Erie County Department of Mental Health Adult Leadership





















- Slides: 22

Erie County Department of Mental Health Adult Leadership Meeting Challenges & Opportunities in Emerging Managed Care/RHBO Environment WESTERN REGION BEHAVIORAL HEALTH ORGANIZATON WITH BEACON HEALTH STRATEGIES, LLC AND COORDINATED CARE SERVICES, INC November 7, 2012

AGENDA n Review behavioral health managed care programs already in place focused on how they assess performance/impact Pennsylvania Health. Choices n Beacon Select n n What might we learn from these programs that could help us prepare for the future? n Next steps

Health. Choices: Pennsylvania Behavioral Health Managed Care Program

Health. Choices: Pennsylvania Behavioral Health Managed Care Program n Requires that BH Managed Care Organizations (BH-MCOs) supporting the publicly funded system participate in the State’s Performance /Outcomes Management System (POMS) n Database managed by PA’s Department of Public Welfare (DPW). n Produces set of performance measures/ indicators DPW uses as tool for continuously evaluating (CQI) the effectiveness of the BHMCO contractors in achieving system level outcomes.

PA Health. Choices: Outcome Dimensions n Increase Community Tenure and Less Restrictive n n n n Services Increase Vocational and Educational Status Reduce Criminal/Delinquent Activity Improve Health Care Increase Penetration Rates Increase Consumer/Family Satisfaction Implement continuous quality improvement (CQI) Actions Increase Range of Services and Improve Utilization Patterns

PA Health. Choices Outcome Dimensions Detail n Increase Community Tenure and Less Restrictive Services n n n n Increase in appropriate use of BH inpatient days Decrease criminal incarcerations Increase appropriate use of MH residential care Decrease out-of-home placements Decrease homelessness Decrease placements in C& Y custody Increase residential stability n Increase Vocational and Educational Status n Increase school attendance n Increase school performance n Improve school behavior n Increase vocational status for adults

PA Health. Choices Outcome Dimensions Detail n Reduce Criminal/Delinquent Activity Reduce number of arrests n Reduce positive drug screens n Improve probation/parole status n Reduce status offenses (focus on truancy) n Improve Health Care n Meet of exceed DPW’s EPSDT screening n Increase % of consumers with annual physical exams n Reduce hospital medical ER use n

PA Health. Choices Outcome Dimensions Detail n Increase penetration rates (% of enrollees who received BH treatment thru BH contractor) n n Increase appropriate utilization by priority group and type of service Increase appropriate utilization by age and type of service n Increase Range of Services and Improve Utilization patterns n n n Improve/increase array of trxt, support and rehab service options Decrease % of priority group consumers using only inpatient and/or ER services Reduce inpatient re-hospitalization rate Reduce rate of perinatal addictive disorders Reduce “drop-out” rates

Beacon Select Initiative What is it? Managed Care Program Model Pilot: Now in MA and moving into NY Purpose: Create a more sustainable model of BH care that supports a system of care for the client (effective linkages among services) and create a set of metrics that will support and monitor such development.

Beacon Select Initiative Program Goals n n n Redistribute administrative resources to target effective aftercare and support transition to the community. Target resources to assist outlier providers in appropriately managing utilization and quality measures, thus focusing attention on the providers for whom there will be the greatest impact. Transition the managed care process from an adversarial relationship of routine member management to a more collaborative and sustainable model. This enhanced collaboration will shift focus to ensuring access of quality care for members while containing cost through aggregate data management.

Beacon Select Initiative FACTORS CONTRIBUTING TO SUCCESS n Senior Management o A commitment from all levels of the organization is necessary, including the CEO and Medical Director. n Medical Necessity Criteria o In addition to having the utilization review staff understand Beacon’s Medical Necessity Criteria, it is imperative that the UR staff have the conversations around medical necessity during internal meetings that the managed care entity would have in a more traditional utilization management approach. n Infrastructure o Providers that have been successful with the Beacon Select Initiative have an infrastructure in place that allows self management to occur. n Communication o Select providers are assigned a Beacon Select Clinician. The provider is asked to designate staff to review systems issues, barriers to treatment or community resources.

Beacon Select Initiative Inpatient Processes and Procedures

Beacon Select Inpatient ADMISSIONS n There are no changes to the admission process for Beacon Select providers. Initial authorization is obtained in the same way regardless of whether the admission is to a Select or Non-Select provider. n Following admission; Select providers are not required to complete utilization reviews to obtain authorization for continued stay. n Authorizations are maintained by Select providers through an electronic portal. n Authorizations for inpatient admission at Select facilities will trigger treatment plan and discharge plan templates that can be accessed through Beacon’s web portal.

Beacon Select Inpatient PROVIDER SUCCESS IS DETERMINED THROUGH MEASUREMENT OF THE SELECT INITIATIVE’S KEY METRICS Average length of stay Rate of coordination between provider and PCP 7 / 30 day readmission rates Rate or coordination between provider and outpatient BH providers Administratively necessary days Aftercare appointment rate scheduled by facility within seven days of discharge

Beacon Select Inpatient ANALYSIS AND REVIEW n During the initial six months of a provider’s participation in the Beacon Select Initiative, provider performance on the identified metrics will be reviewed. n After the initial six month period, provider performance will be measured an assessment of provider performance will be completed. The provider will be supplied with data before and after participation in the Select Initiative. n All providers in the Select program have a site visit by the Beacon Select management team to review facility specific data. This site visit includes action items to identify best practices and opportunities for improvement. n For providers that do not maintain performance within the identified targets, additional analysis will be completed to determine if other factors should be considered. Beacon Select status may be lost, in which case the provider returns to Beacon’s standard UM procedures.

Beacon Select Outpatient Processes and Procedures

Beacon Select Outpatient n Beacon Select Outpatient targets high volume outpatient mental health providers who, in addition to meeting utilization targets, have demonstrated quality in the delivery of care. n Participating providers only register members annually with Beacon to receive outpatient services authorization-free. (Psychological testing is excluded). n “Report Cards” are distributed monthly measuring utilization and quality metrics.

Beacon Select Outpatient Selection PARTICIPATING PROVIDERS FALL INTO THREE CATAGORIES: 1. Very low utilization. Goal: Monitor to ensure there is no significant increase in utilization. 2. Average utilization. Goal: Maintain current utilization. 3. Utilization slightly above average. Goal: Modest reduction in utilization.

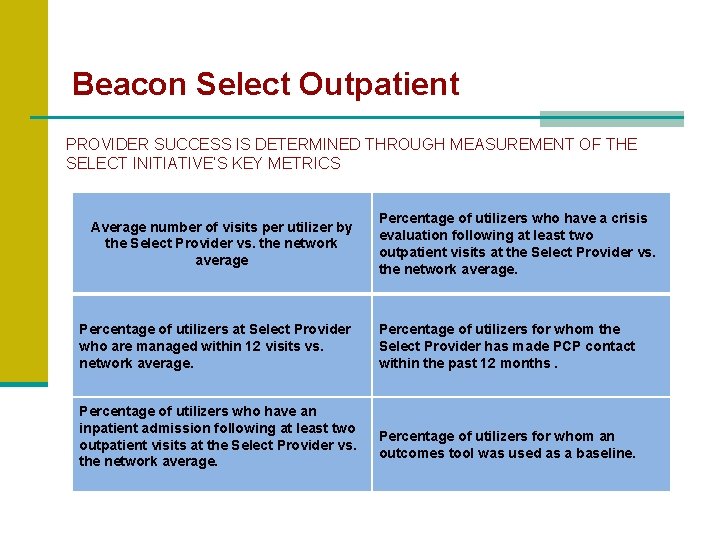
Beacon Select Outpatient PROVIDER SUCCESS IS DETERMINED THROUGH MEASUREMENT OF THE SELECT INITIATIVE’S KEY METRICS Average number of visits per utilizer by the Select Provider vs. the network average Percentage of utilizers at Select Provider who are managed within 12 visits vs. network average. Percentage of utilizers who have an inpatient admission following at least two outpatient visits at the Select Provider vs. the network average. Percentage of utilizers who have a crisis evaluation following at least two outpatient visits at the Select Provider vs. the network average. Percentage of utilizers for whom the Select Provider has made PCP contact within the past 12 months. Percentage of utilizers for whom an outcomes tool was used as a baseline.

Other Possible Sources of Information n WRBHO Quarterly Reports n Ideas generated through the small group conversations that took place during the June BEST Meeting n OMH BHO Portal- metrics for state and region n WRBHO Inpatient Psychiatric Experience Report (due out mid November) n Health Home work now taking place

What do we see in the approaches these models take that we might want to pay attention to? n Systems metrics n Other

Next Steps… n How do we best use data to support change in the county as we move towards some form of BH managed care? n How can the BHO be of assistance?
 Erie county department of mental health
Erie county department of mental health Northern nevada adult mental health
Northern nevada adult mental health Mental health and mental illness chapter 20
Mental health and mental illness chapter 20 Stress management jeopardy
Stress management jeopardy Oklahoma department of mental health
Oklahoma department of mental health Mental health america san diego
Mental health america san diego Bexar county mental health services
Bexar county mental health services Mental health connection of tarrant county
Mental health connection of tarrant county King county mental health court
King county mental health court Davidson county mental health court
Davidson county mental health court Lenawee county community mental health
Lenawee county community mental health Douglas county mental health initiative
Douglas county mental health initiative Outagamie county mental health
Outagamie county mental health Sotch orange
Sotch orange 204 e holly ave sewell nj 08080
204 e holly ave sewell nj 08080 Cowlitz county health department
Cowlitz county health department Tuscarawas county health department
Tuscarawas county health department Sussex county health department
Sussex county health department Pueblo city county health department
Pueblo city county health department Milwaukee county human services
Milwaukee county human services Leelanau county health department
Leelanau county health department Barnstable county department of health and environment
Barnstable county department of health and environment Ldh health standards
Ldh health standards