Terapia delle Micosi Invasive Trieste Pneumo Trieste 2017










- Slides: 36

Terapia delle Micosi Invasive Trieste, Pneumo. Trieste 2017 Roberto Luzzati SC Malattie Infettive, Ospedale Maggiore Azienda Ospedale/Università ASUITS, Trieste

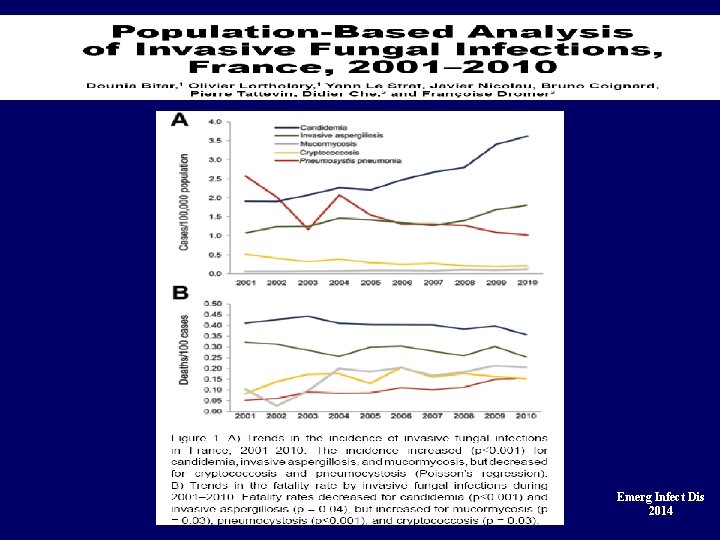
Emerg Infect Dis 2014

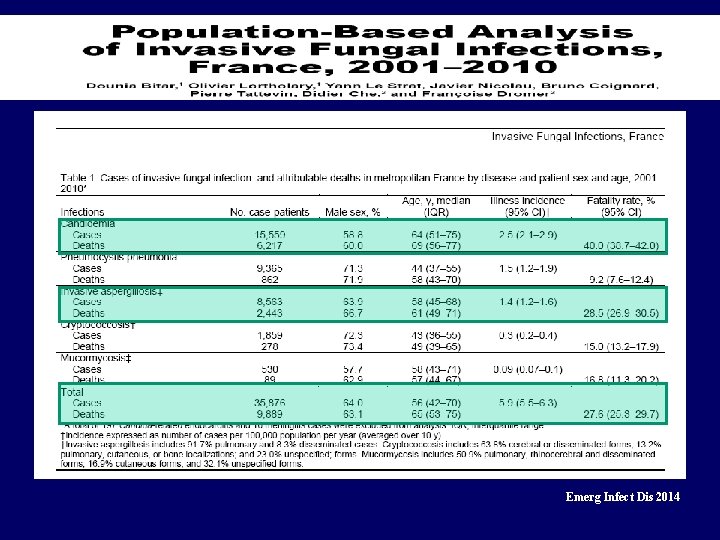
Emerg Infect Dis 2014

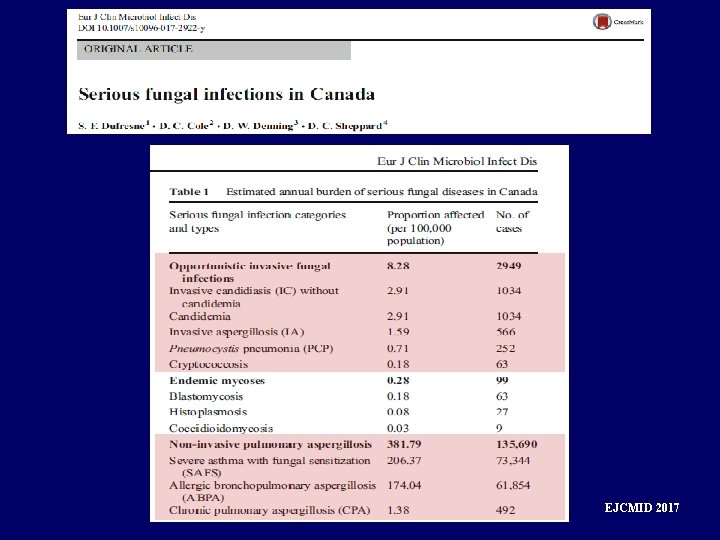
EJCMID 2017


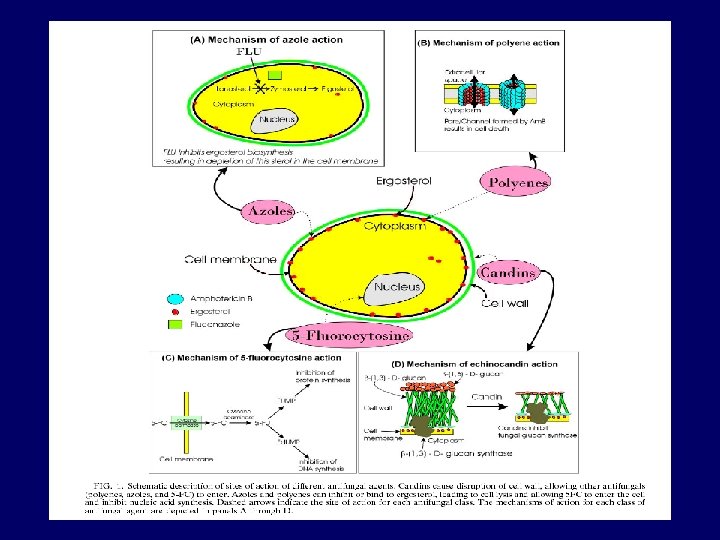
Principali antifungini disponibili per uso clinico o in sviluppo • • Polieni – Amfotericina B (AMB) desossicolato (D-AMB) – AMB liposomiale (L-AMB) – AMB complessi lipidici (ABLC) Azolici – Fluconazolo – Itraconazolo – Voriconazolo – Posaconazolo Flucitosina Echinocandine – Caspofungin – Anidulafungin – Micafungin Novità approvate o in fase II/IIIa -Isavuconazolo (Basilea) -Posaconazolo e. v (MSD) -echinocandina long-acting (Cidara, US)


ANTIFUNGAL AGENTS Range of Activity for Selected Pathogens Moulds Yeasts AMB FCZ ITZ VCZ PCZ IVZ CF MF AF Candida albicans Candida tropicalis Candida parapsilosis Candida krusei Candida glabrata* Cryptococcus neoformans Aspergillus fumigatus Mucor spp Rhizopus spp Fusarium spp * Strains with reduced susceptibility to azoles AMB, Amphotericin B Azole: FCZ, Fluconazole; ITZ, Itraconazole; VCZ, Voriconazole; PCZ, Posaconazole; IVZ, Isavuconazolo Echinocandin: CF, Caspofungin; MF, Micafungin; AF, Anidulafungin Adapted from JP Donnelly, by Malcolm Richardson.

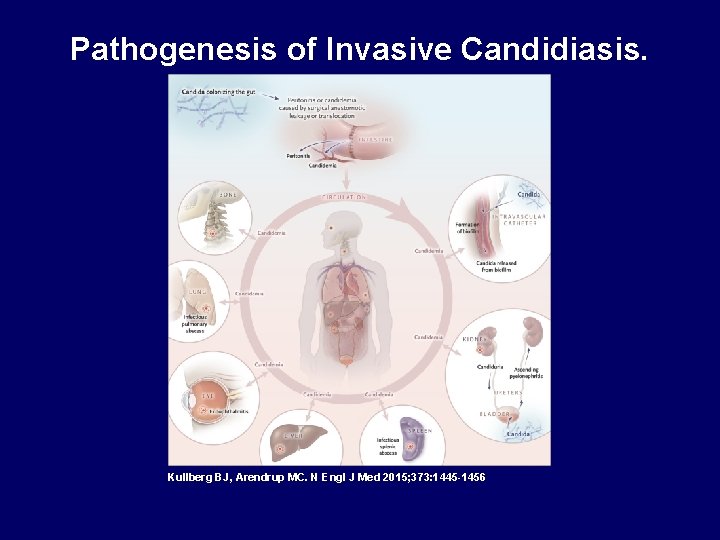
Pathogenesis of Invasive Candidiasis. Kullberg BJ, Arendrup MC. N Engl J Med 2015; 373: 1445 -1456

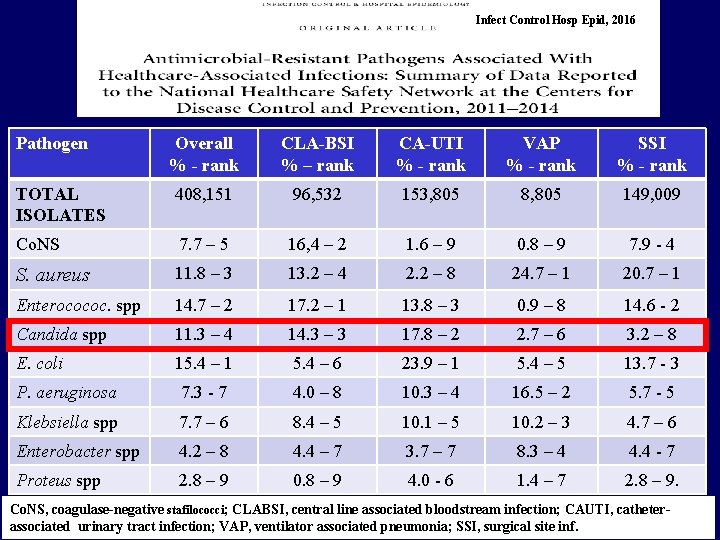
Infect Control Hosp Epid, 2016 Pathogen Overall % - rank CLA-BSI % – rank CA-UTI % - rank VAP % - rank SSI % - rank TOTAL ISOLATES 408, 151 96, 532 153, 805 8, 805 149, 009 Co. NS 7. 7 – 5 16, 4 – 2 1. 6 – 9 0. 8 – 9 7. 9 - 4 S. aureus 11. 8 – 3 13. 2 – 4 2. 2 – 8 24. 7 – 1 20. 7 – 1 Enterocococ. spp 14. 7 – 2 17. 2 – 1 13. 8 – 3 0. 9 – 8 14. 6 - 2 Candida spp 11. 3 – 4 14. 3 – 3 17. 8 – 2 2. 7 – 6 3. 2 – 8 E. coli 15. 4 – 1 5. 4 – 6 23. 9 – 1 5. 4 – 5 13. 7 - 3 P. aeruginosa 7. 3 - 7 4. 0 – 8 10. 3 – 4 16. 5 – 2 5. 7 - 5 Klebsiella spp 7. 7 – 6 8. 4 – 5 10. 1 – 5 10. 2 – 3 4. 7 – 6 Enterobacter spp 4. 2 – 8 4. 4 – 7 3. 7 – 7 8. 3 – 4 4. 4 - 7 Proteus spp 2. 8 – 9 0. 8 – 9 4. 0 - 6 1. 4 – 7 2. 8 – 9. Co. NS, coagulase-negative stafilococci; CLABSI, central line associated bloodstream infection; CAUTI, catheterassociated urinary tract infection; VAP, ventilator associated pneumonia; SSI, surgical site inf.


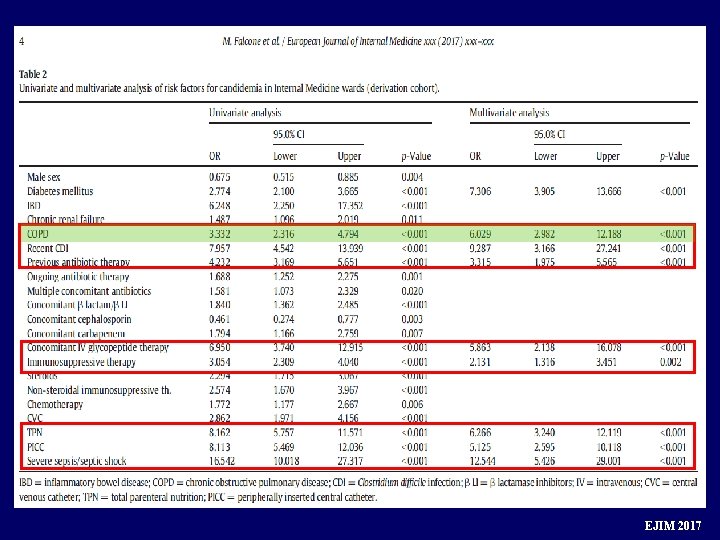
EJIM 2017

EJIM 2017

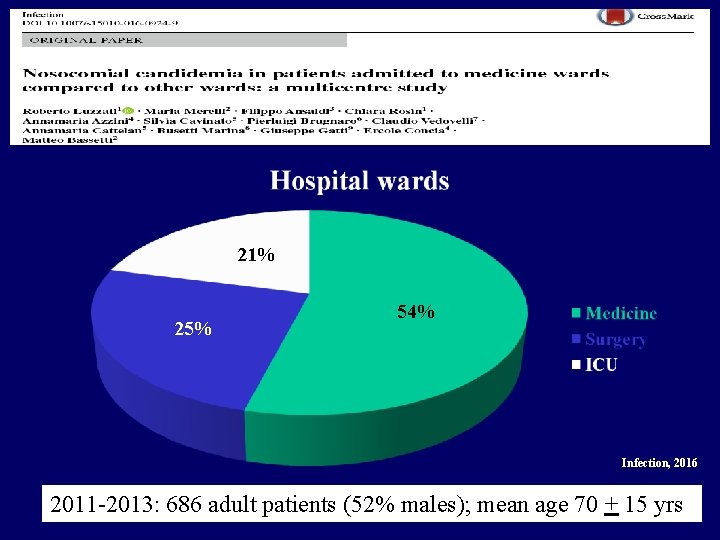
21% 25% 54% Infection, 2016 2011 -2013: 686 adult patients (52% males); mean age 70 + 15 yrs

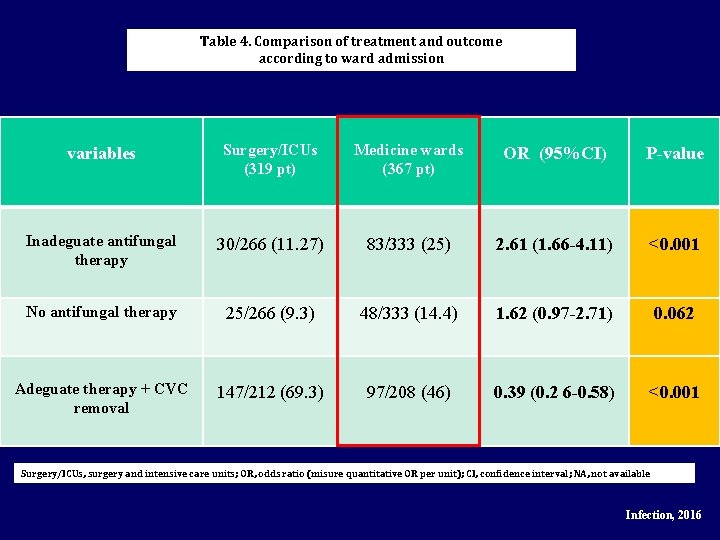
Table 4. Comparison of treatment and outcome according to ward admission variables Surgery/ICUs (319 pt) Medicine wards (367 pt) OR (95%CI) P-value Inadeguate antifungal therapy 30/266 (11. 27) 83/333 (25) 2. 61 (1. 66 -4. 11) <0. 001 No antifungal therapy 25/266 (9. 3) 48/333 (14. 4) 1. 62 (0. 97 -2. 71) 0. 062 Adeguate therapy + CVC removal 147/212 (69. 3) 97/208 (46) 0. 39 (0. 2 6 -0. 58) <0. 001 Surgery/ICUs, surgery and intensive care units; OR, odds ratio (misure quantitative OR per unit); CI, confidence interval; NA, not available Infection, 2016

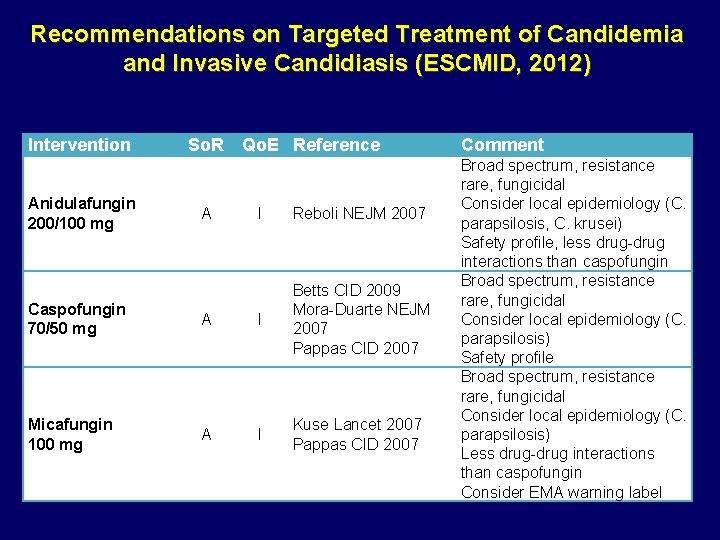
Recommendations on Targeted Treatment of Candidemia and Invasive Candidiasis (ESCMID, 2012) Intervention Anidulafungin 200/100 mg So. R Qo. E Reference A I Reboli NEJM 2007 Caspofungin 70/50 mg A I Betts CID 2009 Mora-Duarte NEJM 2007 Pappas CID 2007 Micafungin 100 mg A I Kuse Lancet 2007 Pappas CID 2007 Comment Broad spectrum, resistance rare, fungicidal Consider local epidemiology (C. parapsilosis, C. krusei) Safety profile, less drug-drug interactions than caspofungin Broad spectrum, resistance rare, fungicidal Consider local epidemiology (C. parapsilosis) Safety profile Broad spectrum, resistance rare, fungicidal Consider local epidemiology (C. parapsilosis) Less drug-drug interactions than caspofungin Consider EMA warning label

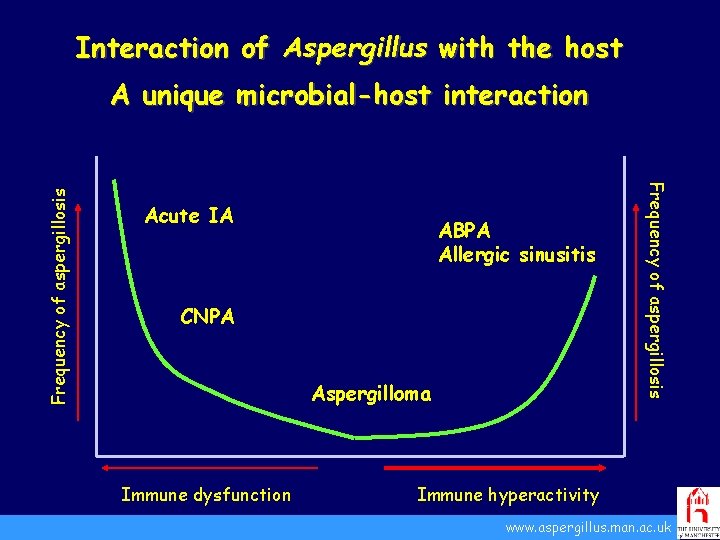
Interaction of Aspergillus with the host Acute IA ABPA Allergic sinusitis CNPA Aspergilloma Immune dysfunction Frequency of aspergillosis A unique microbial-host interaction Immune hyperactivity. www. aspergillus. man. ac. uk


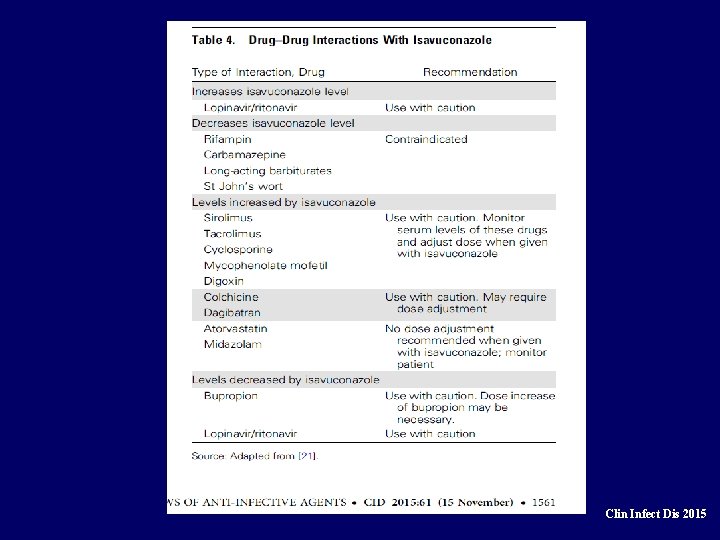
Clin Infect Dis 2015

Clin Infect Dis 2015

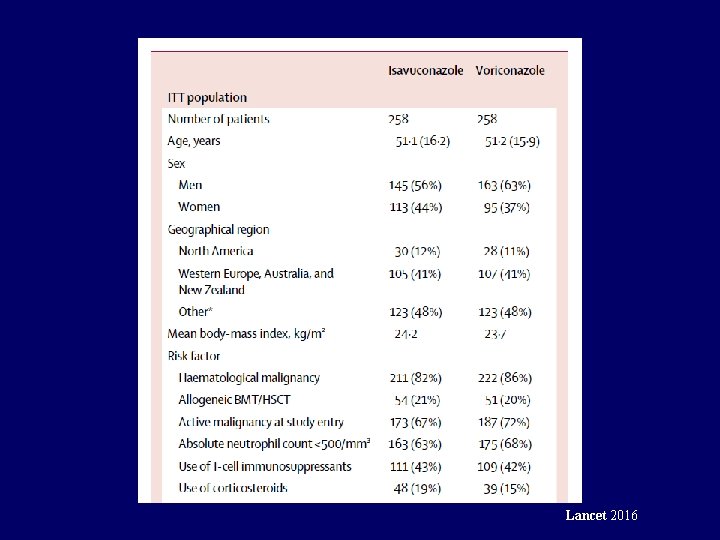
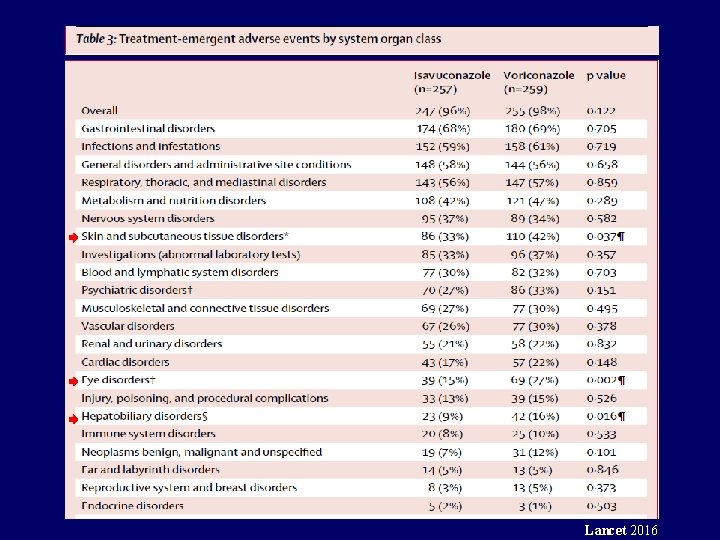
Lancet 2016

Lancet 2016

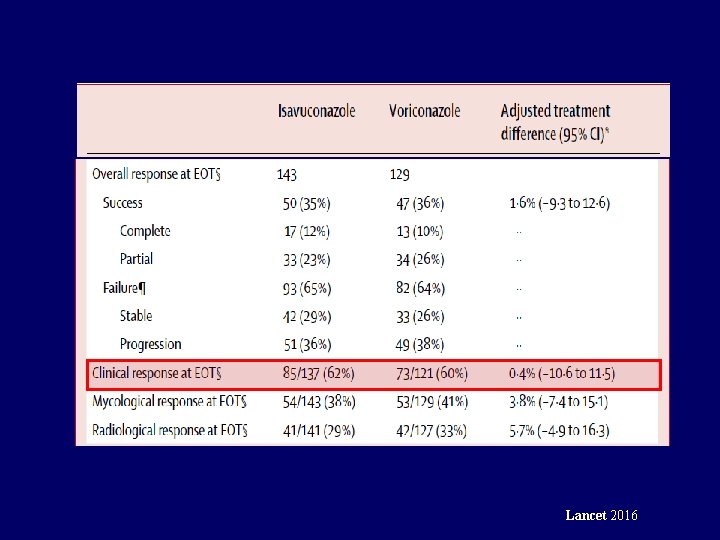
Lancet 2016

Lancet 2016

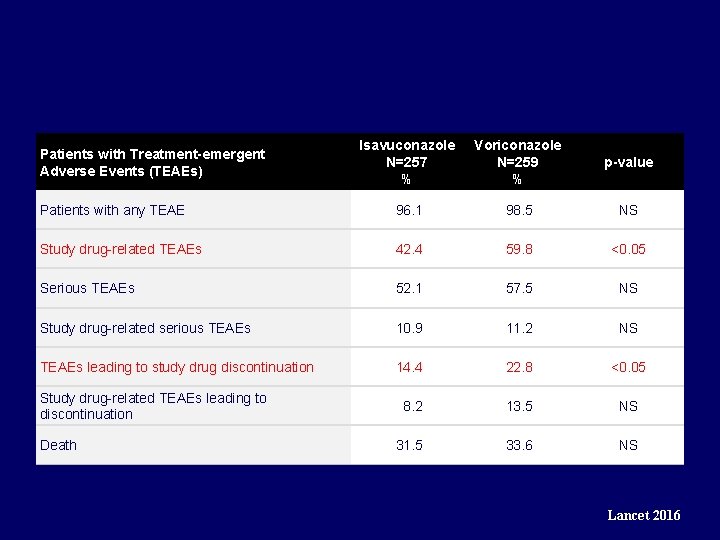
Isavuconazole N=257 % Voriconazole N=259 % p-value Patients with any TEAE 96. 1 98. 5 NS Study drug-related TEAEs 42. 4 59. 8 <0. 05 Serious TEAEs 52. 1 57. 5 NS Study drug-related serious TEAEs 10. 9 11. 2 NS TEAEs leading to study drug discontinuation 14. 4 22. 8 <0. 05 8. 2 13. 5 NS 31. 5 33. 6 NS Patients with Treatment-emergent Adverse Events (TEAEs) Study drug-related TEAEs leading to discontinuation Death Lancet 2016

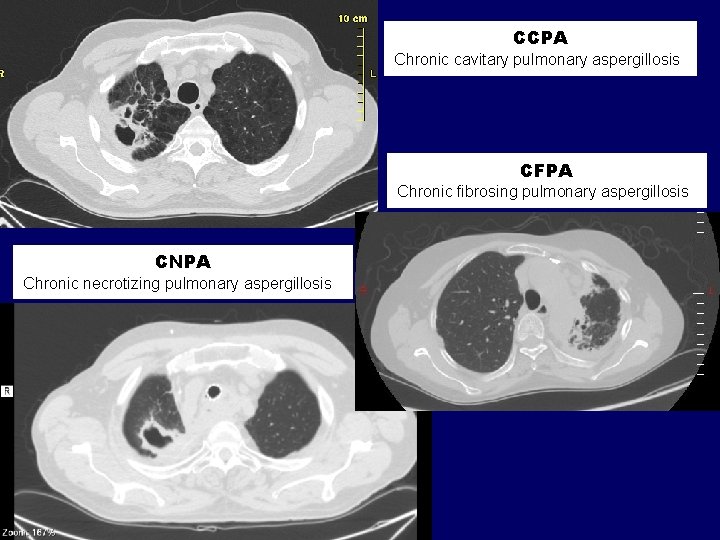
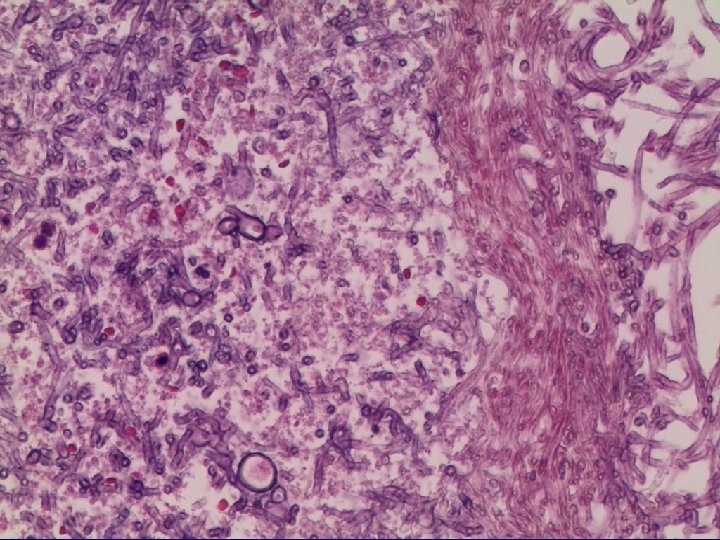
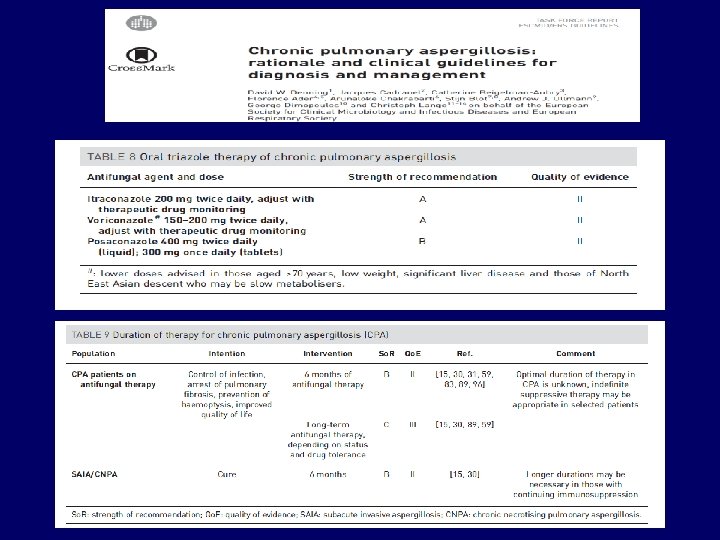
CCPA Chronic cavitary pulmonary aspergillosis CFPA Chronic fibrosing pulmonary aspergillosis CNPA Chronic necrotizing pulmonary aspergillosis



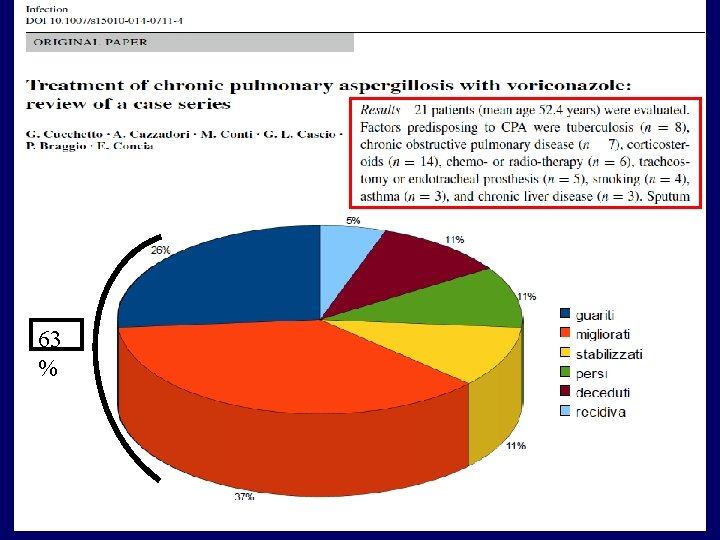
63 %

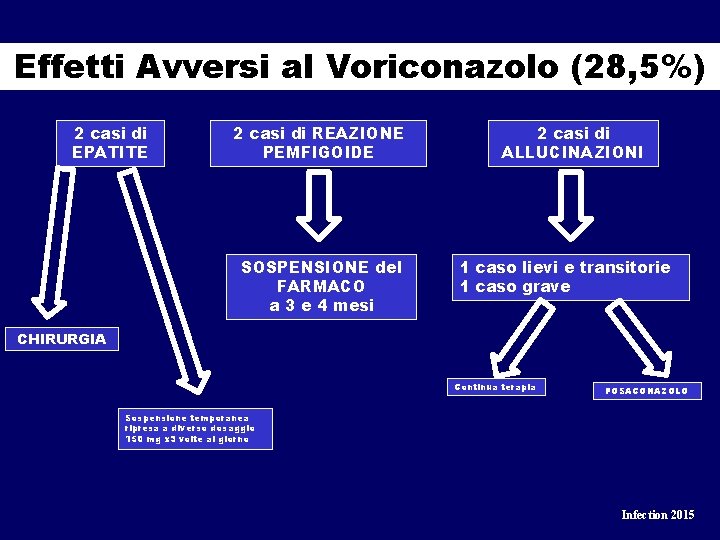
Effetti Avversi al Voriconazolo (28, 5%) 2 casi di EPATITE 2 casi di REAZIONE PEMFIGOIDE SOSPENSIONE del FARMACO a 3 e 4 mesi 2 casi di ALLUCINAZIONI 1 caso lievi e transitorie 1 caso grave CHIRURGIA Continua terapia POSACONAZOLO Sospensione temporanea ripresa a diverso dosaggio 150 mg x 3 volte al giorno Infection 2015

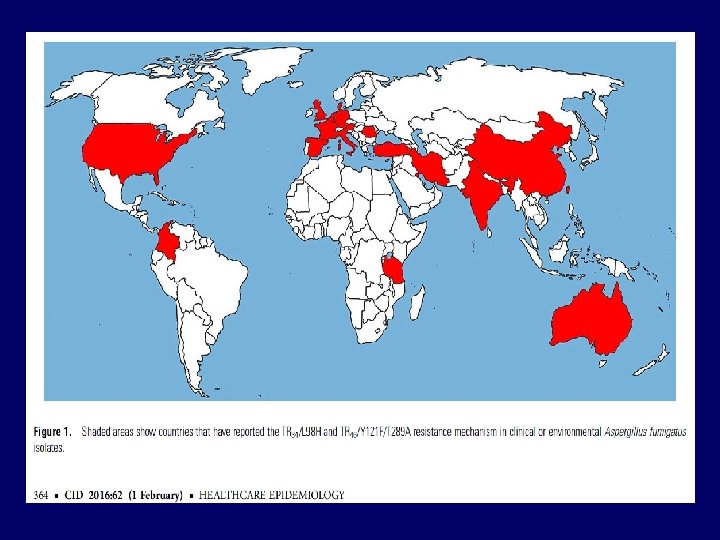
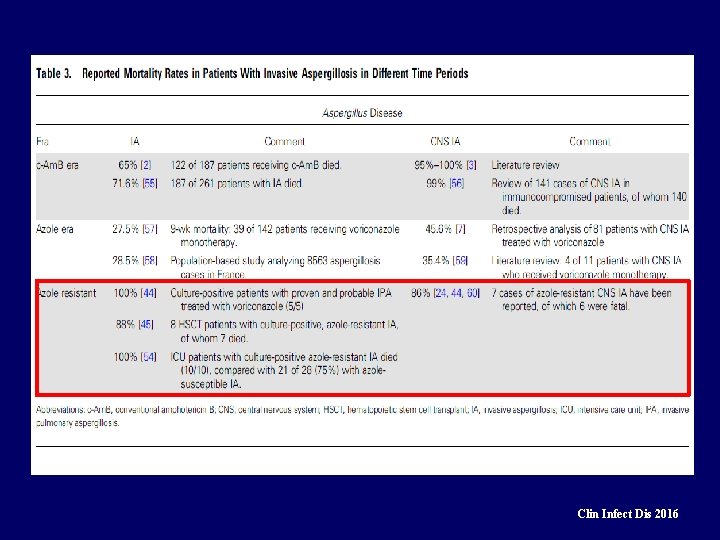
Clin Infect Dis 2016


Clin Infect Dis 2016

AAC 2016

Clin Infect Dis 2016
