Child and Adult Obesity in Ohio 2008 Ohio

Child and Adult Obesity in Ohio: 2008 Ohio Family Health Survey Supporting Decision-Making Through Research: Findings from the 2008 Ohio Family Health Survey Leona Cuttler, M. D. * Lisa Simpson, MB, BCh, MPH^ JB Silvers, Ph. D* Andrew Gallan, Ph. D* Ann Nevar, MPA* Mendel Singer, Ph. D* *The Center for Child Health and Policy at Rainbow Babies & Children’s Hospital, Case Western Reserve Univ. ^Child Policy Research Center, CCHMC, Univ. of Cincinnati

We hear a lot about Obesity…

…But what are the actual data? ? …. . impact on health during childhood? and adulthood? …. . in Ohio now? - rates of childhood & adult obesity? - policy-relevant risk factors? - impact on health? health services? - implications for policy?

Does Childhood Obesity Really Have an Impact? Health during childhood Psychological poor quality of life, depression, ADHD, eating disorders (cause? ) Sleep Apnea 3 x rise over 30 yrs 25% obese Asthma Cardiovascular: 2 -fold rise in obese • Hypertension (2. 5 -3. 7 x inc) • Dyslipidemia • Risk factors: 60% of obese 5 -10 yo have > 1 risk factor • Metabolic syn (30% obese) Gallstones Fatty Liver Type 2 Diabetes: Up to 50% in obese Bone disease Arthritis, SCFE up to 45% new onset pediatric diabetes

Does Childhood Obesity Really Have an Impact? Health during Adulthood Childhood obesity tends to persist into adulthood, and predisposes to: • Diabetes • Cardiovascular disease • Cancer (colon, pancreas, breast, etc. ) • and much more

Obesity: 1 of 3 Americans to develop diabetes
Childhood obesity increases the risk of adult heart disease Obese at 7 -13 y higher risk of heart disease after age 25 y Current adolescent obesity will cause 100, 000 excessive cardiac deaths by 2035

Adult obesity impacts health and costs Medical costs of obese 37% more than normal weight Obesity accounted for 27% of the rise in inflationadjusted per capita spending between 1987 -2001

What is the current state of child and adult obesity in Ohio? Sponsored by: The Ohio Family Health Survey 2008 Funded by: State of Ohio Departments of Insurance, Job and Family Services, Health, and Mental Health Directed by: Ohio Colleges of Medicine Government Resource Center at The Ohio State University and the Health Policy Institute of Ohio

The Ohio Family Health Survey • Telephone interviews: 50, 092 households • Adults: height, weight, health • If child between 10 -17 yrs in household: child’s height, weight, health (n= 6086) provided by adult (86% parents) • Body Mass Index (BMI) calculated – Classification of BMI: underweight, healthy, overweight, obese

Obesity: terminology • Body Mass Index (BMI) is used to assess “fatness” • “Overweight” refers to individuals who are above normal weight but not obese (children: BMI 85 th-94 th percentile; adults: BMI 25 -29. 9 kg/m²) • “Obese” refers to individuals who are markedly above normal weight (children: BMI> 95 th percentile; adults: BMI > 30 kg/m²)
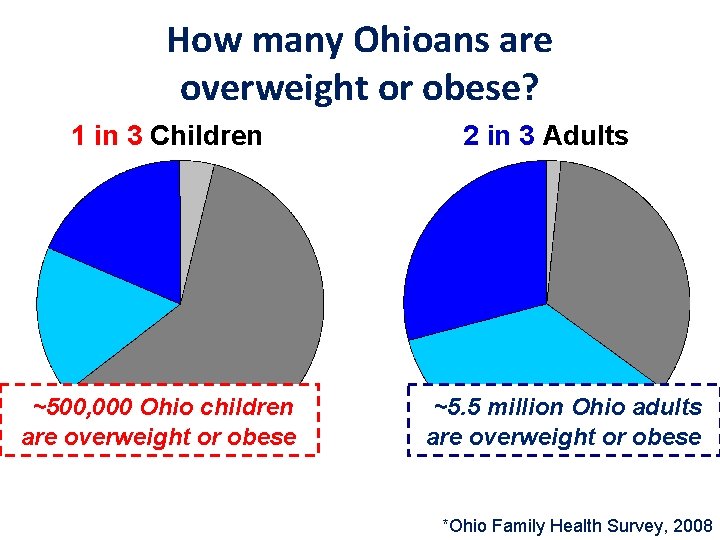
How many Ohioans are overweight or obese? 1 in 3 Children ~500, 000 Ohio children are overweight or obese 2 in 3 Adults ~5. 5 million Ohio adults are overweight or obese *Ohio Family Health Survey, 2008
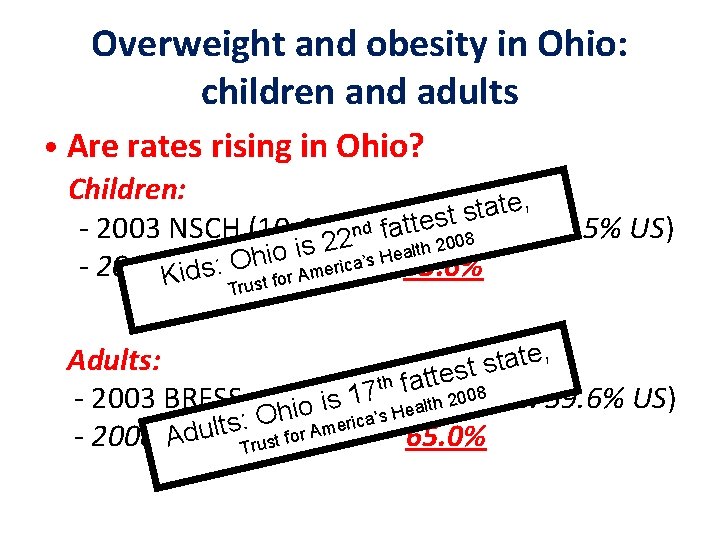
Overweight and obesity in Ohio: children and adults • Are rates rising in Ohio? Children: , e t a t s ttest 08 (vs. 30. 5% US) nd fa 30. 5% - 2003 NSCH (10 -172 y): 2 ealth 20 s i o i h O ca’s H 35. 6% i r : e - 2008 KOFHS (10 -17 y): s m A id st for Tru , e t a Adults: t s st th fatte 2008 (vs. 59. 6% US) - 2003 BRFSS: hio is 17’s H 60. 9% h t l a e a O c i : r e s - 2008 OFHS: 65. 0% Adult Trust for Am
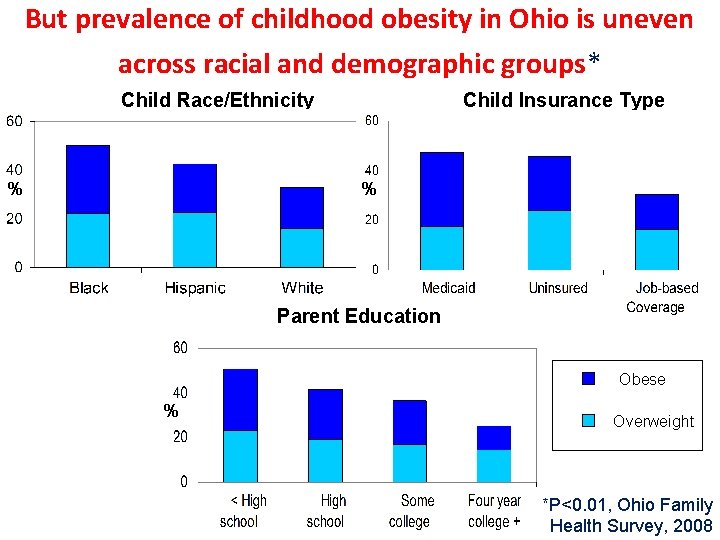
But prevalence of childhood obesity in Ohio is uneven across racial and demographic groups* Child Race/Ethnicity % Child Insurance Type % Parent Education Obese % Overweight *P<0. 01, Ohio Family Health Survey, 2008
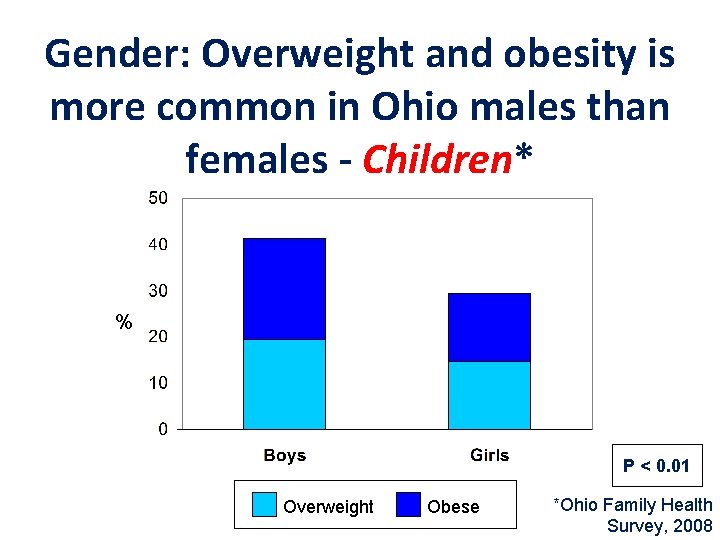
Gender: Overweight and obesity is more common in Ohio males than females - Children* % P < 0. 01 Overweight Obese *Ohio Family Health Survey, 2008
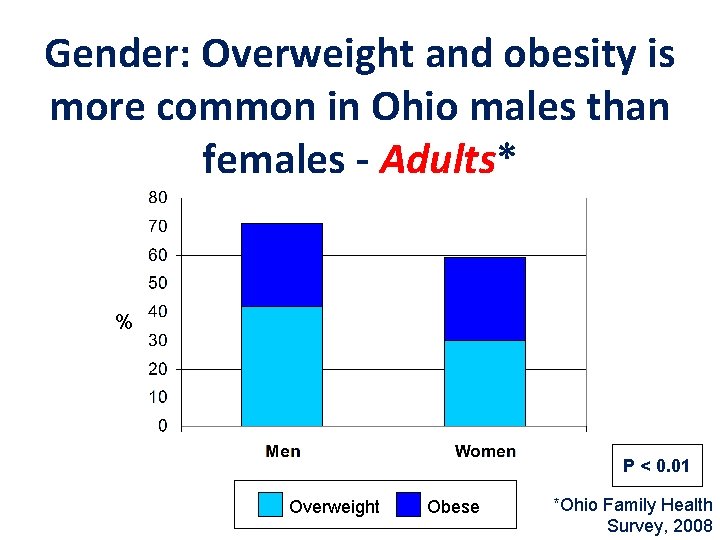
Gender: Overweight and obesity is more common in Ohio males than females - Adults* % P < 0. 01 Overweight Obese *Ohio Family Health Survey, 2008
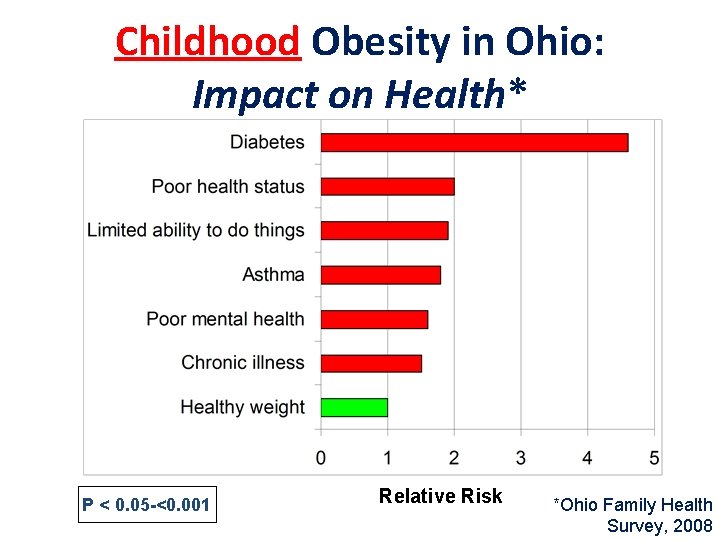
Childhood Obesity in Ohio: Impact on Health* P < 0. 05 -<0. 001 Relative Risk *Ohio Family Health Survey, 2008
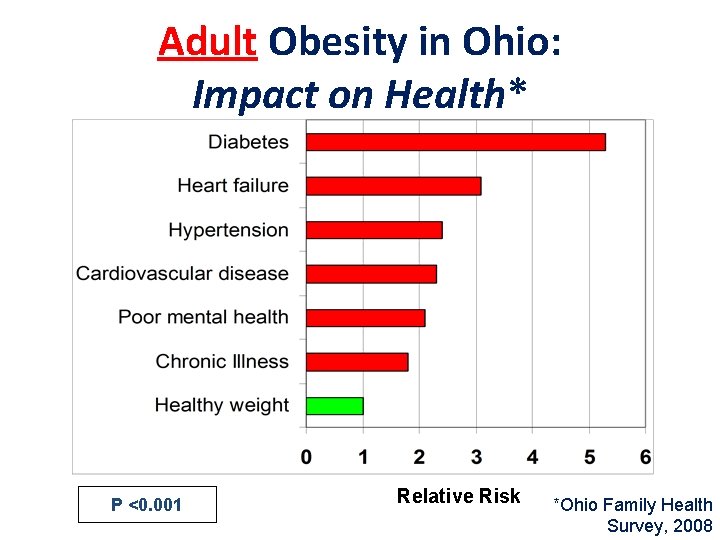
Adult Obesity in Ohio: Impact on Health* P <0. 001 Relative Risk *Ohio Family Health Survey, 2008

Obese Ohioans need more health services than those who are normal weight (P<. 01) Children Adults • Special health care needs: 1. 4 -fold higher 1. 6 -fold higher • Chronic medications: 1. 4 -fold higher 1. 6 -fold higher • Emergency room visits – Two or more: 1. 8 -fold higher 1. 5 -fold higher • Hospitalizations – Two or more: 2. 1 -fold higher 1. 5 -fold higher

Therefore, obesity is currently a major public health threat to Ohio: prevalence, impact on health, use of health resources • What should we do about it? • Do the data help identify policy directions?

Given the scope of the problem, policy is important to address obesity 1. 2. 3. 4. 5. 6. 7. Start young Target parent + child Not focus on a single geographic region Multilevel approach: global + some subgroups Change perceptions of health, food, activity Develop policies for prevention + treatment Consider defining obesity as a chronic disease

1. Start Young If we want to overcome obesity in Ohio, we have to target children because: • Obesity starts very young, and becomes more prevalent with advancing age
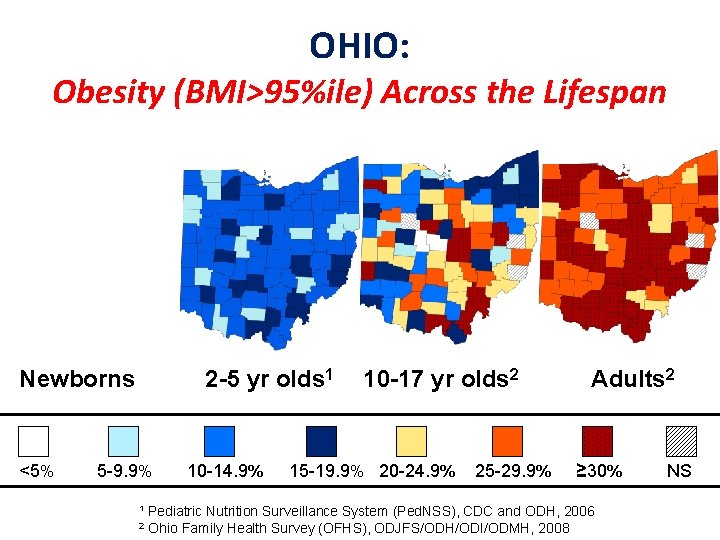
OHIO: Obesity (BMI>95%ile) Across the Lifespan Newborns <5% 2 -5 yr olds 1 5 -9. 9% 10 -14. 9% 10 -17 yr olds 2 15 -19. 9% 20 -24. 9% 25 -29. 9% Adults 2 ≥ 30% ¹ Pediatric Nutrition Surveillance System (Ped. NSS), CDC and ODH, 2006 2 Ohio Family Health Survey (OFHS), ODJFS/ODH/ODI/ODMH, 2008 NS

1. Start Young If we want to overcome obesity in Ohio, we have to target children because: • Obesity starts very young, and becomes more prevalent with advancing age • Obese children generally become obese adults

2. Target Parents + Children • Parent obesity is a strong independent predictor of childhood obesity
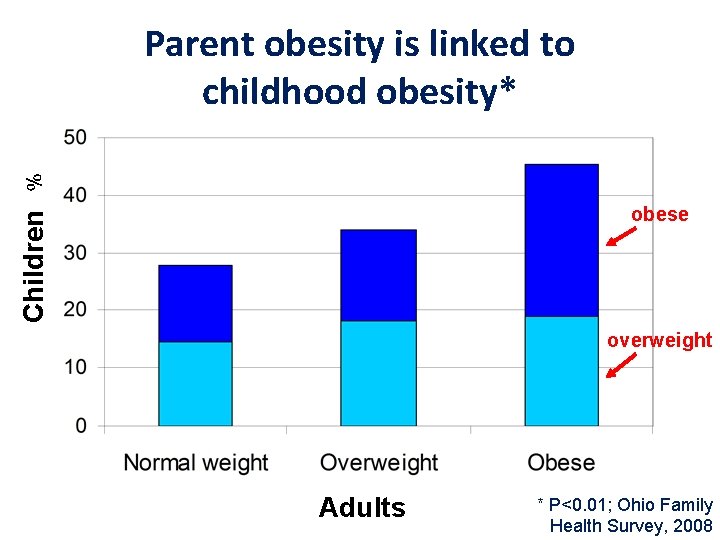
% Parent obesity is linked to childhood obesity* Children obese overweight Adults * P<0. 01; Ohio Family Health Survey, 2008

2. Target Parents + Children • Parent obesity is a strong independent predictor of childhood obesity • Targeting parents includes focus on their educational attainment
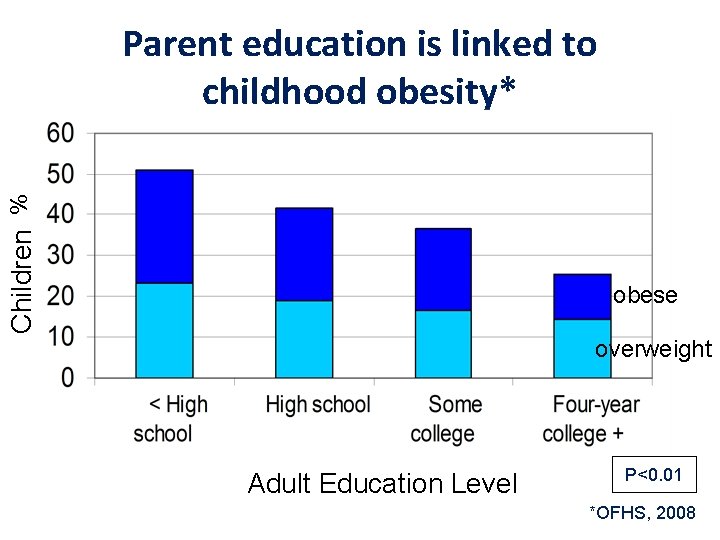
Children % Parent education is linked to childhood obesity* obese overweight Adult Education Level P<0. 01 *OFHS, 2008

3. We should not focus on a single geographic region Obesity is not easily targeted geographically: • Child and adult obesity is widespread in OH • No specific region or type of region is dominant
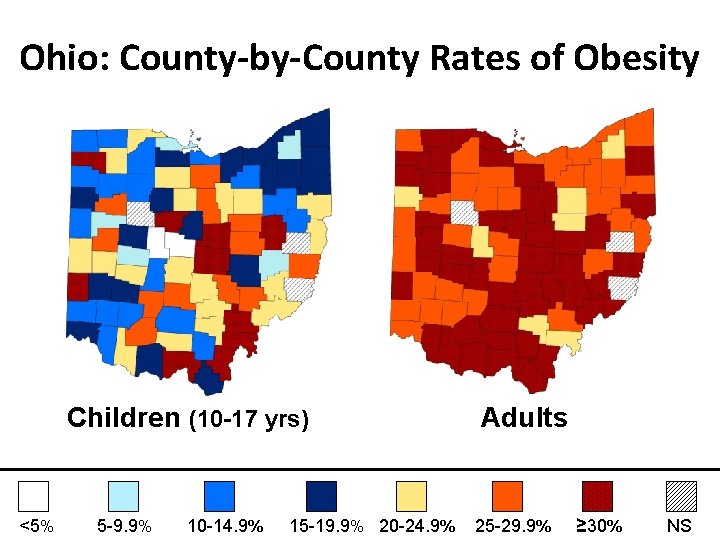
Ohio: County-by-County Rates of Obesity Children (10 -17 yrs) <5% 5 -9. 9% 10 -14. 9% 15 -19. 9% 20 -24. 9% Adults 25 -29. 9% ≥ 30% NS

4. Consider multilevel approach, recognizing demographic subgroups Independent risk factors for obesity CHILD ADULT more likely Male (vs female) Medicaid (vs job-based) Income 100 -200% FPL (vs >300% FPL) Black female (vs white female) 1. 8 x 1. 3 x 1. 3 1. 4 x 1. 2 x 1. 8 x 1. 5 x

In addition, other independent risk factors for childhood obesity Children: more likely to be obese – 10 -11 Years-Old (vs 16 -17 years-old) 2. 2 -fold – Adult is Obese (vs healthy weight) 1. 7 -fold – Adult High School (vs 4 year college) 1. 4 -fold

Other policy recommendations 5. Change perceptions of health, food, and activity 6. Develop policies that address prevention and treatment 7. Consider defining obesity as a chronic disease

Summary (1) In Ohio: • 35. 6 % of children and 65% of adults are overweight or obese • Rates of obesity differ according to demographic factors (gender, race, income, insurance, and parent education) • Obesity is associated with both - a substantial increase in diseases, and - marked increased use of health resources

Summary (2) • 1. 2. 3. 4. 5. 6. 7. The extent/impact of obesity suggest that policy interventions are needed. The data suggest: Start young Target parent + child Not focus on a single geographic region Multilevel approach: global + some subgroups Change perceptions of health, food, activity Develop policies for prevention + treatment Consider defining obesity as a chronic disease

Summary (3) • Act now. When is the evidence enough? When the problem is big enough: Get data Act on best available evidence Re-evaluate Modify

Thank you • Thanks to Ohio Dept. of Job and Family Services, Ohio Dept. of Health, Ohio Dept. of Insurance, and Ohio Dept. of Mental Health, OSU-HPIO • Thanks to Rainbow Board of Trustees • Research team: Leona Cuttler, A. Gallan, Ann Nevar, JB Silvers, Mendel Singer, Lisa Simpson • Reviewer team: Cynthia Burnell, James Gearheart, Lorin Ranbom, Barry Jamieson
- Slides: 37