Emergency Assessment and Procedures Emergency Assessment and Procedures


























- Slides: 28

Emergency Assessment and Procedures

Emergency Assessment and Procedures • Athletic Trainers can begin emergency procedures only after determining the problem • They must first gather pieces of information during an assessment to determine what is going on with the athlete • Mechanism of Injury • History • Primary Assessment • Secondary Assessment • Vital signs

Permission to Treat • If working with an unfamiliar athlete, first introduce yourself and ask permission to treat the athlete • Most athletes are teenagers and can’t refuse treatment • Parents also customarily sign waivers that allow for treatment in their absence • If a parent refuses treatment, document the refusal of treatment • Have athlete sign refusal in front of a witness • Refusal of treatment is rare, but must be followed

Sign or Symptom? • When investigating an athlete’s injuries, the Athletic Trainer must ask question and observe for signs and symptoms • Sign • Objective evidence that a rescuer can measure of sense • Ex. Sweating, breath odor, temperature, blood pressure, breathing rate, heart rate • Symptom • Cannot be seen smelled or heard • Ex. Pain, nausea, and anxiety

Types of Assessments • Primary Assessment • Deals with injuries that are life threatening, or injuries involving the ABCs • Airway, Breathing, Circulation • Secondary Assessment • Involves all non-life threatening injuries

Primary Assessment • • Primary Assessments are done in the following order Check the scene Determining responsiveness CAB • Circulation • Airway • Breathing

Checking the Scene • The first step to preventing any more injuries includes making sure you do not get hurt • Approach the athlete only when the scene appears safe • Ex. If a player is hurt during a football game, ensure that play has stopped so that you don’t get hit by another player when stepping on the field

Determining Responsiveness • The first step is to determine whether an athlete is conscious and able to respond • An unconscious athlete may be able to hear the AT and respond to a voice if they do not have a severe head injury • If there is not response, check the CABs, immediately alert EMS and send for the AED • If an athlete can clearly and logically respond to a responsiveness check the AT knows that the airway, breathing and circulation is OK • At this point in the primary assessment the AT can skip the CABS and proceed to check for other injuries

Initializing the CAB Sequence • If the respiratory or circulation system is impaired, the athlete’s life is in danger and the AT must respond quickly to give the athlete the best chance of survival. • Quick action and early chest compressions without interruptions are recommended

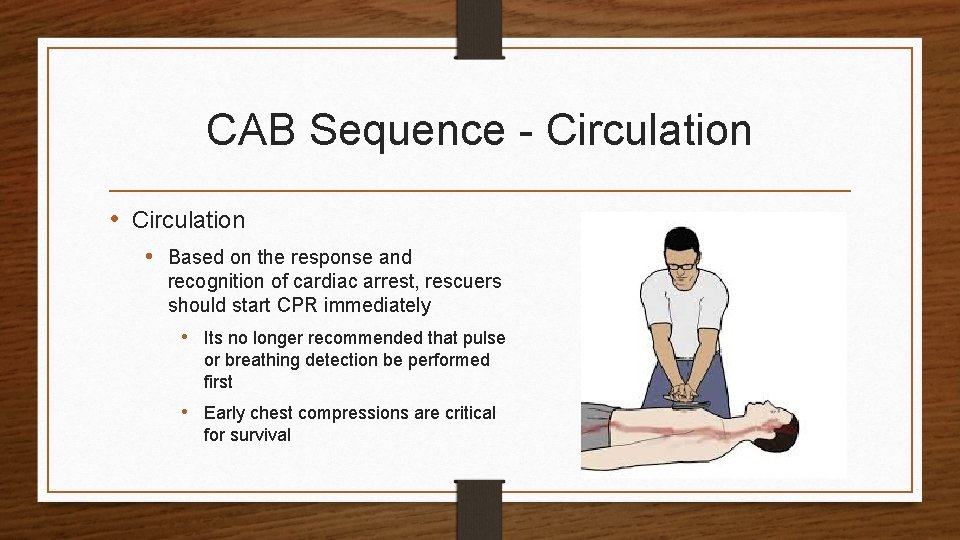
CAB Sequence - Circulation • Based on the response and recognition of cardiac arrest, rescuers should start CPR immediately • Its no longer recommended that pulse or breathing detection be performed first • Early chest compressions are critical for survival

CAB Sequence – Airway • An untrained rescuers should provide hands-only CPR, not interrupting compressions to check the airway or breathing • A trained rescuer who is able, should make sure that the airway is open • Place one hand on the forehead and 2 fingers under the chin and simultaneously lift the chin while controlling the head • This pulls the airway open by pulling the tongue away from the back of the throat • Head-tilt chin-lift procedure

CAB Sequence - Breathing • To check the breathing, the AT will use a technique called look, listen and feel • Look at the chest and watch for the chest to rise and fall • Listen for breathing by placing an ear close to the mouth • Feel for hot breath on his cheek • The check for breathing should last about 10 seconds and should be done by a trained rescuer

Breathing Emergencies • Any situation in which breathing has stopped or is compromised is considered life threatening • If an AT determines that an athlete is not breathing when the primary survey is performed, rescue breaths and CPR may be initiated • An athlete’s airway can be obstructed in a number of ways, but the tongue is the number one airway obstructer

Obstructed Airway • In an unconscious athlete, especially one lying on their back, the tongue likely will relax and obstruct the air passage • Other possible obstructions • • Food Gum Mouth guards Broken teeth Vomit Blood Chewing tobacco • A conscious athlete with an obstructed airway will grab at their throat

Types of Airway Obstructions • An airway obstruction could be partial or total • Athlete will grab for the throat, the universal choking sign, usually an indication that he has a problem with the air passage • Partial airway obstruction • Occurs when an object cover the air passage but still allows some air to flow in and out of the lungs • Total airway obstruction • When an object blocks the entire air passage and does not allow enough air to flow into the lungs for the athlete to breath

Cardiopulmonary Emergencies • There are 2 cardiopulmonary emergencies that concern the AT • Heart attack • Occurs when the heart muscle is damaged by a blockage of a vessel to the heart • Cardiac Arrest • Occurs when the damage to the heart muscle is so severe that it interferes with the hearts electrical system, causing the heart to stop beating

Secondary Assessment • An evaluation of injuries that aren’t life threatening • Performed after the primary assessment has been completed and life threatening injuries taken care of • Performed in the following order • History • Head • Vital signs • Arms • Chest • Abdomen • Hips • Legs

HIT • When dealing with a specific complaint Athletic Trainers will do an assessment on a specific body part and use the HIT technique • History • Takes history to gather information about the situation and injury • Inspection • Visual examination of the body part • Testing • Includes touching, specific evaluations, checking range of motion and neurological testing

History • Taking a history includes asking questions and taking vital signs • Allows athletic trainer to obtain information about what happening as well as previous injuries and illnesses • Vital signs checked in the secondary assessment can include • • Body temperature Skin color Breathing and Heart rate Response to pain Pupillary reaction Ability to move Capillary refill

Inspection • During the inspection the AT will observe the athlete’s body and surrounding for clues as to what happened • Helps to suggest treatment options

Testing • Specific tests are done to determine the following • Severity of the injury • How the athlete should be moved • If they should be splinted • If medical help is immediately necessary

Concussions • A concussion is the temporary impairment of brain function caused by impact to the head or by a rotation force • Causes the athlete to be confused or dazed and some may lose consciousness

Symptoms of a Concussion • • • Nausea Dizziness Headache Vomiting Difficulty speaking • Ringing in the ears (tinnitus) • Loss of balance • Difficulty remembering things before or after (amnesia) • Possible battle signs • Disorientation

Severity of Concussions • The severity of concussions are graded just as strains and sprains • Mild or first-degree • No loss of consciousness • Symptoms dissolve in less than 15 minutes • Moderate or second-degree • No loss of consciousness • Symptoms last more than 15 minutes • Severe or third-degree • Loss of consciousness for any amount of time

Treating a Concussion • When an athlete receives a concussion they must be monitored by a physician to determine when it is safe to reenter competition • In general, an athlete can’t return to play after the first concussion until all signs and symptoms have dissolved • Decisions about return to play are made by the AT and team physician • Most athletes who receive concussions will not return to participation until they’ve completed a progression of physical activity and follow up assessments that begin after they are free of all concussion symptoms

Second-Impact Syndrome • Occurs when an athlete has more than one concussion or blow to the head in a relatively short time • This trauma can disturb the blood supply to the brain, cause the athlete to lose brain function and present signs of a minor concussion followed by a semi comatose state or coma

Gfeller-Waller Concussion Awareness Act • This law was drafted and implemented to protect the safety of student-athletes in North Carolina • Signed into law by Governor Beverly Purdue on June 16, 2011 • Three main areas of focus • Education • Emergency action and post-concussion protocol implementation • Clearance/return to play or practice following concussion

Gfeller-Waller Concussion Awareness Act Matthew Gfellar Passed away August 24, 2008 only 2 days after receiving a concussion during his 1 st high school football game Jaquan Waller Passed away September 20, 2008 from second impact syndrome. He suffered from 2 concussions within a 3 day time frame.