Introduction to Contact Lenses Amy C Nau History






























- Slides: 32

Introduction to Contact Lenses Amy C. Nau

History • 1636 described by Descartes • 1886 first therapeutic lens to aid healing after cataract surgery • 1888 first lens for KC- scleral • 1899 -1912 first concepts of the corneal lens • 1930’s non glass materials • 1948 corneal lenses developed • 1950’s hydrogels • 1970’s rgp • 1990’s silicone hydrogel materials

Demographics • • 32 million Americans wear lenses 98% single vision 2% bifocal 87% soft 12% rgp 1% pmma 66% disposable

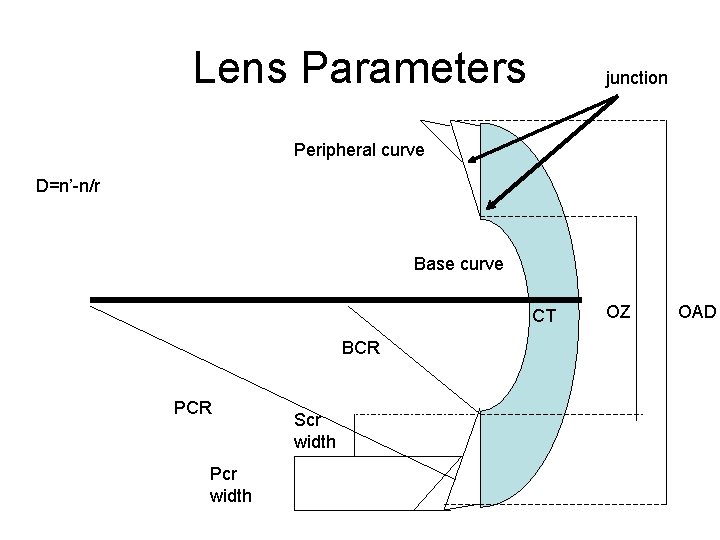
Lens Parameters junction Peripheral curve D=n’-n/r Base curve CT BCR Pcr width Scr width OZ OAD

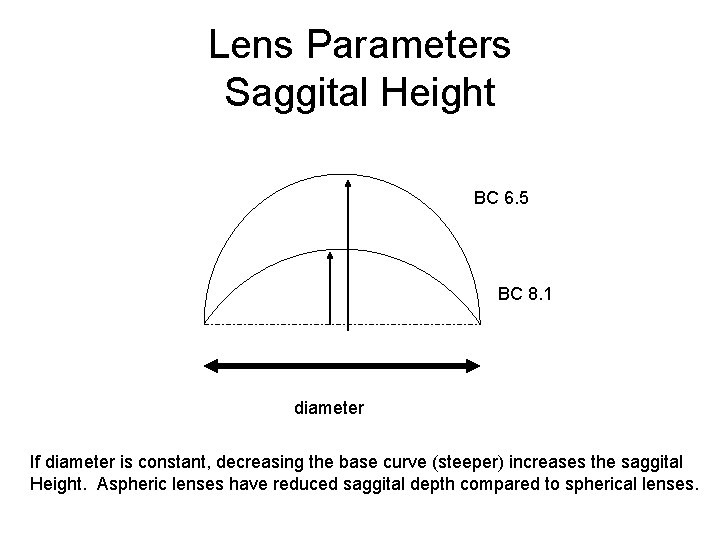
Lens Parameters Saggital Height BC 6. 5 BC 8. 1 diameter If diameter is constant, decreasing the base curve (steeper) increases the saggital Height. Aspheric lenses have reduced saggital depth compared to spherical lenses.

Anatomy of the Contact Rx • Brand/BC/power/diameter/oz/ct/peripheral curve details/material

Oxygen • Dk- measures oxygen permeability of a material. D= diffusion coefficient for oxygen movement in the material k=solubility constant of oxygen in material • Dk/t= the Dk value divided by the center thickness (t). Measures oxygen transmissibility

Lens Designs • Aspheric – Peripheral only, total, bi(posterior OZ/ant pc) • • Ballasted (prism) Fenestrated Lenticular (aphakia) Toric – FST, Bi • Truncated

Lens Materials • RGP • PMMA • Silicone acrylate Dk 15 -55 • Fluoropolymer (FLP) Dk up to 150 • Soft • HEMA (hydroxyethylmethacry late) – Absorbs water. 10% increase = doubles Dk – Water content 37 -79% – Excellent wettability • Silicone Hydrogel – Deposit resistant – Siloxane + cross linker – (non silicone polymers) – Hydrophobic – Reduced water content

Instruments • • Keratometer Lensometer- convex side up (bvp) Slit lamp Topography Radiuscope CL comparators-project image 20 x Thickness gauge

Patient Evaluation • Contraindications – – – Chronic blepharoconjunctivitis Recurrent/inflamed pterygium or pinguecula Bells Palsy with corneal anesthesia Poor hygeine Chemical exposures Severe allergy Inability to handle lens Very dry eye TED Uncontrolled Dm AIDS?

History • • Full medical hx Ocular hx Medication hx Contact lens hx Spectacle hx Hobbies/occupational needs Motivation

Conditions that cause problems • • • Chronic allergy Dry eye GPC Recurrent infections Sometimes prior sx Neovascularization Sometimes strabismus Pregnancy Antihistamine use, OCP Mental status Age +/Lens noncompliance

Physical Examination • Visual acuity / MR • Lid assessment (include upper and lower tarsus), blink patterns, mgd/bleph, apeture • Basic dry eye workup (tbut, LG, Na. Fl, Zone quick) • Corneal status/health, esp epi, old scars and neo • Pupil size, HVID • Keratometry/corneal shape

Lens Selection • • Motivation Current lens problems= need to solve Occupational needs Cosmetic needs Maintain health of eye Cost Compliance

Selection Process- Advantages and Disadvantages • SOFT • RGP Once the modality is selected, next step is to pick the material and the solution Finally, brand power

Soft Lenses • BC range 6. 0 to 11. 0 but most are 8. 4 to 9. 0 • Power range -55 D to +60 D but most are +/ - 10 D • Diameter 11. 0 to 24. 00 mm but most are 13. 00 to 15. 00 mm Tyler’s quartery is an invaluable resource

Soft Classifications • Water Content – Low 37 -45% (DW); medium 46 -58%; high 59 -79% (EW) – More water = thicker – Ionicity • Manufacturing process – Spin casting, lathe cutting, cast molding • • Lens design Function (DW, EW, prosthetic etc) Color Bifocal/monovision Therapeutic (bandage, cosmetic Aphakic Toric (double slab off, prism ballast, truncation) Thickness

Extended Wear • • • Use with caution Make sure eye is healthy Compliant pt Understand accept risk Willing to have regular f/u Willing to remove lenses and wear glasses if needed. Remove q 6, clean leave out for 24 h if possible then reinsert EW risk of UK 20. 9/10 K versus 4. 1 per 10 K

F/U visit for EW • • Acute hypoxia (CLARE) Microcystic edema GPC K neo Striae Infiltrates SPK If found, d/c EW.

Soft fitting evaluation • • • Well centered 0. 5 to 1. 0 mm movement with blink Limbal coverage (at least 1. 0 mm beyond) Stable vision Three point touch

Troubleshooting • Decentration- steepen bc or increase diameter, no spin cast lenses • Late decentration- look for deposits, GPC • Minus OR- flatten BC • Unstable VA- flatten BC if sphere (flexure) – Tight lens clear after blink, loose lens burred after blink • Unstable VA (toric) steepen BC, increase diameter, change modality • Too tight- flatten BC or reduce diameter

Follow up • Be clear about lens regimen • Make sure they can I/R • F/U usually about 3 -4 weeks with cls on 4+hours • VA, OR, fit assessment, remove lens, examine for problems, stain with Na. Fl

CL problem • RX: • OD: -6. 75 -2. 75 x 165 • Os: -8. 00 -0. 75 x 180

RGP lenses- fitting philosophies • • Small and thin-max tear circulation and oxygen Vault apex Small cornea= steep; large cornea = flat Small and steep lens ; large and flat lens On flat K Steeper or flatter than K IP, bit steeper than K, smaller diameter, thin edges • LA (increased comfort); flatter than K, larger

RGP fitting technique • Select the fit you want to use for the pt based on physical exam, MR and K. • Select diagnostic lens if available, evaluate fit, perform OR. • Select material you want to use • Select care regimen

RGP fitting- determining lens power and base curve • Must have MR and Keratometry

RGP fitting- problem

RGP fit- troubleshooting • Discomfort- lens edge (too thick, too sharp, poor blend) • Excessive movement- too flat, limbus irritated. Steepen bc or increase diameter. • Too tight- edema, discomfort, redness. Flatten BC, decrease diameter, flatten PC • Vision-OR, flexure, decentration, deposits, incorrect power • Poor wetting d/t partial blink • Deposits- enzyme, surfactants, change material, plasma tx • Flexure- Over K, increase CT, stiffer material, reduce OAD, reduce OZ • Solution hypersensitivity- try one with different preservative.

Solutions/Lens Care • Surfactants to solubilize debris/mucous/lipids. Remove surface contaminants. RUB and RINSE off. • Disinfection-killing infectious organisms – Chemical, hydrogen peroxide, thermal, UV • Enzyme cleaners remove deposits chemically bound to the lens (lipoprotein, denatured lysozyme) – Papain, pancreatin, subtilisin

Solutions/Lens Care • Wetting agents- reduce wetting angle making lens more comfortable (rgp) q

Follow up • Lens care regimen, insertion and removal and wearing schedule should be outlined • F/U in about one month with cls on 4 h • Visual acuity, OR, lens evaluation, remove lens and evaluate eye.