CARIN Consumerfacing Realtime Pharmacy Benefit Check Connectathon Approach

CARIN Consumer-facing Real-time Pharmacy Benefit Check: Connectathon Approach

Connectathon Overview • • • An HL 7 FHIR® Connectathon is a two-day event of hands-on FHIR development and testing held in conjunction with Working Group Meetings. The event provides an opportunity for implementers and developers to gain experience developing FHIR -based solutions and exchange data with other FHIR interfaces. The Connectathon is not a formal tutorial and there are no lectures or presentations. Participants engage in hands-on, heads down development and testing, working directly with other FHIR developers and senior members of the FHIR standards development team. © 2018 LEAVITT PARTNERS Please visit the CARIN Consumer-Facing RTPBC Connectathon Page for more information and to sign up! https: //confluence. hl 7. org/pages/viewpage. action? page. Id=58654805 2

CARIN Consumer-facing RTPBC Use Cases Overview: Consumer has been prescribed a medication and is looking up the prescription price and/or formulary/benefit information and potentially a location to dispense their prescription on a stand-alone app. Two initial use cases: 1. 2. Lowering patient out-of-pocket cost for initial prescription fill Pricing alternatives for an existing prescription Objectives: • Consumer wants to understand their Rx out of pocket cost, which includes deductible, donut hole, etc. • Include verbiage that says the OOP costs are based on an estimation based on a point in time • Consumer wants to understand their formulary and benefit information (There will be a covered or not covered indicator sent to the member; there is also an explanation as to why it’s not covered) • Consumer wants to understand who their prescribing provider is • Consumer wants to determine their price alternatives, which includes their cash price (Good. Rx) • Simplify or eliminate the prior authorization process • Determine therapeutic alternatives that are covered • Determine any step therapy that may be required © 2019 LEAVITT PARTNERS 3
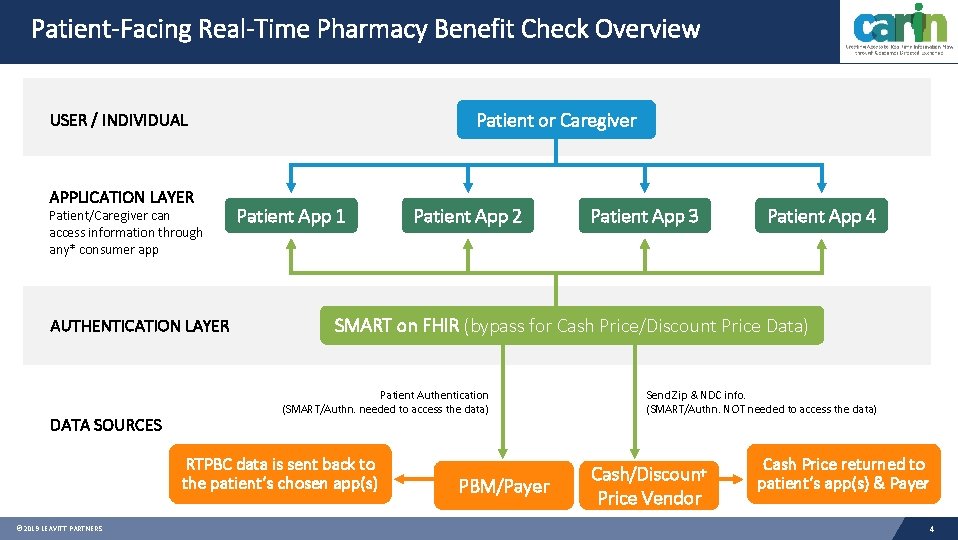
Patient-Facing Real-Time Pharmacy Benefit Check Overview Patient or Caregiver USER / INDIVIDUAL APPLICATION LAYER Patient/Caregiver can access information through any* consumer app AUTHENTICATION LAYER DATA SOURCES Patient App 1 Patient App 3 Patient App 4 SMART on FHIR (bypass for Cash Price/Discount Price Data) Patient Authentication (SMART/Authn. needed to access the data) RTPBC data is sent back to the patient’s chosen app(s) © 2019 LEAVITT PARTNERS Patient App 2 PBM/Payer Send Zip & NDC info. (SMART/Authn. NOT needed to access the data) Cash/Discount Price Vendor Cash Price returned to patient’s app(s) & Payer 4

Pre-Conditions Preconditions • Member is eligible with a health plan and can access their formulary and benefit information • Member has received a Username/Password from their health plan member portal only for access to their formulary and benefit information • Member will choose any app they want; there is no integration with the EHR © 2019 LEAVITT PARTNERS 5

Workflow • Consumer chooses app which has the ability to access the consumer-facing RTPBC • Application manages the medication list (FHIR etc. ) or allows for medication look up feature • Consumer enters the name of the drug and the application displays the Formulary and Benefit information and out of pocket cost information • App will send the prescription information (representative NDC, actual NDC or Rx. Norm) • PBM will return the appropriate information (the application will choose from the following) • Current RTPBC data based on objective • Cash pricing app will return cash pricing information per pharmacy based on the functionality within the end user’s application • NDC information • Zip Code © 2019 LEAVITT PARTNERS 6

Use Case #1: Lowering Patient Out of Pocket Cost for Initial Fill
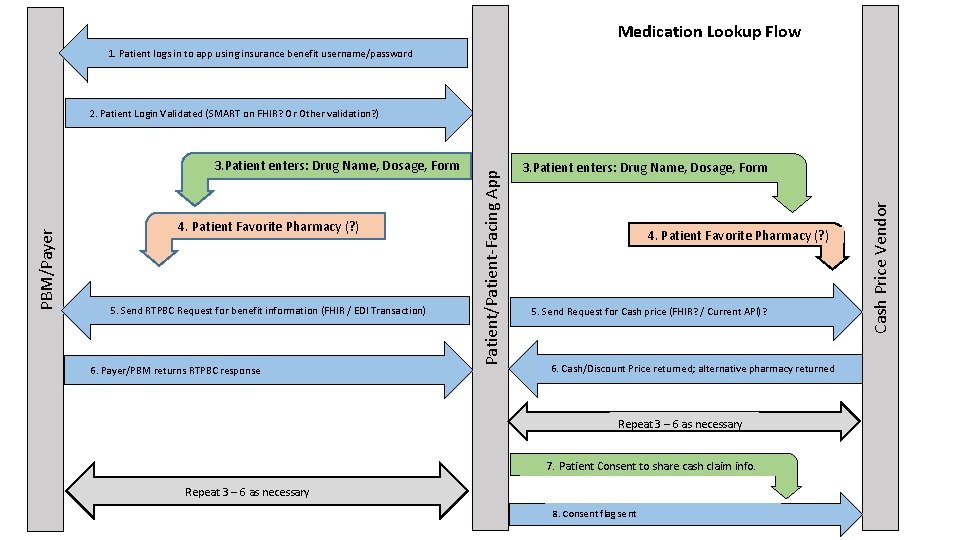
Medication Lookup Flow 1. Patient logs in to app using insurance benefit username/password 4. Patient Favorite Pharmacy (? ) 5. Send RTPBC Request for benefit information (FHIR / EDI Transaction) 6. Payer/PBM returns RTPBC response 3. Patient enters: Drug Name, Dosage, Form 4. Patient Favorite Pharmacy (? ) 5. Send Request for Cash price (FHIR? / Current API)? 6. Cash/Discount Price returned; alternative pharmacy returned Repeat 3 – 6 as necessary 7. Patient Consent to share cash claim info. Repeat 3 – 6 as necessary 8. Consent flag sent Cash Price Vendor PBM/Payer 3. Patient enters: Drug Name, Dosage, Form Patient/Patient-Facing App 2. Patient Login Validated (SMART on FHIR? Or Other validation? )
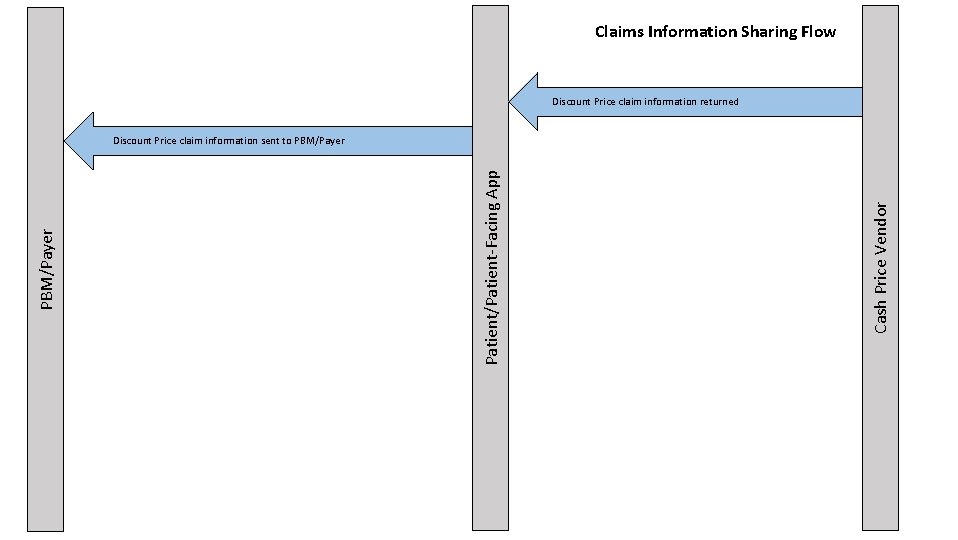
Claims Information Sharing Flow Discount Price claim information returned Cash Price Vendor Patient/Patient-Facing App PBM/Payer Discount Price claim information sent to PBM/Payer

Connectathon Goals and Approach Goal: • Test the implementation approach for the Consumer-facing RTPBC which will allow consumers to access benefit and cash price info. for their prescription medications • Confirm use of Claim, Claim. Response and Medication. Knowledge resources as best approach for RTPBC IG Approach: • • • Data elements identified Map data elements onto existing fields of Claim/Claim. Response Profile “stripped down” versions of referenced resources: • • • Patient Practitioner Coverage Medication. Knowledge (perhaps from Drug Formulary) Leverage Contained Resources (see https: //www. hl 7. org/fhir/claim-example-oral-contained. html) to support allinclusive Claims Define extensions as needed (limited number needed) © 2019 LEAVITT PARTNERS 10

Test Scenarios: • Scenario 1: PBM/Payer • Mobile health app developer sends request for patient level pharmacy benefit information for a specific medication to a PBM/Payer. Mandatory fields include: Patient, Coverage, Medication, Prescriber and Pharmacy • PBM/Payer sends response to mobile health app developer with patient specific coverage information. • Mandatory fields include: On/Off Formulary, If on formulary – patient out of pocket cost. If off formulary, alternative medications with patient out of pocket cost. Scenario 2: Cash/Discount Vendor • Mobile health app developer sends request for cash/discount pricing for a specific medication to a cash/discount vendor. Mandatory fields include: Patient, Medication, Prescriber and Pharmacy • Cash/Discount vendor sends response to mobile health app developer cash price information for requested pharmacy and pharmacy within X mile range of requested pharmacy. • Mandatory fields include: patient out of pocket cost for requested pharmacy, patient out of pocket cost for pharmacies within x mile range of requested pharmacy Underlying Assumption: Request is on behalf of patient and patient has been authenticated using SMART App Launch Framework © 2019 LEAVITT PARTNERS 11

PBM Request and Response Mandatory Fields Claim - https: //www. hl 7. org/fhir/claim. html PBM Request Fields • Patient Name (FN/LN), DOB, Gender, Zip – Claim Resource • Coverage (Member. ID, Rx Benefit ID, Unique PBM ID, Group ID) – Exists in claim Resource • Physician (Provider. ID, Last. Name, First. Name) – Exists in Claim Resource • Pharmacy (Pharmacy. ID and Location) – Requires new extension • Prescription (Product ID - NDC, Rx. Norm, UDI-DI, Quantity, Dose, Days Supply, DAW) Claim. Response - https: //www. hl 7. org/fhir/claimresponse. html PBM Response Fields • Requested Prescription (Product ID - NDC, Rx. Norm, UDI-DI, Quantity, Dose, Days Supply, DAW) – May require new extension • On/Off Formulary (exists in claim. response resource) • Patient Out of Pocket Cost if on formulary (exists in claim. response resource) • If off formulary, potential alternatives with out of pocket cost (Requires new extension) – May require new extension © 2019 LEAVITT PARTNERS 12

Cash/Discount Vendor Request and Response Mandatory Fields Open Question: Two separate API calls or one? GROUP DECISION: One API Call. Cash/Discount Vendor can ignore fields they don’t need. Could mobile health app send same request to both PBMs and Cash/Discount vendors, but receive different responses? Cash/Discount Vendor Request Fields • Patient Name (FN/LN), DOB, Gender, Zip – Claim Resource • Coverage (Member. ID, Rx Benefit ID, Unique PBM ID, Group ID) – Exists in claim Resource • Physician (Provider. ID, Last. Name, First. Name) – Exists in Claim Resource • Pharmacy (Pharmacy. ID and Location) – Requires new extension • Prescription (Product ID - NDC, Rx. Norm, Cash/Discount Vendor Response Fields • Requested Prescription (Product ID - NDC, Rx. Norm, UDI-DI, Quantity, Dose, Days Supply, DAW) – May require new extension • Patient Out of Pocket Cost at requested pharmacy • Patient Out of Pocket cost at pharmacy within x miles of requested pharmacy UDI-DI, Quantity, Dose, Days Supply, DAW) – May require new extension © 2019 LEAVITT PARTNERS 13
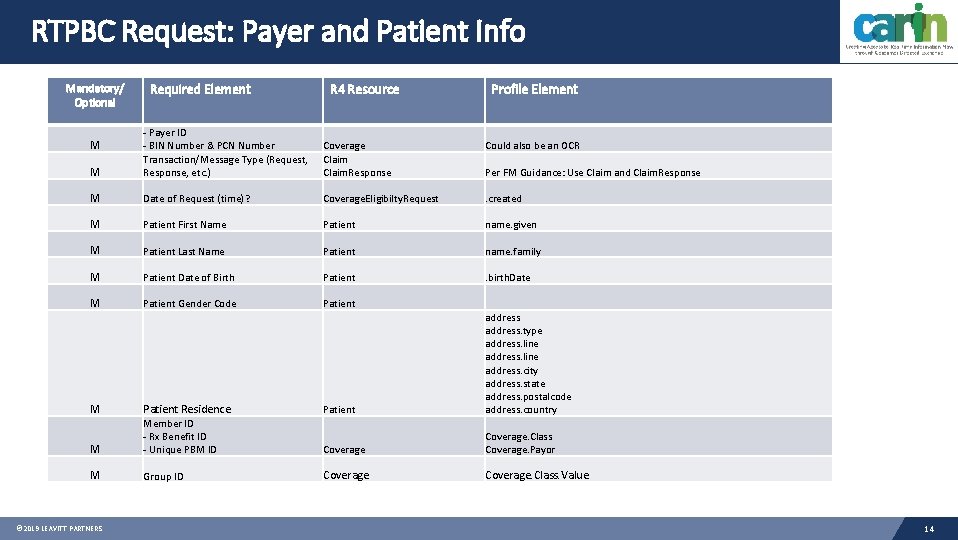
RTPBC Request: Payer and Patient Info Mandatory/ Optional Required Element R 4 Resource Profile Element Coverage Claim. Response Could also be an OCR M - Payer ID - BIN Number & PCN Number Transaction/Message Type (Request, Response, etc. ) M Date of Request (time)? Coverage. Eligibilty. Request . created M Patient First Name Patient name. given M Patient Last Name Patient name. family M Patient Date of Birth Patient . birth. Date M Patient Gender Code Patient M Per FM Guidance: Use Claim and Claim. Response M Patient Residence Patient address. type address. line address. city address. state address. postalcode address. country M Member ID - Rx Benefit ID - Unique PBM ID Coverage. Class Coverage. Payor M Group ID Coverage. Class. Value © 2019 LEAVITT PARTNERS 14
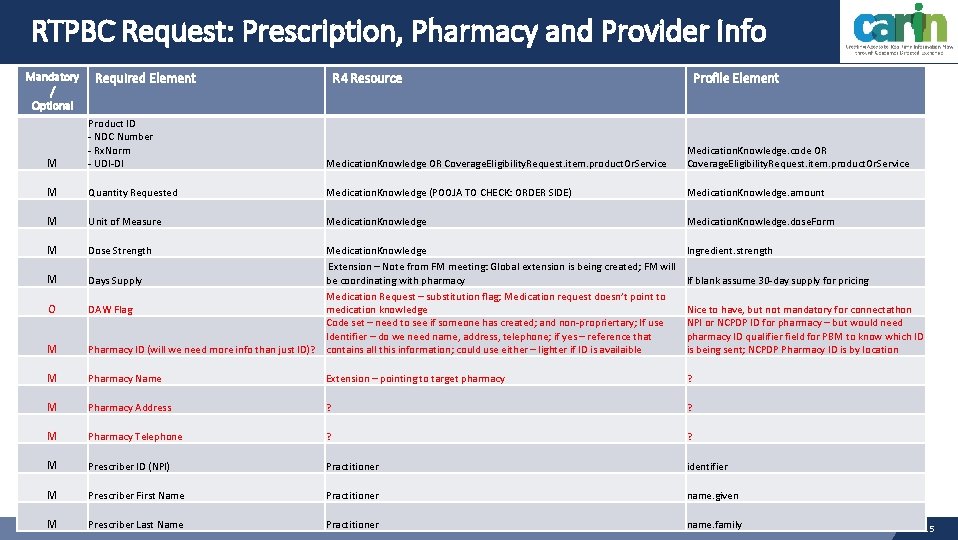
RTPBC Request: Prescription, Pharmacy and Provider Info Mandatory / Optional Required Element R 4 Resource Profile Element M Product ID - NDC Number - Rx. Norm - UDI-DI Medication. Knowledge OR Coverage. Eligibility. Request. item. product. Or. Service Medication. Knowledge. code OR Coverage. Eligibility. Request. item. product. Or. Service M Quantity Requested Medication. Knowledge (POOJA TO CHECK: ORDER SIDE) Medication. Knowledge. amount M Unit of Measure Medication. Knowledge. dose. Form M Dose Strength Ingredient. strength M Medication. Knowledge Extension – Note from FM meeting: Global extension is being created; FM will Days Supply be coordinating with pharmacy Medication Request – substitution flag; Medication request doesn’t point to DAW Flag medication knowledge Code set – need to see if someone has created; and non-propriertary; If use Identifier – do we need name, address, telephone; if yes – reference that Pharmacy ID (will we need more info than just ID)? contains all this information; could use either – lighter if ID is availaible M Pharmacy Name Extension – pointing to target pharmacy ? M Pharmacy Address ? ? M Pharmacy Telephone ? ? M Prescriber ID (NPI) Practitioner identifier M Prescriber First Name Practitioner name. given Practitioner name. family M O M PARTNERS Prescriber © 2019 LEAVITT Last Name If blank assume 30 -day supply for pricing Nice to have, but not mandatory for connectathon NPI or NCPDP ID for pharmacy – but would need pharmacy ID qualifier field for PBM to know which ID is being sent; NCPDP Pharmacy ID is by location 15
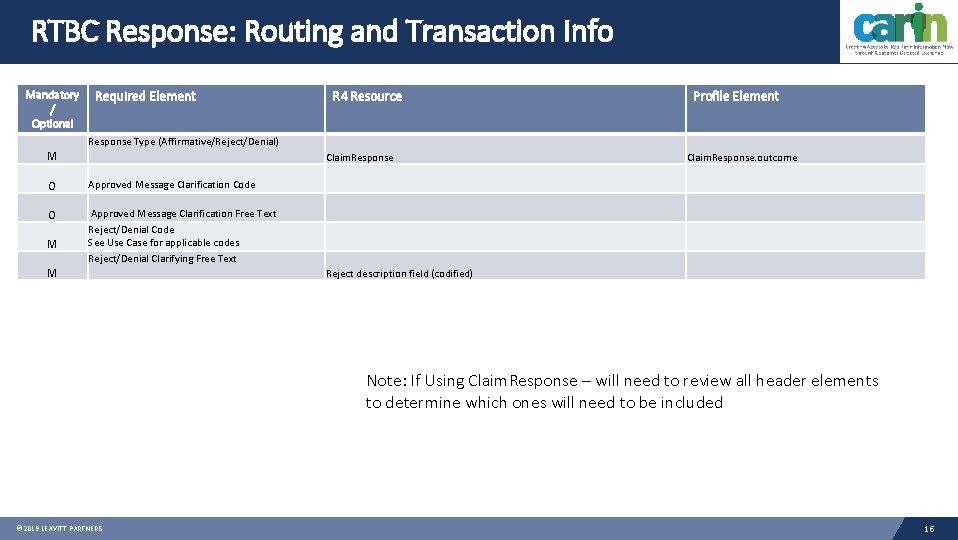
RTBC Response: Routing and Transaction Info Mandatory / Optional Required Element R 4 Resource Profile Element Response Type (Affirmative/Reject/Denial) M Claim. Response O Approved Message Clarification Code O Approved Message Clarification Free Text Reject/Denial Code See Use Case for applicable codes Reject/Denial Clarifying Free Text M M Claim. Response. outcome Reject description field (codified) Note: If Using Claim. Response – will need to review all header elements to determine which ones will need to be included © 2019 LEAVITT PARTNERS 16
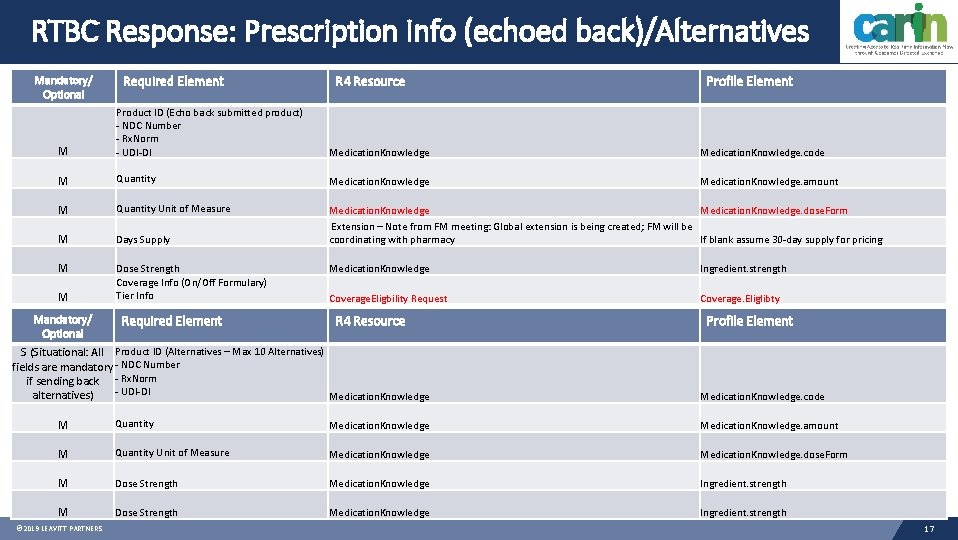
RTBC Response: Prescription Info (echoed back)/Alternatives Mandatory/ Optional Required Element R 4 Resource Profile Element M Product ID (Echo back submitted product) - NDC Number - Rx. Norm - UDI-DI Medication. Knowledge. code M Quantity Medication. Knowledge. amount M Quantity Unit of Measure M Days Supply Medication. Knowledge. dose. Form Extension – Note from FM meeting: Global extension is being created; FM will be coordinating with pharmacy If blank assume 30 -day supply for pricing M Dose Strength Coverage Info (On/Off Formulary) Tier Info M Mandatory/ Optional Required Element Medication. Knowledge Ingredient. strength Coverage. Eligbility Request Coverage. Eliglibty R 4 Resource S (Situational: All Product ID (Alternatives – Max 10 Alternatives) fields are mandatory - NDC Number if sending back - Rx. Norm - UDI-DI alternatives) Medication. Knowledge Profile Element Medication. Knowledge. code M Quantity Medication. Knowledge. amount M Quantity Unit of Measure Medication. Knowledge. dose. Form M Dose Strength Medication. Knowledge Ingredient. strength © 2019 LEAVITT PARTNERS 17
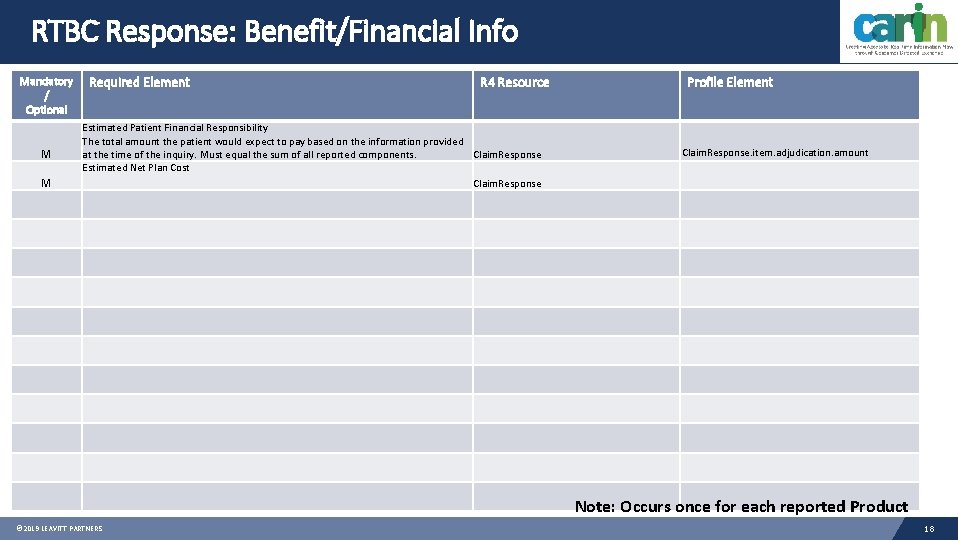
RTBC Response: Benefit/Financial Info Mandatory / Optional M M Required Element R 4 Resource Estimated Patient Financial Responsibility The total amount the patient would expect to pay based on the information provided at the time of the inquiry. Must equal the sum of all reported components. Claim. Response Estimated Net Plan Cost Claim. Response Profile Element Claim. Response. item. adjudication. amount Note: Occurs once for each reported Product © 2019 LEAVITT PARTNERS 18
- Slides: 18