Is monitoring childhood obesity in Wales feasible Dr

Is monitoring childhood obesity in Wales feasible? Dr C Humphreys

Obesity n n n 60% popn. could be obese by 2050 ‘Obesogenic environment’ Life course component ¨ Early growth patterns (weeks/months) may affect later risk of obesity & disease n Generational component ¨ Parents weight are greatest predictor of obesity Foresight Tackling Obesities: Future Choices – Project report UK Government Foresight programme. Image reproduced with permission.
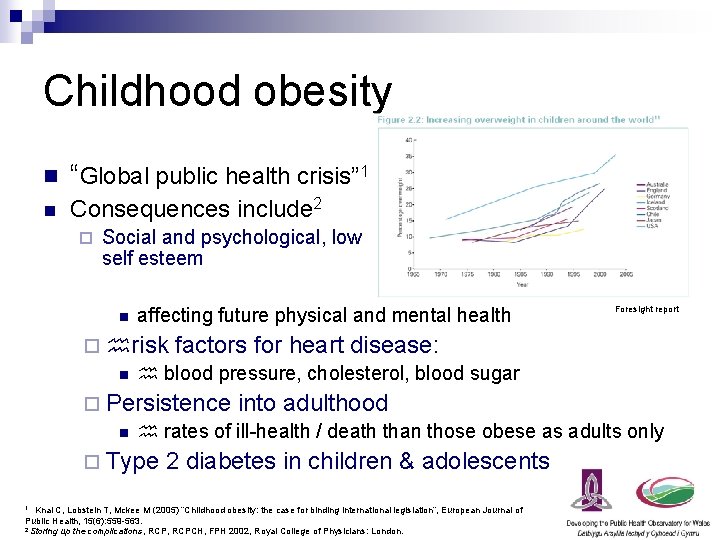
Childhood obesity n “Global public health crisis” 1 n Consequences include 2 ¨ Social and psychological, low self esteem n affecting future physical and mental health Foresight report ¨ risk factors for heart disease: n blood pressure, cholesterol, blood sugar ¨ Persistence into adulthood n rates of ill-health / death than those obese as adults only ¨ Type 2 diabetes in children & adolescents 1 Knai C, Lobstein T, Mckee M (2005) “Childhood obesity: the case for binding international legislation”, European Journal of Public Health, 15(6): 559 -563. 2 Storing up the complications, RCPCH, FPH 2002, Royal College of Physicians: London.

Prevalence of excess body weight WHO Europe Scotland England Wales Prevalence of excess body weight and obesity in children and adolescents. Copenhagen, WHO Regional Office for Europe, 2007: 2 -3 (ENHIS Fact Sheet No 2. 3) Reproduced with permission of WHO Regional Office for Europe Self Reported Heights and Weights. 2001/2.
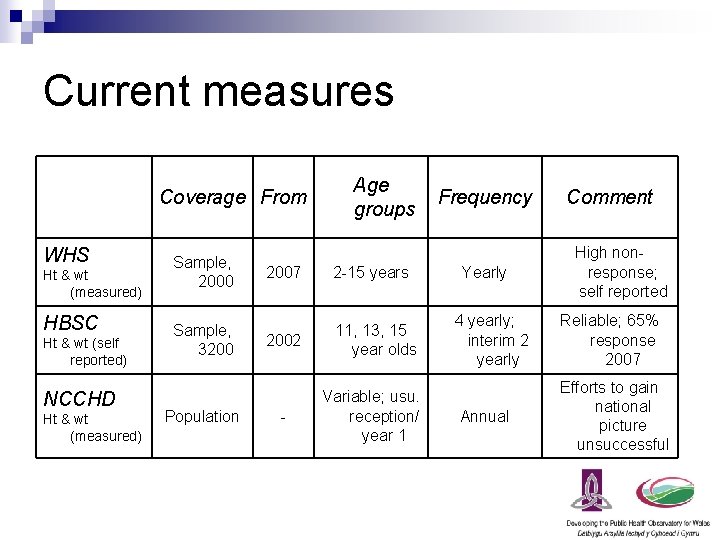
Current measures Coverage From WHS Ht & wt (measured) HBSC Ht & wt (self reported) NCCHD Ht & wt (measured) Sample, 2000 Sample, 3200 Population Age groups 2007 2 -15 years 2002 11, 13, 15 year olds - Variable; usu. reception/ year 1 Frequency Yearly 4 yearly; interim 2 yearly Annual Comment High nonresponse; self reported Reliable; 65% response 2007 Efforts to gain national picture unsuccessful

Feasibility study n Assembly request for pilot 08/09* ¨ Pre-existing measuring systems ¨ NCMP, England (age 4/5 & 11/12) ¨ Legal powers; e. g. giving parents BMI results n Requirement ¨ Local level information – population coverage ¨ Piloting across specific Trusts ¨ To inform standardised national programme *HPV vaccine also introduced

Aim: to inform a standardised national study n National programme would ¨ monitor population trends in (primary school) childhood growth n n including obesity and underweight inform strategies / service development; assess effectiveness of population based interventions ¨ be basis for epidemiological research ¨ n n Surveillance not screening Outcomes relate to Quality of data ¨ Coverage ¨ Acceptability ¨ Cost ¨

The study n Participants ¨ ¨ Reception (NCMP) & Year 4 (COSI) State schools in 5 former Trust* areas n n n Randomisation ¨ Cluster (school) randomised for consent (year 4) n ¨ n Pembs & Derwen; North East Wales; Powys; North Glamorgan; Swansea (part) 30% of Wales population of age groups Opt in versus Opt out, to assess effect on uptake of measures Ethical approval obtained Feedback on request ¨ Three of five Trusts *Including Powys Teaching LHB

The study n Measurement ¨ Community/school nursing services ¨ Training, instruments n Data recording ¨ Community Child Health 2000 System (empty fields) ¨ National Community Child Health Database n Qualitative study ¨ Children, Parents, staff Image reproduced with permission from parent & child

Results n 14, 100 children measured ¨ n Quality of data – mostly very high ¨ ¨ ¨ n School code & exam date ≥ 99. 7% all areas Dob/gender 100% all areas Ethnicity <50% all areas (0. 7% in one Trust) Data from one Trust (N Wales) missed cases ¨ n 457 schools Some of those not consenting to measurement Height & weight data quality ¨ ¨ Very good quality ≥ 99. 4 had BMI within plausible range
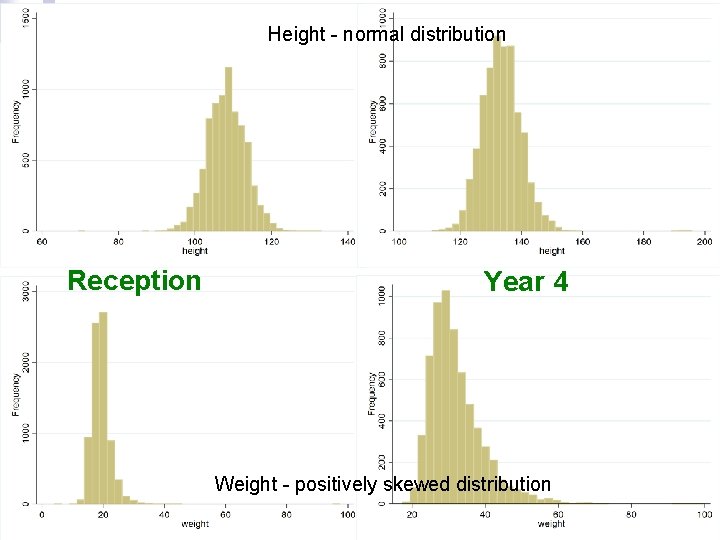
Height - normal distribution Reception Year 4 Weight - positively skewed distribution
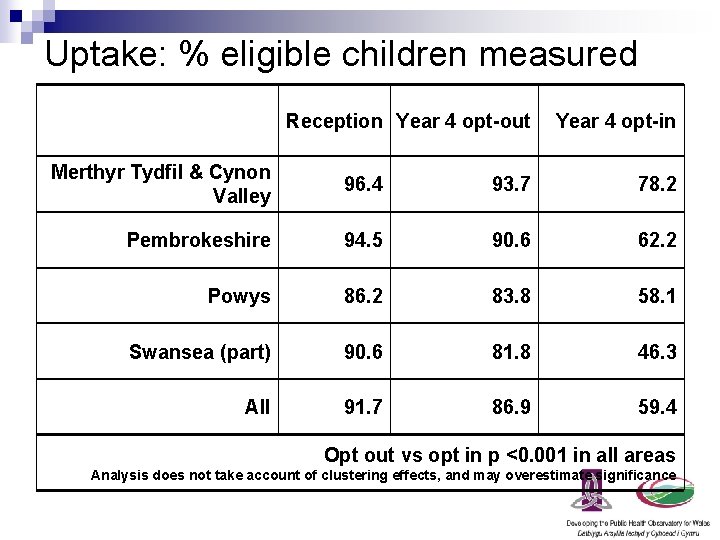
Uptake: % eligible children measured Reception Year 4 opt-out Year 4 opt-in Merthyr Tydfil & Cynon Valley 96. 4 93. 7 78. 2 Pembrokeshire 94. 5 90. 6 62. 2 Powys 86. 2 83. 8 58. 1 Swansea (part) 90. 6 81. 8 46. 3 All 91. 7 86. 9 59. 4 Opt out vs opt in p <0. 001 in all areas Analysis does not take account of clustering effects, and may overestimate significance
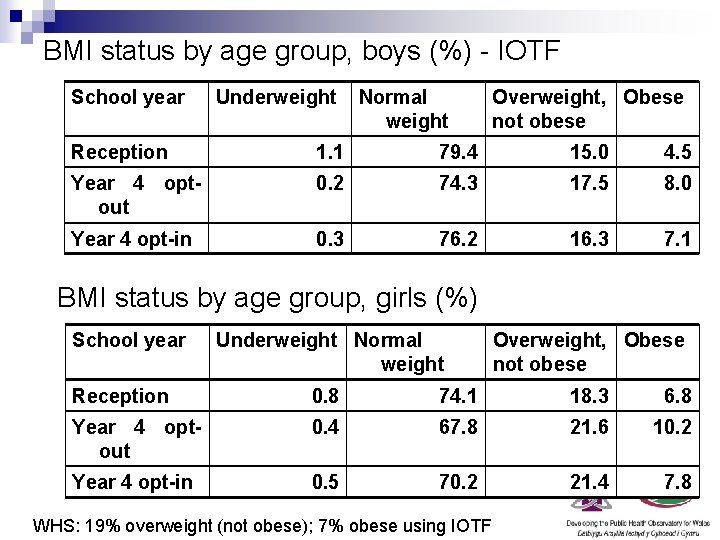
BMI status by age group, boys (%) - IOTF School year Underweight Normal weight Overweight, Obese not obese Reception 1. 1 79. 4 15. 0 4. 5 Year 4 optout 0. 2 74. 3 17. 5 8. 0 Year 4 opt-in 0. 3 76. 2 16. 3 7. 1 BMI status by age group, girls (%) School year Underweight Normal weight Overweight, Obese not obese Reception 0. 8 74. 1 18. 3 6. 8 Year 4 optout 0. 4 67. 8 21. 6 10. 2 Year 4 opt-in 0. 5 70. 2 21. 4 7. 8 WHS: 19% overweight (not obese); 7% obese using IOTF
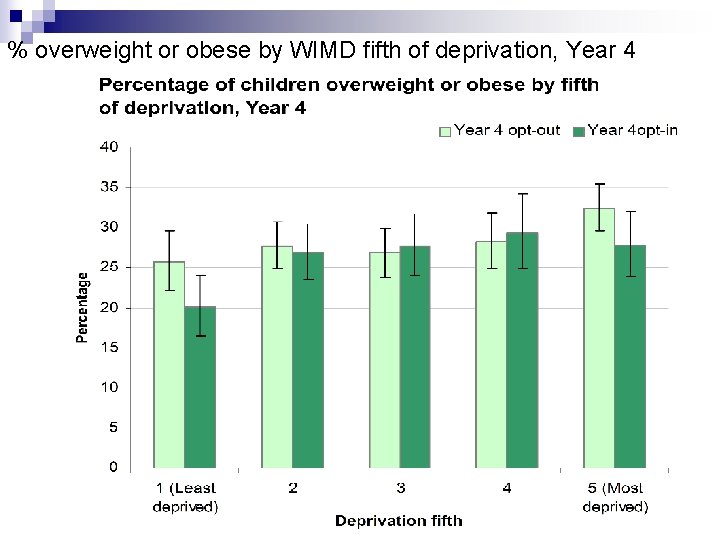
% overweight or obese by WIMD fifth of deprivation, Year 4

Interviews with children, parents & staff n Qualitative study: semi-structured interviews ¨ 10 children ¨ 10 parents ¨ 12 staff n Interviews took place after measurement phase n All interviews recorded, transcribed analysed according to standard qualitative research methods

Qualitative study: key results 1 n Some children were comfortable with being measured, others less so. Areas for improvement: ¨ Privacy including avoiding use of ‘holding area’ ¨ Being accompanied by a familiar adult n Awareness of reasons why measured ¨ Children not aware ¨ Parents and staff mostly aware that it was about population monitoring ¨ Difficulty separating such a programme from taking measures to manage individual children

Qualitative study: key results 2 n Staff more concerned about consent method than parents n Parents and children expressed interest in knowing the results of measurements n Staff found programme was work intensive – especially providing results to parents

Feedback of results n 1, 722 results returned (41% of 4, 202) 70% of opt-in v 27% of opt-out (N Wales) ¨ 70% ‘normal weight’; 29% overweight/very overweight* (Pembs) ¨ n Dedicated phone line & website (hosted by NHS Direct) 11 calls (4 answered) ¨ 7 website hits ¨ n GP survey (Pembs) ¨ n No impact on service (75% response) Nursing service – 1 enquiry relating to results Using clinical cut offs rather than IOTF

Some key conclusions n n n It is feasible to measure ht & wts in primary schools It is feasible to use CCH 2000/NCCHD Data quality good ¨ But changes required to CCH 2000/NCCHD n Opt-out had large impact on uptake ¨ Effect on measured obesity may vary by deprivation n Programme acceptable ¨ But communication, especially with children, could be improved

Next steps n Report to Assembly to inform Minister ¨ June 2009 ¨ Included 28 recommendations n Ministerial submission expected ¨ Oct 2009 n Recommendations from Assembly

Thanks n n Children Parents Nathan Lester (contributed to slides) Other NPHS staff ¨ ¨ Angela Jones Thriveni Beerenahally Sharon Hillier Judith Greenacre n Trust staff ¨ n Swansea University ¨ ¨ n n Anne Farr, Sandra Jones, Lesley Taylor, Yvonne Harding, Susan Jones, and Helen Jones and Paula Davies Rhys Williams Centre for Child Health Research: Justine Howard, Helen Elton HSW esp Louise James, David Jones NHS Direct

- Slides: 22