Department of Orthopedic Surgery Vertebroplasty vs Kyphoplasty and

Department of Orthopedic Surgery Vertebroplasty vs Kyphoplasty and the Osteoporotic Fracture: Is it worth the time, who should do it, and why? Jeffrey M. Spivak, M. D. December 8, 2018
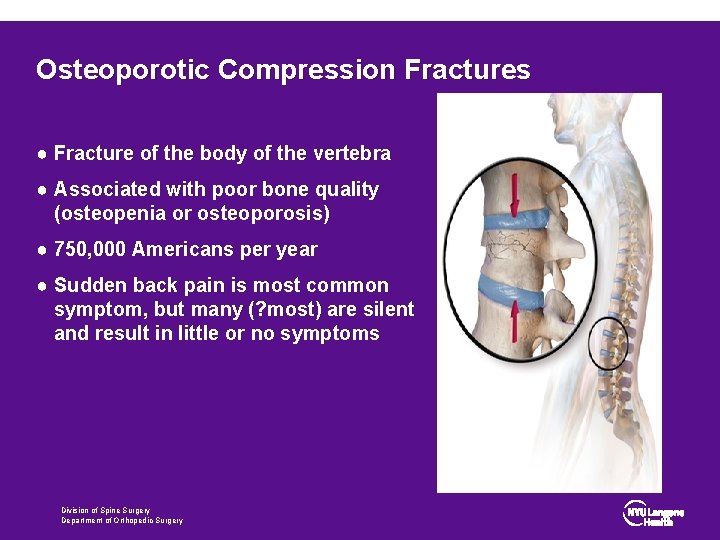
Osteoporotic Compression Fractures ● Fracture of the body of the vertebra ● Associated with poor bone quality (osteopenia or osteoporosis) ● 750, 000 Americans per year ● Sudden back pain is most common symptom, but many (? most) are silent and result in little or no symptoms Division of Spine Surgery Department of Orthopedic Surgery

Initial Management ● Diagnosed typically by x-ray ● MRI can be very helpful in assessing acuity ● Initial management is usually nonsurgical: • • • Pain control Possibly bracing and/or physical therapy Medical management of osteoporosis ● Nonsurgical treatment is typically trialed for at least 2 -3 weeks ● Pain symptoms typically subside over 6 -8 weeks in patients treated non-operatively Division of Spine Surgery Department of Orthopedic Surgery

Percutaneous Cementation Procedures ● Indications: • Continued pain/dysfunction despite 2 -3 weeks of nonoperative treatment • Acute kyphosis >20 degrees • Progressive collapse/kyphosis ● Relative contraindications: • • > 70% loss of vertebral body height Fracture fragments abutting neural structures (burst component) Neurologic symptoms Healed fractures ● Vertebroplasty vs. Kyphoplasty Division of Spine Surgery Department of Orthopedic Surgery
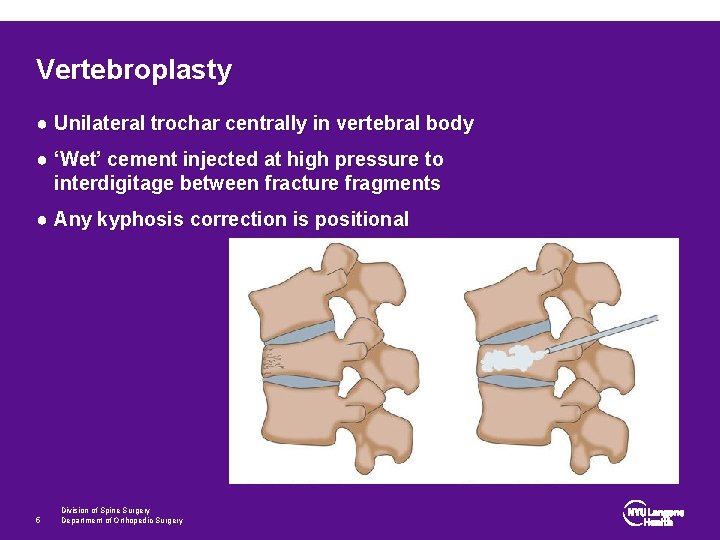
Vertebroplasty ● Unilateral trochar centrally in vertebral body ● ‘Wet’ cement injected at high pressure to interdigitage between fracture fragments ● Any kyphosis correction is positional 5 Division of Spine Surgery Department of Orthopedic Surgery
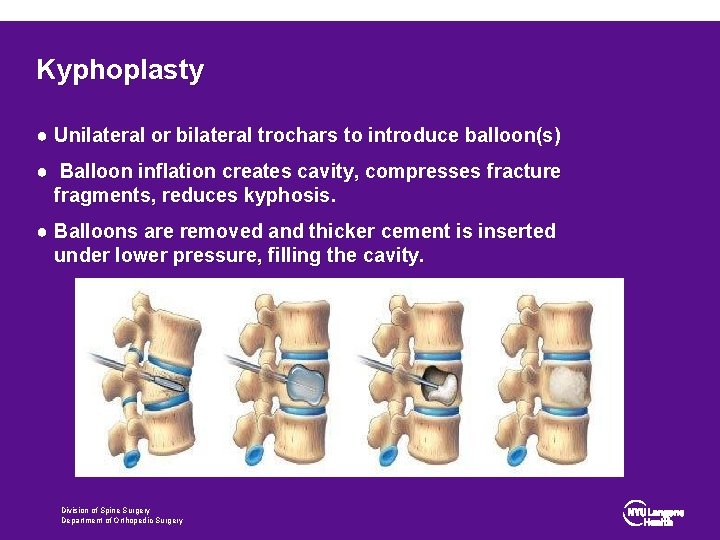
Kyphoplasty ● Unilateral or bilateral trochars to introduce balloon(s) ● Balloon inflation creates cavity, compresses fracture fragments, reduces kyphosis. ● Balloons are removed and thicker cement is inserted under lower pressure, filling the cavity. Division of Spine Surgery Department of Orthopedic Surgery
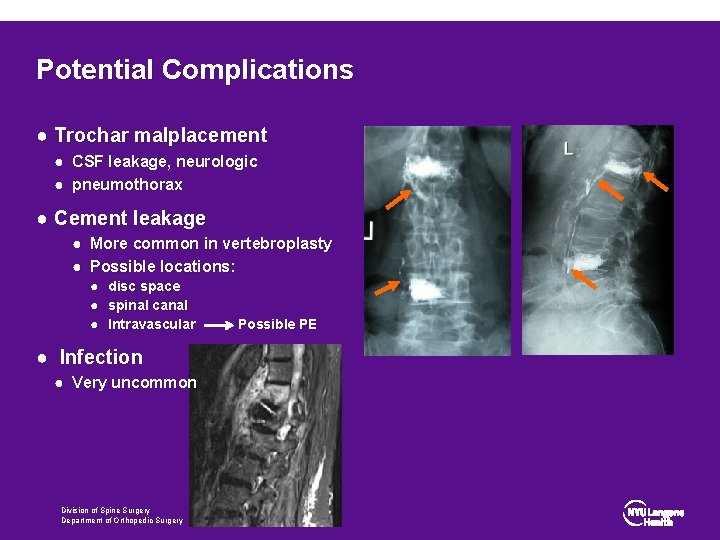
Potential Complications ● Trochar malplacement ● CSF leakage, neurologic ● pneumothorax ● Cement leakage ● More common in vertebroplasty ● Possible locations: ● disc space ● spinal canal ● Intravascular ● Infection ● Very uncommon Division of Spine Surgery Department of Orthopedic Surgery Possible PE

Outcomes: Vertebroplasty vs Sham Procedure ● In 2010 AAOS recommended “strongly” against vertebroplasty for treatment of compression fractures based on two level 1 multi-center NEJM studies comparing vertebroplasty to sham procedure ● These studies concluded there was no significant difference in outcomes between vertebroplasty and sham procedure (anesthetic injection) for compression fracture ● Both heavily criticized for methodology Division of Spine Surgery Department of Orthopedic Surgery

Outcomes: Vertebroplasty vs Sham Procedure Kallmes Study Criticisms ● Did not require MRI imaging ● No nonoperative group ● Outcomes taken only at 1 month postprocedure ● By 3 months 43% of sham group had crossed over to vertebroplasty making longer term follow-up impossible ● Fracture chronicity: only 40% of fractures were less than 3 months old; remainder from 3 -12 months ● Large number of Workers Compensation patients Division of Spine Surgery Department of Orthopedic Surgery

Outcomes: Vertebroplasty vs Sham Procedure Buchbinder Study Criticisms ● Required MRI but not physical exam ● No nonoperative group ● Follow-up was only up to 6 months ● Fracture chronicity: only 32% of fractures were less than 6 weeks old ● 68% of subjects were from one center Division of Spine Surgery Department of Orthopedic Surgery

Outcomes: Vertebroplasty vs Nonoperative Management ● The 2010 VERTOS II Trial compared vertebroplasty to nonoperative/medical treatment ● Was criticized for lack of blinding but excluded fractures > 6 weeks old ● Concluded that: • Vertebroplasty yielded better pain relief at 1 year • Vertebroplasty resulted in satisfactory pain relief 3 months faster than nonoperative management • Most nonoperative subjects achieved sufficient pain relief at 3 months leading authors to conclude that vertebral augmentation may be justified in patients without sufficient pain relief after 3 months of nonoperative management -Klazen CA et al. , Lancet. 2010 Sep 25; 376(9746): 1085 -92. Division of Spine Surgery Department of Orthopedic Surgery

Outcomes: Vertebroplasty vs Sham/Nonoperative Treatment ● There have since been multiple prospective RCTs ● Conclusions difficult to draw given heterogenous results ● A 2013 meta-analysis concluded that vertebroplasty had improved pain, functional and HRQOL outcomes compared to non-operative management or sham procedures at early and late follow-up points -Anderson PA, et al. , J Bone Miner Res. 2013 Feb; 28(2): 372 -82. ● Despite these more recent studies, vertebroplasty is less commonly used in treatment of compression fractures given 2010 AAOS recommendations Division of Spine Surgery Department of Orthopedic Surgery

Outcomes: Kyphoplasty vs Vertebroplasty • AAOS has provided a “limited” recommendation supporting the use of kyphoplasty for compression fractures based on separate studies comparing kyphoplasty to non-operative treatment • A few prospective RCTs have compared vertebroplasty directly to kyphoplasty Division of Spine Surgery Department of Orthopedic Surgery

Outcomes: Kyphoplasty vs Vertebroplasty • A systematic review concluded no significant difference in pain or disability outcomes at 1 -year follow-up between the two -Han S, et al. Int Orthop. 2011 Sep; 35(9): 1349 -58. • Kyphoplasty achieves greater correction of kyphotic deformity than vertebroplasty, but this has not been shown to be clinically significant -Van Meirhaeghe J, et al, Spine. 2013 May 20; 38(12): 971 -83. -Wang et al. , J Orthop Surg Res, 2018 Oct 22; 13(1): 264. • A 2016 meta-analysis additionally determined that kyphoplasty resulted in lower incidence of cement leakage though no significant difference in -Gu CN, et al, J Neurointerv Surg. 2016 Jun; 8(6): 636 -42. symptomatic cement leakage • Overall complication rate in both less than 1% -Chandra RV, et al, Am J Neuroradiol. 2018 May; 39(5): 798 -806. Division of Spine Surgery Department of Orthopedic Surgery

Cost Effectiveness of Vertebral Augmentation A 2012 study of Medicare patients concluded: ● Vertebral augmentation (both vertebroplasty and kyphoplasty) more costeffective than nonoperative management in terms of cost per life-yeargained, including in patients above 85 years of age ● Kyphoplasty procedure more expensive than vertebroplasty procedure but more cost-effective in terms of cost per life-year-gained -Edidin AA, et al. , Appl Health Econ Health Policy. 2012 Jul 1; 10(4): 273 -84. Division of Spine Surgery Department of Orthopedic Surgery
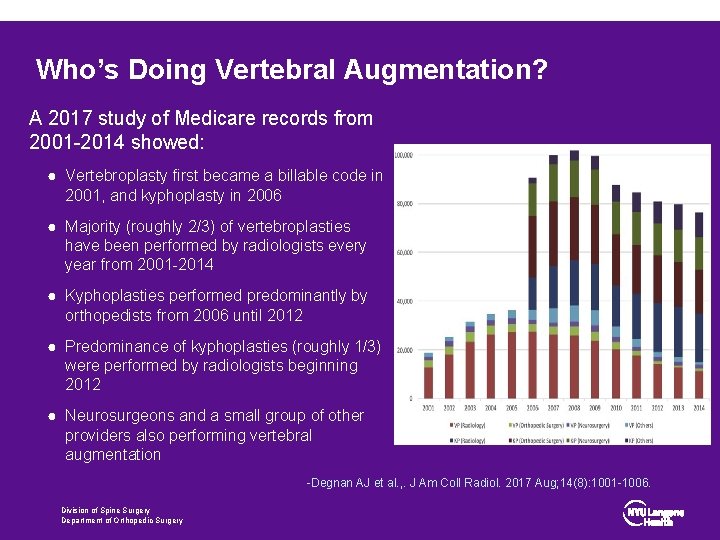
Who’s Doing Vertebral Augmentation? A 2017 study of Medicare records from 2001 -2014 showed: ● Vertebroplasty first became a billable code in 2001, and kyphoplasty in 2006 ● Majority (roughly 2/3) of vertebroplasties have been performed by radiologists every year from 2001 -2014 ● Kyphoplasties performed predominantly by orthopedists from 2006 until 2012 ● Predominance of kyphoplasties (roughly 1/3) were performed by radiologists beginning 2012 ● Neurosurgeons and a small group of other providers also performing vertebral augmentation -Degnan AJ et al. , . J Am Coll Radiol. 2017 Aug; 14(8): 1001 -1006. Division of Spine Surgery Department of Orthopedic Surgery

Summary ● Some controversy persists regarding vertebral cement augmentation for use in osteoporotic compression fractures; studies are ongoing ● At present vertebroplasty not commonly used given 2010 AAOS recommendations ● Kyphoplasty is commonly used, and is accepted as efficacious ● It can provide improved pain and function sooner than nonoperative treatment ● Kyphoplasty is more commonly being done by interventional radiologists Division of Spine Surgery Department of Orthopedic Surgery

THANK YOU
- Slides: 18