ANIMAL HUSBANDRY PROJECT Europe Aid125672CSERCY Animal Health and

ANIMAL HUSBANDRY PROJECT Europe. Aid/125672/C/SER/CY Animal Health and Infectious Diseases Prevention MVDr. J. Holejšovský Ph. D. Czech University of Life Sciences Prague Institut Tropics and Subtropics Lefcosa/Nicosia June 2009

PART TWO D DANGEROUS INFECTIOUS ANIMAL DISEASES ZOONOSIS

ZOONOSIS What’s Zoonosis ? Zoonosis is an infection or infestation shared in nature by humans and animals. Zoonoses- transmission of the infectious agent to humans from an ongoing reservoir life cycle in animals, without the permanent establishment of a new life cycle in humans. Animals raised on farms that are well managed (good housing, hygienic conditions , and balanced diet) on most occasions are free of zoonotic diseases that occur naturally in animals

ZOONOSIS Zoonotic agents (bacteria, viruses, and parasites) • Zoonotic agents prevalent in many animal operations (1 -50%) – – – Salmonella Campylobacter Listeria monocytogenes – Clostridial spp. – Path. Escherichia coli – Cryptospordia • Zoonotic agents prevalent in few animal operations (< 5%) – Leptospira – Coxiella brunetii • Zoonotic agents ALMOST non existent in animal operations – Brucella spp. – Tuberculosis

Waterborne Zoonoses Pathogens • Cryptosporidium • Giardia • E. Coli 0157: H 7 • Salmonella • Leptospiria • Toxoplasma • Campylobacter • Entamoeba • Ascarsis • Viruses and Prions? SARS?

Most Common Foodborne Pathogens • Campylobacter • Salmonella • E. coli 0157: H 7 • Yersinia • Listeria • Cryptosporidium • Cyclospora • Norwalk-like viruses
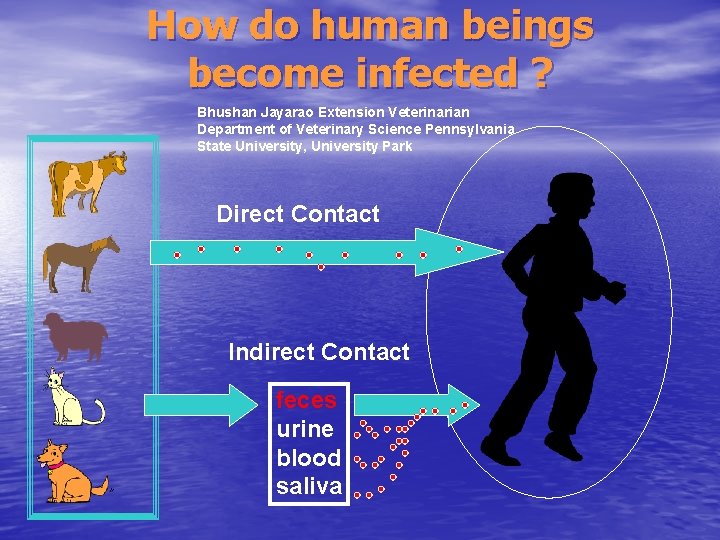
How do human beings become infected ? Bhushan Jayarao Extension Veterinarian Department of Veterinary Science Pennsylvania State University, University Park Direct Contact Indirect Contact feces urine blood saliva

Horses, asses, zebras (Equidae) • Actinobacillus spp. • Anthrax • Brucellosis • Cryptosporidiosis • Equine morbillivirus • Glanders • Leptospirosis • Rabies • Salmonellosis • Yersiniosis Bhushan Jayarao Extension Veterinarian Department of Veterinary Science Pennsylvania State University, University Park

Cats • • • Afipia felis Anthrax Bartonella (Rochalimaea) henselae Bergeyella zoohelcum Brucella suis Campylobacteriosis Capnocytophaga canimorsus CDC group NO-1 Chlamydia psittaci (feline strain) Cowpox Cutaneous larva migrans Dipylidium caninum • Leptospirosis • Neisseria canis • Pasteurella multocida • Plague • Poxvirus • Q-fever • Rabies • Rickettsia felis • Salmonellosis • Scabies • Sporothrix schenckii • Trichinosis • Toxoplasmosis • Visceral larva migrans • Yersinia pseudotuberculosis

Sheep and Goats • • Leptospirosis Louping ill Orf Q-fever Rabies Salmonellosis Yersinia enterocolitica • • • Actinobacillus spp. Anthrax Brucellosis Campylobacteriosis Chlamydia trachomatis (ovine) Cryptosporidiosis European tick-borne encephalitis Francisella tularensis Giardiasis

Dairy Cattle • • Actinomyces pyogenes Anthrax Brucellosis Campylobacteriosis Cowpox Cryptosporidiosis E. coli O 157: H 7 European tick-borne encephalitis • • • Foot and mouth disease Giardiasis Leptospirosis Mycobacterium bovis Pseudocowpox Q-fever Rabies Salmonellosis Strep. zooepidemicus Taenia saginata Yersinia enterocolitica

Swine • • • Anthrax Ascaris suum Botulism Brucella suis Cryptosporidiosis Entamoeba polecki Erysip. rhusiopathiae Flavobacterium Influenza Leptospirosis Pasteurella aerogenes Pasteurella multocida Pigbel Salmonella cholerae-suis • Salmonellosis • Sarcosporidiosis • Scabies • Strep. dysgalactiae (group L) • Streptococcus milleri • Strep. suis type 2 (group R) • Swine vesicular disease • Taenia solium • Trichinella spiralis • Yersinia enterocolitica • Yersinia pseudotuberculosis

Diseases Acquired From Rabbits and Hares • Brucella suis biotype 2 • Cheyletiella infestation • Francisella tularensis • Plague • Q-fever • Trichophyton mentagrophytes
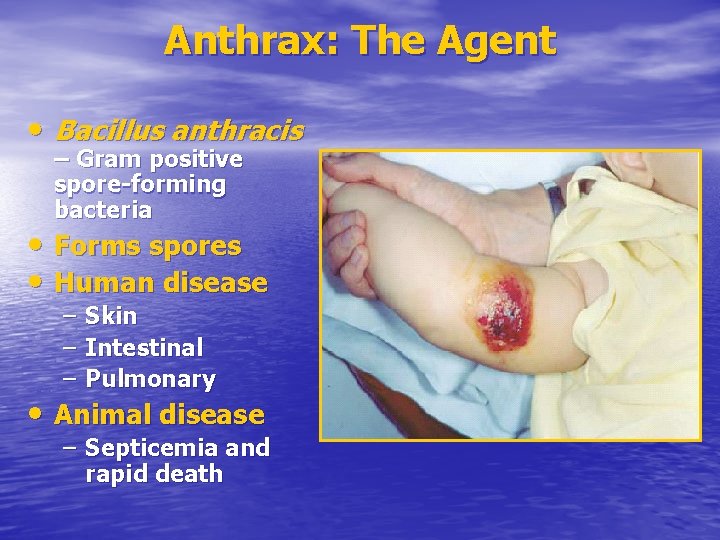
Anthrax: The Agent • Bacillus anthracis – Gram positive spore-forming bacteria • Forms spores • Human disease – – – Skin Intestinal Pulmonary • Animal disease – Septicemia and rapid death
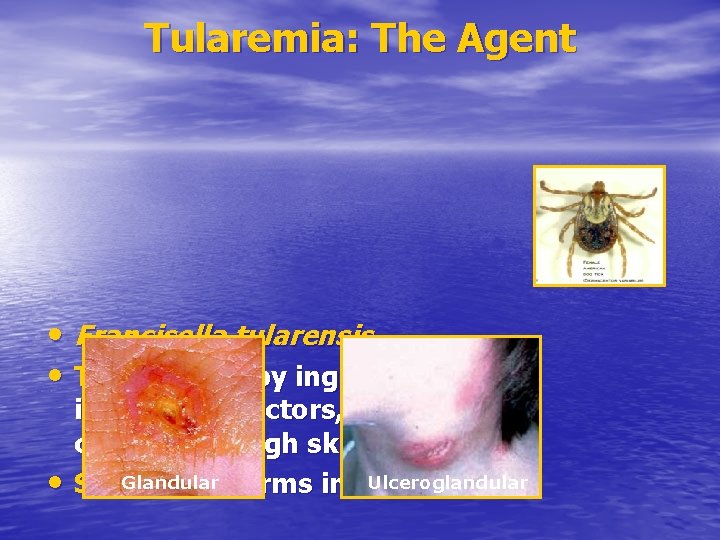
Tularemia: The Agent • Francisella tularensis • Transmitted by ingestion, • inhalation, vectors, direct contact through skin Ulceroglandular Six Glandular clinical forms in humans

Tularemia: The Agent • Sheep, young pigs, horses, dogs, cats • Sudden fever, lethargy, stiffness, prostration, and death • Wildlife • Usually find dead • Rabbits behave strangely • Cattle, older pigs resistant

Brucellosis: The Agent • Gram-negative bacteria • Ingestion, inhalation, or direct contact • Clinical signs – Humans: cyclic fever and flu-like symptoms – Animals: reproductive signs

Brucellosis: The Agent Species Natural Host Human Pathogen B. abortus Cattle, bison, elk, horses Yes B. melitensis Goats, sheep, cattle Yes B. suis Swine, hares, reindeer, caribou, rodents Yes B. canis Dogs, other canids Yes B. ovis Sheep No

Glanders: The Agent • Burkholderia mallei: Gram • negative Transmission by ingestion, inhalation, or direct contact – Animal-to-human transmission is inefficient • Clinical signs – Humans & horses: cutaneous & pulmonary lesions, rapidly fatal illness

Rabies Common Carriers Cats Dogs Raccoons Skunks Bats Foxes
Rabies Transmission • Animal Bite • Contact with infected tissue, fluids or feces Clinical presentation • • • Fever Headache Agitation Confusion Seizures Excessive salivation

Psittacosis Common Carriers Pigeons Parrots Turkeys Parakeets

Psittacosis Transmission • Inhalation from • • • infected birds Carcasses Secretions Contaminated facilities Clinical presentation • Fever • Headache • Pneumonia

Toxoplasmosis Common carriers Cats Sheep

Toxoplasmosis Transmission • Ingestion of Clinical Presentation • Fever infected meats • Swollen nodes • Abortion • Fecal contaminated • Still-birth soil • Mental retardation

Scabies Common Carriers Dogs Raccoons
Scabies Transmission Clinical presentation • Direct contact with • Itching skin lesions infected animals

Brucella sp. Primarily affects people who work with animals or animal products (slaughterhouse workers, veterinarians, farmers, dairy workers) Four different species of Brucella are known to infect humans

Brucella reservoir Species Animal reservoir B. abortus Cattle B. canis Dogs B. suis Swine B. melitensis Goats and sheep
Morphology & physiology Fastidious & aerobic Facultative intracellular Gram negative non motile cocobacilli

Brucellosis in animals Transmitted by contact with infected tissue or milk (oral, aerosol or abrasion) Predilection for erythritol rich organs (breast, uterus, epididymis, ect. ) Abortions, mastitis and sterility

Brucellosis in humans Skin abrasion, conjunctivae, inhalation or ingestion Engulfed by neutrophils and monocytes (resistant to killing) Localize regional lymph nodes Infect phagocytic cells in the RE system and form granulomas

Symptoms Aches, chills, fever (undulating) Drenching sweating Fatigue, myalgia, muscle weakness Relapse common

Diagnosis Symptoms and history Blood culture on enriched media (slow: 4 -6 weeks) Organisms grow very slowly (6 weeks) Serology (titer >640) Skin test with brucellergin - delayedtype

Treatment Prolonged use (several months) of rifampin with tetracycline or streptomycin

Escherichia coli O 157: H 7 • Bacteria: Facultative anaerobic, motile or nonmotile GNR • Source: Intestines of animals and poultry • Illness: Hemorrhagic colitis (HC), hemolytic uremic syndrome (HUS), thrombotic thrombocytopenic purpura (TTP) • Symptoms: (HC) diarrhea & vomiting, HUS) diarrhea & acute renal failure, TTP) diarrhea, GI hemorrhage, blood clots in brain

Escherichia coli O 157: H 7 • Foods: Meat, poultry, potatoes, raw milk • Transmission: Cross-contamination, sewage pollution of coastal waters • Control: Proper cooking, temperature control, preventing cross-contamination, proper personal hygiene

Salmonella spp. • Bacteria: Facultative anaerobic, motile, GNR • Source: Intestine of mammals, birds, amphibians and reptiles • Illness: Infection (gastroenteritis) • Symptoms: Nausea, vomiting, abdominal cramps, fever

Salmonella spp. Foods: Poultry, poultry salads, meats, dairy products, egg products Transmission: Cross-contamination, human contamination, sewage pollution of coastal waters Control: Proper cooking, temperature, preventing cross-contamination, personal hygiene

How does Salmonella gain access to a farm ? Most important sources of infection Replacement heifer/ cows birds /pests Bhushan Jayarao Extension Veterinarian Department of Veterinary Science Pennsylvania State University, University Park calves feed trucks water visitors

Personal hygiene practices on farm for preventing illnesses Wash hands with soap and water before and after: 1. Attending sick animals 2. Handling animals 3. Manure handling Dress and boots 1. 2. 3. 4. Change into farm boots on the farm Wash farm boots regularly Leave farm boots on the farm Wash and disinfect farm clothes IF available: shower before leaving the farm Avoid drinking and eating on animal Bhushan Jayarao Extension Veterinarian housing units Department of Veterinary Science Pennsylvania State University, University Park

Agents of Bioterrorism
- Slides: 42

































































