Political economy issues and systems capacity development illustrated













- Slides: 16

Political economy issues and systems capacity development - illustrated for health financing Presentation prepared for the GTZ/GIZ Forum 2011 Inke Mathauer, MSc. , Ph. D Department of Health Systems Financing 1|

Outline 1. Political economy analysis: - Main actors and relations, typical interests and conflicts - Understanding institutions, organizations and incentives 2. Capacity development to strengthen accountability relationships 3. Political economy challenges to systems capacity development 4. Way forward and implications for system capacity development 2|

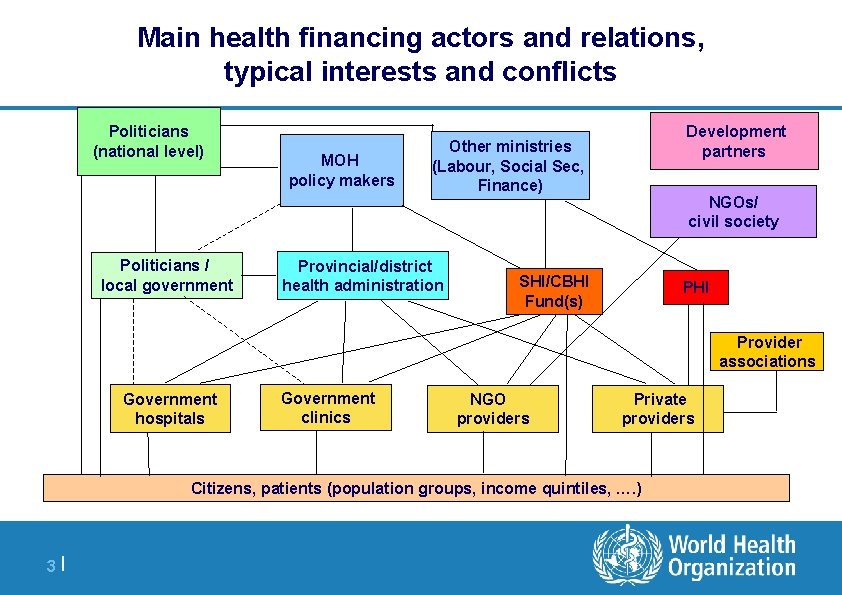
Main health financing actors and relations, typical interests and conflicts Politicians (national level) Politicians / local government MOH policy makers Development partners Other ministries (Labour, Social Sec, Finance) Provincial/district health administration NGOs/ civil society SHI/CBHI Fund(s) PHI Provider associations Government hospitals Government clinics NGO providers Private providers Citizens, patients (population groups, income quintiles, …. ) 3|

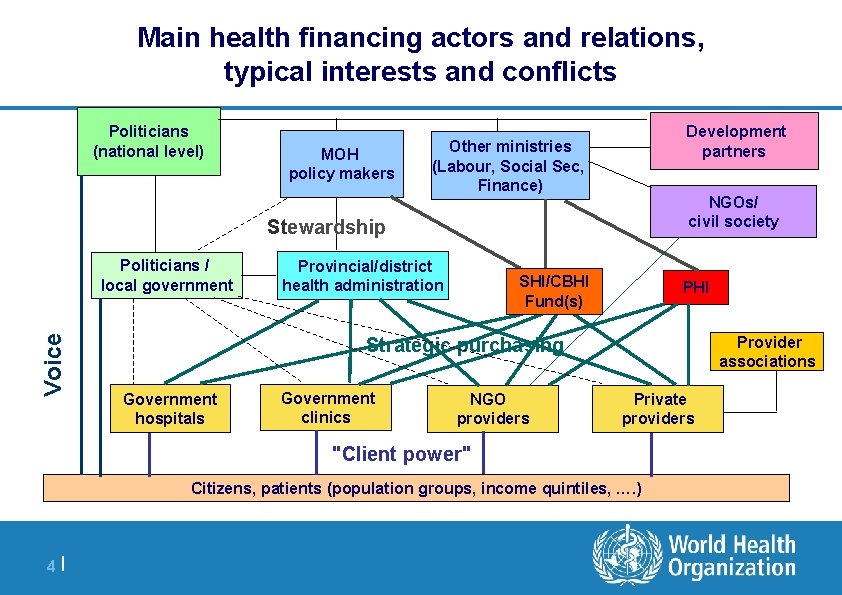
Main health financing actors and relations, typical interests and conflicts Politicians (national level) MOH policy makers Development partners Other ministries (Labour, Social Sec, Finance) NGOs/ civil society Stewardship Voice Politicians / local government Provincial/district health administration SHI/CBHI Fund(s) PHI Provider associations Strategic purchasing Government hospitals Government clinics NGO providers Private providers "Client power" Citizens, patients (population groups, income quintiles, …. ) 4|

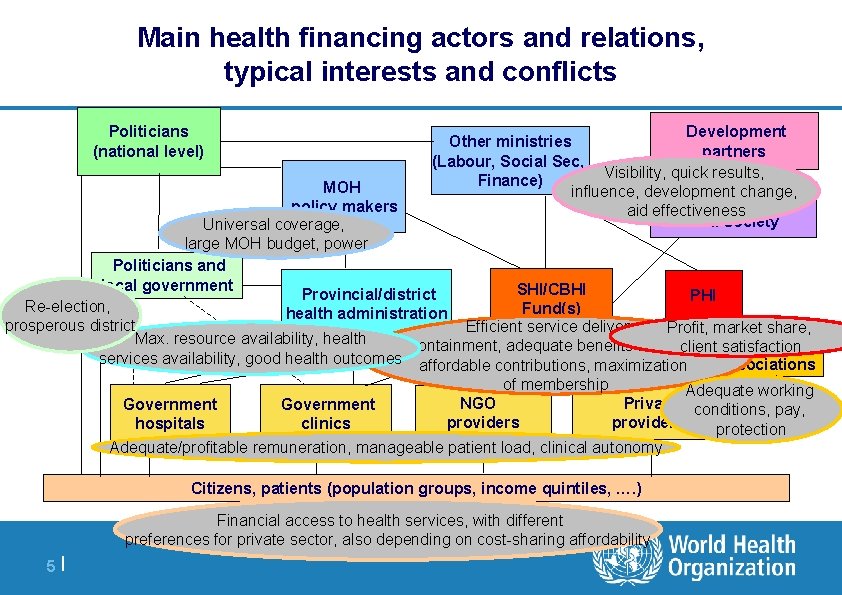
Main health financing actors and relations, typical interests and conflicts Politicians (national level) Development Other ministries partners (Labour, Social Sec, Visibility, quick results, Finance) influence, development change, NGOs/ aid effectiveness civil society MOH policy makers Universal coverage, large MOH budget, power Politicians and local government SHI/CBHI Provincial/district PHI Re-election, Fund(s ) health administration prosperous district Efficient service delivery, Profit, market share, Max. resource availability, health cost-containment, adequate benefits for members, Provider client satisfaction services availability, good health outcomes affordable contributions, maximization associations of membership Adequate working NGO Private conditions, pay, Government providers clinics hospitals protection Adequate/profitable remuneration, manageable patient load, clinical autonomy Citizens, patients (population groups, income quintiles, …. ) Financial access to health services, with different preferences for private sector, also depending on cost-sharing affordability 5|

Reality is even more complex: Example from Benin One of the proposals for the SHI framework in Benin 6|

Political economy analysis: Understanding institutions, organizations, interests and incentives in health financing Institutional design of health financing: l Rules, legal / regulatory provisions, specifying the health financing functions (reforms are a package of new/revised rules) => Rules have a purpose and oblige or enhance individuals or organizations to behave in a certain way, usually by means of enforcement characteristics (incentives, disincentives, constraints). Organizational practice of health financing: l mainly determined by power relations and the organization's / individuals' specific interests, shaped by – self-interest, profit maximization, work conditions, staff needs for recognition and status, preferences, informal rules, solidarity motivations, etc. <= Incentives and disincentives derive from the benefits or disadvantages that actually or potentially accrue to individuals due to health financing rules or other rules. 7|

Designing rules / reforms Health financing actors try to shape rules (reforms) along their interests Frequent deficits in institutional design: - Absence of rules (e. g. , lack of PHI regulation) Inadequate rules (e. g. fragmented SHI membership groups) Non-aligned rules (e. g. , minimum contribution not in line with real minimum wage) Implementing rules / reforms Health financing actors may/may not want or be able to comply with rules, i. e. implement rules (reforms) Frequent deficits in organizational practice: - Weak enforcement of rules (e. g. , weak inspection) - Non-conducive inter-organizational relationships (e. g. , little info exchange between ministries) - Weak organizational capacity Core aim: understanding root causes of poor performance 8|

WHO's OASIS approach Institutional and Organizational ASsessment for Improving and Strengthening HF 1. Health financing system review and performance assessment 2. Detailed institutional-organizational analysis to identify the strengths and deficits in institutional design and organizational practice – Map actors and stakeholders – Identify incentives and interests => Understand reform agendas/arenas and potential entry points 3. Identifying / assessing context-appropriate options and reforms that contribute to moving towards universal coverage – – – 9| Anticipation of reform impacts Assessment of political/technical/institutional/implementation feasibility Assessment of financial implications

Capacity development activities to enhance accountability relationships - aligning stakeholder incentives with policy objectives - between citizens and politicians/policy-makers: l Support development of a health financing policy/strategy – Clarification of strategic choices that a country has to make – Stronger focus on process management (wide stakeholder consultations) l Reinforce Ministries of Health in their negotiation capacity and "economic speak" with Ministries of Finance l Support reform development and reform implementation capacity l Strengthen organizational capacity of health committees and district health administrations in planning, budgeting, monitoring l Provide support to particular civic associations for their lobbying l Support benefit package (re-)definition to better address needs 10 |

Capacity development activities to enhance accountability relationships (cont. ) - aligning stakeholder incentives with policy objectives - between users and providers: l Support coverage increase via pooled prepayment l Promote targeted demand-side strengthening (vouchers, subsidized premiums, exemptions from cost-sharing) for low-income groups – combined with provider choice and some degree of provider autonomy l Strengthen community monitoring schemes of provider performance l Include utilization rates as one criteria for provider remuneration 11 |

Capacity development activities to enhance accountability relationships (cont. ) - aligning stakeholder incentives with policy objectives - between providers and purchaser (strategic purchasing): l Promote provider autonomy l Promote revision of provider remuneration to set right incentives for equity and efficiency, e. g. – Clear and enforceable contracts – Move to a mix of provider payment mechanisms – Results-based/ performance-related payment l Needs based formula for resource allocation from national to subnational levels 12 |

Political economy challenges to system capacity development in health/social protection l "Technical" aspects + their efficiency / equity impacts are complex – What is a "good enough" and feasible institutional design in a given context? l Enormous complexity for system capacity development in health: – Multiple actors, overlapping sub-systems, policy agendas, reform arenas, sector governance, decision-making structures: Where, when and how to enter? l Public/societal objectives (equity, universal coverage) vs. private interests l (Limited) notions of solidarity cannot be changed quickly; expectations by the middle class as an important voting group l Political economy concerns within the development partner community – Duplication, fragmentation, competition among development partners – Donor programs are power assets for policy makers/senior MOH staff – Accountability towards their own citizens (need for quick results) 13 |

Way forward and implications for (bilaterals') system capacity development l Need for a (more explicit) political economy analysis of potential impacts of capacity development activities, also of development partner arena in health sector – jointly undertaken l Alignment of donor staff incentives with the Paris Declaration logic – Visibility versus coordinated, harmonized donor actions? l Stronger support to and guidance of donor actions by national health sector plans – All development partners' activities should be integral part of the Government's Program; no channeling of funds / support that fragments or bypasses the country structures l Speaking with one voice, donor partnerships (e. g. , P 4 H, IHP+) 14 |

Thank you! Questions? 15 | Comments!

References Mathauer I and Carrin G (2010): The role of institutional design and organizational practice for health financing performance and universal coverage, Health Policy, doi: 10. 1016/j. healthpol. 2010. 09. 013. also available as Discussion Paper, DP 5 -2010, Health Systems Financing Department, Geneva: World Health Organization; 2010. http: //www. who. int/health_financing/documents/dp_e_10_05 -instit_uc. pdf. Mathauer I and Carrin (2010): OASIS. A tool for Health financing system reviews - Performance assessment - Options for improvement, Geneva: WHO, Department of Health Systems Financing WHO (2010): World Health Report 2010: Health systems financing – a path to universal coverage, WHO: Geneva. www. who. int/health_financing 16 |