Congenital SucraseIsomaltase Deficiency CSID among Alaska Native People

































- Slides: 35



Congenital Sucrase-Isomaltase Deficiency (CSID) among Alaska Native People Presented by: Claire Siekaniec, MS, RD, LD - CSID Outreach and Education Coordinator Community Health Services, ANTHC

Disclosure ANTHC CSID Program and Coordinator position received past support through a grant from QOL Medical, LLC.

Objectives • Increase awareness of CSID among Alaska Native people • Identify symptoms of CSID • Understand management of CSID symptoms • Discuss ANTHC’s CSID Outreach and Education Program

Outline • Background – Symptoms – Genetics – Diagnosis – Prevalence • Management – Nutrition therapy – Medication therapy • ANTHC CSID Program

Congenital Sucrase-Isomaltase Deficiency (CSID) • Genetic disorder - affects ability to digest certain sugars • Polysaccharides – starch, glycogen • Disaccharides – sucrose, maltose, lactose • Monosaccharides – glucose, fructose, galactose • Digestive enzymes break down poly and disaccharides to monosaccharides

Digestive Enzyme Activity • Sucrase-isomaltase (SI) is a disaccharidase on the brush border membrane of the small intestines – Sucrase • Breaks down sucrose and maltose • Sucrose = fructose + glucose – Isomaltase • Breaks down isomaltose and maltose • Maltose = glucose + glucose • In CSID, activity of the SI enzyme is absent or reduced

CSID Symptoms When disaccharides are not broken down: • Bacteria feed off the sugar in the colon causing fermentation • Undigested sugars retain water causing osmotic diarrhea

CSID Symptoms Common symptoms: • Watery diarrhea • Bloating/gas • Abdominal pain Severe symptoms may lead to malnutrition or failure to thrive

Possible Indicators of CSID • History of watery diarrhea that can be traced to introduction of table foods • Family history of “allergy” or intolerance to sugar • Symptoms appear when eating more store bought foods and less Alaska Native traditional foods

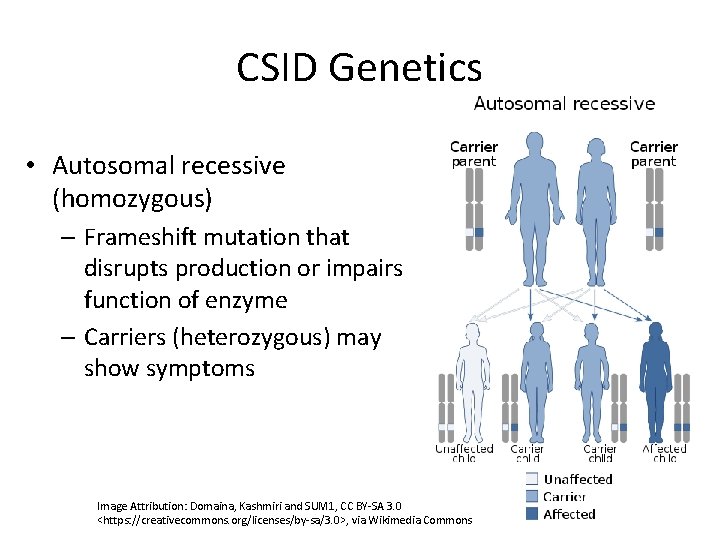
CSID Genetics • Autosomal recessive (homozygous) – Frameshift mutation that disrupts production or impairs function of enzyme – Carriers (heterozygous) may show symptoms Image Attribution: Domaina, Kashmiri and SUM 1, CC BY-SA 3. 0 <https: //creativecommons. org/licenses/by-sa/3. 0>, via Wikimedia Commons

CSID Genetics Title: Congenital sucrase-isomaltase deficiency: identification of a common Inuit founder mutation Authors: Marcadier JL, Boland M, Scott R, et al. Published in Canadian Medical Association Journal in 2015 Results and Interpretation: identification of a homozygous, frameshift mutation, SI c. 273_274 del. AG (p. Gly 92 Leufs*8), responsible for high prevalence of CSID among Inuit people.

CSID Testing • Genetic testing through Fulgent Genetics • Blood sample + test requisition form + testing consent • Full sequencing of SI gene • Cost: $895 • Known mutation • Cost: $200 • Other testing methods – Intestinal biopsy: disaccharidase assay – Breath tests

Breath Test • Carbon-13 sucrose breath test – 8 hours fasting – 20 g sucrose – Series of 4 small tubes the patient blows into over a period of 90 minutes • A healthcare professional can order the test by calling 1 -800 -705 -1962

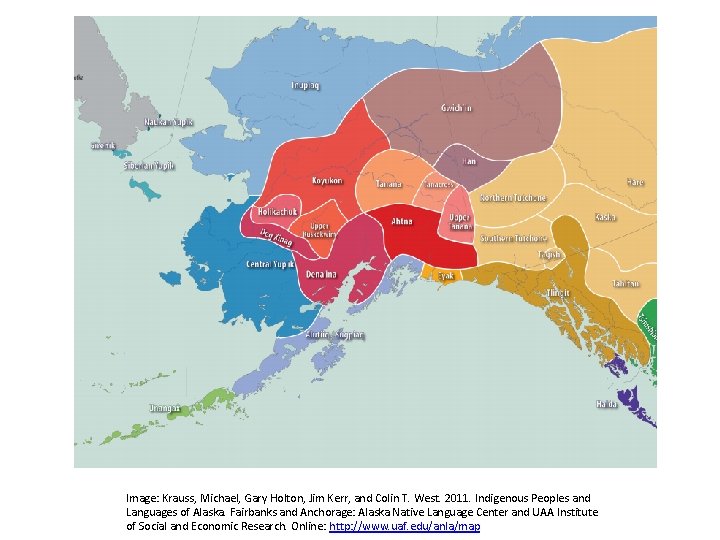
CSID Prevalence • 0. 2% of North Americans of European ancestry • 5 -10% of Greenland/Canadian Inuit people • Unknown at this time in Alaska Native people Image: Krauss, Michael, Gary Holton, Jim Kerr, and Colin T. West. 2011. Indigenous Peoples and Languages of Alaska. Fairbanks and Anchorage: Alaska Native Language Center and UAA Institute of Social and Economic Research. Online: http: //www. uaf. edu/anla/map

Management of CSID

CSID Management Goals: • Minimize symptoms • Improve quality of life • Promote physical growth for infants and children

Nutrition and CSID • Modify diet - Avoid or limit foods high in sucrose and starch Alaska Native traditional foods are naturally low in sucrose and starch making them perfect for managing CSID Image Credits: ANTHC Health Promotion staff

Changes in Eating Patterns • May be increase in sedentary lifestyle • May be decrease or loss of traditional knowledge – Move out of village – Busy lives (working, other priorities) – Increase in store bought foods with cash economy – Gas is expensive for travel/hunting – Climate change

Nutrition and CSID • Store bought foods are often high in sucrose and/or starch • Can be difficult to manage CSID symptoms with higher intake of foods that contain sucrose and starch – Leads to poor nutrition, failure to thrive, and/or poor quality of life

Nutrition and CSID • Fruits and Vegetables – Many fruits and vegetables contain sucrose – use food guides to help determine tolerances • Dairy – Most plain/unsweetened dairy products are tolerated • Fats and Oils – Most are tolerated

Nutrition and CSID • Protein – Most animal protein sources are tolerated – Starchy plant based proteins such as beans/lentils/nuts may not be tolerated • Starches – Individual tolerance varies – Processed foods often contain sucrose and starch o Read ingredient labels

Infant Formula & Supplements • • Infants Breast milk and standard, lactose-based formulas are usually tolerated Most other formulas contain sucrose and/or starch Carbohydrate free (RCF ®) formula available – not nutritionally complete Children Nutritional supplements (Pediasure ®, Ensure ®, etc. ) all contain sucrose and/or starch as carbohydrate source

CSID Management and Tolerance • Will not “outgrow” disorder but tolerances may change as the GI tract lengthens • Food tolerances are different for every person – Determine individual tolerances • Introduce 1 new food at a time and track symptoms • Work with a Registered Dietitian for nutrition education and ongoing support

Prescription Medication • Sacrosidase (Brand name: Sucraid®) – Enzyme replacement therapy for sucrase – Dosage weight dependent • Taken with every meal/snack that contains sucrose – Is not covered by Medicaid • Covered by most private insurance – Requires refrigeration – Does not help with starch digestion

T-SHIP Tribally Sponsored Health Insurance Program – Aids in coverage of sacrosidase – ANTHC TSHIP assists with enrolling patients – Visit anthc. org/tship for more information

ANTHC CSID Program Goals of the Program: • Increase awareness of CSID • Resource center for patients, families, and medical staff • Maintain culturally relevant educational materials – CSID education materials for clinics, waiting rooms, health fairs – Find materials and other resources on anthc. org/csid




Resources and References • ANTHC CSID webpage: anthc. org/csid • Pocket Guide to Alaska Native Pediatric Diagnoses http: //anmc. org/files/Pocket-Guide-to-Alaska-Native-Pediatric. Diagnoses_web. pdf • CSID Cares: http: //csidcares. org/ • Sucraid®: http: //sucraid. com • Fulgent Genetics https: //www. fulgentgenetics. com/congenital-sucrase-isomaltase-deficiency • CSID ADN article http: //www. adn. com/article/20150119/sugar-intolerance-northernpopulations-linked-specific-gene-researchers-say

Additional References 1. Treem, W. (2012). Clinical Aspects and Treatment of Congenital Sucrase-Isomaltase Deficiency. Journal of Pediatric Gastroenterology and Nutrition, 55, pp. S 7 -S 13. 2. Gericke, B. , Amiri, M. and Naim, H. (2016). The multiple roles of sucrase-isomaltase in the Intestinal physiology. Molecular and Cellular Pediatrics, 3(1). 3. Marcadier, J. , Boland, M. , Scott, C. , Issa, K. , Wu, Z. , Mc. Intyre, A. , Hegele, R. , Geraghty, M. and Lines, M. (2014). Congenital sucrase–isomaltase deficiency: identification of a common Inuit founder mutation. Canadian Medical Association Journal, 187(2), pp. 102107. 4. Husein, D. , Wanes, D. , Marten, L. , Zimmer, K-P. , and Naim, H. (2019). Heterozygotes Are a Potential New Entity among Homozygotes and Compound Heterozygotes in Congenital Sucrase-Isomaltase Deficiency. Nutrients, 11 (10), 2290; https: //doi. org/10. 3390/nu 11102290. 5. Genetics. edu. au. (2020). [online] Available at: http: //www. genetics. edu. au/publications -and-resources/facts-sheets/fact-sheet-7 -autosomal-recessive-inheritance [Accessed Dec. 2020]. 6. Rarediseases. info. nih. gov. (2018). Congenital sucrase-isomaltase deficiency | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program. [online] Available at: https: //rarediseases. info. nih. gov/diseases/7710/congenital-sucrase-isomaltasedeficiency [Accessed 4 Sep. 2018].

Thank You Image by Samantha Maloney in Kotzebue
