SMOKING CESSATION SOME FACTS Very Brief Advice VBA

SMOKING CESSATION SOME FACTS! Very Brief Advice (VBA) Smoking Cessation Referral Nicotine Replacement Therapy (NRT) CQUIN 2018 -2019 R HAQQEE BTS Stop Smoking Champion Clinical Lead CQUIN 2018 -2019

Smoking Facts • SMOKING KILLS PEOPLE ! • Smoking accounts for approximately 79, 000 deaths a year in the United Kingdom • About half of all life-long smokers will die prematurely, losing on average about 10 years of life • Smoking remains the single biggest preventable cause of EARLY death & illness in the UK – more than obesity, alcohol, illicit drugs, road traffic accidents and HIV infection combined • The cost of smoking to the NHS is estimated to be £ 2. 5 billion a year

DEATHS CAUSED BY SMOKING Most smoking-related deaths arise from one of three types of disease: • In 2015 Total Deaths 79, 000 deaths • lung cancer 37, 400 deaths • chronic obstructive pulmonary disease (COPD) • coronary heart disease (CHD) 16, 400 deaths 23, 200 deaths

Smoking & Stroke • Smoking is a strong independent predictor of stroke mortality and incidence • Cigarette smokers have two to three times the risk of thromboembolic or haemorrhagic stroke • Smoking is an independent risk factor for silent brain infarcts • The rates of stroke among former smokers ( >10 yrs. )are not different from those of never-smokers

Smoking & Stroke • Smoking increases the risk of stroke in individuals 40 – 64 years of age • Smoking >20 cigarettes per day increases the risk of stroke in men, especially in hypertensive • Compared with never-smokers, smoking ≥ 10 cigarettes/day had an increased risk of death from stroke at 25 years • The risk of ischemic stroke at younger ages is greatly increased by current cigarette smoking

Smoking and stroke: the more you smoke the more you stroke Reena S Shah and John W Cole Considerable scientific evidence implicates a strong dose–response relationship between smoking and stroke risk

Smoking & Dementia WHO Tobacco knowledge & Dementia 14% of Alzheimer’s disease cases worldwide are potentially attributed to smoking – Smoking is a risk factor for dementia, and quitting could reduce the dementia burden – Second-hand smoke exposure may also increase the risk of dementia – A meta-analysis of studies undertaken mostly in the 1990 s and early 2000 s found that relative to never smokers, current smokers had risks of 1. 79 for AD and 1. 78 for Va. D – Past history of smoking presents less consistent results, possibly indicating that quitting smoking later in life is still beneficial and could reduce the risk of AD or other forms of dementia compared with continued smoking – As no treatments are currently available to cure or alter the progressive course of dementia, it is essential to identify modifiable risk factors for reducing the occurrence of the disease, delaying its onset or reducing its burden

Pathophysiology of Smoking & Dementia Smoking tobacco is hypothesized to cause dementia via several mechanisms. The most recognized causal pathway is via • Vascular risk factors/atherosclerosis that may ultimately cause cerebrovascular disease, stroke and coronary heart disease • Smoking increases total plasma homocysteine, an independent risk factor for stroke, cognitive impairment, Alzheimer's & other dementias • Smoking can cause oxidative stress, which is associated with excitotoxicity, leading to neural death. Oxidative stress is also associated with an inflammatory response that may be directly or indirectly related to the neuropathology of AD • Apolipoprotein E (APOE) ε 4 allele, is a genetic risk factor for dementia, & smoking tobacco can increase the risk for carriers of this gene

Second-hand smoke (SHS)and dementia • Some studies have suggested an increased risk of AD or other forms of dementia among those exposed to SHS • Three publications from a large-scale population-based crosssectional survey in Anhui, China linked SHS exposure with risk of dementia in the general population and among never smokers • These studies also showed that risk of dementia increased with duration and level of exposure. Exposure to SHS at any location (e. g. home or work) increased the risk for all dementias by 78%. The association was strongest for exposure in the home • A study evaluating dementia severity prior to diagnosis concluded that exposure to SHS significantly increased the risk for severe dementia syndromes , and this was related to duration and frequency of exposure to SHS in a dose-dependent manner

Smoking Cessation Why Am I here today ?

BTS National Audit on Smoking Cessation 2016 Key Findings 1. 1 in 4 patients were asked if they smoke 2. 3 out of 4 smokers were not asked if they would like to quit smoking 3. Only 1 in 13 patients who smoked were referred to a smoking cessation service 4. Only 1 in 20 patients who smoked was given NRT to help them abstain from smoking and reduce nicotine withdrawal symptoms whilst in hospital 5. 1 in 16 institutions completely enforce smoke-free grounds 7. 50% of frontline healthcare staff were not offered regular smoking cessation training.

BTS National Tobacco audit 2016 UHNM vs Nationally Summary Report Route of contact: 96. 6% emergency admission • • • Smoking status not documented: 28% vs 27% smokers not asked if they would like to quit 95%vs 79% Non cig smoking status documented: 0% vs 27% Current smokers : 32% vs 25% Quitting Advise : 5% vs 28% Poor communication of referrals and pharmacotherapy in letters/discharge

LOCAL PROBLEM Stoke On Trent Tobacco Control Strategy 2015 -2018 • • • Major burden in terms of mortality and morbidity, killing 1500 people each year Negative impact on local economy Cost 80 million in lost productivity & healthcare costs • Smoking rates – adults – 15 yr old • • • 28% vs 18% nationally Some areas 35 -45% 13% vs 10% nationally 1: 3 adults in Stoke-on-Trent smoke youth smoking rates are 3% above the national average 1: 5 women smoke in pregnancy 23% vs 14% women in SOT were smoking at time of delivery 30% of children in SOT are exposed to the harmful effects of second hand smoke in the home & 40% to second hand smoke in the car
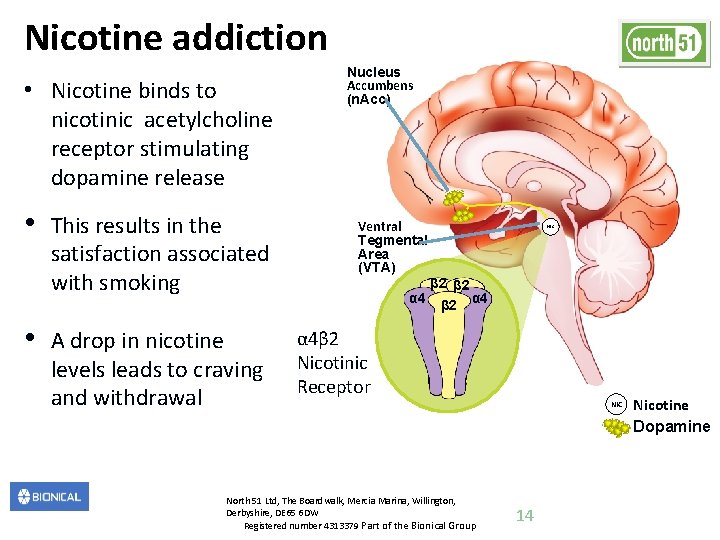
Nicotine addiction • Nicotine binds to nicotinic acetylcholine receptor stimulating dopamine release • • This results in the satisfaction associated with smoking A drop in nicotine levels leads to craving and withdrawal Nucleus Accumbens (n. Acc) Ventral Tegmental Area (VTA) α 4 NIC β 2 α 4β 2 Nicotinic Receptor North 51 Ltd, The Boardwalk, Mercia Marina, Willington, Derbyshire, DE 65 6 DW Registered number 4313379 Part of the Bionical Group NIC 14 Nicotine Dopamine

What we should be doing – Very Brief Advice • ASK – all patients if they smoke • ADVISE – the best way to stop • ACT – provide a referral or offer behavioural support and drug treatment • Visit www. ncsct. co. uk to complete a short course on how to deliver Very Brief Advice

1. ASK smoking status • All patients should be asked their smoking status – ‘Current, Ex- or Never Smoker’ • This should be clearly documented • Consider use of a proforma or a stamp ‘Are you still smoking? ’ ‘Do you smoke? ’ ‘I know you recent gave up smoking – are you still off the cigarettes? ’

2. ADVISE – on best way to quit Offering support to help smokers quit is more effective than simply telling them to stop ‘The best way to stop smoking is with the combination of treatment and support that is available on the NHS – is that something that would interest you? ’ ‘With the right support and treatment, it can be much easier to stop, and stay stopped’

3. ACT – by providing support • Provide a referral to a dedicated stop smoking advisor OR • Provide a prescription • NRT • Bupropion • Varenicline • Give ‘common sense’ behavioural support

Very Brief Advice Why the SMOKING CESSATION Team is proposing it ? The evidence of effectiveness in hospital � Cochrane Review of smoking cessation interventions for hospitalised patients ◦ increased rate of long term quitting, if they include regular behavioural support and pharmacotherapy that is continued at least one month after discharge ◦ Quit rates among patients who want to quit and take up a referral to stop smoking services are between 15 -20% compared to 3 -4% without a referral

Quit Smoking VERY Brief Advice • Everyone who smokes should be advised to quit (NICE) • Offering support to help smokers quit is more effective than simply telling them to stop • The best way to stop smoking is with the combination of treatment and support that is available on the NHS. . • With the right support and treatment, it can be much easier to stop, and stay stopped

Why the SMOKING CESSATION Team is proposing it ? Case for medical patients � Smoking cessation is associated with a 43% decreased risk in hospitalization in COPD & reduced risk of developing bronchitis and pneumonia � Smoking cessation before the initiation of radiation therapy in lung cancer is associated with an increased rate of complete response to treatment � Reduces the risk of re-hospitalisation for people with heart disorders Case for surgical patients � Smoking is associated with Ø Local wound complications & delayed healing Ø Pulmonary & cardiac complications Ø Increased need for postoperative intensive care and longer periods of hospitalisation Ø Increased anaesthetic dosage and increased experience of postoperative pain

Why inpatients? � Hospitalisation offers an opportune time to encourage patients to stop smoking for four reasons. 1. This time is often a “teachable moment” where patients are more receptive to intervention and are motivated to quit 2. The hospital smoke free environment creates an external force to support abstinence ( National CQUIN 2018) smoke free hospital! 3. 4. Patients are ideally placed to be given information about treatment options, support through withdrawal and signposted to specialist services Abstaining from smoking at this time can lead to significant health benefits
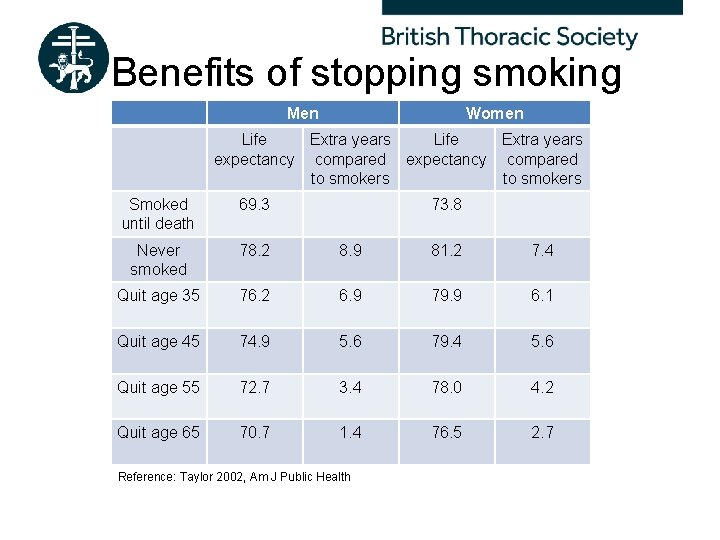
Benefits of stopping smoking Men Women Life Extra years expectancy compared to smokers Smoked until death 69. 3 73. 8 Never smoked 78. 2 8. 9 81. 2 7. 4 Quit age 35 76. 2 6. 9 79. 9 6. 1 Quit age 45 74. 9 5. 6 79. 4 5. 6 Quit age 55 72. 7 3. 4 78. 0 4. 2 Quit age 65 70. 7 1. 4 76. 5 2. 7 Reference: Taylor 2002, Am J Public Health

Prescribing for Smoking Cessation � Knowledge of indications for and side-effects of ◦ Nicotine replacement therapy (NRT) ◦ Varenicline (Champix) ◦ Bupropion (Zyban)

Nicotine replacement therapy (NRT) � � � Ø Ø Ø Use instead of cigarettes after stopping smoking suddenly Use to reduce the amount of cigarettes smoked prior to quitting Use to treat cravings in smoke-free settings such as hospitals NRT works best in conjunction with behavioural support NRT doubles rates of quitting: 17. 6% vs 10. 6% placebo Combination NRT 31. 5% ( PATCHES & LOZENGES) Use NRT to cover temporary abstinence in hospital

Prescribing NRT FLOW CHART � � NRT Patches ◦ Cig >10/day – start with high-strength patch 21 mg ◦ Cig <10/day – start with medium strength patch 14 mg ◦ Increase strength if withdrawal symptoms NRT Quick-acting ( Lozenges, gums etc) ◦ Use when urge to smoke occurs (or to prevent cravings) PRN
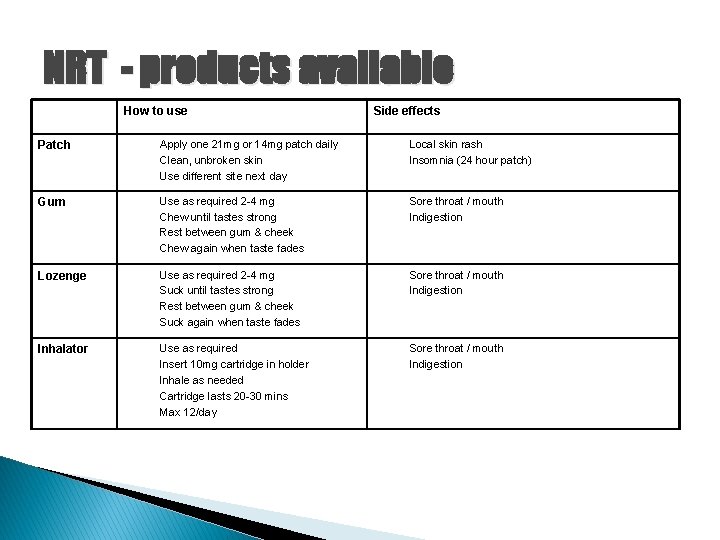
NRT - products available How to use Side effects Patch Apply one 21 mg or 14 mg patch daily Clean, unbroken skin Use different site next day Local skin rash Insomnia (24 hour patch) Gum Use as required 2 -4 mg Chew until tastes strong Rest between gum & cheek Chew again when taste fades Sore throat / mouth Indigestion Lozenge Use as required 2 -4 mg Suck until tastes strong Rest between gum & cheek Suck again when taste fades Sore throat / mouth Indigestion Inhalator Use as required Insert 10 mg cartridge in holder Inhale as needed Cartridge lasts 20 -30 mins Max 12/day Sore throat / mouth Indigestion

Cautions with NRT � � � NRT is less risky than smoking Care with acute cardiac events, but safe in chronic disease Watch blood sugars in diabetics Care with inhalator in COPD Caution in severe hepatic / renal impairment Short-acting products best in pregnancy if required

Bupropion • Slow release prep - Zyban® • Selective inhibitor (weak) of dopamine & noradrenalin uptake • Prescription only • Licensed only for smoking cessation with motivational support

Bupropion � � � Reduces urge to smoke and symptoms of nicotine withdrawal Use in those who are motivated to stop but ◦ Can’t use NRT, or ◦ Failed to stop using NRT Similar efficacy to NRT – 19. 1% cessation vs 10. 6% with placebo

Bupropion: cautions and side-effects � � Generally safe Risk of seizures less than 1 in 1, 000 (contra-indicated in epilepsy) Avoid in eating disorders, bipolar disorder, liver cirrhosis, pregnancy Caution in those with low seizure threshold

Varenicline ‘Champix’ in UK � � First drug specifically designed to help smokers NICE approved for NHS prescription to aid quitting in 2007 Very effective for daily smokers Most smokers can take it irrespective of their health status or other medication ◦ apart from pregnant and breastfeeding mothers , under 18 s and those with end stage renal disease

Varenicline � � � Reduces cravings for nicotine by binding to nicotinic acetylcholine receptors in the brain - High affinity & selectivity Reduces withdrawal symptoms by releasing reduced levels of Dopamine Relieves craving and withdrawal symptoms, reduces rewarding effect of smoking More than doubles chances of quitting More effective than bupropion, similar efficacy to combination NRT – 27. 6% cessation vs 10. 6% with placebo Most effective monotherapy and few interactions

Varenicline: dosing 1 -2 weeks before stop date Start varenicline - 500 micrograms daily (days 1 -3) - 500 micrograms twice daily (days 4 -7) - 1 mg twice daily (day 8 onwards) Stop date Stop smoking Continue varenicline 12 weeks Complete course

Varenicline: Champix cautions and side-effects � � Generally safe Main side-effect is nausea (30%) ◦ Usually mild ◦ Only 3% have to stop ◦ Take with food Reduce dose in renal impairment There have been reports of mood change and suicidal ideation in patients on varenicline, but no causation has been established, and a recent meta-analysis of 17 trials found no evidence of higher rates of suicidal events, depression, or aggression/agitation in those on varenicline compared to placebo. ◦ ◦ ◦ References: BNF – www. bnf. org Cahill et al (2013) Pharmacological intervention for smoking cessation: an overview and network meta-analysis. Cochrane Database Syst Rev. 5: CD 009329. doi: 10. 1002/14651858. CD 009329. pub 2. Cahill et al (2014) Pharmacological treatments for smoking cessation. JAMA. 311(2): 193 Gibbons and Mann (2013). Varenicline, smoking cessation, and neuropsychiatric adverse events. Am J Psychiatry. 170: 1460 -7. Zwar et al (2014) Supporting smoking cessation. BMJ. 348: f 7535

Electronic cigarettes? � Also known as: ◦ E-cigarettes ◦ Electronic nicotine delivery systems’(ENDS) ◦ Vapourisers � Battery-operated devices that delivery nicotine via vapour – inhaled similar to cigarettes Do not contain tobacco (‘vaping’ rather than ‘smoking’) �

What are the benefits of e-cigarettes? � Less harmful than conventional cigarettes ◦ Far fewer harmful components ◦ UK Government report: 95% less harm ◦ Main concern is contaminants (lack of regulation)

Preventing ill health by risky behaviours – alcohol and tobacco � CQUIN 2018 -2019 !!

9. Preventing ill health by risky behaviours – alcohol and tobacco CQUIN 2018 -2019
Proud to Care Nursing Document

“Blue” Post take Proforma on AMU

Guidance for Prescribing Nicotine Replacement Therapy

SMOKING CESSATION REFERRAL PATHWAYS AT UHNM � 2 PATHWAYS INPATIENT PATHWAY Ordercom ICM OUTPATIENT PATHWAY(Community Smoking Hub) PORTAL→→ STRUCTURED NOTE→→LIVING WELL REFERRAL FORM→→SUBMIT AS COMPLETE I

Summary � � � � 70% of smokers want to stop smoking but need help to do so All health professionals should ask and advise about stopping smoking Behavioural support and pharmacotherapy can increase the chances of successful quitting All agents should be used with behavioural support Varenicline and combination NRT most effective Review cautions and ensure follow-up to assess side-effects CQUIN compliance will earn us MONEY!

STUDIES! • • Asplund et al. Eight European countries 93, 695 men and women. Smoking confers an increased risk of stroke Men: 1. 82 ; Women: 2. 84 Putaala et al. Silent brain infarcts and leukoaraiosis in young adults with first-ever ischemic stroke Finland; 669 young adults. Smoking is an independent risk factor for silent brain infarcts • Myint et al. Risk factors for first-ever stroke in the EPIC-Norfolk prospective population-based study. UK. 25, 000 individuals. There is an increased risk of stroke among current smokers compared with never-smokers. Ex-smokers did not have increased risk of stroke compared with nonsmokers Zhang et al. Incidence and risk factors for stroke in American Indians: the Strong Heart study. USA: Native American tribes/communities 7252 individuals. Current smokers had significantly higher stroke incidence than past smokers and nonsmokers Song et al. Risk of stroke and myocardial infarction after reduction or cessation of cigarette smoking: a cohort study in Korean men. 475, 734 men. Sustained ex-smokers and never-smokers had lower risks of all stroke Assmann et al. Assessing risk of myocardial infarction and stroke: new data from the Prospective Cardiovascular Munster (PROCAM) study, Germany. 26, 975 individuals. Cigarette smoking was found to be independently predictive of stroke risk Weikert et al. Joint effects of risk factors for stroke and transient ischemic attack in a German population: the EPIC Potsdam study, Germany. 25, 538 individuals. There is a stronger association between the risk factor of smoking with ischemic stroke than TIA. The attributable risk of smoking for ischemic stroke is 8. 1% Harmsen et al. Long-term risk factors for stroke: twenty-eight years of follow-up of 7457 middle-aged men in Goteborg Sweden. Smoking increased the risk of stroke during the follow-up period of 16– 21 years. Dagenais et al. Impact of cigarette smoking in high-risk patients participating in a clinical trial. A substudy from the Heart Outcomes Prevention Evaluation (HOPE) trial Canada, USA, Mexico, Brazil, Argentina and 14 Western European countries. 9541 individuals. Smokers had an increased risk of stroke compared with never-smokers. The rates of stroke among former smokers were not different from those of never-smokers Feigin et al. Risk factors for SAH: an updated systematic review of epidemiological studies. Various countries around the world; 14 longitudinal and 23 case–control studies. 3936 individuals; Smoking is one of the most important risk factors of stroke Li et al. Risk factors for stroke in subjects with normal blood pressure: a prospective cohort study Sweden. 28, 449 individuals. Besides age, smoking was the risk factor that accounted for most strokes. The population-attributable risk was 39% Mannami et al. Cigarette smoking and risk of stroke and its subtypes among middle-aged Japanese men and women: the JPHC Study Cohort. 41, 282 individuals. Smoking raises risks of total stroke and SAH for men and women, and the risk of ischemic stroke, either lacunar or large-artery occlusive infarction, for men. Total stroke: 1. 27; Ischemic stroke: 1. 66 Rodgers et al. Risk factors for first-ever stroke in older people in the North East of England: a population-based study UK. 4440 individuals. Smoking is a risk factor first stroke in individuals >65 years of age Yamagishi et al. Smoking raises the risk of total and ischemic strokes in hypertensive men Japan. 3626 individuals. Smoking >20 cigarettes per day increases the risk of stroke in men, especially in hypertensives Tanizaki et al. Incidence and risk factors for subtypes of cerebral infarction in a general population: the Hisayama study; Japan; 1621 individuals. Smoking is a risk for lacunar stroke in men • • • • • • Hart et al. Comparison of risk factors for stroke incidence and stroke mortality in 20 years of follow-up in men and women in the Renfrew/Paisley Study in Scotland. 15, 406 individuals. Smoking is a strong predictor of stroke mortality and incidence≥ 20 cigarettes/day: Men: 1. 47; Women: 1. 64 Nakayama et al. Population attributable fraction of stroke incidence in middle-aged and elderly people: contributions of hypertension, smoking and atrial fibrillation. Japan 2302 individuals. Smoking increases the risk of stroke in individuals 40– 64 years of age. The risk was not statistically significant in those over the age of 65 years Jacobs et al. Cigarette smoking and mortality risk: twenty-five-year follow-up of the Seven Countries Study, Europe, USA, Japan; 12, 763 individuals Compared with never-smokers, smokers smoking ≥ 10 cigarettes/day had an increased risk of death from stroke at 25 years You et al. Risk factors for stroke due to cerebral infarction in young adults Melbourne, Australia 201 individuals. Current smoking is a risk factor for stroke in adults aged 15– 55 years. Whisnant et al. A population-based model of risk factors for ischemic stroke: Rochester, Minnesota. USA; 1444 individuals. Rochester Epidemiology Project. The risk of ischemic stroke at younger ages was greatly increased by current cigarette smoking. At older ages, risk was increased but by a lesser amount Ever-vs never-smoker Rohr et al. Traditional risk factors and ischemic stroke in young adults: the Baltimore– Washington Cooperative Young Stroke study, USA (Baltimore– Washington). 1516 individuals. Cigarette smoking is an important modifiable cause of stroke in young adults, particularly in black individuals You et al. Risk factors for lacunar infarction syndromes Australia. 203 individuals. Current smoking increases the risk of lacunar stroke. Lindenstrom et al. Lifestyle factors and risk of cerebrovascular diseases in women. The Copenhagen City Heart Study, Denmark. 7060; Cigarette smoking increases the risk of cerebrovascular disease Shaper et al. Risk factors for stroke in middle aged British men, UK. 7735 individuals. Current smokers had >two times the risk of stroke compared with men who have never smoked<20 cigarettes/day: Boysen et al. Stroke incidence and risk factors for stroke in middle-aged men in Copenhagen, Denmark. 13, 088 individuals. Smokers have three times the risk of stroke than nonsmokers at age 35 years. Abbott et al. Risk of stroke in male cigarette smokers, Honolulu. 8006 individuals, Compared with nonsmokers, cigarette smokers had two to three times the risk of thromboembolic or hemorrhagic stroke

Useful sources of information • NICE guidance http: //www. nice. org. uk/guidance/lifestyle-andwellbeing/smoking-and-tobacco • UK National Centre for Smoking Cessation and Training http: //www. ncsct. co. uk/ • Action on Smoking and Health (ASH) http: //www. ash. org. uk/ • NHS Smoke free http: //www. nhs. uk/smokefree • NHS Choices Stop Smoking website http: //www. nhs. uk/livewell/smoking/Pages/stopsmokingn ewhome. aspx

Please Help your Patients to QUIT!
- Slides: 47