Using the IBM Fraud and Abuse Management System

Using the IBM Fraud and Abuse Management System to detect suspicious healthcare claims using a shared services model Texas Technology Forum July 28, 2008 © 2008 IBM Corporation 1

AGENDA § IBM Fraud and Abuse Management System § Business Problem § Verify. NY Project § Other IBM Risk Management Solutions and Contact Information 2 © 2008 IBM Corporation

AGENDA § IBM Fraud and Abuse Management System § Business Problem § Verify. NY Project § Other IBM Risk Management Solutions and Contact Information 3 © 2008 IBM Corporation

IBM’s Fraud and Abuse Management System (FAMS) uses a scientific approach to detect suspicious claims and behaviors FAMS § Developed in 1993 with CIGNA § Specifically built for healthcare fraud and abuse detection (not retrofit from another industry) § Rich data mining and data visualization capabilities § Over 8, 500 risk indicators in the FAMS library § Over two dozen pre-built medical modules (including DME, Transportation, and Home Health Care) § Analysis is completed on peer groups (medical specialty and geography) § FAMS ranks entities (providers, institutions, etc) based on suspicious behaviors 4 © 2008 IBM Corporation

We analyze the claims data by medical specialty We have a library of over 8, 500 features, or risk indicators, specific to medical specialties § The medical models group the questions into areas for investigation or hypotheses § Sample hypotheses include: – – 5 Diagnosis Abuse Services Not Rendered Upcoding Ordered Services © 2008 IBM Corporation

Existing medical models include § Physician – – – – – Cardiology Dentist Dermatology ER Physician Gastroenterology Neurology OB/GYN Pain Management Psychology Cross Specialty/Family Practice § Pharmacy 6 © 2008 IBM Corporation § Facility –ER Hospital Facility –Inpatient Hospital –Surgical Center § Other –Ambulance –Chiropractor –DME –Home Health Care –Pathology –Patient –Physical Therapy –Radiology

AGENDA § IBM Fraud and Abuse Management System § Business Problem § Verify. NY Project § Other IBM Risk Management Solutions and Contact Information 7 © 2008 IBM Corporation
Most sources agree that approximately 10% of healthcare spending may be attributable to fraud, waste and abuse As much as 10% of all healthcare expenditures in the United States may be lost each year to fraud, abuse and waste. These same practices can be seen in the Medicaid program “…at least 10 percent of state Medicaid dollars were spent on fraudulent claims, while 20 or 30 percent more were siphoned off [by abuse]. ” 8 © 2008 IBM Corporation

The Business Problem in New York § New York State requires all of its counties to contribute to the State’s share of Medicaid expenses § In FY 2004, the State of New York spent approximately $44 Billion on Medicaid. This was more than any other state § Medicaid spend continued to accelerate resulting in higher taxes § Counties wanted to do something to address Medicaid fraud, waste and abuse 9 © 2008 IBM Corporation

AGENDA § IBM Fraud and Abuse Management System § Business Problem § Verify. NY Project § Other IBM Risk Management Solutions and Contact Information 10 © 2008 IBM Corporation

The Solution: Verify. NY § The New York State Association of Counties (NYSAC) challenged IBM to provide a solution at the county level § Verify. NY utilized IBM’s Fraud and Abuse Management System in an on demand model § The program provided the Counties with analytics to assist them in accurately verifying their Medicaid expenditures – No additional money spent on technology – No additional training of resources – No need for the Counties to hire data analysts or statisticians to do the analysis 11 © 2008 IBM Corporation
Verify. NY- Results § Twelve counties were invited to participate in the Demonstration Project § 49 peer groups analyzed Clinton § Over 500 reports delivered Saint Lawrence Franklin Jefferson Essex Lewis Hamilton Warren Oswego Herkimer Oneida Wayne Monroe Ontario Wyoming Livingston Seneca Yates Schuyler Cattaraugus Saratoga Allegany Steuben Tompkins Montgomery Schenectady Madison Cayuga Otsego Cortland Chautauqua Fulton Onondaga Genesee Erie Washington Orleans Niagara Rensselaer Schoharie Albany Chenango Greene Chemung Tioga Delaware Columbia Broome Ulster Sullivan Dutchess Putnam Orange Rockland Westchester Bronx New York Nassau Queens 12 © 2008 IBM Corporation Suffolk
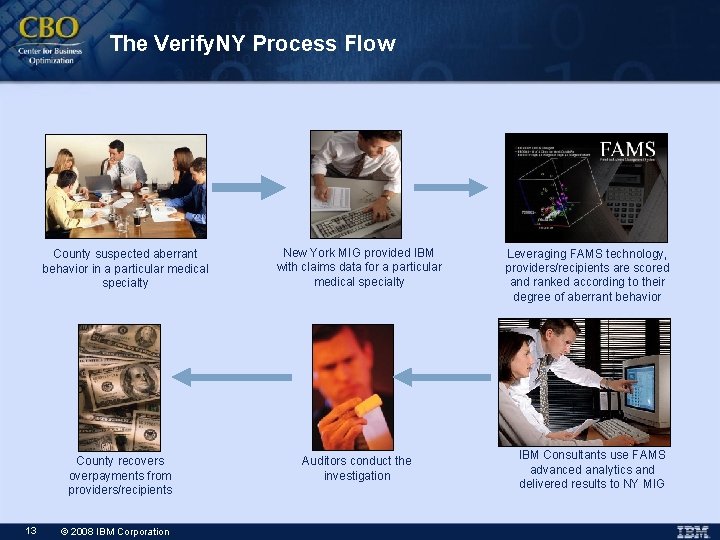
The Verify. NY Process Flow County suspected aberrant behavior in a particular medical specialty County recovers overpayments from providers/recipients 13 © 2008 IBM Corporation New York MIG provided IBM with claims data for a particular medical specialty Auditors conduct the investigation Leveraging FAMS technology, providers/recipients are scored and ranked according to their degree of aberrant behavior IBM Consultants use FAMS advanced analytics and delivered results to NY MIG

Mechanics of the Verify. NY Process Flow § New York Office of the Medicaid Inspector General provided IBM with an extract of claims data called a “Service Level Extract” for the chosen medical specialty § IBM performed a preliminary analysis to ensure that the data provided was for the specialty that the County expected § Further analysis confirmed that there were no obvious errors in data provided § Data was analyzed and reports were delivered to the County for further investigation 14 © 2008 IBM Corporation

Output provides investigators a detailed view of where the potential fraud, waste and abuse may be occurring The output is targeted at two different audiences – The Executive Summary is targeted at the Medicaid Inspector General or their Cabinet, many of whom do not have time to review the in-depth reports – Detailed reports are used by Investigators as the basis for further investigation 15 © 2008 IBM Corporation

Verify Reports Executive Summary This is a high level report targeted at the Medicaid Inspector General or their Cabinet. It provides an overview of the underlying Verify analyses For Illustrative Purposes Only 16 © 2008 IBM Corporation

Verify Reports- cont This Profile Analysis Detail Report is targeted at an investigator and gives an in-depth look at each entity analyzed. For example, this provider is submitting claims long after performing treatment. For Illustrative Purposes Only 17 © 2008 IBM Corporation

Sample press from the Verify. NY project Memo of Understanding Between IBM in conjunction with New York State Department Association of Counties is pleased to of Health I am also announce the Verify. NY solution for pleased And expendit to report Medicaid fraud detection and investigation. ures mad t h a t ____County c e o unty seve to u “ se Veri nty-fiv DOH as e percent (75%) fy. NY w ill be. DOH is the single state agency for the reimburs Whereas, a Medicaid program in New Yorkri. State ct iswitin aid admi e d expende t b y s i t h the responsibility for the proper andnt nistrativ e D d in 200 s and e of e g e expens efficient administration supervision c a 5…” i v… f r H ethe e O of if provision S ts o D Ne udi cal d the a o r L n o Now Therefore, DOH hereby d ateand _______County d i Se w n Theagree n e l a. l g i 2 o as follows: pt Yo C. by des eviews rs enr e r m e rk e r 1 t. Scope vid ion andpr. Purpose he. Section b o c e u This d agreementtis intended to set forth the r 3 Po ts o roles and responsibilities of the. WH con erespective n , 2 st m EN with respect to audits of providers. d pay iparties 00 i I enrolled the ca in the Medicaid Program and. BM AT NE d 6 e protection of the integrity of the program M GE TA RD as well as define and identify those. A areas R C E S requiring mutual cooperation in the … R ES KS K A T FR IM AU TO D 18 © 2008 IBM Corporation

Why Verify? § The Verify program is an IBM on demand offering that allows Medicaid agencies to contract for analysis of one or many medical specialties § In this model IBM consultants use advanced analytics to ferret out anomalous behavior by entities § The client receives analyses which allow investigators to focus on the most egregious offenders 19 © 2008 IBM Corporation

AGENDA § IBM Fraud and Abuse Management System § Business Problem § Verify. NY Project § Other IBM Risk Management Solutions and Contact Information 20 © 2008 IBM Corporation

The Entity Profiling Management System (EPMS) is the core of all the Risk Management Solutions IBM BEHAVIOR ANALYSIS PLATFORM DETECTION ANALYTICS HEALTHCARE INTERNAL AUDIT CUSTOMS DASHBOARD INSURANCE REPORTING FOOD COUPONS BEHAVIOR MODEL LIBRARIES 21 © 2008 IBM Corporation TAXATION

Contact Information § For further information about IBM’s Fraud and Abuse Management System, Verify or other Risk Management Solutions please contact Patreece Williams, patreece. t. williams@us. ibm. com 22 © 2008 IBM Corporation
- Slides: 22