Smoking Cessation training Very Brief Advice Presented by

Smoking Cessation training Very Brief Advice Presented by Julia Wolska Written by Jane Stephenson-Glynn and Julia Wolska Public Health, LBTH
Tower Hamlets • Tower Hamlets has one of the highest smoking rates in the country 22. 1% (nationally 18%) 2014 • High prevalence of smokeless tobacco users 2 • • 30% of Bangladeshi man 49% of Bangladeshi women • Shisha pipe use is increasing in young adults • Illicit tobacco is highly accessible

Tobacco use in Tower Hamlets

Chewing

Tobacco Chewing/Smokeless Tobacco Chewing tobacco • Pieces of tobacco are chewed or placed between the cheek and gum or teeth. The nicotine in the piece of chewing tobacco is absorbed through the mouth tissues Paan chewing • Can include mixture of tobacco, spices, supari (betel nuts), grated coconut wrapped in betel leaf • 20% of Tower Hamlets pop regularly use Paan • Belief that it aids digestion • Act as mouth freshener • Oral health risk – 5 time more likely to be at risk of oral cancer (Mouth Cancer Foundation 2009)

Shisha Facts • Shisha is as harmful as cigarettes. • Water does not filter out toxins. • Shisha can cause serious heart and lung diseases and cancers. • Herbal and fruit flavours mask the cancer chemicals. • Herbal shisha is as bad as tobacco shisha (due to presence of combustion products caused by burning of herbs and charcoal, responsible for lung and heart disease, and cancer).

Shisha Facts cont. • Second-hand smoke from shisha session is more damaging than passive smoke from cigarettes. • Light headed feeling is the start of carbon monoxide poisoning. • Shisha has nicotine and can lead you to smoking cigarettes. • Sharing same shisha is not safe and may spread infections like herpes.

What’s in tobacco smoke?
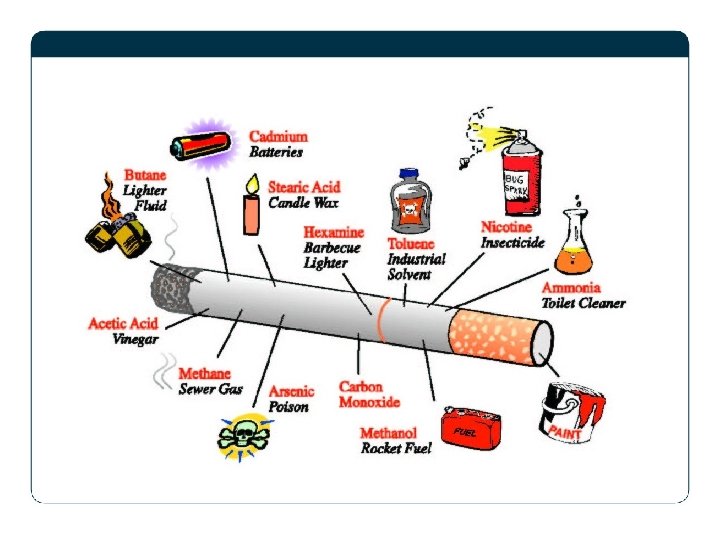

Contents of a cigarette • Lead – high blood pressure, nerve disorders, muscle pain and even fertility problems • Copper – Smokers have about twice as much of this metal in their bodies as do non-smokers. Chronic (long term) exposure can result in a build up in the kidneys, causing kidney disease • Mercury – Chronic exposure is known to cause adverse effects on mood, behaviour and memory, including irritability, tiredness, sleeplessness, tremors and damage to the nerves in the arms and legs • Aluminum – Chronic exposure can cause shortness of breath, weakness and cough • Acetone – Inhalation cause dizziness and headache

The three main components are: • Nicotine • Tar • Carbon Monoxide

Tar • The name given to all the other chemicals in the smoke particles • Linked to cancer, lung disease, heart disease and many others diseases • Approximately 4, 000 chemical compounds have been identified in cigarette smoke, of which 69 are known to cause cancer • The sticky brown substance that stains smokers’ fingers and teeth a yellowy-brown • About 70% of the tar inhaled stays in the smokers lungs • Many of the substances in tar are known to cause cancer • Irritants in tar can also damage the lungs by causing narrowing of the small tubes (bronchioles) and damaging the small hairs (cilia) that help protect the lungs from dirt and infection

Carbon Monoxide (CO) A very poisonous gas • Colourless • Odourless • Tasteless Carbon Monoxide (CO) results from: • Incomplete burning of natural gas and any carbon containing material • It is produced in car exhaust fumes, fires and from tobacco smoke

What Does CO Do to the Body? Heart: • To compensate for the shortage of oxygen, the heart has to work harder (beat faster) to get enough oxygen to all parts of the body • The heart itself gets less oxygen increasing the risk of heart damage Circulation: • CO binds much easier to Haemoglobin (Hb) in the blood than oxygen binds to Hb • The COHb causes thicker blood and the arteries get coated with a thick fatty substance • This causes circulation problems and high blood pressure, with increased risk of a heart attack and stroke • Hands and feet can become colder as less blood circulates to the extremes

What Does CO Do to the Body? Breathing: • The reduced supply of oxygen means smokers can easily get out of breath when exercising as there is little extra oxygen available for the increased demand • The lack of oxygen can also cause tiredness and lack of concentration Pregnancy: • The supply of oxygen required by the baby for healthy growth is reduced when the pregnant mother smokes

Nicotine • Nicotine is what makes smoking addictive, while carbon monoxide and tar can cause serious disease. Nicotine’s Effect on the Brain • Nicotine is not a natural substance in the body, it affects neurotransmitters in the brain • When nicotine stimulates receptors in the brain ‘feel good’ chemicals are released • Exposure to nicotine at a young age will fundamentally change the structure of the brain, resulting in an acquired drive or desire for nicotine

Withdrawal symptoms Duration Prevalence (%) Urges to smoke < 2 weeks 70% Increased appetite > 10 weeks 70% Restlessness > 4 weeks 60% Poor concentration > 2 weeks 60% Irritability/aggression < 4 weeks 50% Sleep disturbance < 1 week 25% Low mood/Depression > 4 weeks 60% Constipation >4 weeks 17% Mouth Ulcers >4 weeks 40% Light headedness < 48 hrs 10%
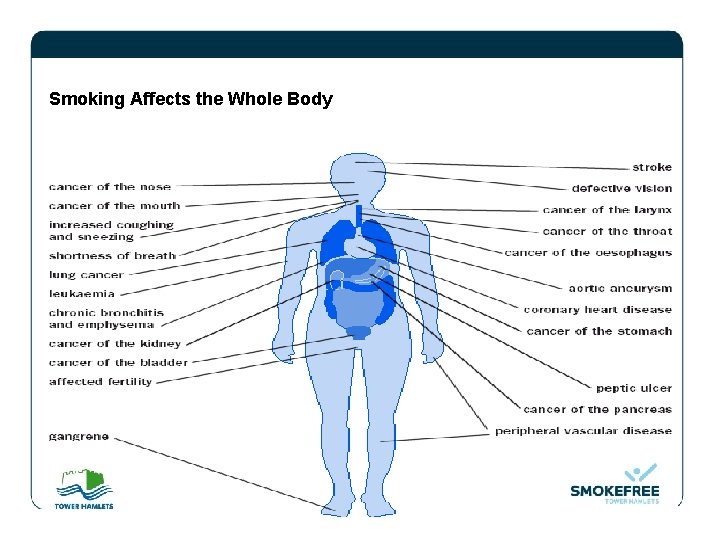
Smoking Affects the Whole Body

Diseases caused by smoking Smoking causes many serious and fatal diseases, the most common are: • Coronary heart disease • Cancer – lung, mouth, nose and throat, larynx, oesophagus, pancreas, bladder, stomach, leukaemia, kidney • Chronic bronchitis • Chronic obstructive pulmonary disease (COPD) Ø Emphysema Ø Pneumonia Others • Impotence • Peptic ulcers • Adverse effects on fertility (both men and women) • Diabetes (Type 2 non insulin dependant)

Health benefits of giving up • • Stopping smoking is the biggest single thing a person can do to improve their health Once a person stops taking in carbon monoxide, tar and the other chemicals their body can start to repair the damage done by smoking Giving up increases a persons chances of living a longer and healthier life Giving up will: Ø Reduce chances of developing cancer Ø Help breathing Ø Reduce phlegm in the lungs – cough less (eventually) Ø Improve sense of taste and smell Ø Stop hair, skin and breath smelling of smoke Ø Stop any decline in lung efficiency
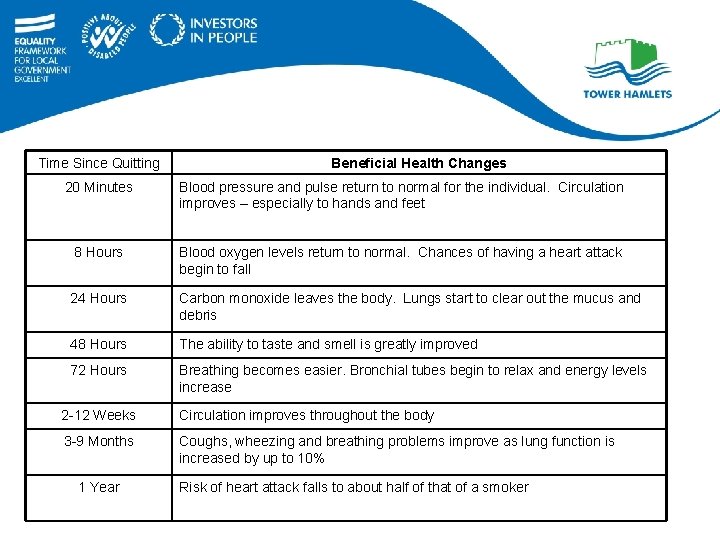
Time Since Quitting Beneficial Health Changes 20 Minutes Blood pressure and pulse return to normal for the individual. Circulation improves – especially to hands and feet 8 Hours Blood oxygen levels return to normal. Chances of having a heart attack begin to fall 24 Hours Carbon monoxide leaves the body. Lungs start to clear out the mucus and debris 48 Hours The ability to taste and smell is greatly improved 72 Hours Breathing becomes easier. Bronchial tubes begin to relax and energy levels increase 2 -12 Weeks Circulation improves throughout the body 3 -9 Months Coughs, wheezing and breathing problems improve as lung function is increased by up to 10% 1 Year Risk of heart attack falls to about half of that of a smoker

Stop Smoking Medications

NRT • Nicotine Replacement Therapy (NRT) is licensed for use in YP (12 years and up) • There are 8 different NRT products (patch, gum, inhalator, microtabs, mini lozenges, nasal spray, mouth strips) • Research shows that using NRT doubles the smokers chances of successfully stopping • NRT works by giving ‘clean’ nicotine to prevent withdrawal symptoms and gradually ‘weans’ the patient off the nicotine (as the amount of nicotine is reduced over the course of treatment)

Champix (Varenicline) • Prescription only stop smoking medicine • Very effective although not a magic pill! (will power is still essential) • Works by blocking nicotine receptors in brain – reducing addictive power of smoking and helping with cravings and withdrawal symptoms

Very Brief Advice (VBA) A simple form of advice designed to be used opportunistically in less than 30 seconds in almost any consultation with a smoker.
VBA - 3 A’s ASK ADVICE ACT

ASK - and record smoking status Do “Do you smoke? ” Don’t “Do you want to stop? ”

ADVISE “The most effective way to stop and stay stopped is with support and medication. ”

ACT On client’s response. Build confidence and refer to appropriate service.

ASK open ended questions, offer smokers opportunity to process information and decide if they are ready. ADVICE - dispel any misconceptions – shisha just as bad. Inform them that the most successful way of quitting is with support. ACT – refer them onto specialist service.

VBA for smoking cessation is about…. • Raising the issue, routinely asking smoking status • Exploring what smoking means to the individual • Enabling the smoker to believe that they could stop smoking if they choose to do so • Checking levels of knowledge and beliefs about smoking • Correcting misinformation • Giving further information, advice and support • Outlining the benefits of getting help and making quitting easier for them if they access the service • Referring to stop smoking service.

Stop smoking interventions Brief interventions: • Brief opportunistic advice provided by front line staff coming into contact with smokers • Smokers are asked about their smoking status and given relevant information • Smokers are signposted/referred to relevant stop smoking service Intermediate interventions: • Delivered by level 2 advisors • Offering one to one sessions which include preparation and setting a quit date, advice on medications, behavioural support and follow up sessions

Stop smoking interventions cont. Specialist interventions delivered by Specialist Stop Smoking Services: • Smokers with complex needs • Further support e. g. heavy smoker/one who has tried unsuccessfully to quit before • Specialist support for language/culture • 1: 1 and group sessions • Pregnant • Mental health patients • It’s also a service of choice

Our tobacco cessation services • Pharmacies – 6 weeks programme based on 1: 1 sessions • GP surgeries hosting specialist stop smoking service clinics (8 weeks programme, 1: 1 or group sessions) • Specialist service – for those who need more intensive support, 1: 1 and group sessions • Pregnancy service • BME Tobacco Project

Local Stop Smoking Services Contact Details Specialist smoking cessation service Service of choice and also for patients with further needs, e. g. mental health, COPD, heavy smokers. Tel: 0800 169 1943 or 020 7882 8230 Fax: 020 7791 1774 E-mail: BHNT. smokersclinic@nhs. net

Local Stop Smoking Services Contact Details Specialist Pregnancy Service Tel: 0800 169 1943 or 020 7882 8230 Fax: 020 7791 1774 E-mail: BHNT. smokersclinic@nhs. net

Local Stop Smoking Services Contact Details BME Stop Tobacco Project Offers culturally sensitive advice for the Black and Minority Ethnic community who smoke cigarettes or chew paan with tobacco. Both male and female specialist advisers are available and clients can be seen in a number of venues. Tel (men): 020 7882 8660 Tel (women): 020 7882 8669 E-mail: bhnt. bstp@nhs. net Fax: 020 7791 1774

Your role • Providing high quality Very Brief Advice on benefits of stopping smoking and the most effective way to stop and stay stopped, which is with support and medication • Recording smoking status in the Lifestyle Intervention template, incl. taking CO reading (as a motivational tool) • Actively referring, if appropriate, via referral on EMIS web

Further training, reading and resources Training: VBA- online training : National Centre for Smoking Cessation and Training – Its free and covers 2 subjects: how to offer brief smoking cessation support & the effects of passive smoking http: //elearning. ncsct. co. uk/vba-launch & http: //elearning. ncsct. co. uk/shs_vba -launch Advisor training http: //www. ncsct. co. uk/training-and-assessment National Centre for Smoking Cessation and Training – covers higher level training on becoming a stop smoking practitioner. All courses are Department of Health accredited and you will gain a certificate for each upon completion. Free stop smoking resources: http: //smokefree. nhs. uk/resources/ http: //www. orderline. dh. gov. uk/ecom_dh/public/home. jsf

LBTH Public Health Tobacco Control Team Jane Stephenson-Glynn Jane. stephenson-glynn@towerhamlets. gov. uk Public Health Strategist/Programme Manager 0207 092 7537 Julia Wolska Julia. wolska@towerhamlets. gov. uk Public Health Advisor 0207 092 7387 Mutiur Rahman Mutiur. rahman@towerhamlets. gov. uk Public Health Advisor 0207 092 7385
- Slides: 40