STD AND RTI SYPHILIS Syphilis is a sexually

































- Slides: 34

STD AND RTI


SYPHILIS �Syphilis is a sexually transmitted disease caused by the spirochete bacterium Treponema pallidum

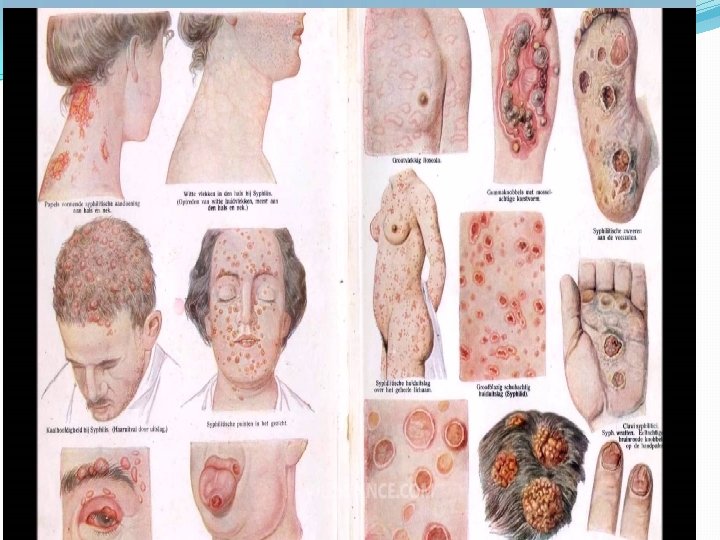
CLINICAL FEATURES q PRIMARY STAGE Ø Small red spot is noticed on the penis 3 – 4 weeks after sexual intercourse Ø Painless develop to a well defined hard sore or hard chancre Ø A painless bubo in the groin Ø Glands in neck, axilla and epitrochlear region q SECONDARY STAGE Ø Sore throat, anemia, skin rashes, enlargement of glands Ø Pain and swelling in bones and joints Ø Soft warty condylomata are seen on the moist surface Ø Ulcer in throat Ø White mucous patch inside the cheeks

CAUSATIVE AGENT �TREPONEMA PALLIDUM �Dies rapidly outside the body �It is killed by drying, heating, ordinary antiseptics

SOURCE OF INFECTION �Saliva �Urine �Broken and ulcerating gum in throat �Skin may be infective

MODE OF TRANSMISSION � Sexual intercourse � Rarely by kissing � Saliva � Semen � Blood � Vaginal discharges � Congenital syphilis � Extragenital infection

PERIOD OF COMMUNICABILITY �As long as primary sore, condylomata, mucous patches or ulcerating gummata are not healed

SUSCEPTIBILITY AND RESISTANCE �Susceptibility in general �No natural immunity

INCUBATION PERIOD � 10 days to 10 weeks �Average 3 weeks

METHOD OF CONTROL…Contd q PREVENTIVE MEASURES Ø Congenital syphilis • Serological examination and treatment Ø Acquired syphilis • Health and sex education • Personal prophylaxis before, during and after exposure • Control of prostitution • Early diagnosis and treatment

METHOD OF CONTROL q. CONTROL OF PATIENTS, CONTACTS AND THE IMMEDIATE ENVIRONMENT Ø Report to health authority Ø Isolation Ø Contacts • Congenital syphilis ( All immediate family members) • Primary syphilis (sexual contact preceding 3 months) • Secondary syphilis (sexual contact preceding 6 months) Ø Specific treatment • Acquired syphilis (Benzathine penicillin G) • Congenital syphilis (Procaine penicillin ) • In case of pencillin allergy erythromycin or tetracycline is given

GONORRHOEA �Gonorrhea is a sexually transmitted disease caused by the bacteria Neisseria Gonorrhoeae or Gonococcus

CLINICAL FEATURES q MALE Ø Inflammation of urethra Ø Acute burning sensation with pain and pus discharge while passing urine Ø Infection spread to prostate, seminal vesicles, bladder, renal pelvis or rectum q FEMALE Ø Inflammation of urethra Ø Acute burning sensation with pain and pus discharge while passing urine Ø Infection spread to uterus, tubes, peritoneum and bartholin glands INFECTION MAY SPREAD THROUGH BLOOD TO HEART, MENINGES, JOINTS , MUSCLES, TENDONS AND EYE

COMPLICATIONS �Urethral stricture in males �PID in females �Infertility

DIAGNOSIS �It is a gram negative diplococci �Male urethral smear �Female smear from cervix and uterus �No reliable serological test are available

CAUSATIVE AGENT �Neisseria Gonorrhoeae �Kidney shaped diplococci

SOURCE OF INFECTIONPERIOD OF INFECTIVITY �Untreated cases are infective for months �Women form largest reservoir

MODE OF SPREAD � Sexual intercourse � Oropharyngeal gonorrhea due to orogenital sexual contact � Infected towels � Purulent conjunctivitis � Ophthalmia neonatorum due to infection in the birth canal

INCUBATION PERIOD � 2 – 7 days

METHOD OF CONTROL q. PREVENTIVE MEASURES q TREATMENT �Procaine pencillin G �Pencillin allergy tetracycline or erythromycin �Sex partner should be treated q OPTHALMIA NEONATORUM ü Pencillin injection ü Pencillin eye drop

TRICHOMONAL VAGINITIS AND URETHRITIS �Trichomonal vaginitis is a protozoal infection of the vagina and the urethra caused by a flagellate parasite – Trichomonas vaginalis

CAUSATIVE ORGANISM � Trichomonas vaginalis � The parasite lives in the vagina and urethra of females � And in male urethra

DIAGNOSIS �By detecting parasite in vaginal and urethral discharge

CLINICAL MANIFESTATION q MALE Ø Mucoid discharge Ø Slight irritation q FEMALE Ø Vulvar irritation Ø Frothy yellowish discharge Ø Putrid odour of discharge

TREATMENT q Metronidazole 200 mg thrice daily for 7 days

CHANCROID (SOFT SORE) q FEATURES Ø Small red lesion appear on the genitals as a papule or vesicle which becomes a pustule and ulcerated Ø Ulcers multiple and painful Ø Soft bleeding surface Ø Ragged undermined edges Ø Lymph glands are enlarged, tender and matted Ø Suppuration of lymph glands Ø Phimosis in male Ø Extragenital lesions on the lips, tongue, chin, breast and umbilicus

CHANCROID (SOFT SORE) EPIDEMIOLOGY q CAUSATIVE AGENT Ø Duncrey bacillus (H. duncrey) Ø Abrasions, cut and wound predispose to infection q PERIOD OF INFECTIVITY Ø Person remains infective till the lesions are healed q INCUBATION PERIOD Ø 2 -5 days , 24 hrs if there is abrasion q TREATMENT Ø Sulphadimidine 4 gm daily for 10 -15 days in divided doses Ø Tetracycline 0. 5 gm four times a day for 10 days

LYMPHOGRANULOMA VENEREUM � LGV is a sexually transmitted disease caused by the organism Chlamydia trachomatis �It is more common in South India

LYMPHOGRANULOMA VENEREUM q CAUSATIVE ORGANISM Ø Chlamydia trachomatis q ROUTE OF ENTRY Ø Breaks in the skin Ø It can cross epithelial cell layer of the mucous membranes q INCUBATION PERIOD Ø 3 – 30 days

LYMPHOGRANULOMA VENEREUM q. CLINICAL FEATURES Ø Primarily an infection of the lymphatics and lymph nodes Ø Climatic bubo Ø Iguinal glands are enlarged and matted, forming tender mass and which may burst Ø Discharging sinuses Ø Ano rectal stricture Ø Urethral lesions with fistulae Ø Fever Ø Body aches

LYMPHOGRANULOMA VENEREUM q DIAGNOSIS Ø Serological testing q TREATMENT Ø Surgical correction of deformity Ø Doxycycline, Erythromycin and Tetracycline

GRANULOMA INGUINALE(DONOVANOSIS) q CAUSATIVE ORGANISM Ø Calymmatobacterium granulomatis (Donovanis granulomatis) q MODE OF TRANSMISSION Ø Contact with lesions q INCUBATION PERIOD Ø 8 – 80 days q SPECIFIC TREATMENT Ø Tetracycline 500 mg four times daily for 10 days Ø Clotrimoxazole and chloramphenicol

GRANULOMA INGUINALE(DONOVANOSIS) q CLINICAL FEATURES Ø Lesions appear on the genitals as a hard papule or vesicles that are ulcerated Ø Floor of the ulcer is painless with red velvety granulation Ø Extra genital lesions occur in the warm and moist area (scrotum, labia and vagina)