PICU Primer II Kevin M Creamer M D












































- Slides: 50

PICU Primer II Kevin M. Creamer M. D. Pediatric Critical Care Walter Reed AMC

The Primer Outline ¨ Physiology ¨ ICU Care – Hypoxia / Hypoxemia – Postoperative – ABG’s and Acidosis issues – Sodium and H 2 O – Mechanical metabolism Ventilation – Hemodynamics and ¨ Common Problems Cardiopulmonary – Head trauma interactions – Toxicology

Postoperative Issues ¨ Borrowed in part from Akron syllabus ¨ Know the surgery – what can you expect from a posterior spinal fusion is different than a tracheal reconstruction ¨ Know the patient – Age, PMHx, Syndromes ¨ Be there when they get out of the OR

Postoperative Evaluation ¨ ABC’s ¨ Look at the breathing pattern ¨ Listen to the chest--breath sounds, stridor? ¨ Listen to the heart--gallop, murmur? ¨ Feel the pulses--strong, weak, thready? – Cap refill? , Extremity warmth?

The Anesthesia Report ¨ “History of present illness” for surgical patients – Difficulties with induction or intubation? – Drugs used during case – Regional techniques employed? – Extubation-problems? ¨ Vital signs- BP, HR, RR, Sa. O 2, temp – Patients are frequently cold!

The Anesthesia Report ¨ Ventilation parameters/difficulties ¨ Fluids--ins and outs ¨ Any “events”? ¨ Lines and tubes

Intraoperative Fluids ¨ Pediatrician: “Why do they always get so much fluid? ” ¨ Anesthesiologist: “Because they need it” – maintenance + replacement of “third space” losses • “third space” losses can be 15 cc/kg/hr + replacement of 3 X blood loss

Anesthesia and Fluid Balance ¨ General anesthesia produces vasodilation and some decrease in myocardial contractility. ¨ Increased intrathoracic pressure, and stress response to surgical stimulus, may lead to increased ADH production and decreased urine output

BLOOD loss and replacement ¨Blood loss is estimated ¨ Transfusion Criteria - it depends – Check Hct, HR, UOP, p. H, ongoing loss, Hemodynamics … ¨ When do you need Component Tx? – after a “massive” transfusion or ( 0. 75 -3. 0 blood volumes)

Blood Products - How much? ¨ PRBCs - 4 cc/kg of will Hb 1 gm/dl ¨ Platelets - 1 unit/5 kg will count by 50000 ¨ FFP - 10 ml/kg round up/down to closest unit ¨ Cryoprecipitate - 1 bag/every 5 -10 kg Surgeons get extremely persnickety if you transfuse THEIR patient without letting them know ahead of time!

The Surgical Report ¨ Since we are not surgeons we need to know what they anticipate and worry about – Amount of pain – Third spacing – Possible complications ¨ Their wish list: – Extubate tomorrow, MRI at midnight – Special meds: antibiotic and stress ulcer prophylaxis

The Surgical Report ¨ What to touch and not to touch? – NG, foley, chest tube, rectum, etc. ¨ Check all their orders for appropriate dosing and fluids – mg/kg/dose is not in surgical vocabulary ¨ Who is in Charge? (Us vs. Them) ¨ Surgical POC? – Interface with surgeons before they return to the OR in AM regarding the plan

Assessment of Fluid Balance: ¨ Vital signs (HR/BP) ¨ Urine output ¨ Extremity warmth, CRT ¨ Acid-base status ¨ Occasionally invasive monitoring – Remember the Liver!

Extubation Time? ¨ Adequate airway (edema? , Leak? ) ¨ Maintain oxygenation and ventilation ¨ Neurologically able to protect the airway and maintain adequate drive. ¨ Small/young infants are at increased risk of apnea – Especially if post-conceptual age < 50 weeks

Sedation and Analgesia ¨ Analgesia for painful diseases and procedures ¨ Compliance with controlled ventilation and routine intensive care ¨ Sedation for amnesia for the periods of noxious stimuli ¨ Reduce the physiologic responses to stress

Sedation and Analgesia ¨ The idea of titrating drugs to effect-- there is no “dose”. – Keep in mind what the “target” response is. ¨ Consider Round-the-clock Tylenol for 24 -48 hours as adjunct – First PR dose may be 30 -40 mg/kg ¨ Anesthesia service manages Epidurals ¨ Consider a continuous drip

BP: hypotension, H: Histamine, A: Apnea, CWR: chest wall rigidity

Muscle Relaxants ¨ They provide ZERO sedation/analgesia. ¨ Indications (always relative) – Mechanical ventilation where risk of extubation is great, or risk of baro/volutrauma is high – Procedures such as central line placement or biopsy in the intubated patient – Intractable intracranial hypertension (IF ICP being monitored)

Problems with Blockade ¨ Fluid retention ¨ Long term weakness – continuous infusions – most commonly the steroid based NMBs – myopathy associated with Atracurium – consider using cis-Atracurium ¨ Consider Train of Four testing ¨ FREQUNTLY OVERUSED

¨ NEXT UP – Mechanical ventilation This is not the NICU!

Lesson Learned: VALI –Predisposing Factors ¨ High lung Volumes – With high peak pressure and alveolar overdistension ¨ Repeated alveolar collapse and reopening ¨ High inspired oxygen Concentrations ¨ Preexisting lung injury Slutsky Am J Resp CCM, 1999, Dreyfuss Am J Resp CCM 1998

Mechanical Ventilation ¨ Do’s and Don’ts – Avoid Overdistension and High Pressure by limiting Tv – Avoid Hyperoxic Lung damage by turning FIO 2 down (Sat 90% okay) – Avoid cyclic collapse by using PEEP to recruit FRC and keep it above Closing volume ¨ Infant high risk 2° high elastic recoil and complaint chest wall

Open Lung Strategy

Getting Started (Parameters)

Getting Started (Mode)

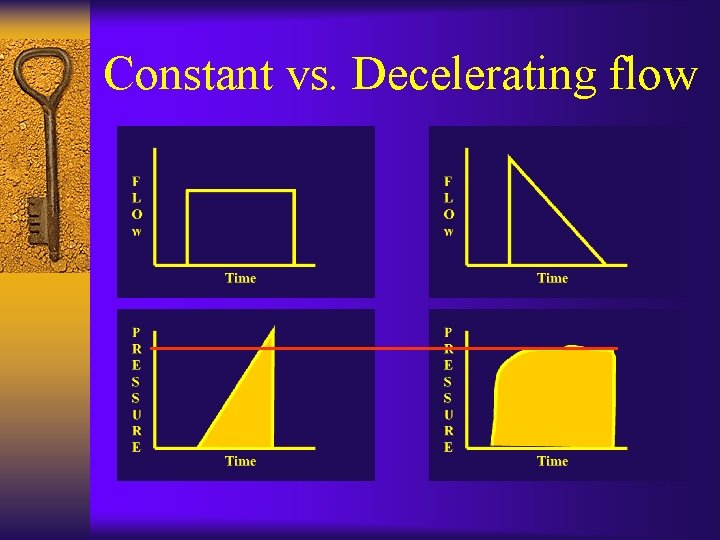
Constant vs. Decelerating flow

Getting Started (Settings) ¨ FIO 2 - 50%, if sick 100% ¨ It - minimum. 5 sec, older kids 1 sec ¨ Rate - age appropriate 15 -30 to start ¨ Tv - 10 ml/kg to start ¨ Look / Listen / Ask ¨ PEEP - 4 cm, higher if FRC compromised

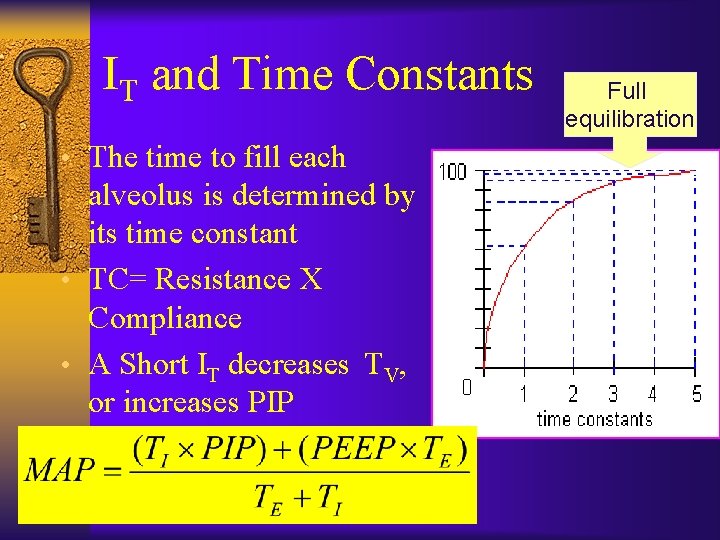
IT and Time Constants • The time to fill each alveolus is determined by its time constant • TC= Resistance X Compliance • A Short IT decreases TV, or increases PIP Full equilibration

Mechanical Ventilation ¨ First hour – CXR and “Blood Gas” – Watch peak pressures as compliance estimate • PP << 20 ideal • PP 20 -30 moderately compliance • PP >> 30 severely compliance • PP >> 35 high risk for VALI, DO SOMETHING

Mechanical Ventilation ¨ Change Tv only for inappropriate chest rise or for elevated inspiratory pressures (Don’t WEAN Tv) ¨ Sedation to allow patient - ventilator synchrony (Paralytics aren’t required)

Monitoring adjuncts ¨ Pulse oximeter ¨ End tidal CO 2 - can use for Dead space estimate ¨ ABG’s and CBG’s ¨ Calculate Compliance, A-a gradient, Oxygenation Index (OI), check for Autopeep ¨ Graphics - PV and flow-volume loops

Equations ¨ Dead Space = 1 - (Et. CO 2/Pa. CO 2) ¨ Static Comp. = Tv/ (Pplat- PEEP) ¨ A-a gradient = – (Pb-PH 2 O) x FIO 2 - (PCO 2/. 8) - Pa. O 2 ¨ OI = (Paw x FIO 2 x 100)/ Pa. O 2

When things go wrong ¨ Don’t be a DOPE ¨ Hypoxemia - PEEP to FRC, to allow FIO 2 wean to < 50% ¨ Elevated peak pressures - suction, adopt Permissive hypercapnia, consider changing to pressure mode ¨ Check circuit size – an inappropriately large circuit can gobble up lots of tidal volume

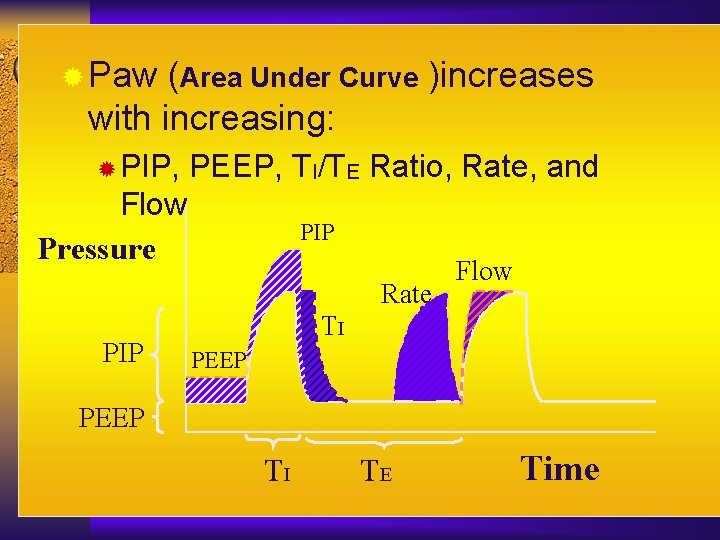
® Paw (Area Under Curve )increases with increasing: ® PIP, PEEP, TI/TE Ratio, Rate, and Flow Pressure PIP Rate PIP Flow TI PEEP TI TE Time

Circuit compliance ¨ When using volume ventilation the ventilator circuit or tubing will stretch – Neonatal 0. 35 ml / cm H 2 O – Pediatric 1. 4 ml / cm H 2 O – Adult 2. 8 ml / cm H 2 O ¨ This means the stiffer the lung the more volume is lost in the circuit

Mechanical Ventilation ¨ First day and beyond – Watch for fluid overload • all patients on positive pressure ventilation retain lung water – Assist patient efforts • Pressure support or volume support • Trigger sensitivity (age and disease appropriate) – Treat underlying condition – Feed patient

Weaning ¨ Get condition under control ¨ Stop paralytics (PEEP < 8) ¨ Encourage patient’s efforts – Rate (slow then fast) – add Pressure support (2/3 P) ¨ Wean PEEP and PS slowly in 1 -2 cm H 2 O increments ¨ Wean FIO 2 to 30% if possible

Signs of weaning failure ¨ Increased Work of breathing – fast spontaneous RR – small spontaneous Tv ¨ Increased FIO 2 requirement ¨ Hemodynamic compromise

Time for Extubation? ¨ Think SOAP – Secretions / Sedation / Spontaneous Tv (>5 ml/kg) – Oxygenation <35% – Airway - Maintainable? , Leak? , Steroids? – Pressures - PP <25, PEEP < 5

Extubation success predictors Khan, CCM 1996

Special situations I ¨ Obstructive Diseases – Asthma and RSV Bronchiolitis – Watch for air trapping / breath stacking • Low rate, larger Tidal volume, long Expiratory time • check Autopeep • preserve I-time • Consider Heliox, Ketamine, Halothane

Special situations II ¨ ARDS – Limit Tv accept hypercapnia – Increase PEEP for FRC – Prone positioning – Ca. O 2 and tolerate lower Sat % – consider High Frequency Oscillatory Ventilation>>> Surfactant>>> Nitric Oxide

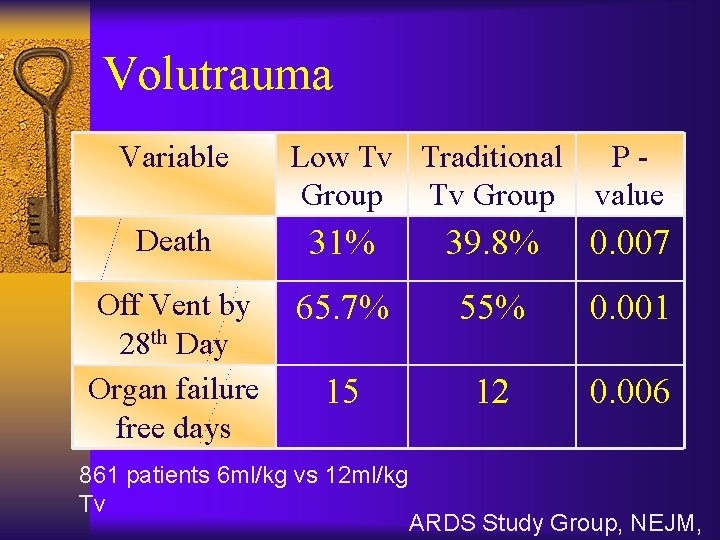
Volutrauma Variable Low Tv Traditional Group Tv Group Pvalue Death 31% 39. 8% 0. 007 Off Vent by 28 th Day Organ failure free days 65. 7% 55% 0. 001 15 12 0. 006 861 patients 6 ml/kg vs 12 ml/kg Tv ARDS Study Group, NEJM,

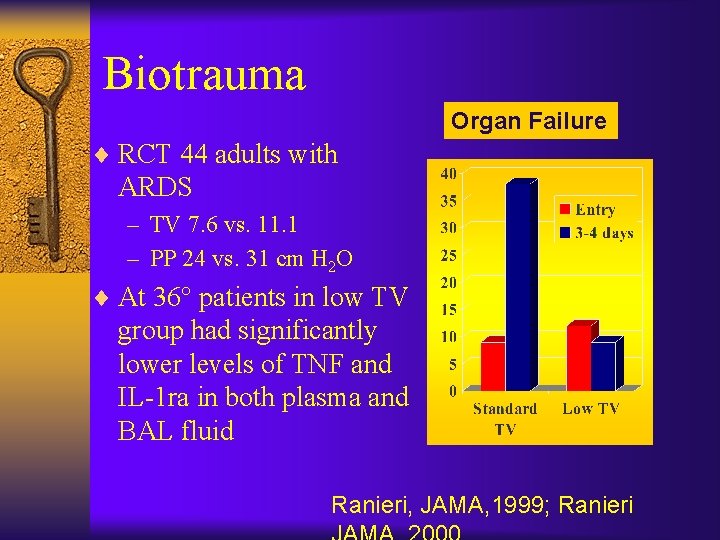
Biotrauma Organ Failure ¨ RCT 44 adults with ARDS – TV 7. 6 vs. 11. 1 – PP 24 vs. 31 cm H 2 O ¨ At 36° patients in low TV group had significantly lower levels of TNF and IL-1 ra in both plasma and BAL fluid Ranieri, JAMA, 1999; Ranieri

Special situations III ¨ Head Trauma – Avoid Hypercarbia (PCO 2 < 35) – Avoid Hypoxemia – PEEP may adversely effect venous return and ICP – Coughing/gagging extremely bad (Use paralytics)

Special situations IV ¨ HFOV Indications – ARHF with OI > 13 for 6 hours – Contraindicated in High airway resistance, ICP, unstable hemodynamics ¨ Part of an Open lung strategy with Mean airway pressure and Tv < dead space

HFOV vs. CMV ¨ Crossover study acute hypoxemic respiratory failure in children ¨ HFOV 17/29 responded, 0/17 died ¨ CMV 10/29 responded, 4/10 died ¨ X-over to HFOV 11/19 survived ¨ X-over to CMV 2/11 survived Arnold, CCM 1994

Ventilation Simulator ¨ Not for the weak of heart

The End Mind what you have learned. Save you it can.

Questions?