Jen Mac Pherson Unrecognized suffering in the ICU













- Slides: 15

Jen Mac. Pherson Unrecognized suffering in the ICU: Addressing dyspnea in mechanically ventilated patients

“…dyspnea per se can only be perceived by the person experiencing it. ”- American Thoracic Society

Mechanical Ventilation in the ICU “MV experiences are considered stressful and are strongly associated with spells of terror. ” Rotondi et al. � 45% of patients with an ETT recalled “feeling choked by the ETT” � 24% recalled “not getting enough air from the ETT” Other studies � 90% of COPD ICU survivors reported traumatic events during their stay � Of whom, 55% reported “Suffocation” � 47% of patients reported a median VAS measure of 50% of full scale

Optimizing Patient Comfort Identify any potential discomfort 2. Diagnose the reason for discomfort 3. Initiate therapeutic response to treat the discomfort 1.

Assessing Dyspnea Direct Approach � Use simple yes or no questions �“Is your breathing comfortable/okay/difficult? ” � Rating scales for quantitative measurements �VAS �Modified Borg scale �Numerical ordinal scale �Faces scale


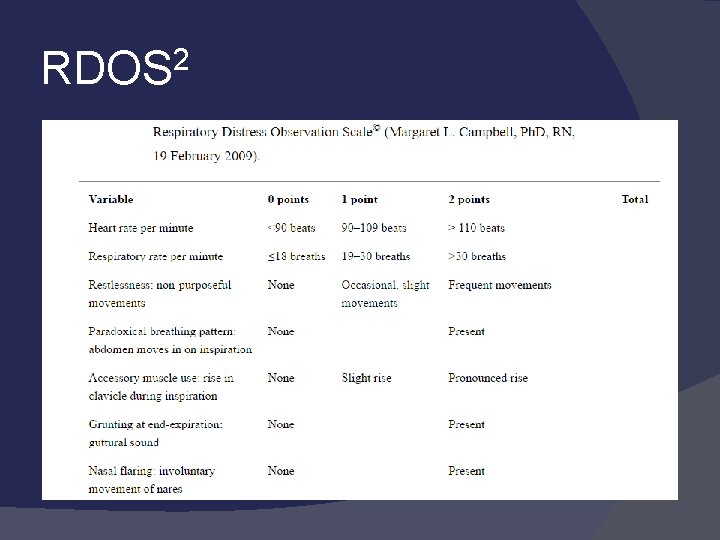
Assessing Dyspnea Indirect Approach � Respiratory Distress Observation Scale (RDOS) � Measures HR, RR, use of inspiratory neck muscles, presence of paradoxical abdominal movement, restlessness, presence of end-expiratory grunting and nasal flaring, as well as fearful facial displays � Individual clinical signs correlate poorly EMG measurements of extra-diaphragmatic inspiratory muscles � EEG: Premotor cortical activity � � Associated with inappropriate vent settings and respiratory discomfort

RDOS 2

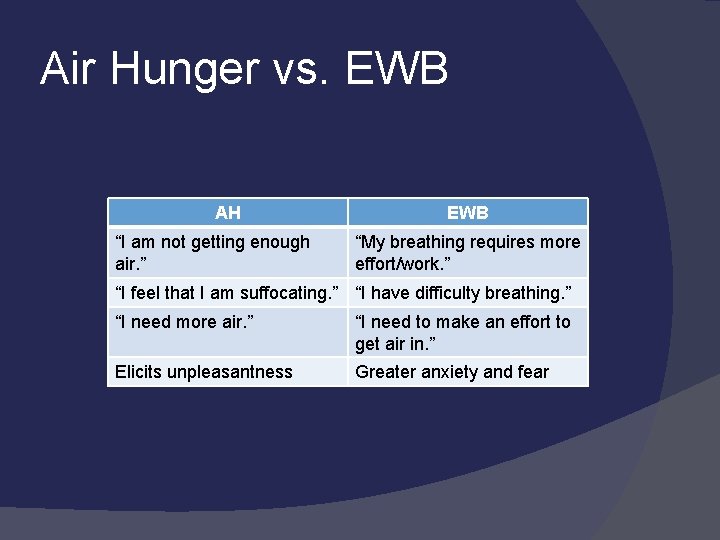
Air Hunger An “unpleasant, unsatisfied urge to breathe. ” Causes: hyperventilation, acidosis/ketoacidosis, infection (PNA, sepsis), heart failure, pulmonary embolism, severe pain, fight/flight response

Excessive Work of Breathing “Excessive breathing effort when gas exchange needs are adequately met. ” Cause: An imbalance between the load on respiratory muscles and their capacity to overcome it -increased respiratory impedance-> decreased respiratory muscle strength

Air Hunger vs. EWB AH “I am not getting enough air. ” EWB “My breathing requires more effort/work. ” “I feel that I am suffocating. ” “I have difficulty breathing. ” “I need more air. ” “I need to make an effort to get air in. ” Elicits unpleasantness Greater anxiety and fear

Determinants of Dyspnea Intrinsic Cardiopulmonary Status Ventilator Settings Patient-Ventilator Interface Non-respiratory Care Activities Extrinsic Physiological Stimulations Anxiety and Pain

Mechanical Ventilation & Anxiety � Anxiety and dyspnea= independently associated � 47% of ICU patients reported having felt anxiety and/or fear during MV � PTSD symptom scores are correlated with duration of MV � Anxiety may increase dyspnea by stimulating the ventilatory drive

Case Study

References Schmidt M, et al. Unrecognized suffering in the ICU: Addressing dyspnea in mechanically ventilated patients. Intensive Care Med. 2014; 40(1): 1 -10. 2. Campbell ML, Templin TN. Intensity cutpoints for the Respiratory Distress Observation Scale. Palliat Med. 2015; 29(5): 436 -442. 1.