Peripheral Vascular System Assessment Overview of Peripheral Vascular
















- Slides: 24

Peripheral Vascular System Assessment

Overview of Peripheral Vascular Disease Characterized by disturbances in blood flow Damage can occur from any disorder that: Narrows Obstructs Injures The blood vessels thus impeding blood flow Includes both peripheral arterial disease (PAD) and chronic venous insufficiency

Peripheral Arterial Disease Can effect any part of vascular system Can manifest as acute or chronic condition Causes of decreased arterial blood flow Atherosclerosis or Spasm Embolism or thrombus Hypotension or Hypercoagulability Trauma Compartment syndrome Risk factors are same as all cardiovascular disease

Peripheral Arterial Disease Also referred to as: PVD 1) Chronic, progressive, arterial narrowing 2) Reduced blood supply resulting in ischemia 02 needs exceed supply, areas of ischemia & ultimately necrosis will develop Symptoms are manifested based on the extent to which tissues are deprived of 02 The ability of the vascular system to develop collateral circulation will have an effect on the development of clinical symptoms

Intermittent Claudication Aching pain or cramping sensation that occurs in the muscle distal to the occlusion that occurs with activity and disappears with rest Due to inadequate oxygenation. Similar to angina, predictable and reproducible. May escalate into rest ischemia or pain (urgent attention needed)

Intermittent Claudication Rest ischemia May be accompanied by coldness and/or paresthesias May be aggravated by elevation of extremities Gravity improves perfusion and decreases symptoms

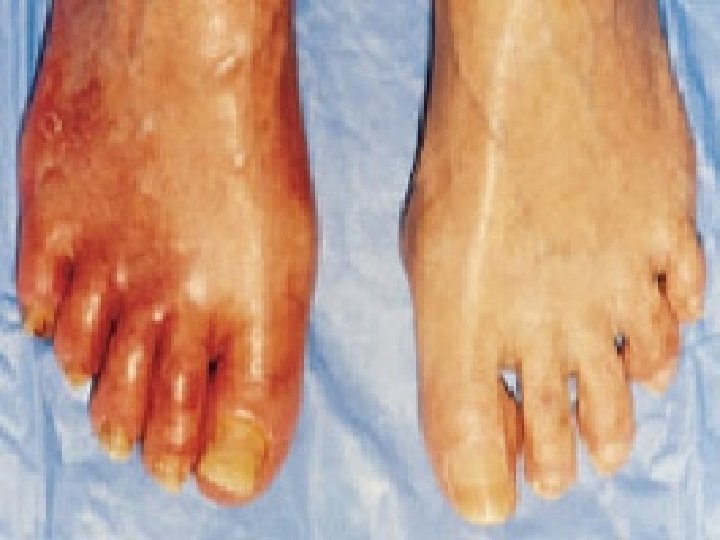
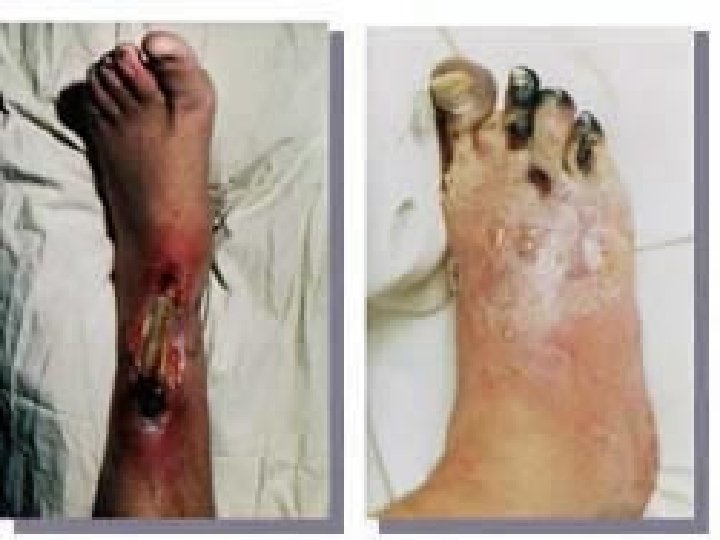
Symptoms of Arterial Disease Absence of hair Shiny skin, thick ridged toenails Pale with elevation Dependent rubor Cool to touch Pulses decreased to absent Small, painful ulcers on pressure points, trauma, toes Gangrene



Venous Symptoms Venous Insufficiency Blood gets to tissues but decreased blood return to heart. Prolonged venous HTN leading to venous congestion & stasis, stretching the veins & damaging the valves. Chronic Venous Insufficiency Edema Color Ulcers

Chief Complaint: Venous Insidious onset History of work involving standing Swelling increasing with time Erythema Lipodermatosclerosis Dry and flaky stasis dermatitis Ulcers most commonly above the medial malleolus

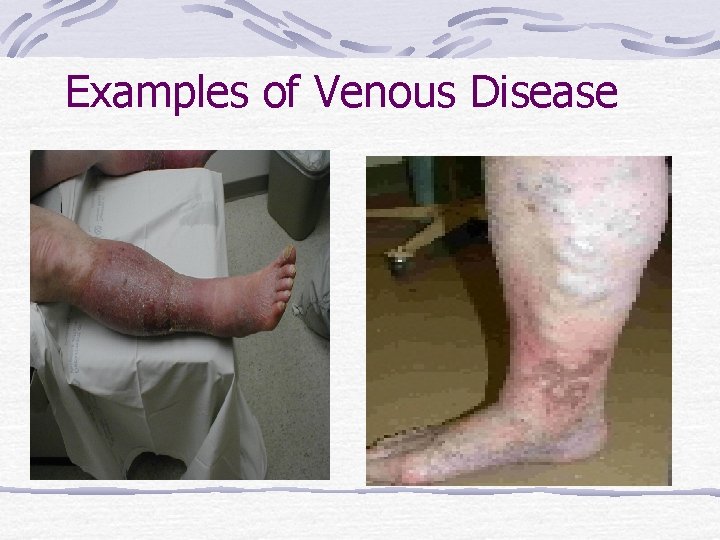
Examples of Venous Disease

Chief Complaint: Lymphatic Lymph edema- accumulation of lymph in soft tissue Prolonged edema in tissues may lead to fibrosis and lack of ability to compress

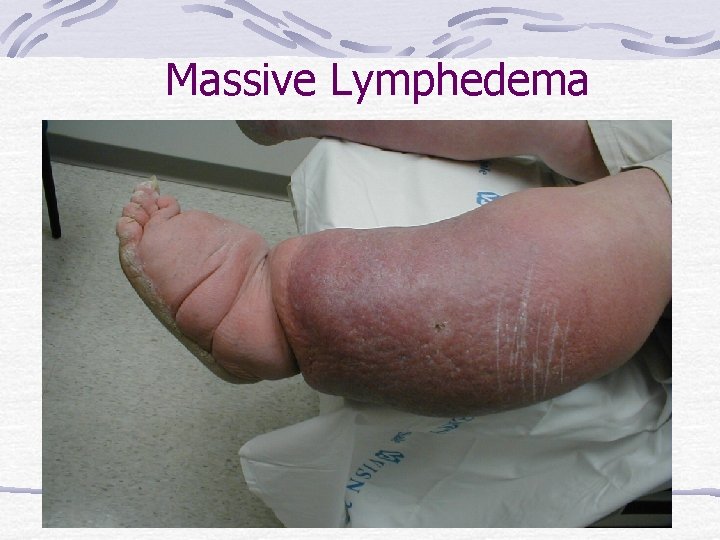
Massive Lymphedema

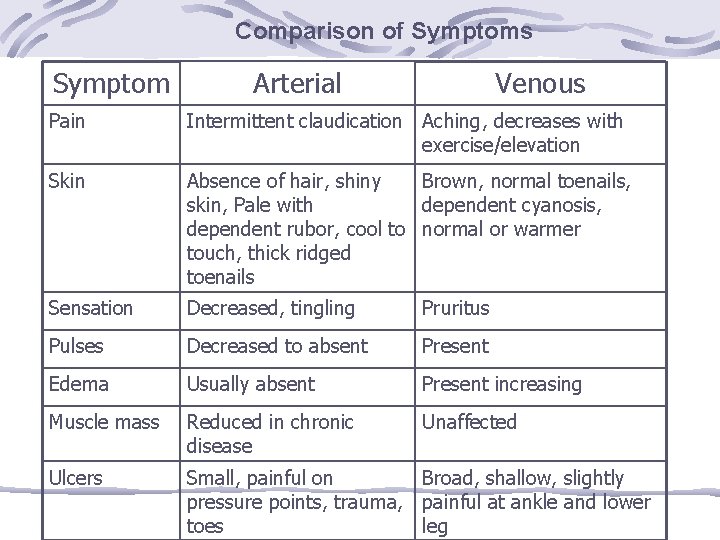
Comparison of Symptoms Symptom Arterial Venous Pain Intermittent claudication Aching, decreases with exercise/elevation Skin Absence of hair, shiny Brown, normal toenails, skin, Pale with dependent cyanosis, dependent rubor, cool to normal or warmer touch, thick ridged toenails Sensation Decreased, tingling Pruritus Pulses Decreased to absent Present Edema Usually absent Present increasing Muscle mass Reduced in chronic disease Unaffected Ulcers Small, painful on Broad, shallow, slightly pressure points, trauma, painful at ankle and lower toes leg

Physical Assessment: Inspection Skin color – pallor, rubor, cyanosis Hair distribution Nail beds Capillary refill Muscle atrophy Edema Ulcers

Physical Assessment: Palpation Temperature Pulses Allen’s test Homan’s sign - unreliable

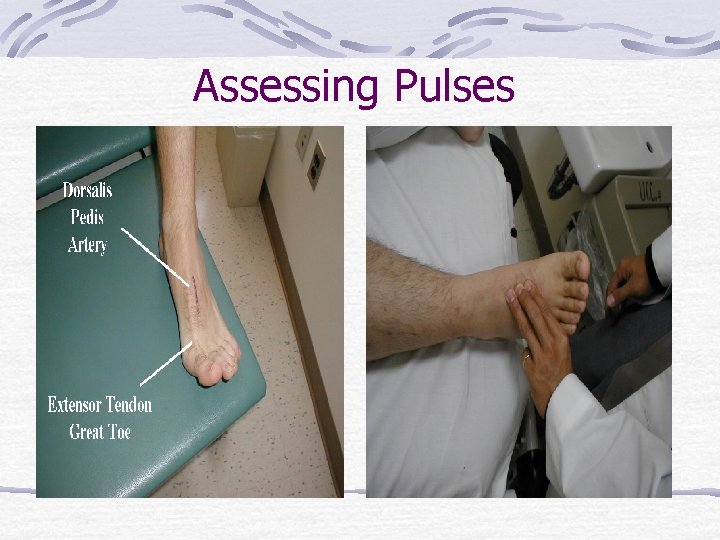
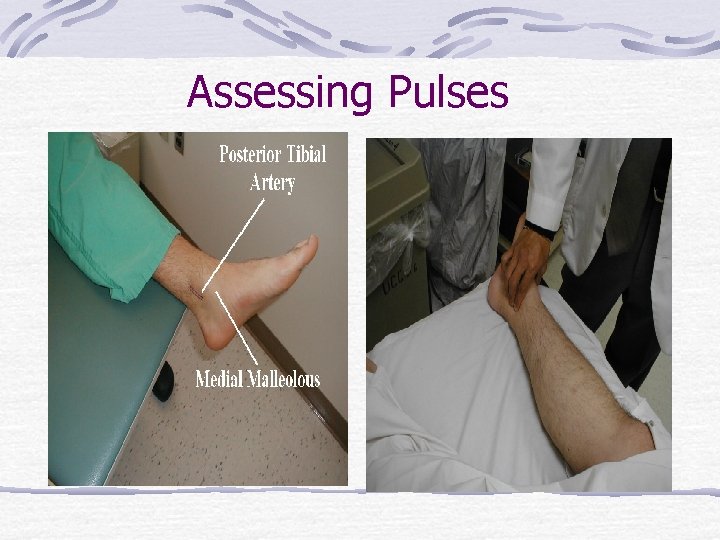
Assessing Pulses

Assessing Pulses

Physical Assessment: Ausculation Limb blood pressure Single best indicator of arterial perfusion Bruits – whooshing sound from turbulent blood flow from vessel wall abnormalities Carotid, aorta, renal, femoral, popliteal

Diagnostic Tests: Non-Invasive Doppler ultrasound – audible arterial signals and measurement of limb pressures B Mode (Brightness Mode)Ultrasound – 2 dimensional image: size, compressibility, thrombus and valve functions Ankle-Brachial index – Equation using pressures obtained from cuffs Image exams – CT scan, MRI

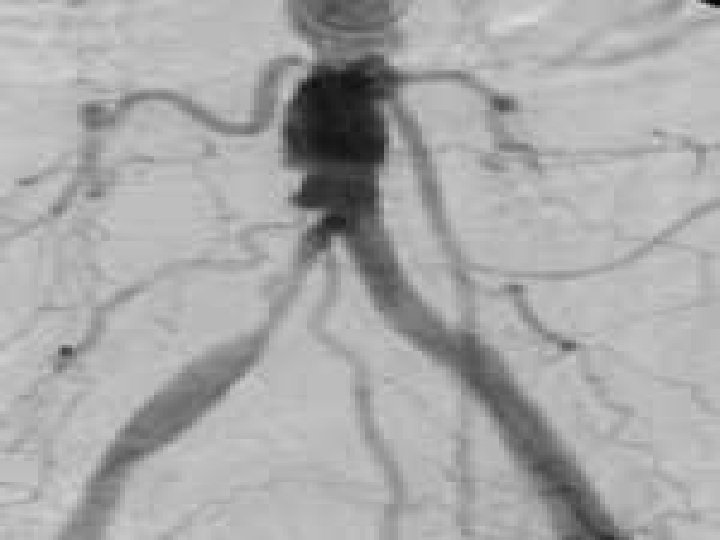
Diagnostic Tests: Invasive Angiography – most invasive and highest risk to client. Usually done prior to surgical intervention Involves injecting contrast agent into an arterial system and obtaining radiological pictures


Angiography Pre-procedure Explain procedure Informed consent Renal function assessment NPO 2 -6 hours Mild sedative Post-procedure Frequent assessment of VS, pulses, access site Bedrest for 6 -8 hours IV/oral hydration Reassessment of renal function Manage complications