9102021 0 Investigations Unit Fraud Awareness 9102021 1




























- Slides: 30

9/10/2021 0

Investigations Unit Fraud Awareness 9/10/2021 1

Session Outline 9/10/2021 n About Fraud n Types of Fraud n Motives n Compensation Claims n Risk Indicators n Community Sourced information n Code of Conduct n Confidentiality n Response to members n Emerging areas of risk 2

What is Fraud? “Telling lies or being dishonest with the intent to obtain a benefit that you are not entitled to. ” Make false statement with intent to obtain financial advantage 178 BB Crimes Act 40/1900 – NSW 9/10/2021 3

What’s wrong? ? 9/10/2021 4

What’s Wrong? ? 9/10/2021 5

Why should you be aware of Fraud? Fraud accounts for nearly 20% of all reported crime in this country; OR 5. 8 Billion Dollars Around 10% of all general insurance claims are estimated to be fraudulent (ICA) - Insurance Council of Australia Industry estimates of PHI fraud are believed to be between 1 -3% but there are no accurate figures 9/10/2021 6

Why commit Fraud? Fraud is seen as an attractive alternative to other types of crimes. The reasons include: § Socially Acceptable § Perceived Entitlement § Cheap § Little Risk of Detection § Non-Violent 9/10/2021 7

Health Insurance Fraud Different types of fraud within the Health Insurance industry: § Hospital, Ancillary, Medical benefits § Contribution § Staff 9/10/2021 8

Hospital Fraud § Upcoding § Extra nights of stay claimed § Overcharging for prostheses (not implanted) § Claiming for services for which they are not entitled § Outreach services not performed, (no physical attendance) 9/10/2021 9

Ancillary Fraud § Limit surfing § Falsifying treatment documents § Falsifying account documents § Over servicing § Padding § Collusion between Provider and Member 9/10/2021 10

Medical Fraud § Incorrect use of item numbers § Collusion with provider § Incorrect Invoicing § Treatment outside period of cover § False claims 9/10/2021 11

Contribution n Making claims knowing that contribution payments will be dishonored (direct debit, cheque, credit card) n Receiving 30% rebate knowing contribution payments will be dishonored. 9/10/2021 12

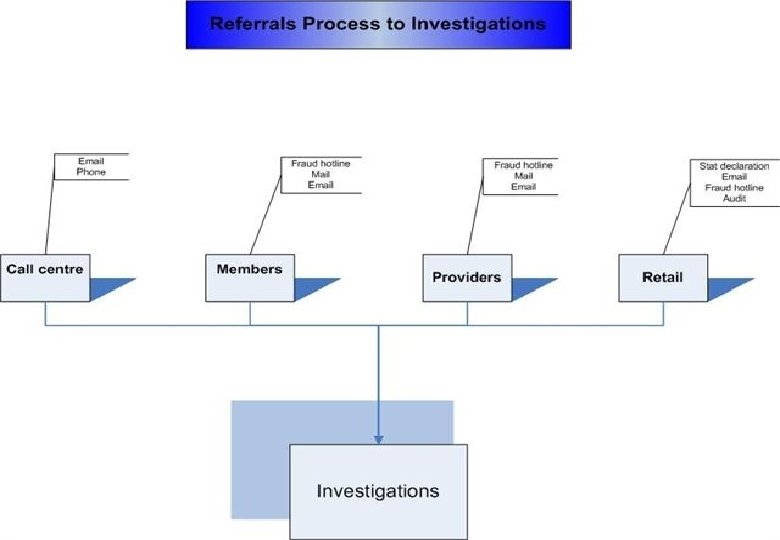
Compensation Claims n Should any information be obtained from members or other sources in relation to compensation matters being pursued by a member, this information should be relayed to the Investigations Department for follow up by our contractors. n Our contractors are: n National Health Recovery Agents - Mark Hall For Debt recovery: n Newcomen Commercial Services - Ron Stephenson n 9/10/2021 13

Staff n Making claims on receipts that are not official (made by the staff member). n Collusion with friends/family members/providers. n Changing bank account details on memberships so direct credit claims benefits will be deposited into their own account. n Knowing a staff member is committing fraud and not doing anything about it. 9/10/2021 14

Risk Indicators for suspicious claims, sometimes known as “fraud indicators” include: § Photocopied receipts § Members statements § Phone calls where member is being prompted by another person during the claims process § Members acting suspiciously during claiming § Member not willing to sign documents § Never bringing a card with them § Always reaching $300 cash limit when claiming 9/10/2021 15

Risk Indicators – Ancillary § Multiple people having same service / same day § Amount Charged the same as Benefit Paid § Limit surfing ie. , using the limits of all dependants on membership 9/10/2021 16

Risk Indicators – Hospital § Item numbers different to service provided § Item numbers not matched between hospital and specialist § Patients records don’t match care claimed (ICU) § Neonatal care claimed for well baby 9/10/2021 17

Risk Indicators – Medical § Overcharging § Service not carried out § Double charging – submitting the same account more than once § Changing item numbers so members can claim (level of cover) 9/10/2021 18

Community Sourced Information What is Community Sourced Information? § This is information which has been provided by persons alleging a suspicious event that has, may, or will occur § People provide us with information freely and we use it to assist us for investigation purposes. § Sarbanes-Oxley Act 2002 requires effective complaint management 9/10/2021 19

Community Sourced Information Why we receive Community Sourced Information § Their conscience compels them § Concern regarding the cost to the community and rising insurance premiums § Annoyed with a person/s boasting § Seeking revenge towards another person, vexatious complaint i. e. competitors § Giving the information as general interest without knowing it’s usefulness and/or relevance 9/10/2021 20

Community Sourced Information A Fraud Hotline has been established to take community sourced information nationally for NIB. 9 am – 5 pm (EST) Monday – Friday 1800 663 223 9/10/2021 21

Community Sourced Information § The email address for information is investigations@nib. com. au § Any documents or hand-written notes should be forwarded or faxed to: NIB Investigations Unit Level 2 384 Hunter Street Newcastle 2300 Fax No. 02 4927 2197 9/10/2021 22

Code of Conduct The NIB Code of Conduct states in part that “. . . employees must report any unsafe practices or suspected corrupt behavior to their manager / supervisor who will forward the report to the Investigations Department. ” 9/10/2021 23

Confidentiality All information supplied either by NIB staff or community sources is confidential. For further information please read the NIB Confidentiality Agreement published on Insite. 9/10/2021 24

Standard Response “Your claim has been selected for random review and will be forwarded to head office for processing. This is not meant to cause you any inconvenience and your claim will be processed as quickly as possible. ” Should the member or provider have any concerns, they should be referred to the NIB Investigations Unit 1800 663 233 9/10/2021 25

Emerging Areas of Risk § Ecommerce Fraud (online claims lodgments) § Identity Fraud § Expansion of electronic claiming networks 9/10/2021 26

In Conclusion Should you identify any areas of risk to the business, please report to your manager or email the NIB Investigations Unit to discuss the matter. Our commitment to you is to respond within 48 hours of your notification of any concerns. We will also keep you updated on the progress and the final result of the information supplied to the Investigations Unit. 9/10/2021 27

Case Examples Case Example 1. Chiropractor claiming benefits for services not rendered using the HICAPS facility. Provider profiling and investigation revealed in excess of $28000 in overcharging which was refunded to NIB. Case Example 2. A part time dental receptionist who was also a member of NIB was fabricating false invoices for dental treatment for both her and her husband which were not performed. Police have charged the member with numerous counts of fraud relating to the deception of NIB and other financial establishments. Over $8000 was refunded to NIB by the member. 9/10/2021 28

Question Time? ? 9/10/2021 29