PHM 456 Common Infectious Diseases of Childhood James







































- Slides: 41

PHM 456 Common Infectious Diseases of Childhood James Tjon, BSPhm, Pharm. D, RPh Department of Pharmacy The Hospital for Sick Children October 21, 2004

Objectives Review the epidemiology, etiology, pathophysiology, clinical presentation, treatment and prevention associated with the following pediatric infectious diseases: Ø Croup Ø Pertussis Ø Bronchiolitis Ø

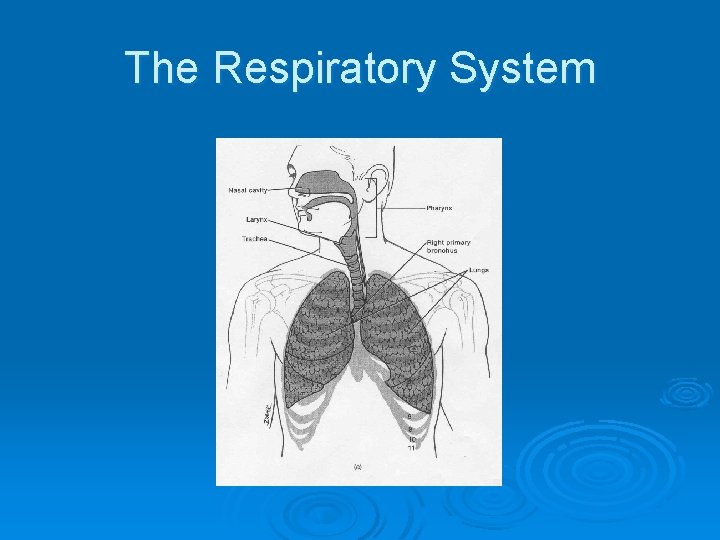
The Respiratory System

Croup Ø 4 different classifications of Croup Syndrome: l l Laryngotracheitis Spasmodic Bacterial tracheitis Epiglottitis

Croup Ø Definition Involves inflammation and edema of the larynx, subglottic tissues and trachea, causing airway obstruction and is due to an infectious agent

Croup Ø Epidemiology l l l > 15% of respiratory tract disease in pediatric practice Age: 6 months to 3 years Peak age: 2 years More common in boys Late fall and winter

Croup Ø Microbiology l l l Primarily viral Parainfluenza (types 1, 2 & 3) Influenza A & B Adenovirus, Respiratory Syncytial Virus (RSV), measles Bacterial

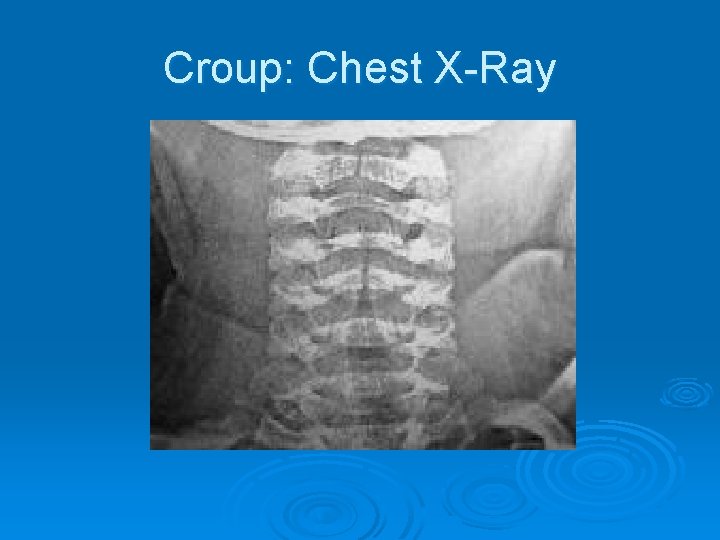
Croup Ø Pathophysiology l l Begins in nasopharynx Spreads to larynx and trachea Inflammation, erythema and edema in trachea Subglottic area is major site of airway obstruction

Croup: Chest X-Ray

Croup Ø Clinical Presentation l l l l Gradual onset Duration normally 5 days Low grade fever Classic “barking” cough Hoarse voice Stridor Dyspnea Sore throat

Croup Ø Clinical Presentation l l Worsening of breathing difficulty Cyanosis Difficulty swallowing Possible hospital admission

Croup Ø Treatment l l Cold air Humidified air • cool mist vaporizer • steamy bathroom • humidified oxygen l Croup tents


Croup Ø Treatment l Epinephrine • anti-inflammatory activity decreases subglottic edema • can improve stridor, decrease need for hospitalization & intubation and decrease mortality rates • onset: 10 to 30 minutes • duration of effect: 2 hours

Croup Ø Treatment l Racemic epinephrine inhalation • Dose: 0. 5 m. L of 2. 25% solution in 3 m. L 0. 9% Na. Cl q 1 -2 h up to q 20 minutes l l-epinephrine inhalation • • • l 1: 1, 000 solution (1 mg/m. L) dose: 2 -5 m. L q 1 -4 hours as effective as racemic epinephrine Side effects

Croup Ø Treatment l • Corticosteroids (moderate-severe Croup) Dexamethasone 0. 6 mg/kg IV/IM x 1 • oral versus parenteral • Budesonide inhalation • strong topical effects with low systemic activity • 2 mg x 1, repeated q 12 -24 h prn

Croup: Canadian Study N Engl J Med 2004; 351: 1306 -13 Ø Randomized, double-blind, multi-centre study (n= 720 children, mild Croup) Ø Dexamethasone 0. 6 mg/kg oral or placebo Ø Primary & secondary outcomes Ø Dexamethasone effective treatment for mild Croup Ø

Pertussis Whooping cough syndrome Ø 100 Day Cough Ø “Intense cough” Ø Epidemiology Ø l l l Seasonal, fall and winter Transmission by coughing All ages, 60% under 5 years

Pertussis Ø Microbiology l l Bordetella pertussis Bordetella parapertussis, Bordetella bronchiseptica, adenovirus

Pertussis Ø Pathophysiology: l l l Inhalation of organism Adherence to ciliated cells Proliferation and spread Paralysis of cilia Production and accumulation of mucous Possible progression to pneumonia

Pertussis Ø Complications l l l Hospitalization Pneumonia Central nervous system • encephalopathy • seizures l Mortality

Pertussis Complications by Age *Cases reported to CDC 1997 -2000 (N=28, 187)

Pertussis Ø Treatment • Supportive • oxygen • suctioning • Antibiotics

Pertussis Ø Antibiotics l l Erythromycin estolate 40 mg/kg/day po QID x 10 -14 days Clarithromycin 15 mg/kg/day po BID X 10 days Azithromycin 10 mg/kg/day po x 1 day, then 5 mg/kg/day po daily x 4 days Cotrimoxazole 8 mg TMP /kg/day po BID

Pertussis: Canadian Study Pediatrics 2004; 114(1): e 96 Ø Randomized, multi-centre study comparing azithromycin and erythromycin estolate (n=477, 6 months - 16 years) Ø Outcomes: bacterial cultures, serology & PCR, ADRs, compliance and symptoms Ø As effective, fewer ADRs & good compliance Ø

Pertussis Ø Prevention l l l Highly communicable Household contacts Same drugs as for treatment

Pertussis Ø Prevention l l l Acellular pertussis vaccine (DTa. P) Part of routine immunization schedule: Administration: 2, 4, 6 and 18 months with booster at 4 to 6 years

Bronchiolitis Ø Definition: acute respiratory illness resulting from inflammation of small airways, characterized by wheezing and caused by viral infection

Bronchiolitis Ø Epidemiology l l l Young children Peak incidence between 2 to 6 months Winter and early spring

Bronchiolitis Ø Microbiology l l l Respiratory syncytial virus (RSV) Parainfluenza Influenza A & B Adenoviruses Transmission by direct contamination

Bronchiolitis Ø Pathophysiology l l l Viral replication in bronchioles Necrosis of ciliated cells Increased mucous secretions Bronchial plugging with obstruction Hypoxia

Bronchiolitis Ø Clinical Presentation l l l Fever Nasal discharge Dry cough Wheeze Usually self-limiting Asthma, pneumonia, CHF, cystic fibrosis

Bronchiolitis Ø Progression l l l Risk factors Tachypnea Irregular breathing Cyanosis or pallor Apnea Mortality

Bronchiolitis Ø Treatment l Supportive • • • l oxygen hydration suctioning Inhaled beta-agonists (salbutamol) • controversial l Racemic or l-epinephrine • vasoconstricts mucosa to reduce edema

Bronchiolitis Ø Treatment l Corticosteroids • oral versus inhaled l Ribavirin • controversial • modest clinical benefit • no effect on hospital stay

Bronchiolitis Ø Prevention l Passive immunization • given monthly through RSV season • RSV Immune Globulin (RSVIVIG, Respigam): blood product l Palivizumab • monoclonal antibody • IM injection monthly during RSV season • costly

Bronchiolitis Ø Palivizumab (Synagis®) l l l Approved in Canada in June of 2002 Formerly required Special Access Programme authorization Manufacturer: Med. Immune Inc. Distributor: Abbott Laboratories Funding provided by Canadian Blood Services (CBS) if patients meet high risk criteria

Bronchiolitis Ø Palivizumab Criteria l l Children < 24 months of age with BPD/CLD and who have required oxygen or medical treatment within 6 months of RSV season Premature infants born at 32 weeks gestation and aged 6 months at start of RSV season Children < 24 months of age with hemodynamically significant heart disease Other: 33 -35 week gestation infants at risk, immune deficiency Canadian Paediatric Society Guidelines

Bronchiolitis Ø Prevention l Active immunization • RSV vaccine • Being researched

Pediatric Infectious Disease References Ø Red Book Ø http: //www. cps. ca Ø The Hospital for Sick Children Formulary Ø Pediatric Dosage Handbook Ø Infectious Diseases Handbook Ø Nelson’s Pocket Book of Pediatric Antimicrobial Therapy Ø Nelson Essentials of Pediatrics

QUESTIONS?