Peripheral Vascular Disease Elola Maberry MSN RN Peripheral

Peripheral Vascular Disease Elola Maberry, MSN, RN

Peripheral Vascular Disease • Any condition which causes partial or complete obstruction of the flow of blood to or from the arteries or veins outside the chest.

Chronic Venous Insufficiency • • Obstruction of venous valves Blood refluxs back through valves Vessels wall distend Stretching of the valves which prevents complete closing

Diagnostics • Doppler Ultrasound flow studies • Duplex ultrasound • CT Scans • • CT Angiography Arteriogram Exercise Stress Test Magnetic Resonance Angiography (MRI)

Clinical Manifestations • Intermittent claudication • Coolness • 5 P’s – – – Pain Pallor Pulselessness Paresthesia Paralysis • Nail & skin changes
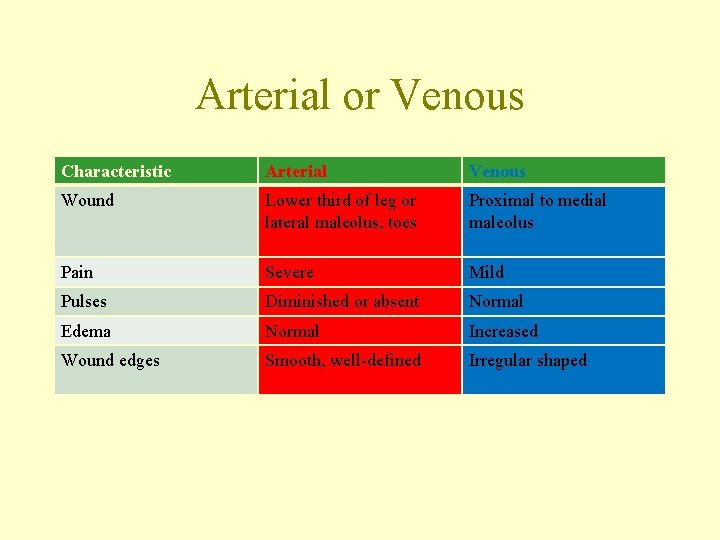
Arterial or Venous Characteristic Arterial Venous Wound Lower third of leg or lateral maleolus, toes Proximal to medial maleolus Pain Severe Mild Pulses Diminished or absent Normal Edema Normal Increased Wound edges Smooth, well-defined Irregular shaped
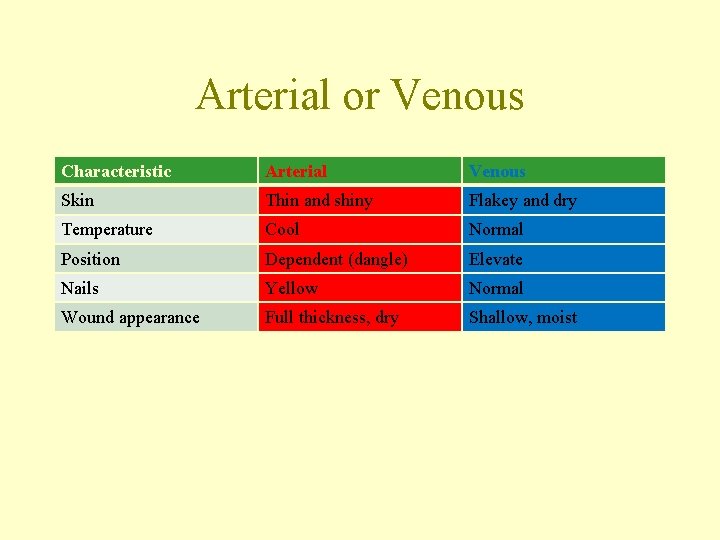
Arterial or Venous Characteristic Arterial Venous Skin Thin and shiny Flakey and dry Temperature Cool Normal Position Dependent (dangle) Elevate Nails Yellow Normal Wound appearance Full thickness, dry Shallow, moist

Arterial or Venous • Arterial Ø Peripheral arterial occlusive disease Ø Buerger’s Disease Ø Arterial Embolism Ø Raynaud Disease • Venous Ø Venous thrombosis Ø Thrombophelebitis Ø Deep vein thrombosis (DVT) Ø Varicose Veins

Warfarin (Coumadin) • Anticoagulant • Action • Therapeutic effect • Side effect

Warfarin (Coumadin) • Anticoagulant • Action • • Therapeutic effect Contraindications Antidote Contingencies • Side effect Nursing Actions • Pt teaching

Surgical Management • Vascular grafting • Endarterectomy • Amputation • PTA • Stent **Treatment depends on location of stenosis or occlusion

Nursing Care • Check pulses • Monitor color, temp. • Maintain tissue integrity • Good nutrition • Patient Education – Avoid • • • leg crossing Nicotine Heating pads Barefoot Constrictive clothing

Management • • Increase blood flow Protect from trauma Prevent ulcers Wound Care

Nursing Diagnosis • Alteration in peripheral tissue perfusion r/t compromised circulation (arterial or venous) • Pain r/t impaired ability of peripheral vessels to supply tissue with oxygen • High risk for impaired skin integrity r/t compromised circulation

Case Study • 69 year old male c/o excruciating left leg pain. Sudden onset, unrelieved with massage/rest, pain does not radiate. Reports a history of left leg aching when he walks long distances • What questions would you like to ask him? • What assessment is necessary?

• • • Past medical history No diabetes, HTN Smoker, social drinker No meds Retired Father died of MI, Mother HTN, CVA

Leg Assessment • Mottled, cyanotic distal to knee, cool to touch- left leg • Right leg is warm and pink • Decreased pulses +1 noted to dorsalis pedis and posterior tibia

• • What is your initial impression? What are the possible causes of his problems? What risk factors can be identified? If problem is not resolved, what potential complications can we expect?

• What therapies could be used to restore perfusion to the leg? • What blood test will be ordered? • With arterial problems, which position will help decrease pain?
- Slides: 19