Overview of Global Recommendations for Antenatal Care for

Overview of Global Recommendations for Antenatal Care for a Positive Pregnancy Experience Module 1 Version 2

Learning objectives By the end of this module, learners will be able to: • Recognize pregnant women in the community • Assess gestational age in pregnant women* • Educate pregnant women about the benefits of antenatal care (ANC) • Describe recommended timings for ANC visits • Enumerate the nutritional recommendations for quality ANC 1

Learning objectives, cont. • List recommended approaches for maternal and fetal assessment in pregnancy* • Describe recommended preventive measures for best pregnancy outcome • List interventions for common physiological symptoms in pregnancy* • Describe health system interventions to improve ANC utilization and quality* *Health care workers only 2

Exercise 1: How do you know that a woman is pregnant? 1. Complaints (symptoms) 2. Examination findings (signs) 3. Test results 3

1. Pregnancy symptoms/complaints • Missed period (amenorrhea) • Morning sickness (nausea/vomiting) • Fatigue or weakness • Breast changes (fullness, pain) • Urinary symptoms (increased frequency, feeling of pressure, etc. ) • Constipation • Enlarging abdomen 4

2. Signs of pregnancy (elicited during physical examination) • Uterine enlargement • Pelvic examination (before 12 weeks) • Abdominal examination (from 12 weeks) • Presence of fetal heart sounds • Detected by Doppler ultrasound from 10 – 12 weeks • Detected by fetoscope from 17– 20 weeks 5 Photo by Karen Kasmauski

2. Signs of pregnancy (elicited during physical examination), cont. • Presence of fetal movements (quickening) • Primigravida feel quickening from 18– 20 weeks • Multigravida feel quickening from 16– 18 weeks 6

3. Tests to detect pregnancy • Pregnancy tests: All pregnancy tests measure levels of circulating beta human chorionic gonadotrophins (also called pregnancy hormone) • Urine tests are qualitative and can detect pregnancy from 5– 6 weeks after last normal menstrual period (LNMP) 7

3. Tests to detect pregnancy, cont. • Blood tests are quantitative and can detect pregnancy from 6– 8 days after ovulation (before missed period) • Ultrasound scan/examination: An ultrasound scan detect an intrauterine gestational sac from 6 weeks pregnancy and detect fetal heart activity by 8 weeks 8

Benefits of ANC Photo by Emmanuel Otolorin, Jhpiego 9
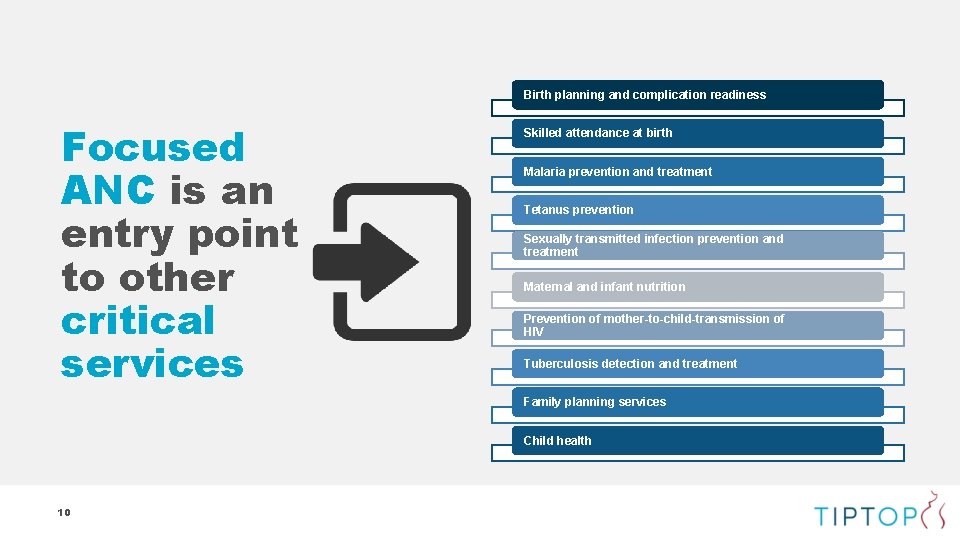
Birth planning and complication readiness Focused ANC is an entry point to other critical services Skilled attendance at birth Malaria prevention and treatment Tetanus prevention Sexually transmitted infection prevention and treatment Maternal and infant nutrition Prevention of mother-to-child-transmission of HIV Tuberculosis detection and treatment Family planning services Child health 10

Exercise 2: Why do some pregnant women fail to attend ANC clinics and/or deliver outside health facilities? • Duration: 10 minutes • Work in pairs • List five reasons why some pregnant women in your subnational area do not attend ANC clinics and/or deliver outside health facilities • Share your list with the rest of the class 11
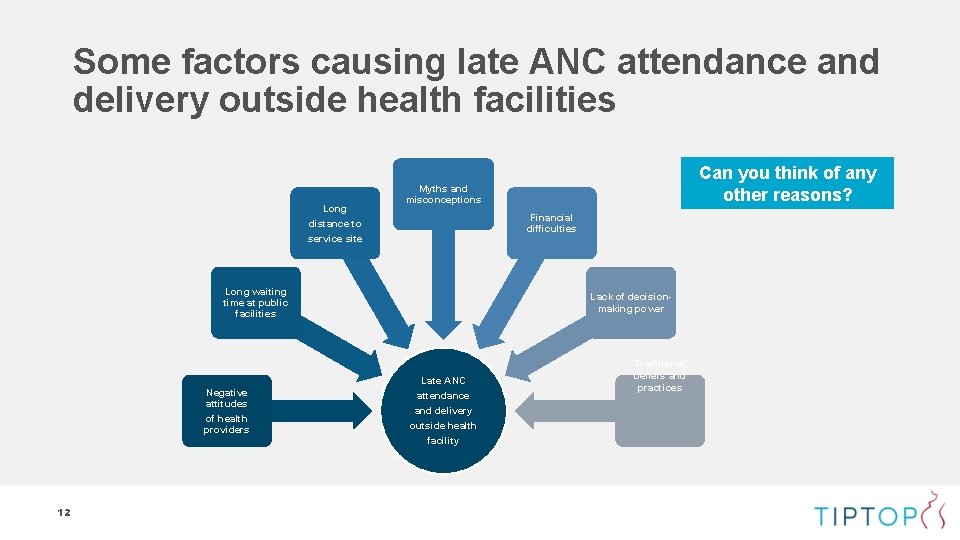
Some factors causing late ANC attendance and delivery outside health facilities Long distance to service site Myths and misconceptions Financial difficulties Long waiting time at public facilities Negative attitudes of health providers 12 Can you think of any other reasons? Lack of decisionmaking power Late ANC attendance and delivery outside health facility Traditional beliefs and practices

Therefore. . . We need to make ANC attendance a pleasurable, rewarding, assuring, empathetic experience for ALL clients 13

Women’s goals in attending ANC Women need: • Medical care • Relevant and timely information • Emotional support and advice 14 Women want a positive pregnancy experience: • A healthy pregnancy for mother and baby (including preventing or treating risks, illness, and death) • Physical and sociocultural normality during pregnancy • Effective transition to positive labor and birth • Positive motherhood (including maternal selfesteem, competence, and autonomy)

Goals of ANC • Provision of information and advice on lifestyle: • • Nutrition (balanced diet and supplements) Exclusive breastfeeding practices Exercise and sexual intercourse in pregnancy Need to avoid smoking, alcohol, use of harmful drugs, etc. • Early detection and treatment of problems and complications: • • Anemia Malaria Urinary tract infections Sexually transmitted infections including syphilis and HIV • Pre-eclampsia • Diabetes 15 • Prevention of complications and disease: • • Tetanus Malaria Severe anemia Hookworm infestation • Birth preparedness and complication readiness

New World Health Organization (WHO) recommendations for ANC 2016 16

Purpose of 2016 WHO recommendations for ANC • Put women at the center of care • Promote innovative, evidence-based approaches to ANC • Enhance the woman’s experience of pregnancy • Ensure that babies have the best possible start in life • Align with Sustainable Development Goals: expand care beyond survival • Complement existing WHO guidelines on the management of specific pregnancy complications • Promote a human rights–based approach to care 17

A. Nutritional interventions 18

Nutrition: All ANC settings Daily oral iron and folic acid (IFA): • 30 to 60 mg of elemental iron and • 400 μg (0. 4 mg) of folic acid 19

Nutrition: Context-specific Women intolerant of IFA side effects: • Intermittent oral IFA with 120 mg of elemental iron and 2, 800 μg (2. 8 mg) of folic acid once weekly Populations with low dietary calcium intake: • Daily calcium supplementation (1. 5– 2. 0 g oral elemental calcium) to reduce risk of pre-eclampsia 20

Nutrition: Context-specific, cont. Areas where vitamin A deficiency is a severe public health problem: • Vitamin A supplementation for pregnant women to prevent night blindness. • Not recommended to improve maternal and perinatal outcomes • Dose: daily up to 10, 000 IU or weekly up to 25, 000 IU vitamin A 21

B. Maternal and fetal assessment 22

Maternal and fetal assessment: All ANC settings One ultrasound scan before 24 weeks is recommended to estimate gestational age, improve detection of fetal anomalies and multiple pregnancies, reduce induction of labor for postterm pregnancy, and improve a woman’s pregnancy experience. 23

Considerations Ultrasound is recommended early (<24 weeks) • Additional scans later in pregnancy not recommended • Effects of introducing antenatal ultrasound on population health outcomes and health systems in rural, low-resource settings are unproven 24

Maternal/fetal assessment: All ANC settings, cont. • Classify hyperglycemia (high blood sugar) first detected at any time during pregnancy as either gestational diabetes mellitus (GDM) or diabetes mellitus in pregnancy, according to WHO criteria. • No recommendation for routine screening for diabetes in pregnancy 25

Maternal/fetal assessment: Context-specific Where tuberculosis prevalence is high (≥ 100/100, 000): • Consider symptomatic screening for active tuberculosis in ANC. Where abdominal palpation is used to assess fetal growth: • Not recommended to change to symphysis-fundal height measurement 26

Maternal/fetal assessment: Context-specific, cont. Where full blood count testing is not available for anemia testing: • Onsite Hb testing with a hemoglobinometer is recommended (over the Hb color scale). Where urine culture is not available for diagnosis of asymptomatic bacteriuria: • Onsite midstream urine Gram stain is recommended (over dipstick tests) 27

C. Preventive measures 28

Preventive measures: All ANC settings A 7 -day antibiotic regimen is recommended for all pregnant women with asymptomatic bacteriuria. 29

Preventive measures: Context-specific In malaria-endemic areas in Africa: • Start intermittent preventive treatment in pregnancy with sulfadoxine-pyrimethamine (IPTp with SP) in the second trimester. Give at least three doses, each 1 month apart. • IPTp can start as early as possible in the second trimester (best between 13 and 16 weeks) and then at least 1 month apart • New ANC schedule should be aligned with new approach of community-based distribution of IPTp 30

Preventive measures: Context-specific, cont. For pregnant women at substantial risk of acquiring HIV infection: * • Offer oral pre-exposure prophylaxis (Pr. EP) containing tenofovir disoproxil fumarate 31

D. Interventions for common physiological symptoms 32

Symptom Recommendation Nausea and Ginger, chamomile, vitamin B 6, and/or acupuncture for relief of nausea in early vomiting pregnancy. Advice on diet and lifestyle to prevent and relieve heartburn in pregnancy. Heartburn Antacid preparations for women with troublesome symptoms not relieved by lifestyle changes. Leg cramps Magnesium, calcium, or nonpharmacological treatment options for relief of leg cramps in pregnancy. Regular exercise throughout pregnancy to prevent low back and pelvic pain. Low back/pelvic Different treatment options can be used, such as physiotherapy, support belts, pain and acupuncture. Fiber supplements to relieve constipation in pregnancy if the condition fails to Constipation respond to dietary modification. Varicose veins Nonpharmacological options, such as compression stockings, leg elevation, and edema water immersion, for management of varicose veins and edema in pregnancy. Note: In general, these interventions should be adopted and adapted, based on women’s preferences and available options. 33

E. Health system interventions to improve the utilization and quality of ANC 34

Health systems: All ANC settings A minimum of EIGHT ANC contacts are recommended to reduce perinatal mortality and improve women’s experience of care. 35

ANC contacts schedule • Previously recommended four visits not enough: • Inadequate contact with health care providers • Less maternal satisfaction with care • More perinatal deaths • Minimum EIGHT contacts improves quality: • Focus on timely detection of risk factors and complications • More contact between pregnant women and knowledgeable, respectful, supportive providers more likely to lead to positive pregnancy experience 36

Contact versus visit • The new WHO guideline uses the term “contact” to imply an active connection between a pregnant woman and a health care provider. • “Contact” can take place at the facility or at community level. • “Contact” helps to facilitate context-specific recommendations (e. g. , malaria, tuberculosis interventions) or health system interventions (e. g. , task-shifting). 37
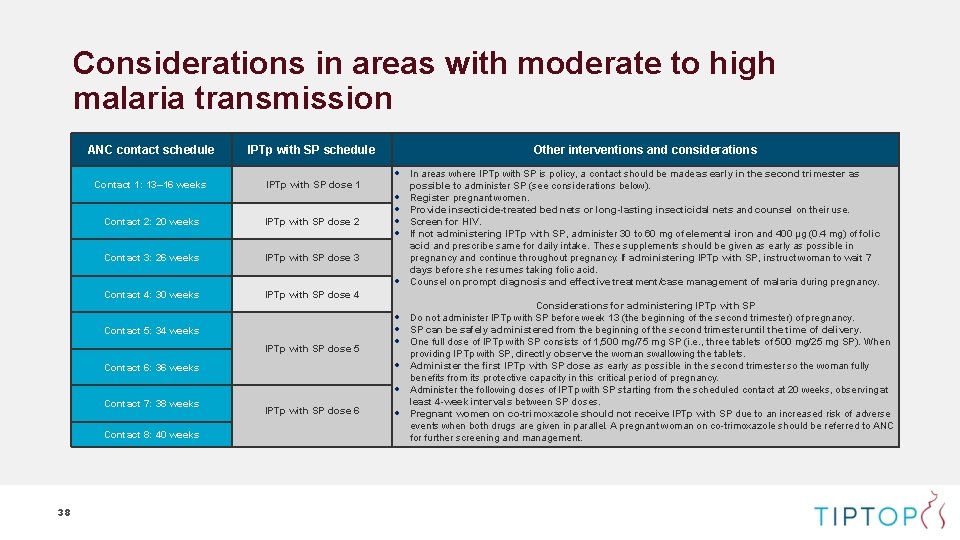
Considerations in areas with moderate to high malaria transmission ANC contact schedule IPTp with SP schedule Contact 1: 13– 16 weeks IPTp with SP dose 1 Contact 2: 20 weeks IPTp with SP dose 2 Contact 3: 26 weeks IPTp with SP dose 3 Contact 4: 30 weeks IPTp with SP dose 4 Other interventions and considerations In areas where IPTp with SP is policy, a contact should be made as early in the second trimester as possible to administer SP (see considerations below). Register pregnant women. Provide insecticide-treated bed nets or long-lasting insecticidal nets and counsel on their use. Screen for HIV. If not administering IPTp with SP, administer 30 to 60 mg of elemental iron and 400 μg (0. 4 mg) of folic acid and prescribe same for daily intake. These supplements should be given as early as possible in pregnancy and continue throughout pregnancy. If administering IPTp with SP, instruct woman to wait 7 days before she resumes taking folic acid. Counsel on prompt diagnosis and effective treatment/case management of malaria during pregnancy. Considerations for administering IPTp with SP Contact 5: 34 weeks IPTp with SP dose 5 Do not administer IPTp with SP before week 13 (the beginning of the second trimester) of pregnancy. SP can be safely administered from the beginning of the second trimester until the time of delivery. One full dose of IPTp with SP consists of 1, 500 mg/75 mg SP (i. e. , three tablets of 500 mg/25 mg SP). When providing IPTp with SP, directly observe the woman swallowing the tablets. Administer the first IPTp with SP dose as early as possible in the second trimester so the woman fully Contact 6: 36 weeks benefits from its protective capacity in this critical period of pregnancy. Administer the following doses of IPTp with SP starting from the scheduled contact at 20 weeks, observing at Contact 7: 38 weeks Contact 8: 40 weeks 38 IPTp with SP dose 6 least 4 -week intervals between SP doses. Pregnant women on co-trimoxazole should not receive IPTp with SP due to an increased risk of adverse events when both drugs are given in parallel. A pregnant woman on co-trimoxazole should be referred to ANC for further screening and management.
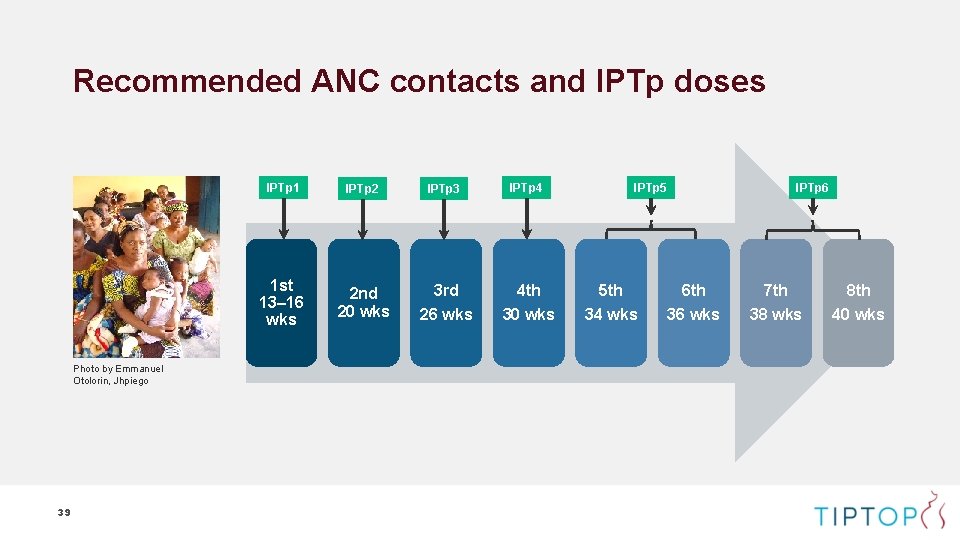
Recommended ANC contacts and IPTp doses Photo by Emmanuel Otolorin, Jhpiego 39 IPTp 1 IPTp 2 1 st 13– 16 wks 2 nd 20 wks IPTp 5 IPTp 6 IPTp 3 IPTp 4 3 rd 4 th 5 th 6 th 7 th 8 th 26 wks 30 wks 34 wks 36 wks 38 wks 40 wks
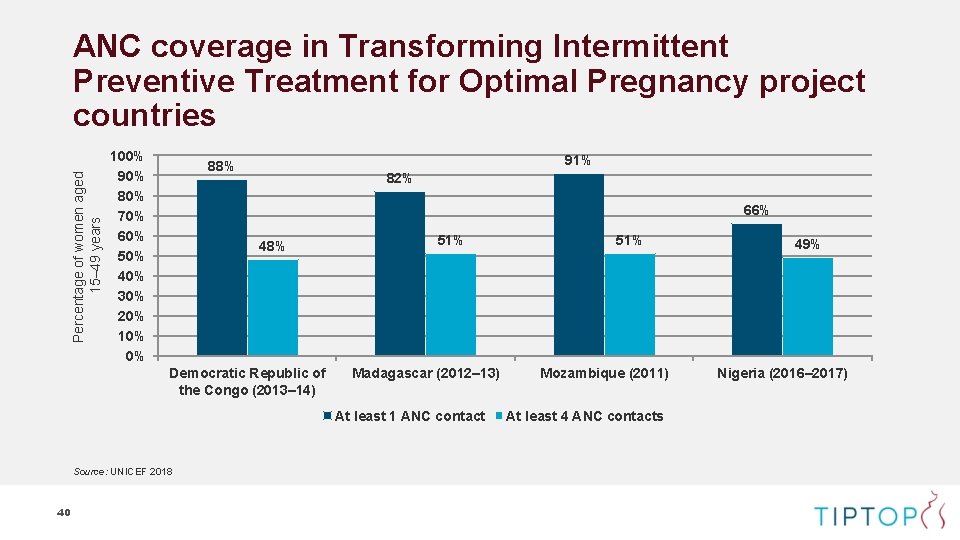
Percentage of women aged 15– 49 years ANC coverage in Transforming Intermittent Preventive Treatment for Optimal Pregnancy project countries 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% 91% 88% 82% 66% 48% Democratic Republic of the Congo (2013– 14) 51% Madagascar (2012– 13) At least 1 ANC contact Source: UNICEF 2018 40 51% Mozambique (2011) At least 4 ANC contacts 49% Nigeria (2016– 2017)

Conclusion 41

Additional slides for health care workers Estimation of gestational age 42

How can you determine the gestational age in a pregnant woman? History 43 Exam Scan
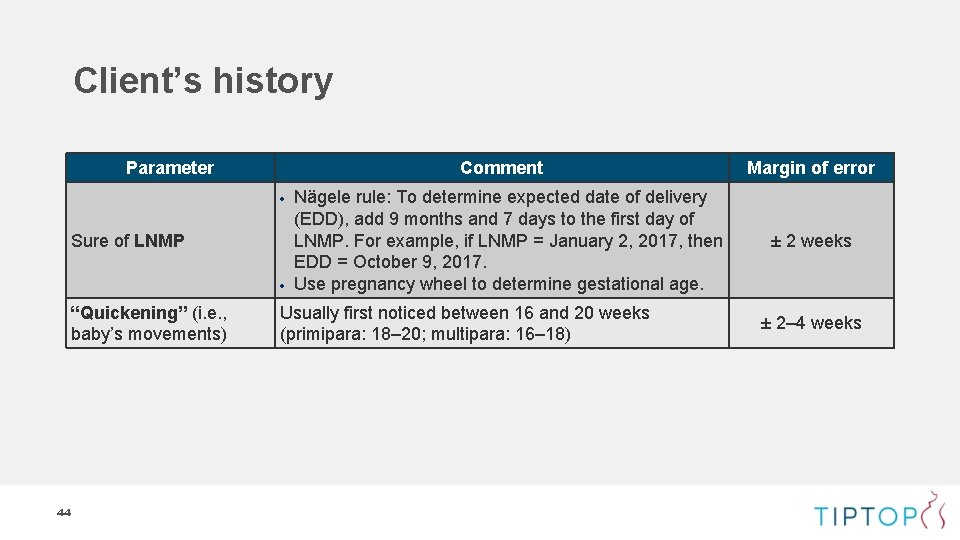
Client’s history Parameter Comment Sure of LNMP “Quickening” (i. e. , baby’s movements) 44 Nägele rule: To determine expected date of delivery (EDD), add 9 months and 7 days to the first day of LNMP. For example, if LNMP = January 2, 2017, then EDD = October 9, 2017. Use pregnancy wheel to determine gestational age. Usually first noticed between 16 and 20 weeks (primipara: 18– 20; multipara: 16– 18) Margin of error ± 2 weeks ± 2– 4 weeks

Exercise 3: Calculating gestational age and EDD Using Nägele rule LNMP = September 21, 2016 Add 9 months = June 21, 2017 Add 7 days = June 28, 2017 45 Calculate EDD and gestational age for the following LNMPs: 1. 2. 3. 4. 5. February 23, 2016 May 30, 2015 April 14, 2017 July 26, 2017 September 8, 2010

Using a pregnancy wheel Calculate the gestational age for the following LNMPs: 1. February 23, 2016 2. May 30, 2015 3. April 14, 2017 4. July 26, 2017 5. September 8, 2010 46
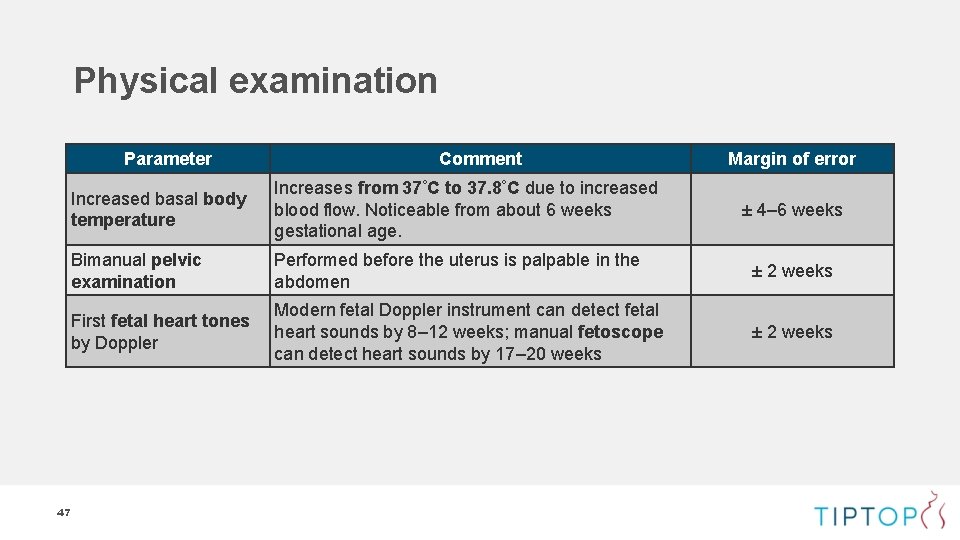
Physical examination Parameter Comment Margin of error Increased basal body temperature Increases from 37°C to 37. 8°C due to increased blood flow. Noticeable from about 6 weeks gestational age. Bimanual pelvic examination Performed before the uterus is palpable in the abdomen ± 2 weeks First fetal heart tones by Doppler Modern fetal Doppler instrument can detect fetal heart sounds by 8– 12 weeks; manual fetoscope can detect heart sounds by 17– 20 weeks ± 2 weeks 47 ± 4– 6 weeks
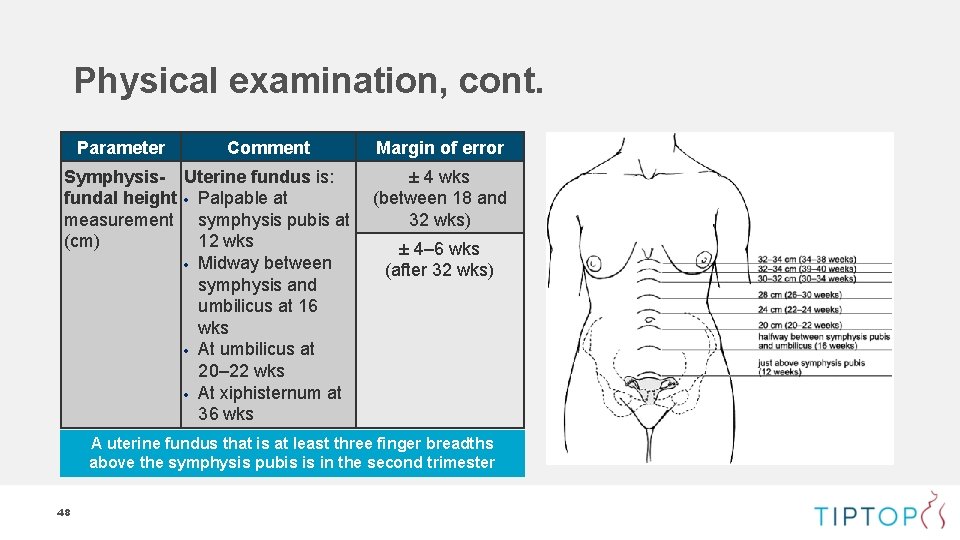
Physical examination, cont. Parameter Comment Symphysis- Uterine fundus is: fundal height Palpable at measurement symphysis pubis at (cm) 12 wks Midway between symphysis and umbilicus at 16 wks At umbilicus at 20– 22 wks At xiphisternum at 36 wks Margin of error ± 4 wks (between 18 and 32 wks) ± 4– 6 wks (after 32 wks) A uterine fundus that is at least three finger breadths above the symphysis pubis is in the second trimester 48
Ultrasound scan Parameter Comment Error margin A. Gestational sac Measurement of gestational sac diameter (in mm) 10 mm = 5 weeks 20 mm = 6. 5 weeks 40 mm = 9. 3 weeks 49 mm = 10. 6 weeks B. Crown-rump length Measurement of the crownrump length (in cm) in the first trimester 1 cm = 7 weeks 2 cm = 8 weeks 4 days 3 cm = 9 weeks 5 days 5 cm = 11 weeks 4 days C. Biparietal diameter D. Others Measurement of the fetal skull biparietal diameter in the second trimester Head circumference Abdominal circumference Adapted from: Mac. Gregor and Sabbagha 2008. 49 3 cm = 14. 4 weeks 5 cm = 20. 7 weeks 8 cm = 31 weeks 9 cm = 36 weeks 10 cm = 42 weeks

References • Mac. Gregor SN, Sabbagha RE. 2008. Assessment of gestational age by ultrasound. Global Library of Women’s Medicine website. doi: 10. 3843/GLOWM. 10206. Accessed October 18, 2018. • UNICEF. 2018. Antenatal care. UNICEF data website. https: //data. unicef. org/topic/maternal-health/antenatal-care/. Published June. Accessed October 18, 2018. • WHO. 2011. WHO Recommendations for Prevention and Treatment of Pre-eclampsia and Eclampsia. Geneva, Switzerland: WHO. http: //apps. who. int/iris/bitstream/handle/10665/44703/9789241548335_eng. pdf. Accessed September 18, 2018. • WHO. 2013. Guideline: Calcium Supplementation in Pregnant Women. Geneva, Switzerland: WHO. http: //apps. who. int/iris/bitstream/handle/10665/85120/9789241505376_eng. pdf? sequence=1. Accessed September 18, 2018. • WHO. 2016. WHO Recommendations on Antenatal Care for a Positive Pregnancy Experience. Geneva, Switzerland: WHO. http: //apps. who. int/iris/bitstream/10665/250796/1/9789241549912 -eng. pdf? ua=1. Accessed September 18, 2018. 50

Thank you! Any questions or comments? 51
- Slides: 52