CAPILLARY PUNCTURE EQUIPMENT AND PROCEDURES Chapter 10 Objectives

CAPILLARY PUNCTURE EQUIPMENT AND PROCEDURES Chapter 10

Objectives List and describe the various types of equipment needed for capillary specimen collection Describe the composition of capillary specimens, identify the tests that have different reference values when collected by capillary puncture methods, and name tests that cannot be performed on capillary specimens Identify indications for performing capillary puncture on adults, children, and infants List the order of draw for collecting capillary specimens Describe proper procedure for selecting the puncture site and collecting capillary specimens

Capillary Puncture Equipment Lancet/Incision Devices Finger puncture Heel puncture Laser lancet

Capillary Puncture Equipment Collection Devices Microcollection Containers Microhematocrit tubes

Capillary Puncture Equipment Plastic/clay sealant Capillary blood gas collection equipment Collection tubes/caps Stirrers/magnets Microscope slides Warming devices

Capillary Puncture Principles Composition of capillary puncture blood Arterial blood Venous blood Capillary blood Interstitial fluid Intracellular fluid More closely resembles arterial blood Reference (normal) values for capillary puncture blood § Higher in capillary puncture blood – glucose § Lower in capillary puncture blood – total protein – calcium – potassium

Capillary Puncture Principles Indications for performing capillary puncture Adults No accessible veins To save veins for chemotherapy Clotting tendencies POCT procedures such as glucose monitoring Children and Infants To prevent anemia To prevent cardiac arrest from removal of large quantities of blood Venipuncture too difficult To prevent injury When capillary blood is preferred

Capillary Puncture Procedures Tests that cannot be performed by capillary puncture Erythrocyte sedimentation rate (ESR) Coagulation studies that require plasma Blood cultures Tests that require large volumes of serum or plasma

Capillary Puncture Principles Order of Draw Slides EDTA specimens Other additive specimens Serum specimens

Capillary Puncture Steps Step 1: Review test request Step 2: Approach, identify, and prepare patient Step 3: Verify diet restrictions and latex sensitivity Step 4: Sanitize hands and put on gloves Step 5: Position patient For finger: hand extended, palm up For heel: supine with foot lower than torso

Capillary Puncture Steps Step 6: Select puncture/incision site General criteria Should be warm, normal color, and free from scars, cuts, bruises, or rashes Do not choose cold, cyanotic, infected or edematous site Finger for adult/older child, heel for infant

Capillary Puncture Steps Adults and older children (over 1 year old) Use the palmar surface of the distal or end segment of the middle or ring finger of the nondominant hand Do not Use same side as mastectomy Use finger on child less than 1 year old Puncture side or tip of finger Puncture thumb, index, or little finger Puncture parallel to whorls of fingerprint

Capillary Puncture Steps
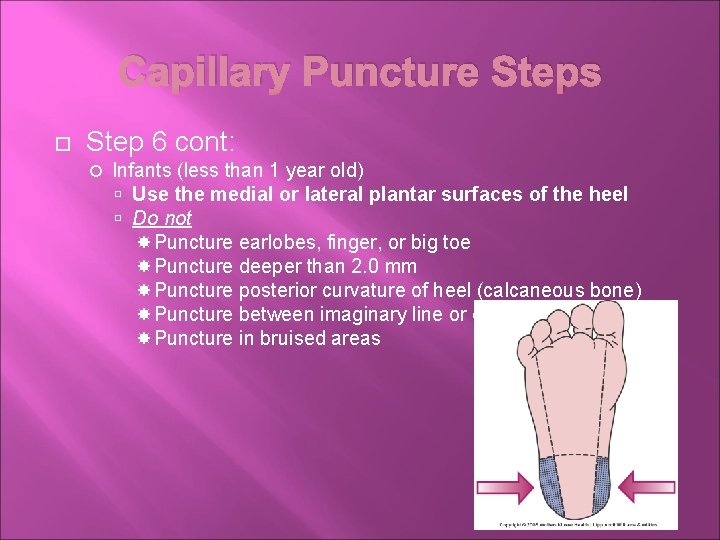
Capillary Puncture Steps Step 6 cont: Infants (less than 1 year old) Use the medial or lateral plantar surfaces of the heel Do not Puncture earlobes, finger, or big toe Puncture deeper than 2. 0 mm Puncture posterior curvature of heel (calcaneous bone) Puncture between imaginary line or on arch Puncture in bruised areas

Capillary Puncture Steps Step 7: Warm site if applicable Increases blood flow to site making collection easier especially in infant heel sticks “Arterializes” blood; essential for capillary blood gases Helps with finger puncture collection when patient has cold hands Step 8: Cleanse and air-dry site Do not use iodine; its yellow color interferes with uric acid, phosphorus, and potassium Step 9: Prepare equipment

Capillary Puncture Steps Step 10: Puncture the site and discard lancet Finger puncture: fleshy area, slightly off center, perpendicular to whorls of fingerprint Heel puncture: medial or lateral plantar surface For both finger and heel punctures Place lancet firmly against site Warn patient Depress lancet trigger Discard lancet in sharps container immediately

Capillary Puncture Steps Step 11: Wipe away first blood drop Step 12: Fill and mix tubes/containers in order of draw Gentle intermittent pressure, do not milk, position site downward to enhance flow Slide first, then EDTA, other additives, serum Microhematocrit tube: use capillary action Microcollection containers: touch blood drop, do not “scoop” or touch site Mix gently Step 13: Place gauze and apply pressure

Capillary Puncture Steps Step 14: Label specimen and observe special handling instructions Label with appropriate information Apply label directly to microcollection container Place microhematocrit tubes in nonadditive tube then label that tube Ice, body temperature, protect from light, etc.

Capillary Puncture Steps Step 15: Check the site and apply bandage Do not bandage children less than 2 years old Step 16: Dispose of used and contaminated materials Step 17: Thank patient, remove gloves, and sanitize hands Step 18: Transport specimen to lab

Special Capillary Puncture Procedures Capillary blood gases (CBG) Less desirable than ABG— exposed to air during collection, contains tissue fluid, rarely done on adults Desirable for infants and small children to avoid hazards of arterial puncture Warm site for 10 -15 minutes to maximize arterial flow Minimize exposure to air during collection
Special Capillary Puncture Procedures Neonatal bilirubin collection Done routinely on jaundiced (yellow) infants Minimize exposure to light during collection and transport Avoid hemolysis Newborn/neonatal screening Done routinely to detect inborn disorders PKU, hypothyroidism, galactosemia Blood drops collected on filter paper, fill circles from 1 side of the paper, air-dry horizontally
- Slides: 21