Characterizing viral load burden among HIV positive women

Characterizing viral load burden among HIV -positive women around time of delivery: Findings from four tertiary obstetric units in Gauteng, South Africa Faith Moyo

Conflict of Interest No disclosure

Acknowledgements • • • Paediatric HIV Surveillance group § NICD: Prof Gayle Sherman, Dr Ahmad Haeri Mazandarani, Dr Tendesayi Kufa, Sr Moipone Piliso, Ms Aurélie Mukendi, Dr Tanya Murray, § NHLS: Prof Sergio Carmona Charlotte Maxeke Johannesburg Academic Hospital – Sr Lerato Mthombeni, Sr Beverley Letsoalo, Dr Coceka Mnyani, Dr Natalie Odell, Prof Mphele Mulaudzi Chris Hani Baragwanath Academic Hospital – Sr Ntaoleng Moreko, Rebecca Kgame, Prof Yasmin Adam, Dr Vuyelwa Baba, Dr Firdose Nakwa, Dr Alison van Kwawegen Kalafong Provincial Tertiary Hospital – Sr Nkele Selepe, Sr Khensani Phelane, Dr Felicia Molokoane, Dr Valerie Vannevel, Dr Khomotso Masemola, Dr Derisha Pillay, Dr Marike Boersema, Prof Nicolette du Plessis, Dr Khosi Ngobese Rahima Moosa Mother and Child Hospital – Prof Karl-Günter Technau, Sonjiha Khan, Lebo Phakathi Funding: -This project is made possible thanks to Unitaid’s support through a grant to CHAI/UNICEF. Unitaid accelerates access to innovation so that critical health products can reach the people who most need them.

Background: PMTCT in South Africa • 1 in 3 pregnant women in South Africa is HIV-positive • Antiretroviral therapy (ART) initiation rate amongst antenatal clinic clients is >95% in the public health sector • VL suppression rates in HIV-positive, pregnant and post partum women are not well documented ◦ Maternal & neonatal health • Maternal VL suppression critical to: ◦ MTCT of HIV ◦ Maternal & neonatal death
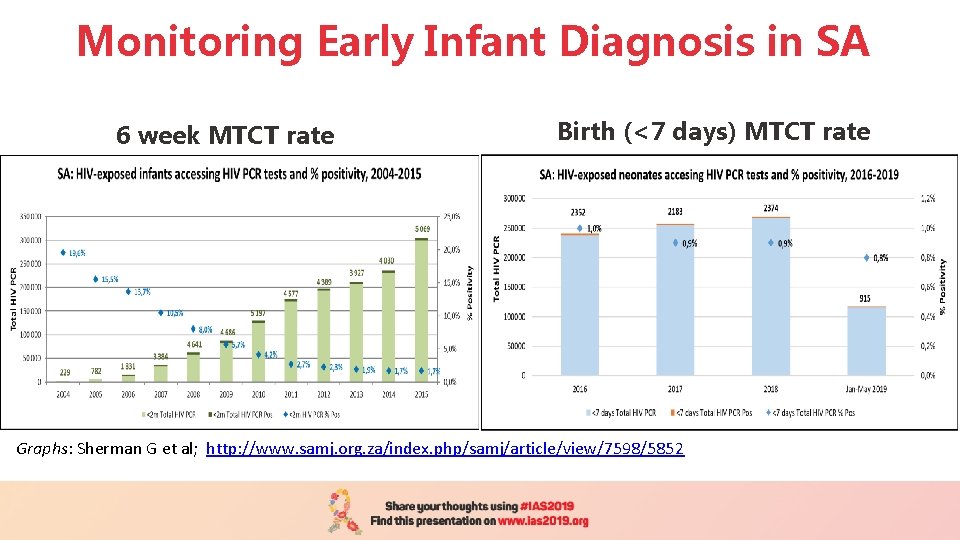
Monitoring Early Infant Diagnosis in SA 6 week MTCT rate Birth (<7 days) MTCT rate Graphs: Sherman G et al; http: //www. samj. org. za/index. php/samj/article/view/7598/5852

Road to e. MTCT in South Africa • Number of women conceiving on ART increasing -universal test & treat strategy • IU transmission rate <1. 0% – Equates to 247 cases/100 000 live births (WHO e. MTCT target = <50 cases/100 000 live births or <5% in breastfeeding populations) • e. MTCT efforts challenged by: o Poor VL monitoring in pregnancy & postpartum Global Plan towards the Elimination of New HIV Infections among Children by 2015 and Keeping Their Mothers Alive. -limited information on VL suppression rates among pregnant and breastfeeding HIVpositive women o High rates of seroconversion in pregnancy & during breastfeeding

Potential e. MTCT Game Changers: Point of Care HIV VL & EID testing • Centralized routine laboratory HIV VL & EID testing remains standard of care in South Africa • Point of care (Po. C) HIV VL (for mothers) & EID (for infants) testing have potential to: – ↓ result turn-around times & ↑ result return-rate – ↑ interventions to improve viral suppression and early ART initiation/initiate high risk infant prophylaxis

Study Objective To describe maternal VL burden and intra-uterine transmission rates among HIV-positive pregnant women and their HIV-exposed neonates using Po. C testing around time of delivery at four tertiary obstetric units in Gauteng, South Africa

Methodology • Study sites: 4 tertiary obstetric units in Gauteng province – (3 Johannesburg sub-districts and 1 in Tshwane Metro) • Study period: June 2018 -Mar 2019 • Specimen handling: – Specimen collection performed by doctors & nurses as part of routine care – Testing conducted by Po. C operators (mostly nurses) on weekdays, between 08 h 00 -16 h 00
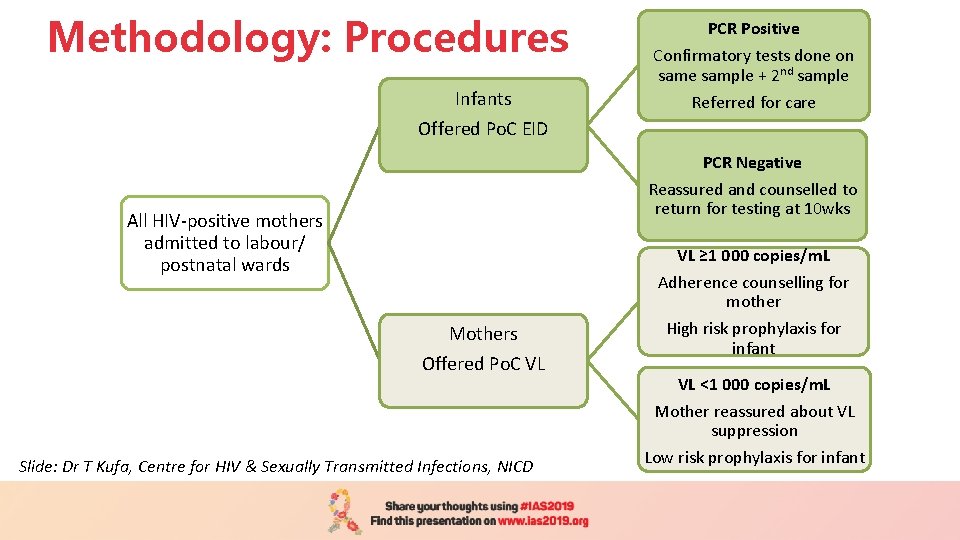
Methodology: Procedures Infants PCR Positive Confirmatory tests done on same sample + 2 nd sample Referred for care Offered Po. C EID All HIV-positive mothers admitted to labour/ postnatal wards PCR Negative Reassured and counselled to return for testing at 10 wks VL ≥ 1 000 copies/m. L Adherence counselling for mother Mothers Offered Po. C VL Slide: Dr T Kufa, Centre for HIV & Sexually Transmitted Infections, NICD High risk prophylaxis for infant VL <1 000 copies/m. L Mother reassured about VL suppression Low risk prophylaxis for infant
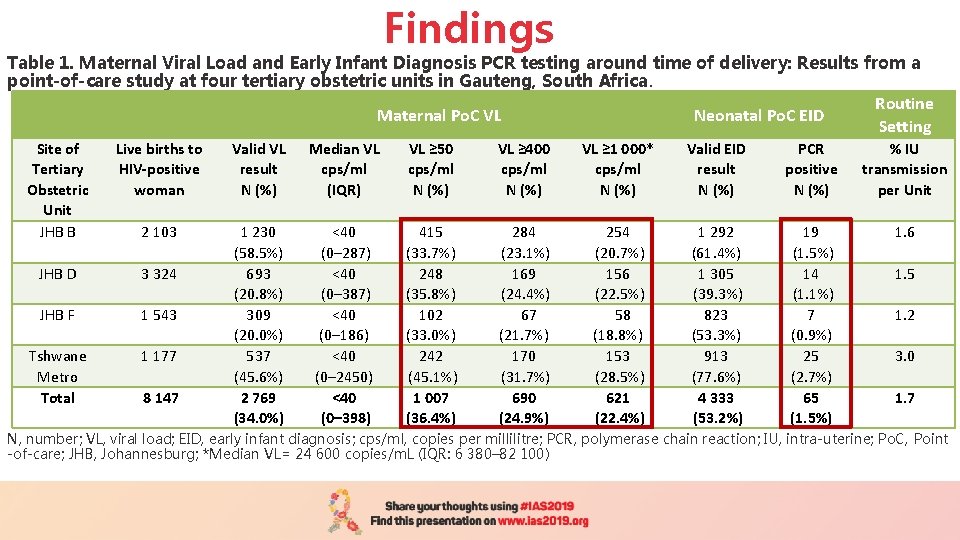
Findings Table 1. Maternal Viral Load and Early Infant Diagnosis PCR testing around time of delivery: Results from a point-of-care study at four tertiary obstetric units in Gauteng, South Africa. Maternal Po. C VL Neonatal Po. C EID Routine Setting Site of Tertiary Obstetric Unit JHB B Live births to HIV-positive woman Valid VL result N (%) Median VL cps/ml (IQR) VL ≥ 50 cps/ml N (%) VL ≥ 400 cps/ml N (%) VL ≥ 1 000* cps/ml N (%) Valid EID result N (%) PCR positive N (%) % IU transmission per Unit 2 103 3 324 JHB F 1 543 Tshwane Metro Total 1 177 <40 (0– 287) <40 (0– 387) <40 (0– 186) <40 (0– 2450) <40 (0– 398) 415 (33. 7%) 248 (35. 8%) 102 (33. 0%) 242 (45. 1%) 1 007 (36. 4%) 284 (23. 1%) 169 (24. 4%) 67 (21. 7%) 170 (31. 7%) 690 (24. 9%) 254 (20. 7%) 156 (22. 5%) 58 (18. 8%) 153 (28. 5%) 621 (22. 4%) 1 292 (61. 4%) 1 305 (39. 3%) 823 (53. 3%) 913 (77. 6%) 4 333 (53. 2%) 19 (1. 5%) 14 (1. 1%) 7 (0. 9%) 25 (2. 7%) 65 (1. 5%) 1. 6 JHB D 1 230 (58. 5%) 693 (20. 8%) 309 (20. 0%) 537 (45. 6%) 2 769 (34. 0%) 8 147 1. 5 1. 2 3. 0 1. 7 N, number; VL, viral load; EID, early infant diagnosis; cps/ml, copies per millilitre; PCR, polymerase chain reaction; IU, intra-uterine; Po. C, Point -of-care; JHB, Johannesburg; *Median VL= 24 600 copies/m. L (IQR: 6 380– 82 100)

Discussion • ≈20% of women delivering across the four obstetric units had a VL ≥ 1 000 cps/m. L; 36% had a VL ≥ 50 cps/m. L – e. MTCT requires VL suppression throughout pregnancy, postpartum and during breastfeeding in HIV-positive women • Tshwane site had higher proportions of viraemic women at delivery compared to Johannesburg sites (p=0. 001). A similar trend was observed for % neonatal positivity – Suggesting the Tshwane site had a higher MTCT-risk maternal population • % IU transmission rates ≈ programmatic IU transmission rates, overall and by site – Suggesting representativity of study population despite low coverage

Concluding Remarks • High maternal VL burden around time of delivery across multi-site tertiary obstetric units in Gauteng province, South Africa • Scale-up of VL monitoring and improving quality of ante- and postnatal care is urgently required for VL suppression around time of delivery and postpartum in breastfeeding populations for e. MTCT
- Slides: 13