Basic Science Peripheral Vascular Disease Peripheral Arterial Occlusive

Basic Science Peripheral Vascular Disease

Peripheral Arterial Occlusive Disease Basic Considerations

Atherosclerosis - Risk factors • • • Hypercholesterolemia Diabetes Hypertension Smoking Relative factors - advanced age, male gender, hypertriglyceridemia, hyperhomocysteinemia, sedentary lifestyle, family history

Pathophysiology of Atherosclerosis • Atheroma – porridge; Sclerosis – hardening • Response to endothelial injury hypothesis – Loss of barrier function, antiadhesive properties and antiproliferative influence on underlying SMCs – Migration and proliferation of SMCs production of ECM – Oxidized lipid accumulation in vessel walls – Recruitment of macrophages and lymphocytes – Adherence of platelets to dysfunctional endothelium, exposed matrix, and macrophages
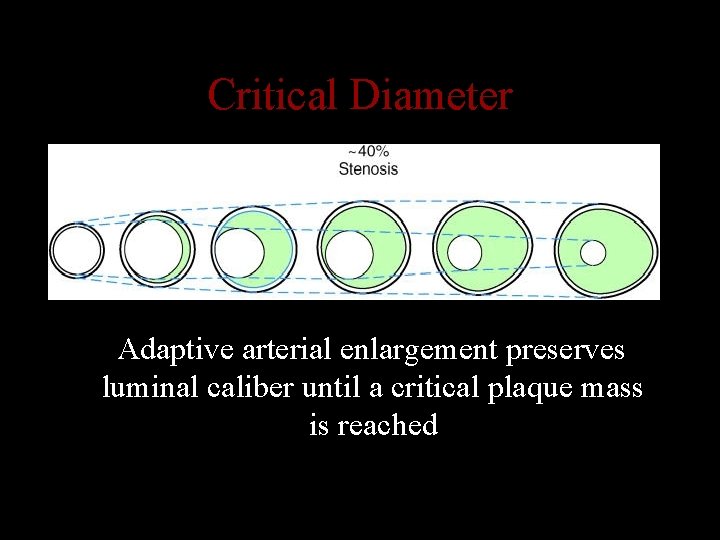
Critical Diameter Adaptive arterial enlargement preserves luminal caliber until a critical plaque mass is reached
Diagnostic Modalities • Non-invasive – ABIs – Segmental limb pressures – Limb plethysmography – Exercise testing – Doppler & duplex ultrasound – MR angiography • Invasive – Contrast arteriography – CT angiography
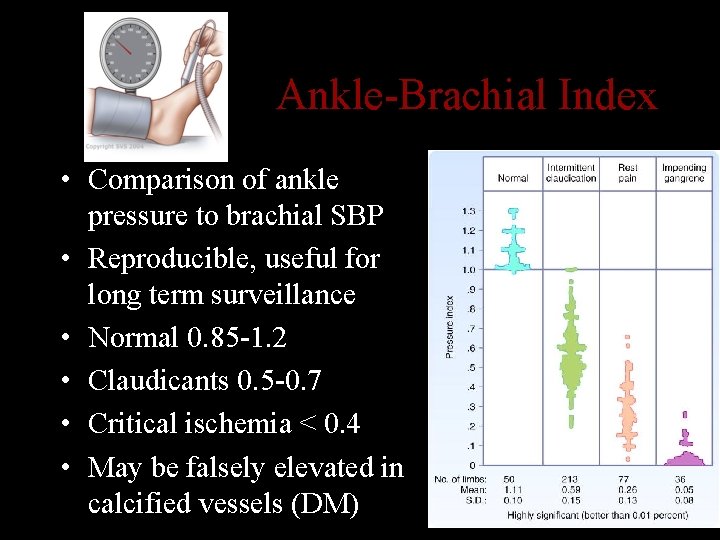
Ankle-Brachial Index • Comparison of ankle pressure to brachial SBP • Reproducible, useful for long term surveillance • Normal 0. 85 -1. 2 • Claudicants 0. 5 -0. 7 • Critical ischemia < 0. 4 • May be falsely elevated in calcified vessels (DM)
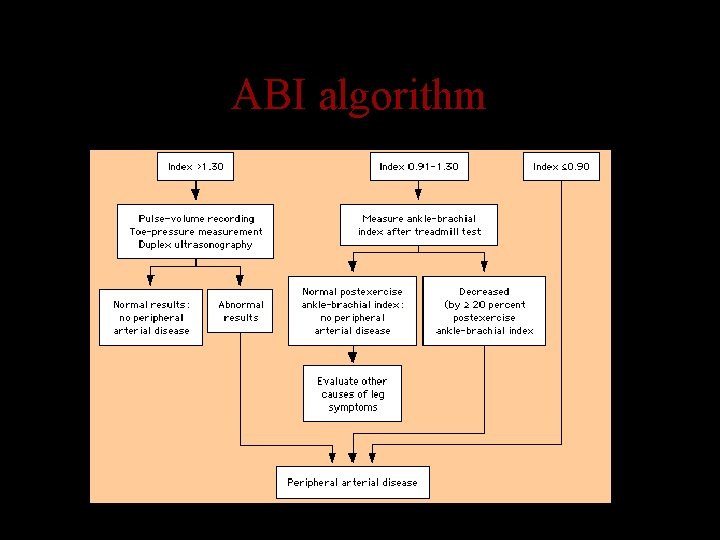
ABI algorithm

PVR • Calibrated air plethysmographic wave form recording system • Helps localize site of obstruction • Placement of cuffs at levels of proximal and distal thigh, calf and ankle

Medical Therapy • Risk factor management – Lipid-lowering therapy – Smoking cessation • Exercise regimen • Antiplatelet therapy - ASA, ticlodipine, clopidogrel • Vasoactive - Cilostazol (Pletal), pentoxyfilline (Trental)
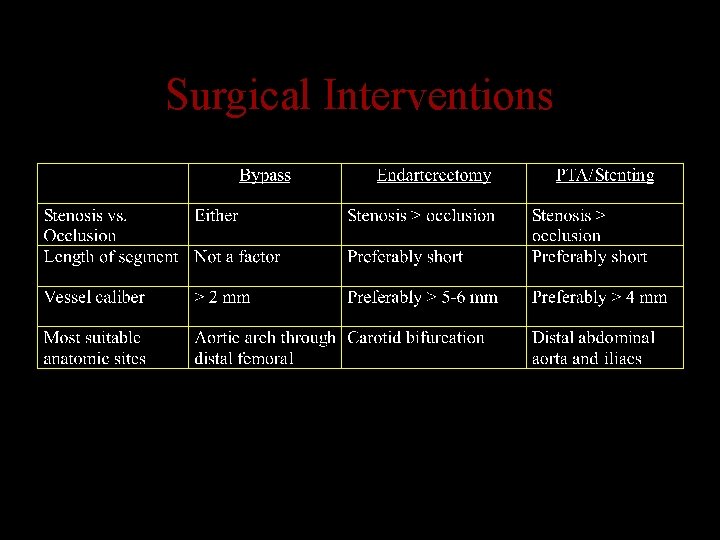
Surgical Interventions

Peripheral Arterial Occlusive Disease Carotid Stenosis

Question A patient with symptomatic 85% carotid stenosis is found to have asymptomatic 50% stenosis on the contralateral side. Appropriate initial treatment includes: A. Simultaneous bilateral CEA B. Staged bilateral CEA with 1 week interval between stages C. CEA on symptomatic side only D. CEA on side of greatest stenosis regardless of symptoms

Question A patient with symptomatic 85% carotid stenosis is found to have asymptomatic 50% stenosis on the contralateral side. Appropriate initial treatment includes: A. Simultaneous bilateral CEA B. Staged bilateral CEA with 1 week interval between stages C. CEA on symptomatic side only D. CEA on side of greatest stenosis regardless of symptoms
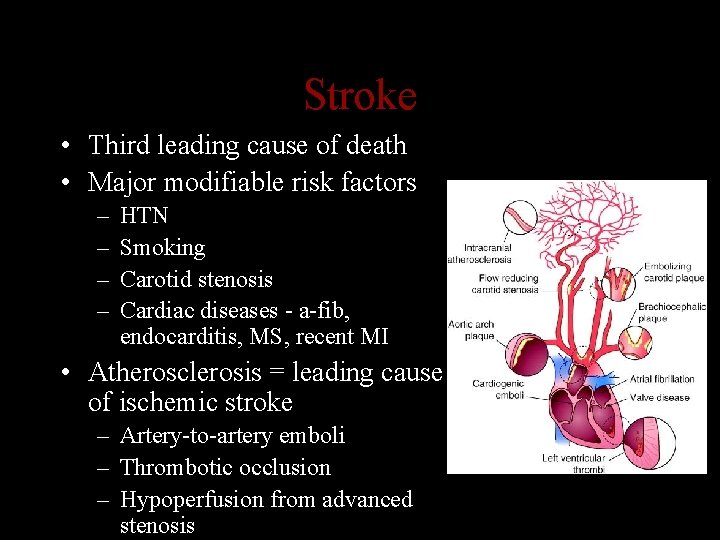
Stroke • Third leading cause of death • Major modifiable risk factors – – HTN Smoking Carotid stenosis Cardiac diseases - a-fib, endocarditis, MS, recent MI • Atherosclerosis = leading cause of ischemic stroke – Artery-to-artery emboli – Thrombotic occlusion – Hypoperfusion from advanced stenosis
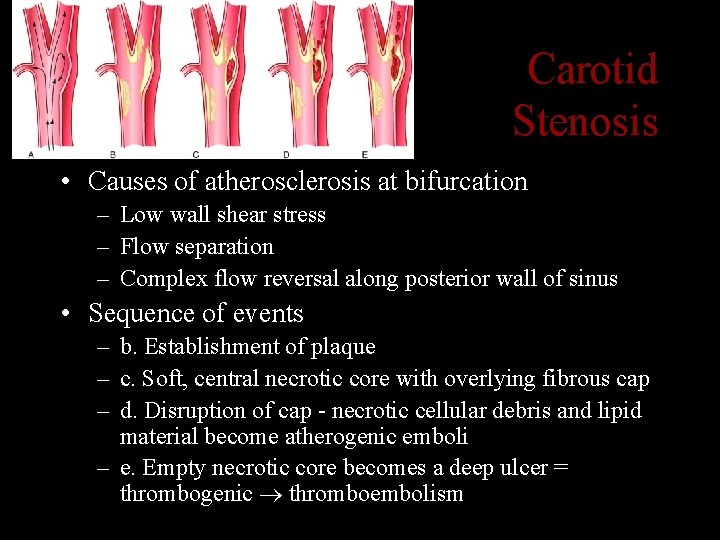
Carotid Stenosis • Causes of atherosclerosis at bifurcation – Low wall shear stress – Flow separation – Complex flow reversal along posterior wall of sinus • Sequence of events – b. Establishment of plaque – c. Soft, central necrotic core with overlying fibrous cap – d. Disruption of cap - necrotic cellular debris and lipid material become atherogenic emboli – e. Empty necrotic core becomes a deep ulcer = thrombogenic thromboembolism

Presentation • Asymptomatic bruit • Amaurosis fugax – transient monocular visual disturbance • Lateralizing TIA • Crescendo TIA • Stroke-in-evolution • CVA
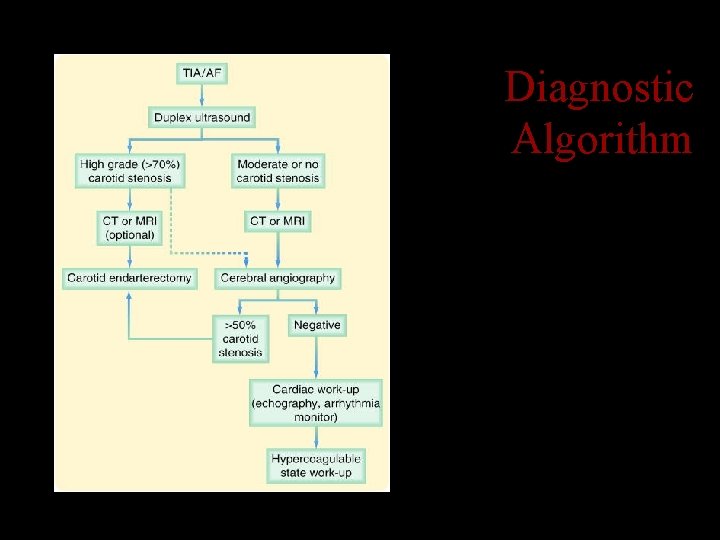
Diagnostic Algorithm
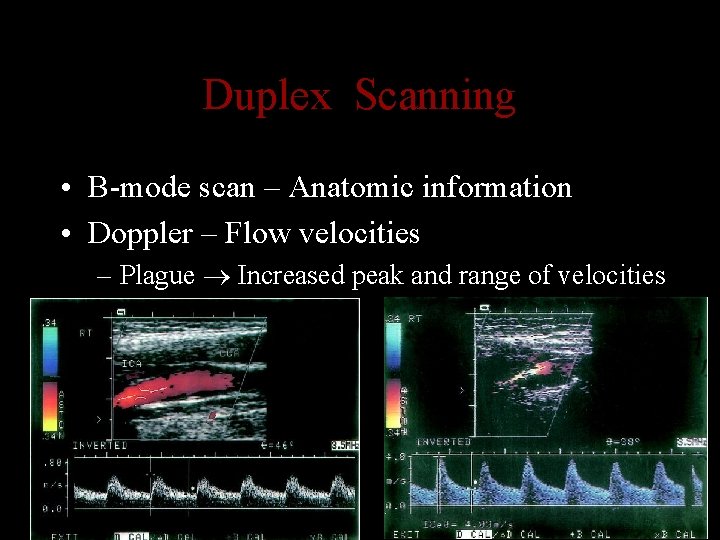
Duplex Scanning • B-mode scan – Anatomic information • Doppler – Flow velocities – Plague Increased peak and range of velocities

Indications for CEA • Symptomatic – TIA, AF, small stroke – Proven – Stenosis > 70% – Acceptable – Stenosis 50 -69% – Lesser symptoms, failed medical therapy • Asymptomatic – Proven – Stenosis > 60%, good risk – Uncertain • • High risk patient Surgeon morbidity-mortality >3% Combined carotid coronary operation Non-stenotic ulcerative lesions • Presence of ulceration or contralateral occlusion may lower threshhold for surgery

Peripheral Arterial Occlusive Disease Chronic Occlusive Disease of the Lower Extremities

Question Which of the following is an indication for bypass? A. Claudication within ½ block B. ABI of 0. 5 C. Rest pain D. Occlusion of the superficial femoral and anterior tibial arteries

Question Which of the following is an indication for bypass? A. Claudication within ½ block B. ABI of 0. 5 C. Rest pain D. Occlusion of the superficial femoral and anterior tibial arteries

Prevalence and survival • 2 -3% population >50 y, 10% > 70 y • Lower extremity ischemia associated with decreased 5 -yr survival – – 97. 4 % intermittent claudication 80% claudication requiring surgery 48% limb-threatening ischemia 12% re-op for limb-threatening ischemia

Signs and symptoms • Claudication – Extremity pain, discomfort or weakness – Consistently produced by the same amount of activity – Relieved with rest • Rest pain – Localized to metatarsal heads and toes – Worse with elevation or recumbent position – Improved with foot dependency
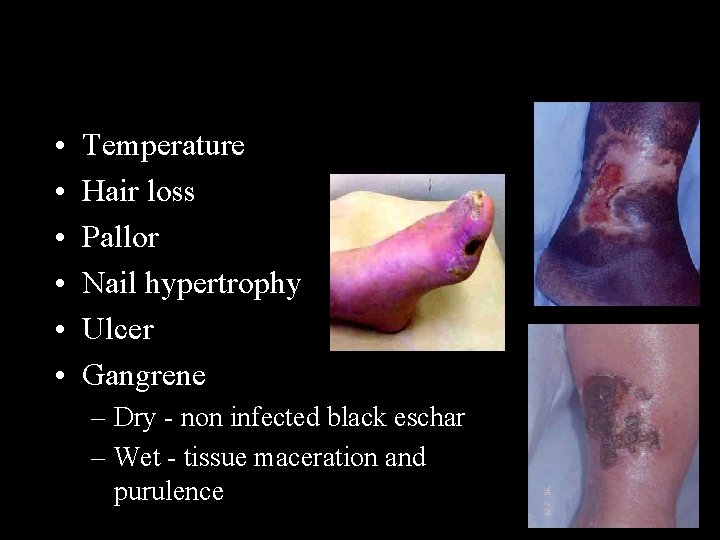
• • • Temperature Hair loss Pallor Nail hypertrophy Ulcer Gangrene – Dry - non infected black eschar – Wet - tissue maceration and purulence
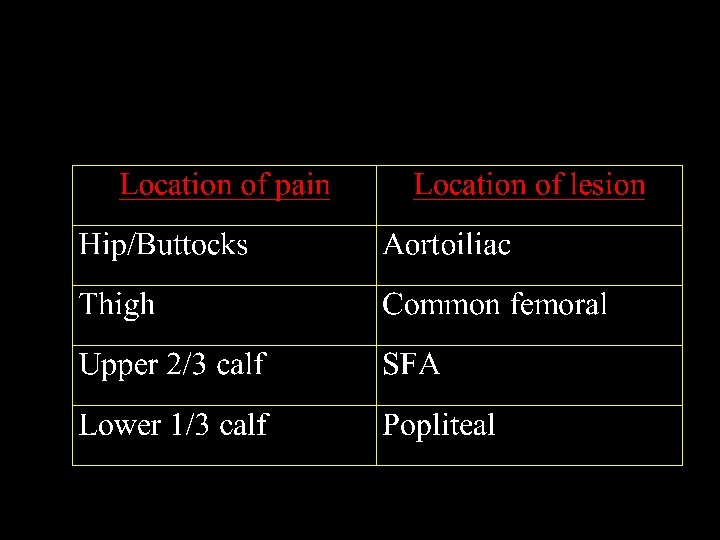
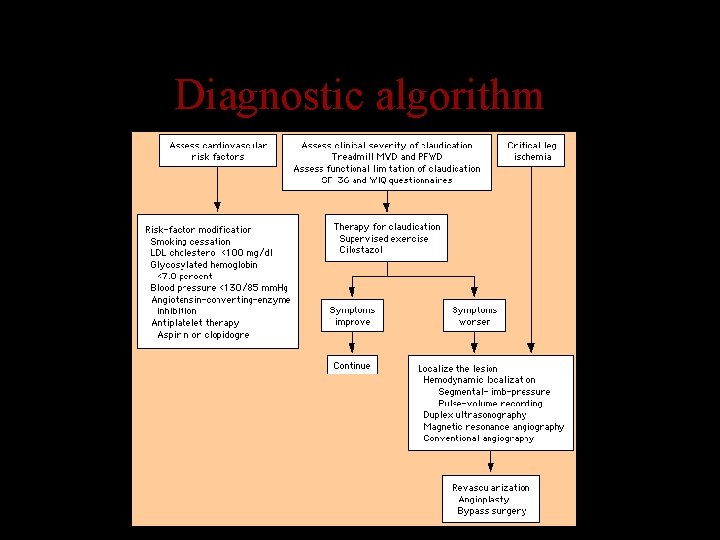
Diagnostic algorithm

Question Late vein graft failure is due to: A. Atherosclerotic changes in the vein B. Vein thrombosis C. Fibrointimal hyperplasia D. Kinking of the vein graft

Question Late vein graft failure is due to: A. Atherosclerotic changes in the vein B. Vein thrombosis C. Fibrointimal hyperplasia D. Kinking of the vein graft

Graft • Autologous Vein Graft - SV, arm vein • Synthetic - PTFE, Decron • Graft failure – 30 days - Technical error – 30 days to 2 years - Intimal hyperplasia – >2 years - Progression of atheresclerosis • Surveillance – Duplex 6 wks peri-op, 3 months/2 yrs, q 6 month

Peripheral Arterial Occlusive Disease Acute Thromboembolic Disease

Question 86 yo F with PMHx CAD, HTN, DM, A fib presents w/ sudden onset left lower extremity pain. Palpable femoral pulses. No palpable or doppler signals on left. Nl on right. Where is her obstruction? A. Common femoral artery B. Popliteal artery C. Iliac bifurcation D. Superficial femoral artery

Question 86 yo F with PMHx CAD, HTN, DM, A fib presents w/ sudden onset left lower extremity pain. Palpable femoral pulses. No palpable or doppler signals on left. Nl on right. Where is her obstruction? A. Common femoral artery B. Popliteal artery C. Iliac bifurcation D. Superficial femoral artery

Epidemiology • • • Incidence: 1. 7 cases / 10, 000 people / Yr. Elderly Male > female Mortality 15%, Amputation 10 -30% Medical co-morbidities common – CVD 12%, CAD 45%, DM, 31%, HTN 60%, CHF 13%
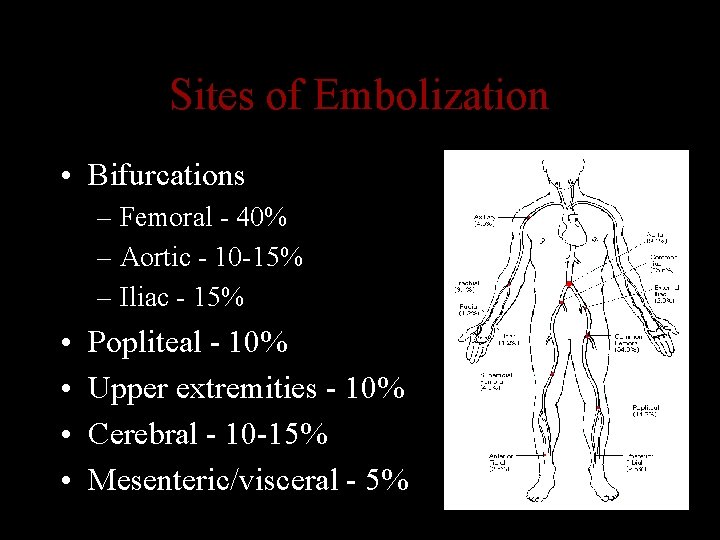
Sites of Embolization • Bifurcations – Femoral - 40% – Aortic - 10 -15% – Iliac - 15% • • Popliteal - 10% Upper extremities - 10% Cerebral - 10 -15% Mesenteric/visceral - 5%

History • The onset and duration of symptoms • Pain – Sudden onset - embolic – Long-standing before acute event - thrombotic • Previous revascularization • Risk factors for atherosclerotic heart disease

6 Ps • • • Pain Pallor Pulselessness Paresthesia Paraparesis Poikilothermia
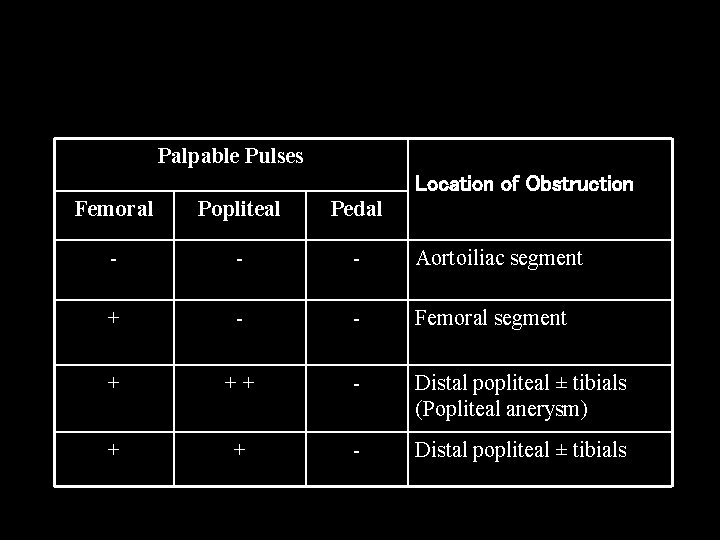
Palpable Pulses Location of Obstruction Femoral Popliteal Pedal - - - Aortoiliac segment + - - Femoral segment + ++ - Distal popliteal ± tibials (Popliteal anerysm) + + - Distal popliteal ± tibials

Management • Arteriography – Operative planning – target vessel – Therapeutic – thrombolysis, angioplasty – Should not delay revascularization & may be obtained intra-operatively • Rapid systemic anticoagulation – Heparin bolus/drip – Prevent propagation of thrombus, distal thrombosis, venous thrombosis • Surgery- Embolectomy • Percutaneous Thrombectomy

Question 6 hours after a femoral-tibial artery bypass for advanced acute ischemia, the lower leg is swollen and painful with palpable pulse. The likely etiology is: A. DVT B. Reperfusion injury C. Thrombosis D. Arterial spasm

Question 6 hours after a femoral-tibial artery bypass for advanced acute ischemia, the lower leg is swollen and painful with palpable pulse. The likely etiology is: A. DVT B. Reperfusion injury C. Thrombosis D. Arterial spasm

Reperfusion injury • Local effects – Oxygen radicals accumulate – Compound cellular insult • Systemic effects – Acid, potassium, cytokines, cardiodepressants accumulate in ischemic limb – Sudden cardiac arrhythmias – Renal failure – Acute lung injury

Prevention and management • Hydration – UO 100 cc/hr • Alkalinization of urine – Prevent myoglobin precipitation in renal tubules • Mannitol – Antioxidant, osmotic diuretic • Insulin/glucose • Fasciotomy

Question Regarding compartment syndrome, which of the following is correct? A. The leg is divided into two compartments--anterior and posterior B. The most commonly affected compartment is the posterior C. The earliest manifestation of acute compartment syndrome is pain D. Patients with compartment pressures greater than 15 mm Hg should undergo fasciotomy

Question Regarding compartment syndrome, which of the following is correct? A. The leg is divided into two compartments--anterior and posterior B. The most commonly affected compartment is the posterior C. The earliest manifestation of acute compartment syndrome is pain D. Patients with compartment pressures greater than 15 mm Hg should undergo fasciotomy
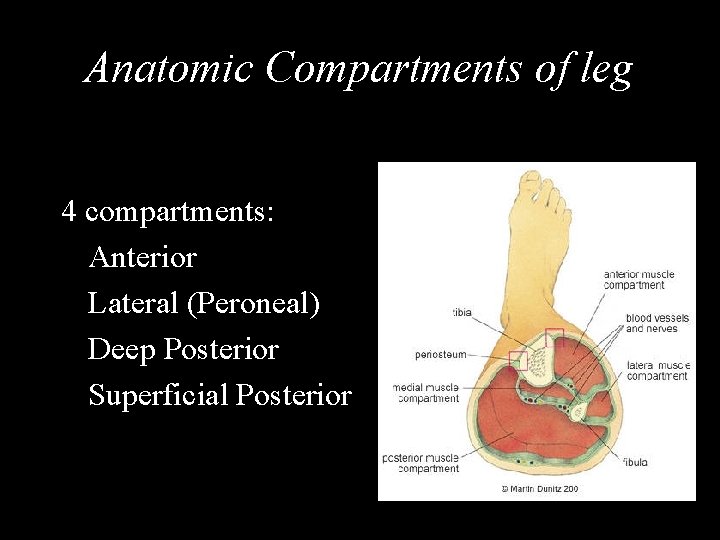
Anatomic Compartments of leg 4 compartments: Anterior Lateral (Peroneal) Deep Posterior Superficial Posterior
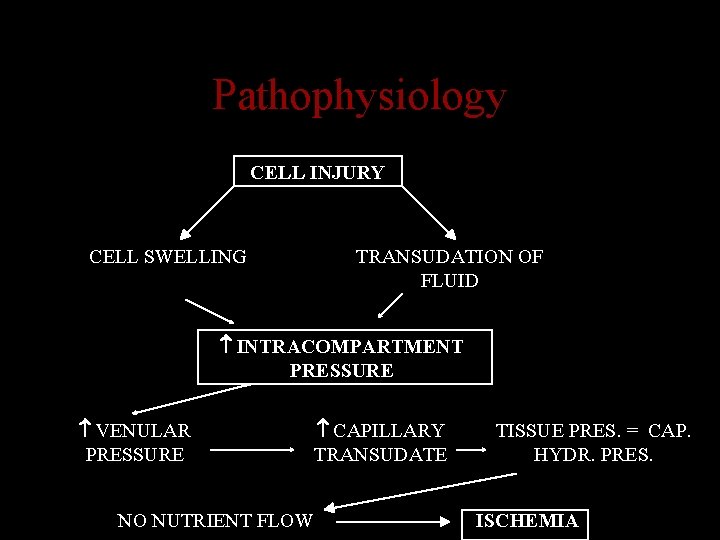
Pathophysiology CELL INJURY CELL SWELLING TRANSUDATION OF FLUID INTRACOMPARTMENT PRESSURE VENULAR PRESSURE NO NUTRIENT FLOW CAPILLARY TRANSUDATE TISSUE PRES. = CAP. HYDR. PRES. ISCHEMIA

Signs and symptoms • Pallor and pulselessness – Not always reliable – Distal pulses may be present • Paralysis - Late symptom • Pain - Severe and out of proportion, increased on passive motion • Paresthesia - Numbness, weak dorsiflexion, numbness in 1 st dorsal web space • Tender, swollen, tense muscle compartments

Indications for fasciotomy • Classically > 40 -45 mm Hg at any point or > 30 mm Hg for 3 -4 hrs • Arterial perfusion pressure is paramount – Mean arterial pressure - interstitial pressure < 30 mm Hg is critical – Diastolic pressure - compartment pressure < 20 mm Hg is critical
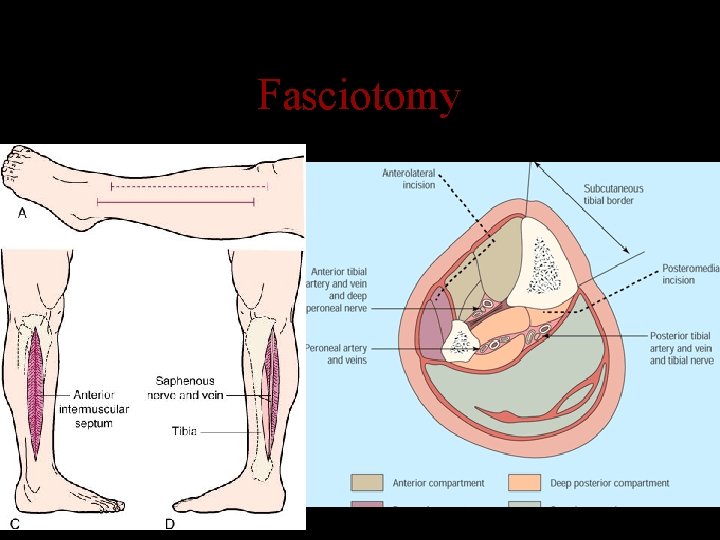
Fasciotomy

Thoracic Outlet Syndrome

Question The most common finding associated with thoracic outlet syndrome is: A. Signs of brachial plexus nerve injury B. Subclavian vein thrombosis C. Subclavian artery aneurysm D. Presence of cervical rib on chest XR

Question The most common finding associated with thoracic outlet syndrome is: A. Signs of brachial plexus nerve injury B. Subclavian vein thrombosis C. Subclavian artery aneurysm D. Presence of cervical rib on chest XR
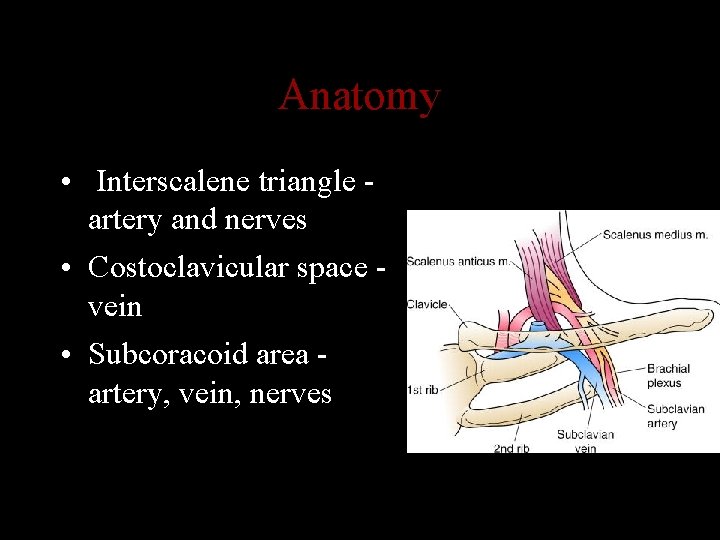
Anatomy • Interscalene triangle artery and nerves • Costoclavicular space vein • Subcoracoid area artery, vein, nerves

Thoracic Outlet Syndrome • Upper extremity symptoms due to compression of the neurovascular bundle in the thoracic outlet area • 3 Types – Neurogenic - most common (95%) – Venous 2 -3% – Arterial 1% • Exacerbated by elevation, abduction, hyperextension of arm

Etiology • Bone - cervical rib, long transverse process of C 7, abnormal first rib, osteoarthritis • Muscles - scalene anomalies • Trauma - neck hematoma, bone dislocation • Fibrous bands - congenital and acquired • Neoplasm • Narrowing of the costoclavicular space – Subclavius muscle, costoclavicular ligament, hypertrophic callus

Management • Conservative – Improvements in postural sitting, standing, and sleeping position – Behavior modification at work – Muscle stretching and strengthening exercises – Successfully treats 50 -90% of patients • Surgery - Transaxillary first rib resection

Buerger’s Disease

Question Which of the following characteristics of Buerger’s disease is true? A. Most commonly observed in young non-smoking females B. It affects mainly the large arteries of the upper ext C. Is characterized by sharply segmental acute and chronic vasculitis of medium-sized and small arteries D. Vascular reconstructive surgery is the main therapy E. Arterial involvement progresses in a proximal to distal fashion

Question Which of the following characteristics of Buerger’s disease is true? A. Most commonly observed in young non-smoking females B. It affects mainly the large arteries of the upper ext C. Is characterized by sharply segmental acute and chronic vasculitis of medium-sized and small arteries D. Vascular reconstructive surgery is the main therapy E. Arterial involvement progresses in a proximal to distal fashion

Buerger’s Disease Thrombangiitis Obliterans • Exclusively associated with cigarette smoking • More prevalent in Middle East and Asia • Occlusive lesions seen in muscular arteries, with a predilection for tibial vessels • Presentation - rest pain, gangrene and ulceration

Buerger’s Disease • Recurrent superficial thrombophlebitis (“phlebitis migrans”) • Young adults, heavy smokers, no other atherosclerotic risk factors • Angiography - diffuse occlusion of distal extremity vessels • Progression - distal to proximal

Buerger’s Disease - Management • Revascularization options are limited • Clinical remission with smoking cessation • Sympathectomy has a limited role in patients with ulcerations
- Slides: 64