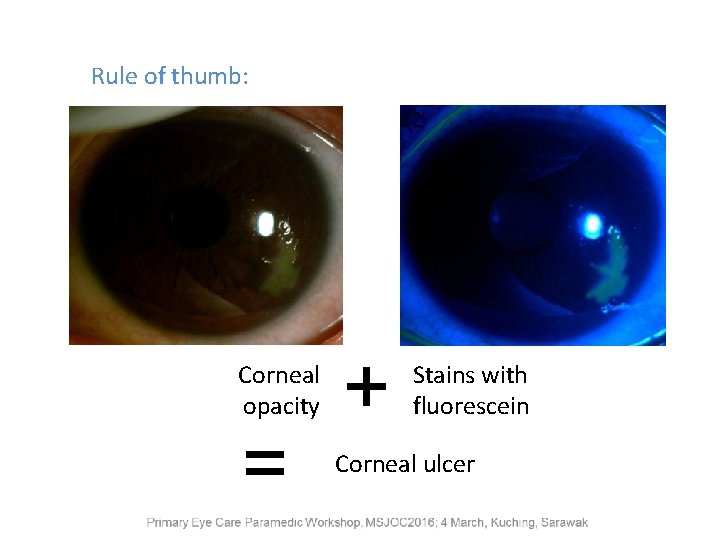
Rule of thumb: Corneal opacity = + Stains with fluorescein Corneal ulcer

Ciliary flush Courtesy of Dr Michael Law

Management • Refer immediately – If >12 hours delay, start antibiotics first – E. g. , gt Tobramycin, Ciprofloxacin, Vigamox, Gentamicin, or Chloramphenicol (Do not use steroids) • Principles – Corneal scraping and culture – Intensive antimicrobial therapy around the clock (hospital admission if necessary) • Complications – Corneal perforation, endophthalmitis, panophthalmitis – Loss of vision, loss of eye

Allergic Conjunctivitis Cause • Environmental allergens – Dust mites, animal dander, plant pollen – Contact allergens Symptoms • Redness, watering • Itch and rubbing Signs • Conjunctival redness, chemosis • Mild lid swelling, papillary reaction Chemosis

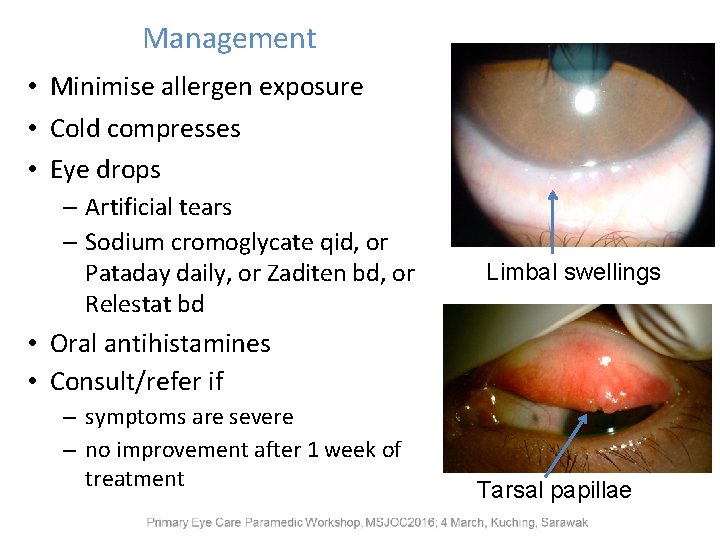
Management • Minimise allergen exposure • Cold compresses • Eye drops – Artificial tears – Sodium cromoglycate qid, or Pataday daily, or Zaditen bd, or Relestat bd Limbal swellings • Oral antihistamines • Consult/refer if – symptoms are severe – no improvement after 1 week of treatment Tarsal papillae

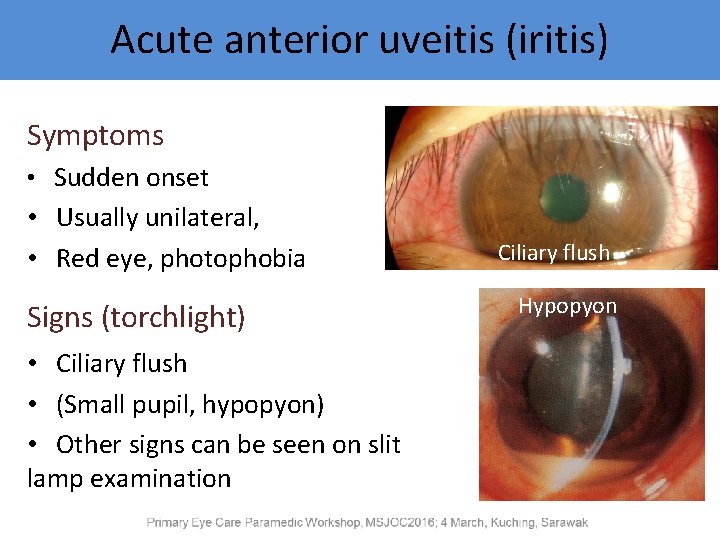
Acute anterior uveitis (iritis) Symptoms • Sudden onset • Usually unilateral, • Red eye, photophobia Signs (torchlight) • Ciliary flush • (Small pupil, hypopyon) • Other signs can be seen on slit lamp examination Ciliary flush Hypopyon

• Management – Referral to eye doctor – Principles • Dilating / cycloplegic eye drops • Steroids • May need investigations in some cases If a patient with red eye does not improve after 1 week of treatment for “conjunctivitis” and has no pseudomembranes, consider possible iritis.

Subconjunctival haemorrhage Bleeding under the conjunctiva Causes – Spontaneous, trauma, conjunctivitis – Risk factors include hypertension, blood thinning medications Management – Ask about bleeding tendency • If present; check full blood counts, refer to doctor – Check blood pressure – Self-limiting, no medications needed

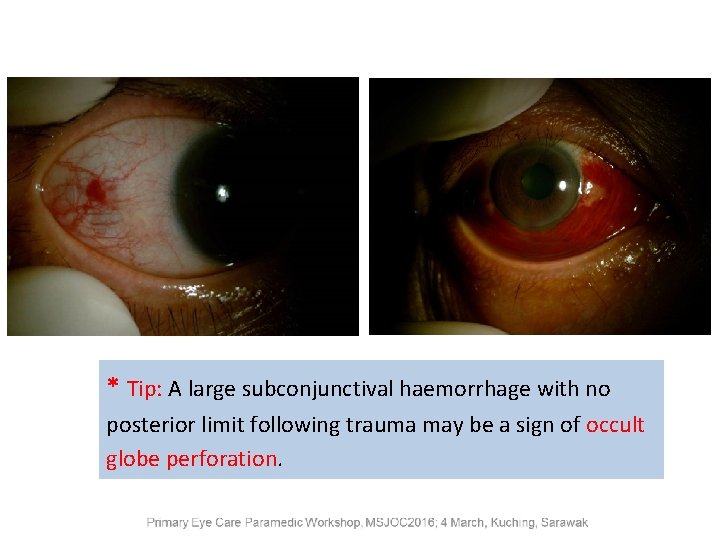
* Tip: A large subconjunctival haemorrhage with no posterior limit following trauma may be a sign of occult globe perforation.

Contact Lens Wear Complications – Poor oxygen transmission to cornea – Mechanical trauma – Allergic reaction – Infection Problems are usually related to: – Chronic wear, long wearing hours – Poor care and cleaning routine – Sleeping with lenses on – Exposure to contaminated water

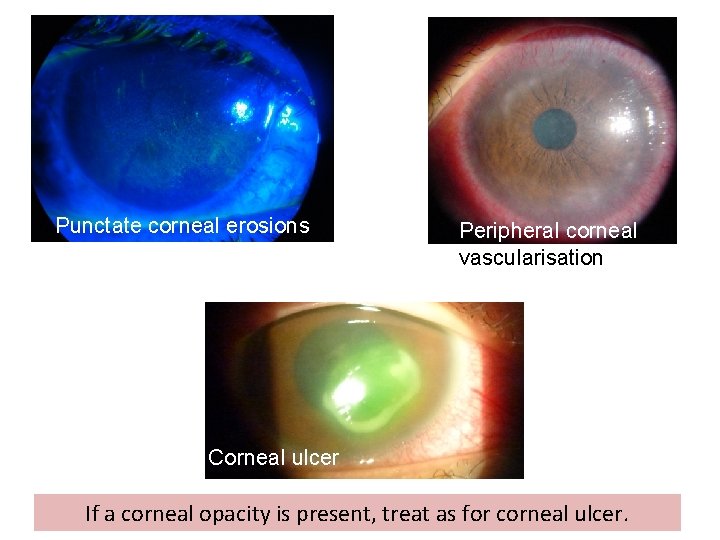
Punctate corneal erosions Peripheral corneal vascularisation Corneal ulcer If a corneal opacity is present, treat as for corneal ulcer.

Symptoms – Eye redness and itch – Unable to tolerate contact lens wear – Blurring of vision Management – Stop contact lens wear (temporary or permanent) – Change contact lens type , reduce wearing time – Eye drops: • artificial tears • non-steroidal drops for allergy In case of uncertainty, the safer course is to treat as for infection using antibiotic drops. *Avoid steroids.

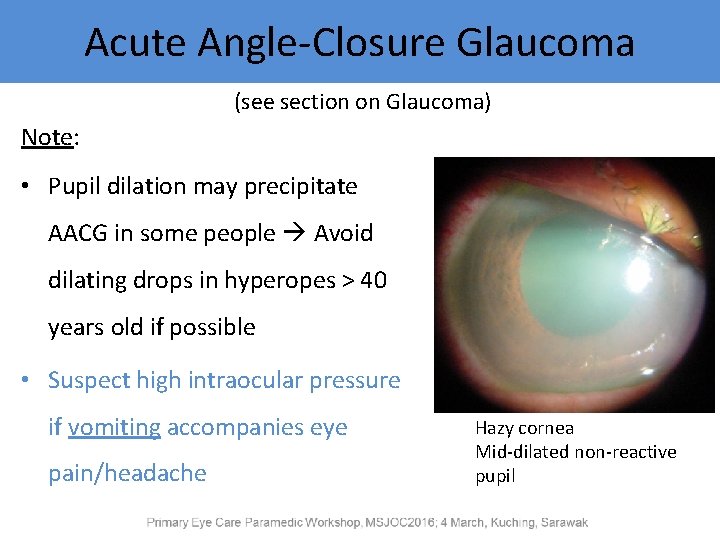
Acute Angle-Closure Glaucoma (see section on Glaucoma) Note: • Pupil dilation may precipitate AACG in some people Avoid dilating drops in hyperopes > 40 years old if possible • Suspect high intraocular pressure if vomiting accompanies eye pain/headache Hazy cornea Mid-dilated non-reactive pupil

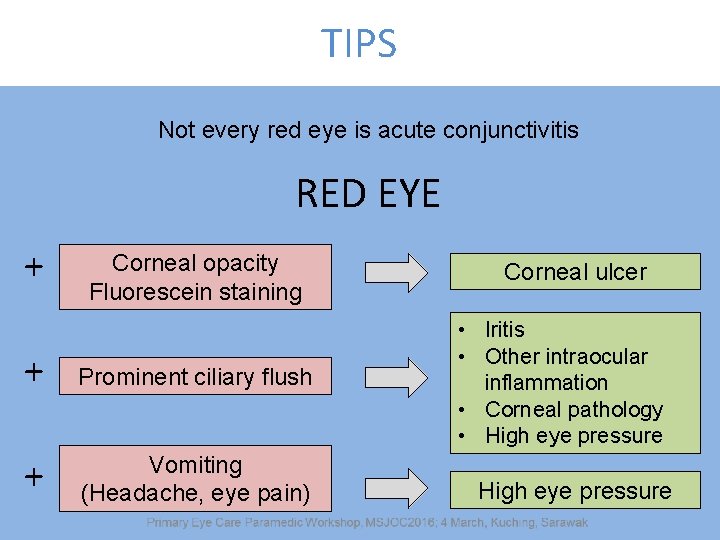
TIPS Not every red eye is acute conjunctivitis RED EYE + Corneal opacity Fluorescein staining + Prominent ciliary flush + Vomiting (Headache, eye pain) Corneal ulcer • Iritis • Other intraocular inflammation • Corneal pathology • High eye pressure

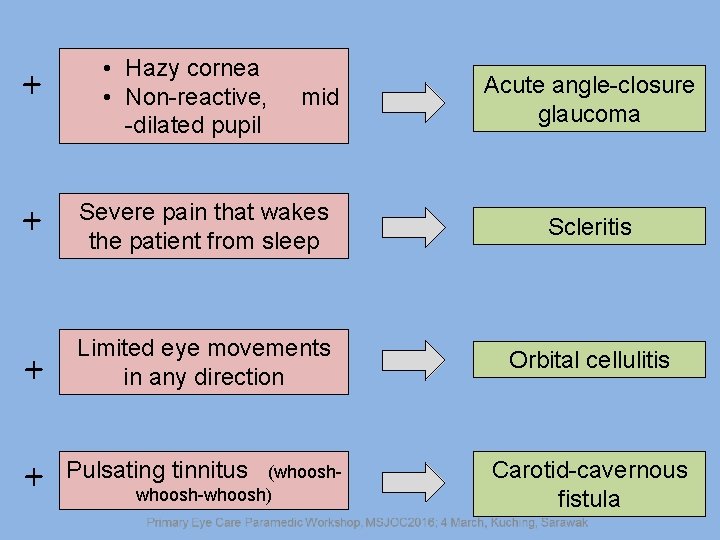
+ • Hazy cornea • Non-reactive, -dilated pupil mid Acute angle-closure glaucoma + Severe pain that wakes the patient from sleep Scleritis + Limited eye movements in any direction Orbital cellulitis + Pulsating tinnitus (whoosh-whoosh) Carotid-cavernous fistula

Topical Steroids Steroid eye drops can cause: • • Worsening of corneal ulcers Reactivation of herpetic keratitis Glaucoma Cataract Antibiotic only Recognising a steroid: • Check composition for “…. . one” • E. g. , dexamethasone, betamethasone, prednisolone, fluoromethalone • Beware of combination drops, especially look-alike, sound-alike drops Steroid eye drops should only be prescribed by an eye doctor and used under supervision. Antibiotic + steroid

Thank you